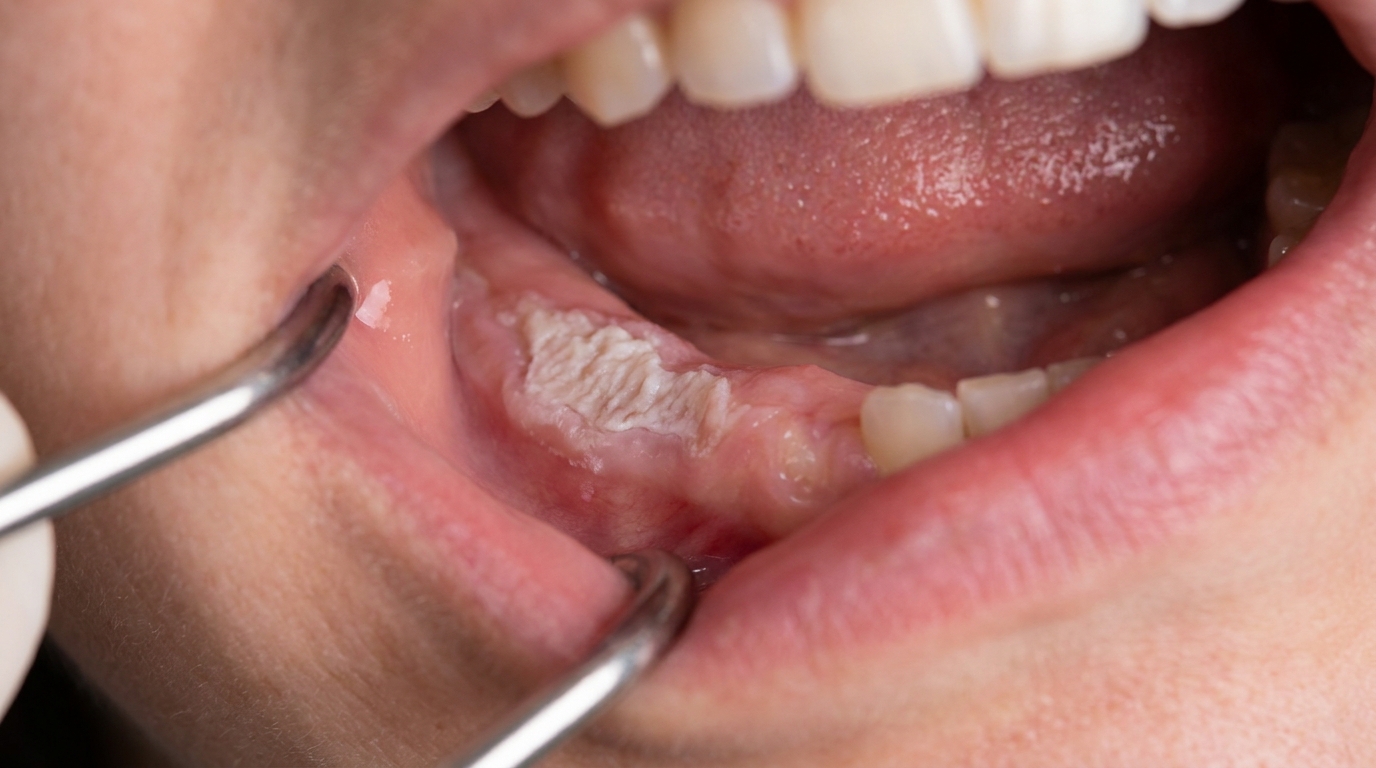
Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker , Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | Erythematous candidosis, thinned (atrophic) thrush (candidiasis), antibiotic sore mouth, denture sore mouth, denture stomatitis, central papillary atrophy, median rhomboid glossitis |
How urgent? | 🟡 Worth a check-up, usually treatable, but a sore red patch that lingers should always be assessed to rule out other causes |
Common or rare? | Common, likely more common than the white pseudomembranous form of thrush, although it is often overlooked |
Who it affects | Adults of any age; particularly denture wearers, people on antibiotics or steroid inhalers, smokers, people with dry mouth, and those with weakened immunity |
Who treats it | General dentist; specialist referral if it does not settle or if an underlying medical cause is suspected |
Based on | Regezi, Neville, Cawson |
What is it?
