Periodontal Surgery
(Gum Surgery)
Saving teeth that others might give up on.
Sometimes gum disease goes deeper than a cleaning can reach. When that happens, periodontal surgery gives us the access we need to clean away infection, repair bone damage, and give your teeth the best possible chance of staying with you for years to come.
What Is
Periodontal Surgery?
- Reduce deep periodontal pockets
- Remove infected tissue under direct vision
- Stabilise supporting bone
- Improve long-term tooth survival
When Periodontal Surgery May Be Recommended
- Persistent deep gum pockets after deep cleaning
- Ongoing bleeding or inflammation
- Progressive bone loss
- Gum recession affecting function or aesthetics
- Localised defects requiring regenerative procedures
Advanced Gum Disease and
General Health
- Cardiovascular disease
- Poorly controlled diabetes
- Respiratory conditions
At ArtSmiles, our clinical team follows a structured, risk-based periodontal protocol. Surgical treatment is recommended only after thorough diagnosis, imaging, and assessment of response to initial therapy. Our focus is preserving natural teeth wherever possible. Patients seeking gum disease treatment in Southport or gum surgery across the Gold Coast can book a comprehensive periodontal assessment to determine whether intervention is indicated.
Book Your Periodontal Surgery Assessment
Share your details and our team will be in touch within 1 business day to confirm your appointment.
Prefer to call? Reach us on (07) 5588 3677
The Treatment
Process
Every case follows a structured pathway from diagnosis through to long-term maintenance. Surgery is only considered after non-surgical options have been fully explored.
Comprehensive Assessment
We evaluate pocket depths, bleeding points, bone levels, and systemic risk factors to determine the severity of disease and the most appropriate treatment pathway.
- —Full periodontal charting
- —CBCT and radiographic bone analysis
- —Bleeding index scoring
- —Systemic risk factor review
 Step 01 · ArtSmiles
Step 01 · ArtSmilesReady to take the next step?
Book a consultation to discuss your personalised plan.
Periodontal Surgery vs
Deep Cleaning
Key Differences
- Surgery provides direct visual access to root surfaces
- Bone defects can be reshaped or regenerated surgically
- Sutures are placed to support healing after surgery
- Recovery time is longer than non-surgical treatment
How to Know When
Surgery Is Needed
 Routine Clean
Routine CleanHealthy
No inflammation, no bleeding, no pocket depth beyond normal. Maintained with regular check-ups and professional cleaning.
 Routine Clean
Routine CleanGingivitis
Reversible gum inflammation with redness and bleeding. No bone loss yet. Early intervention prevents progression.
 Deep Cleaning
Deep CleaningEarly Periodontitis
Mild bone loss begins. Pockets deepen beyond 4 mm. Deep cleaning is highly effective at halting progression.
 Deep Cleaning
Deep CleaningModerate Periodontitis
Deeper pockets, increased mobility risk, and visible bone loss. Non-surgical therapy remains the first-line approach.
 Surgery
SurgeryAdvanced Periodontitis
Extensive structural damage and potential tooth instability. Surgical intervention is typically required at this stage.
Stages 1 and 2 are managed with routine check-ups and professional cleaning. Stages 3 and 4 respond well to deep cleaning (scaling and root planing). Stage 5 typically requires periodontal surgery.
Recovery &
Healing
- Swelling
- Bruising
- Mild to moderate discomfort
- Temporary difficulty chewing
- Minor bleeding
Without structured follow-up, the condition can recur. Long-term outcomes depend on patient compliance, regular periodontal maintenance, and control of systemic risk factors such as smoking and diabetes.
Worried About Losing Your Teeth?
Advanced gum disease doesn’t have to mean tooth loss. Book an assessment and let us show you what can be done to save and protect your smile.
Ready to get started?
Prefer to call? (07) 5588 3677
Periodontal Surgery
Cost Guide
The cost of gum surgery depends on the number of areas treated, type of procedure performed, extent of bone involvement, use of graft materials, and surgical time required. A full periodontal assessment is required before confirming suitability and treatment planning.
- —Number of areas treated
- —Type of procedure performed
- —Extent of bone involvement
- —Use of graft materials
- —Surgical time required
Final pricing confirmed after clinical assessment and treatment planning.
Book a ConsultationPreventive care membership with check-ups, cleans, and savings on treatments. Priority scheduling included.
Flexible Payment Options
We understand that dental treatment is a significant decision. Flexible finance solutions and staged planning options are available. For more information, please visit our dedicated Finance page. For eligible patients facing hardship, structured access may be available under our Blessing Program.
Understand Your
Oral Health Risk
Our risk assessment takes less than two minutes and helps us identify potential vulnerabilities before they compromise your treatment. The results allow our team to build a personalised prevention plan alongside your care.