Erythematous candidiasis is a fungal infection of the mouth caused by an overgrowth of the yeast Candida albicans. Unlike the more familiar white "thrush" patches, this form shows up as flat red, sore-looking areas of mouth lining (mucosa) with very little or no white coating.
The yeast itself lives quietly in the mouths of most healthy people. It only causes trouble when something tips the balance in its favour, antibiotics, steroid inhalers, dry mouth, dentures, smoking, or a dip in immunity.
Who tends to get it?
Erythematous candidiasis affects adults far more often than children. It can appear at any age, but several groups are noticeably more prone to it.
Denture wearers are by far the largest group. Chronic red and inflamed (erythematous) candidiasis under a complete upper denture, known as denture stomatitis or denture sore mouth, has been reported in as many as 65% of older adults who wear full upper dentures. The lower denture is rarely involved because saliva flows more freely beneath it.
People taking broad-spectrum antibiotics or using steroid inhalers form the second main group. The acute version, sometimes called antibiotic sore mouth, often follows a course of antibiotics that has wiped out the bacteria normally keeping yeast in check.
Other people who tend to develop erythematous candidiasis include those with dry mouth (from medications, radiotherapy, or Sjögren syndrome (an autoimmune condition causing dry mouth and dry eyes)), people with diabetes, smokers, and those with weakened immunity, including people living with HIV, where it is one of the earliest oral signs and tends to appear when the immune system is significantly weakened (a CD4 cell count below around 400, the CD4 count is a blood measure used to gauge immune strength in HIV).
The related condition median rhomboid glossitis, a red, smooth, diamond-shaped patch in the centre of the tongue, is found almost exclusively in adults and shows a strong link with smoking.
What causes it?
The direct cause is overgrowth of Candida albicans (and occasionally other Candida species) on the lining of the mouth. The yeast is a normal commensal, meaning it lives there harmlessly in most people, and only becomes a problem when local or whole-body conditions allow it to flourish.
The textbooks list a fairly consistent set of predisposing factors:
Antibiotics, especially broad-spectrum or multiple narrow-spectrum courses, which suppress the competing bacteria that normally keep yeast in check.
Steroid inhalers, for asthma or COPD, particularly when the mouth is not rinsed after use.
Dry mouth (xerostomia), from medications, radiotherapy to the head and neck, or Sjögren syndrome. Saliva contains natural antifungal proteins, so a dry mouth is a friendlier environment for yeast.
Dentures, particularly a well-fitting upper denture, which seals the underlying mucosa off from saliva. Wearing the denture day and night, poor denture hygiene, and a denture that has lost its fit all increase the risk.
Smoking, appears to make the mouth more susceptible to candidal overgrowth, and is strongly linked with median rhomboid glossitis.
Diabetes mellitus, especially when blood sugar is poorly controlled.
Reduced immunity, from HIV, chemotherapy, organ transplant medication, or long-term corticosteroids.
Iron, folate, or vitamin B12 deficiency, anaemia can make the mucosa more vulnerable.
Most people with erythematous candidiasis have at least one of these factors, and often more than one.
How does it develop?
Think of the mouth as a small, busy ecosystem. Saliva, bacteria, yeast, and the mucosal lining all live in balance. Candida is one of many residents, usually peaceful, kept in line by competing bacteria, by saliva washing over the tissues, and by a working immune system.
When one of those checks is removed, the yeast multiplies. It changes from its quiet rounded form into elongated, thread-like structures (called hyphae) that burrow into the tough surface layer of the mouth lining. The body responds with inflammation, and small numbers of immune cells gather just beneath the surface. This combination, yeast in the surface layer plus inflammation in the tissue underneath, strips away the normal pink covering and exposes the redder, more vascular tissue below, which is what gives the lesion its angry red appearance.
Under a denture, the picture is slightly different. The denture base itself becomes a reservoir, with the porous acrylic harbouring yeast that constantly re-seeds the mucosa. The closed environment between denture and palate is warm, moist, and largely cut off from saliva, close to ideal conditions for Candida.
What might you notice?
What it looks like
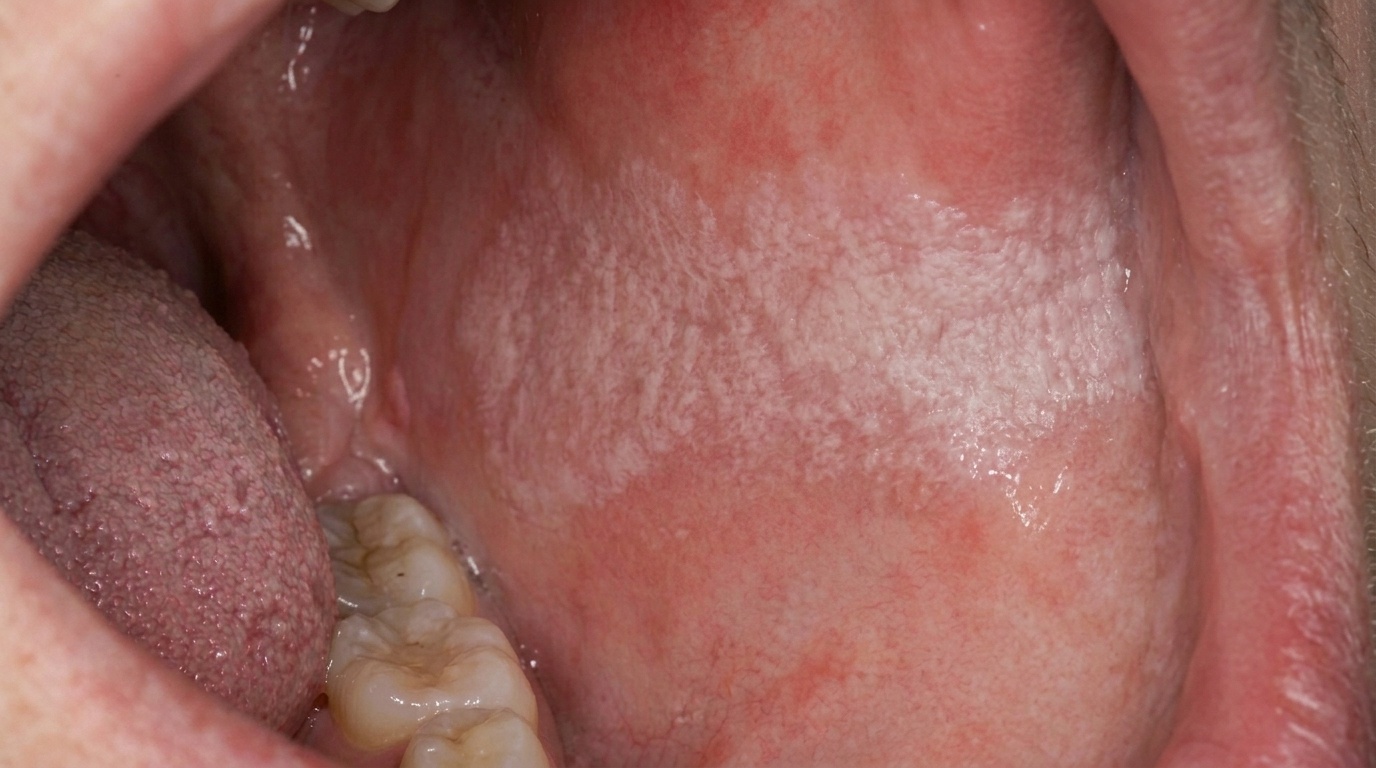
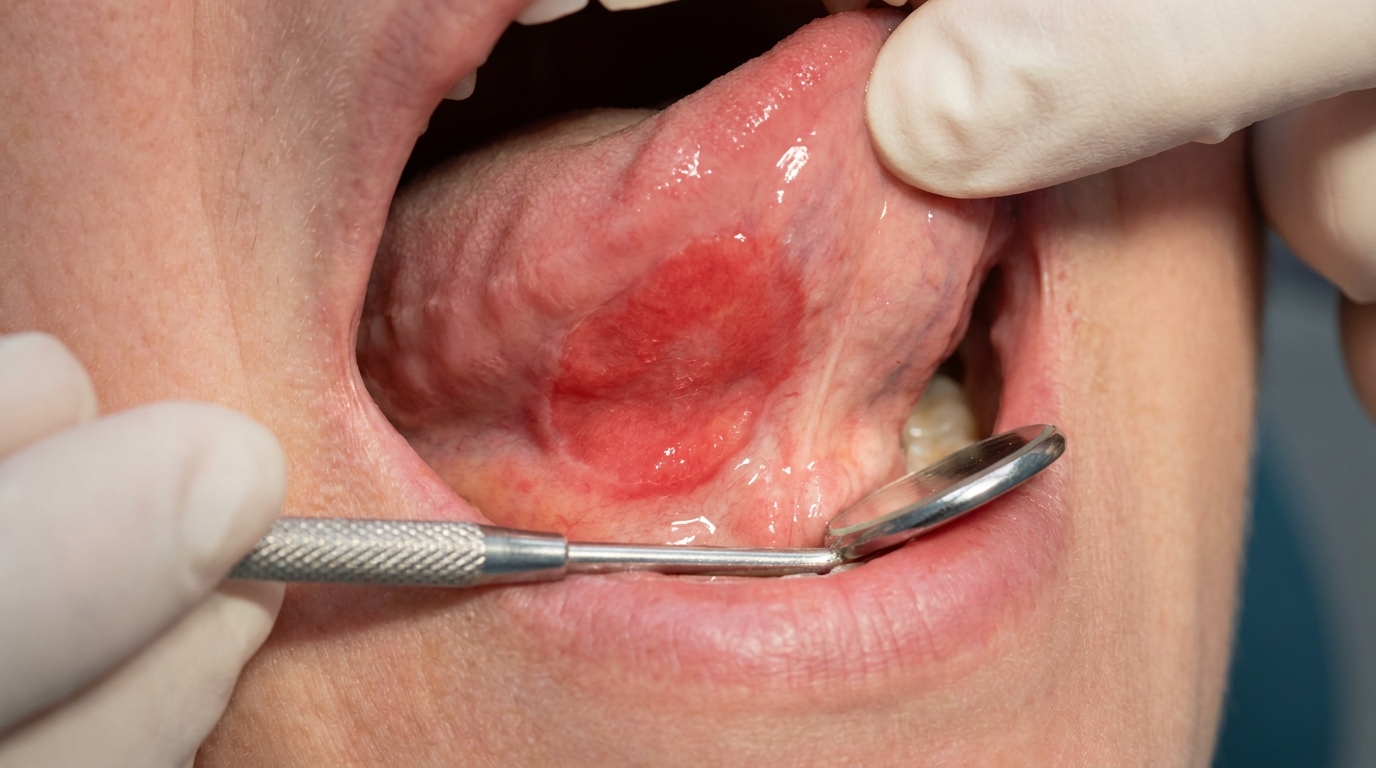
The trademark sign is a flat red patch of mucosa with little or no white coating. Several patterns are described:
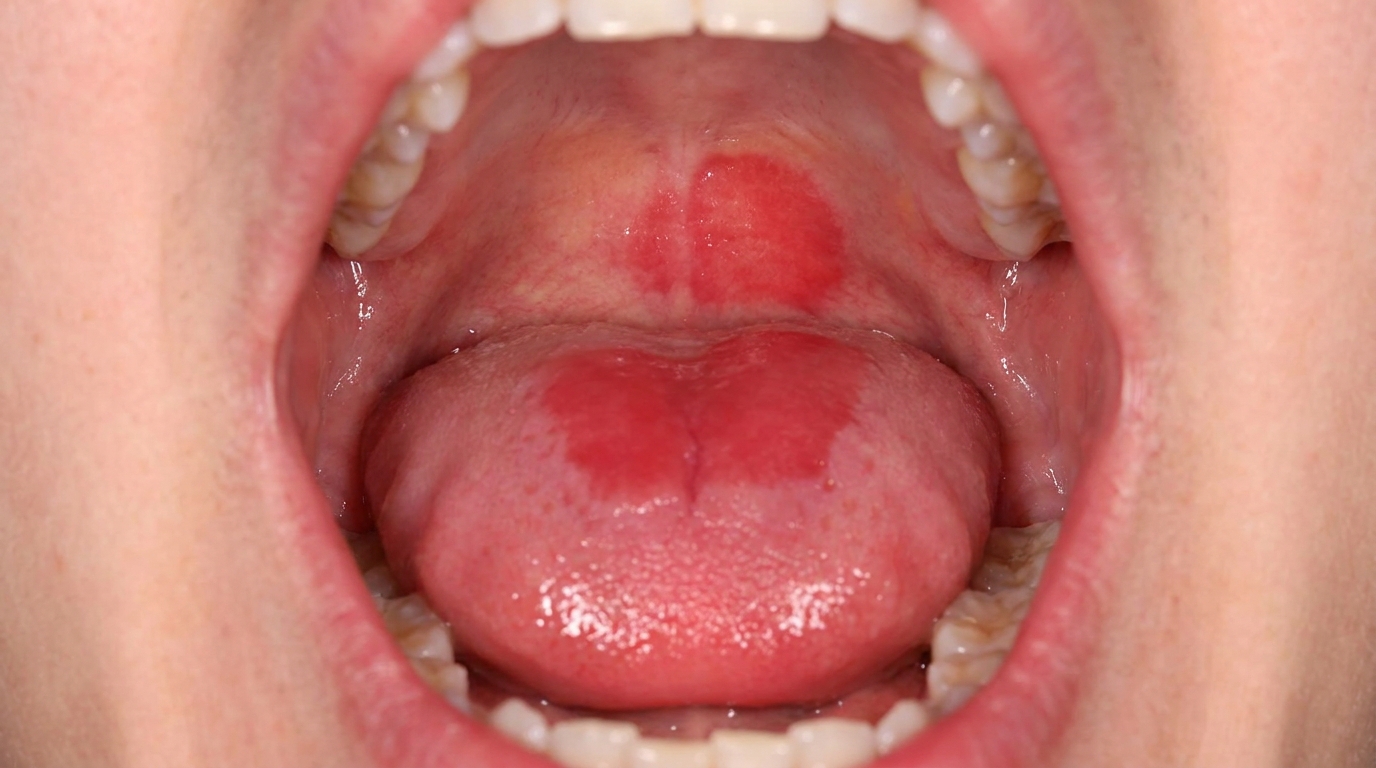
A diffuse red, smooth dorsal tongue, sometimes described as having a "bald" appearance because the tiny filiform papillae (the velvety surface bumps of the tongue) are lost. This is typical of acute antibiotic sore mouth.
A well-defined oval or diamond-shaped red patch in the middle of the tongue, just in front of the V-shaped row of larger papillae at the back. This is median rhomboid glossitis. A matching red "kissing lesion" can sometimes be seen on the palate where the tongue rests.
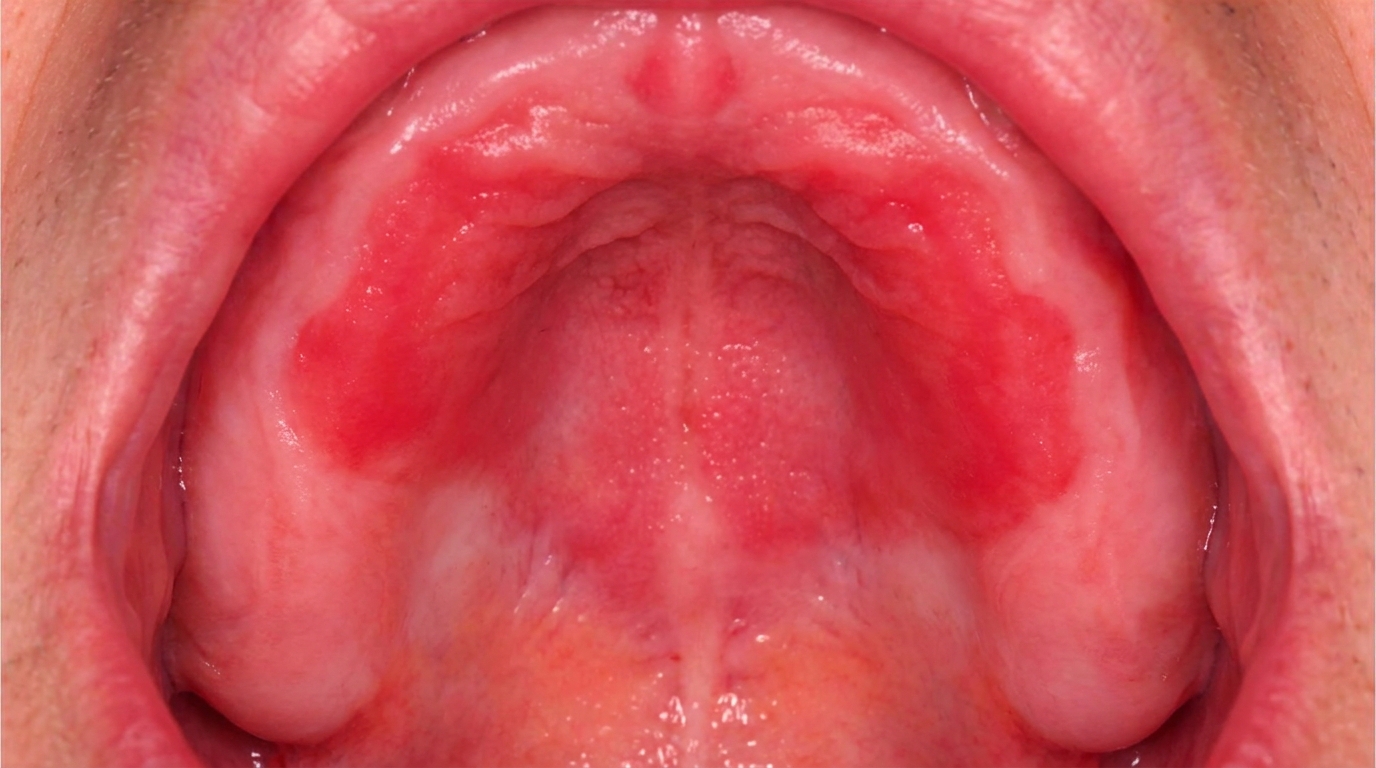
A bright red, velvety or pebbly area on the roof of the mouth that exactly matches the outline of an upper denture, sometimes with tiny pinpoint bleeding spots. This is denture stomatitis.
Red, cracked, sore corners of the mouth (angular cheilitis), which often appears alongside any of the above.
What it feels like
Symptoms vary a lot. Acute antibiotic sore mouth is often genuinely uncomfortable, patients commonly describe a burning, scalded sensation, as though they had taken a sip of a hot drink. Eating spicy or acidic foods can sting. Dry mouth makes everything worse.
Denture stomatitis, by contrast, is usually painless. Most people only discover it when their dentist points it out at a check-up. Median rhomboid glossitis is also typically symptomless.
Reduced taste, a foul or metallic taste, and a vague soreness are all reported. In more severe cases, particularly with a weakened immune system, the soreness may extend back into the throat and make swallowing uncomfortable.
What an X-ray might show
Erythematous candidiasis is a soft-tissue condition. It does not show up on dental X-rays.
What happens at the dentist?
The diagnosis is usually made on appearance, history, and a careful look for the predisposing factors that drive it.
Your dentist at ArtSmiles will typically:
Ask about recent antibiotics, inhaler use, dry mouth, denture wear and cleaning routine, smoking, and any medical conditions.
Examine the whole mouth, including under the dentures if they are worn, the corners of the mouth, the tongue, and the palate.
Sometimes take a swab or a smear from the affected area, which can be stained in the laboratory to confirm the presence of candidal hyphae.
Occasionally take a small biopsy if a red patch does not behave as expected, or if there is any concern about an alternative diagnosis.
Check for underlying causes that may need attention, ask about general health, recommend a blood test if anaemia, iron deficiency or undiagnosed diabetes is suspected, or suggest a medical review.
Refer to an oral medicine specialist if the lesion does not respond to standard treatment, recurs repeatedly, or there is a concern about immunity.
For denture-related cases, the dentist will also review the denture itself, its fit, its age, the cleaning routine, and whether it is being worn overnight.
Is this serious?
🟡 Worth a check-up. Erythematous candidiasis itself is not dangerous, and most cases settle once the predisposing factors are addressed. However, a persistent red patch in the mouth always deserves an assessment, because other conditions can look similar and a few of them are more serious.
Left untreated, the infection can be quite uncomfortable, can affect taste and appetite, and can spread back into the throat or oesophagus, particularly in people who are unwell, frail, or immunocompromised. In adults whose immunity is significantly reduced, oral candidiasis can be a marker of an underlying medical problem that needs investigation.
In an otherwise healthy adult who has not had antibiotics, steroid inhalers or dentures, persistent erythematous candidiasis is unusual enough that it warrants a closer look at general health.
If you've noticed a red, sore patch in your mouth for more than two weeks, or your denture-bearing palate is bright red, it's worth booking an assessment.
Could it be something else?
Several other conditions can produce red, sore areas of mouth lining. Your dentist will work through these by combining the clinical appearance, the history, and sometimes a smear or biopsy.
Pseudomembranous candidiasis (thrush), caused by the same yeast, but with creamy white plaques that wipe off to reveal a red surface. The two forms can coexist or follow on from each other.
Geographic tongue (benign migratory glossitis), produces red patches on the tongue, but with raised pale rims and a pattern that changes over days or weeks. Geographic tongue moves; candidiasis stays put.
Anaemic glossitis, iron, folate or vitamin B12 deficiency can leave the tongue red, smooth and sore, and can look identical to acute antibiotic sore mouth. A blood test settles the question.
Burning mouth syndrome, produces a similar scalded sensation, but the mouth looks normal on examination, with no red patch to match the symptoms.
Erosive lichen planus, gives painful red and white striped or eroded areas, usually on the cheeks. The white lacy pattern at the edges and the chronic course distinguish it.
Discoid or systemic lupus erythematosus (an autoimmune condition that can affect skin and many organs), can cause red atrophic patches, usually with a more delicate radiating white border. Other body sites are typically involved as well.
Allergic contact stomatitis, a localised allergic reaction, particularly to denture base material, food flavourings or oral hygiene products. The redness matches the area in contact with the trigger and improves once that trigger is removed.
Erythroplakia (a true red patch), a velvety red lesion that may not be painful but can be premalignant. It does not respond to antifungals, which is one reason a non-resolving red patch should always be reviewed.
Sjögren syndrome,related mucositis, the mouth becomes red and the tongue acquires a cobblestone texture due to severe dry mouth, often with overlying candidal infection.
Mucous patches of secondary syphilis, can produce red, sometimes ulcerated patches, but with very different blood-test findings.
Median rhomboid glossitis versus a tongue tumour, a nodular form of median rhomboid glossitis can occasionally be mistaken for a growth, which is one reason biopsy is sometimes considered for atypical cases.
Oral hairy leukoplakia (corrugated white tongue patches associated with HIV), a vertically corrugated white lesion on the side of the tongue in HIV-positive patients, which looks different from erythematous candidiasis but can occur in the same patient group.
How is it treated?
Treatment has two parts: clearing the yeast, and addressing whatever let it overgrow in the first place. Without the second part, the infection tends to come back.
Things you can do at home
Rinse the mouth thoroughly with water after every puff of a steroid inhaler, using a spacer device also helps.
Take dentures out at night, every night. Clean them mechanically with a denture brush, then soak overnight in dilute chlorhexidine or a denture-soaking solution. The textbooks specifically mention soaking in dilute hypochlorite or chlorhexidine to clear yeast from the porous denture base.
Stay well hydrated and address dry mouth where possible, sugar-free gum, frequent sips of water, and saliva substitutes can help.
If you smoke, cutting down or quitting helps the mouth lining recover.
Keep on top of general oral hygiene with regular brushing and interdental cleaning.
Professional treatment may include
Topical antifungal medication, most cases respond to a topical antifungal applied to the affected area. Nystatin oral suspension, miconazole gel, and amphotericin lozenges are all commonly used. Treatment usually continues for at least one week beyond the disappearance of clinical signs.
Adjustments to the denture or the way it is used, refitting, relining, or replacing a worn denture; advice on cleaning; and stopping night-time wear are all standard parts of denture stomatitis management.
Treating angular cheilitis at the same time, usually with a topical antifungal cream applied to the corners of the mouth, sometimes combined with an antibacterial if Staphylococcus aureus is also involved.
Reviewing antibiotic or inhaler use, your prescribing doctor may consider whether a narrower-spectrum antibiotic would do, or check inhaler technique.
Systemic antifungal medication, for resistant or extensive cases, or when topical treatment cannot reach the lesion, oral antifungal tablets such as fluconazole or itraconazole may be prescribed. These have more potential side effects and drug interactions, and are usually reserved for cases that don't respond to topical care.
Investigating underlying causes, blood tests for iron deficiency, B12 deficiency, or diabetes; review of medications; and, in selected cases, testing for HIV.
For most patients, treatment is straightforward and works well. The trickier part is keeping the infection from recurring, which is where the lifestyle and denture changes really matter.
What's the long-term outlook?
The outlook is generally very good. Acute erythematous candidiasis, including antibiotic sore mouth, typically clears within one to two weeks of starting topical treatment and removing the trigger. The textbooks describe the prognosis for acute and most chronic forms as excellent.
Denture stomatitis can recur if the denture-cleaning routine slips or the denture is worn overnight again, so long-term denture care really matters. Median rhomboid glossitis often improves in appearance with antifungal treatment but, because it includes a degree of fibrous scarring under the surface, the area may not look entirely normal again, what's important is that it stays stable and symptom-free.
For people with ongoing predisposing factors, long-term steroid inhalers, ongoing dry mouth, diabetes, or reduced immunity, the infection can come back, and many people benefit from periodic review and refresher advice on prevention.
In the small number of cases where erythematous candidiasis is the first sign of an underlying medical problem, identifying that problem early is genuinely useful. That's one of the reasons a persistent sore red mouth is always worth a professional opinion, even if it doesn't seem urgent.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
The cover image above is an AI-generated illustration based on the most common visible features of this condition described in clinical pathology references. It is not a photograph of a real case and should not be used to diagnose or rule out the condition in your own situation. If you are concerned about something you have noticed, please book an assessment with a registered dental practitioner.
References
Regezi, J. A., Sciubba, J. J., & Jordan, R. C. K. (2017). Oral pathology: Clinical pathologic correlations (7th ed.). Elsevier. Chapter 3, White Lesions: Candidiasis, pp. 104 to 108.
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2023). Oral and maxillofacial pathology (5th ed.). Elsevier. Chapter 6, Fungal and Protozoal Diseases: Erythematous Candidiasis and Denture Stomatitis, pp. 201 to 208; Chapter 7, Viral Infections: HIV-associated oral candidiasis, pp. 253 to 254.
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 12, Diseases of the Oral Mucosa: Candidosis, Denture-induced stomatitis, Acute antibiotic stomatitis and Erythematous candidosis, pp. 213 to 218; Chapter 14, Tongue Disorders: Median rhomboid glossitis, pp. 249 to 250.