- —Decay risk, dietary habits, saliva quality, and bacterial balance
- —Gum disease risk, inflammation patterns, bone support, and hygiene effectiveness
- —Grinding & clenching risk, bite forces, wear signs, and jaw tension
Start Your Assessment
Takes less than 2 minutes. No obligation.
Risks and
Clinical Considerations
Potential Risks Include
Post-Operative Swelling
Swelling of the gums and surrounding tissue is expected after surgery and typically peaks within 48 hours. Cold compresses and prescribed medication help manage this during recovery.
Tooth Sensitivity
Temporary sensitivity to temperature changes is common as healing progresses and root surfaces may be exposed. This usually resolves within weeks as tissue matures.
Gum Recession
As surgical sites heal and inflammation resolves, some degree of gum recession may occur. This is particularly relevant in areas of pre-existing bone loss.
Delayed Wound Healing
In some cases, surgical sites may take longer to close, particularly in patients who smoke, have diabetes, or take certain medications that affect healing.
Incomplete Regeneration
Bone grafting and guided tissue regeneration procedures do not guarantee full regeneration. Outcomes depend on defect type, patient health, and post-operative compliance.
Infection
Post-surgical infection is uncommon but possible. Prescribed antibiotics, careful wound care, and structured follow-up visits help minimise this risk.
Related Articles
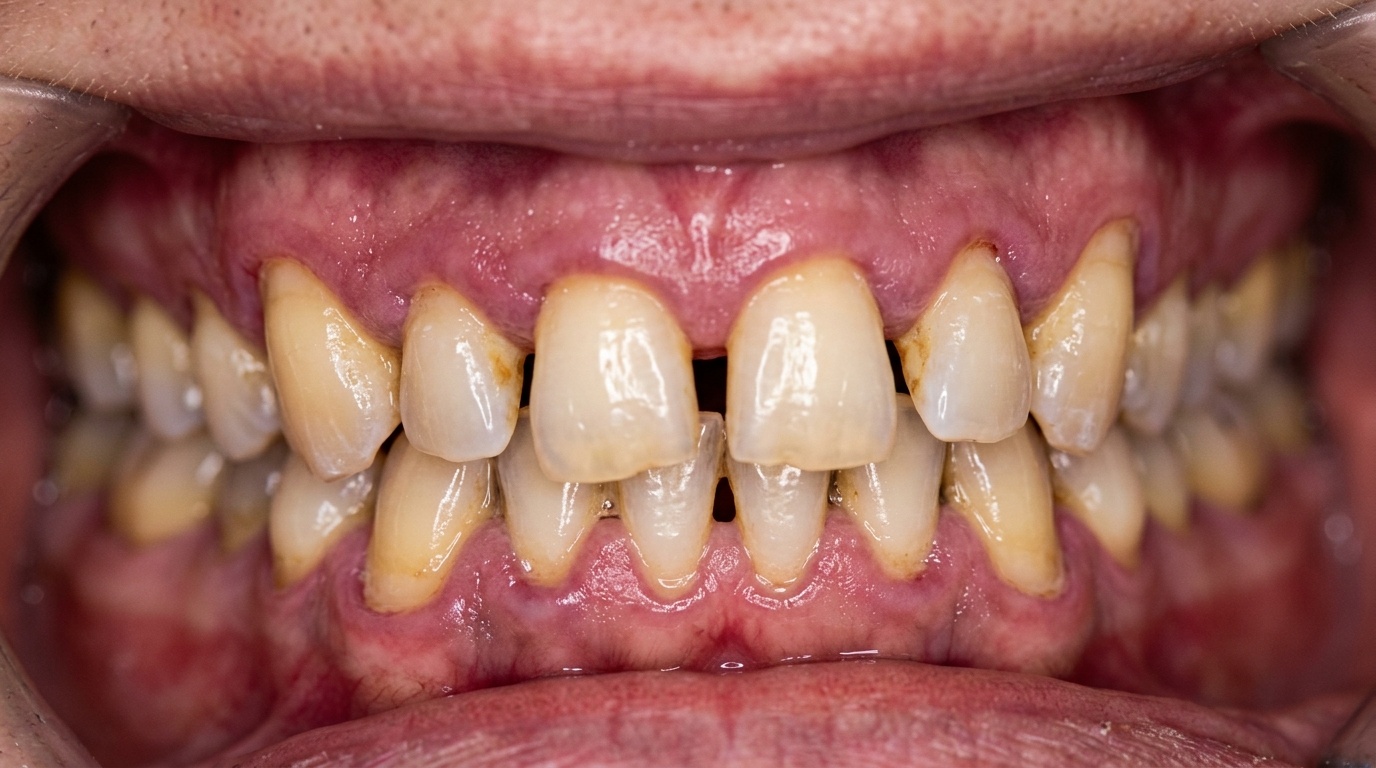
Noticing Your Teeth Moving? Here's Why It Happens as We Age
Updated 25 April 2026

Post-Operative Instructions for Periodontal Flap Surgery
Updated 25 April 2026
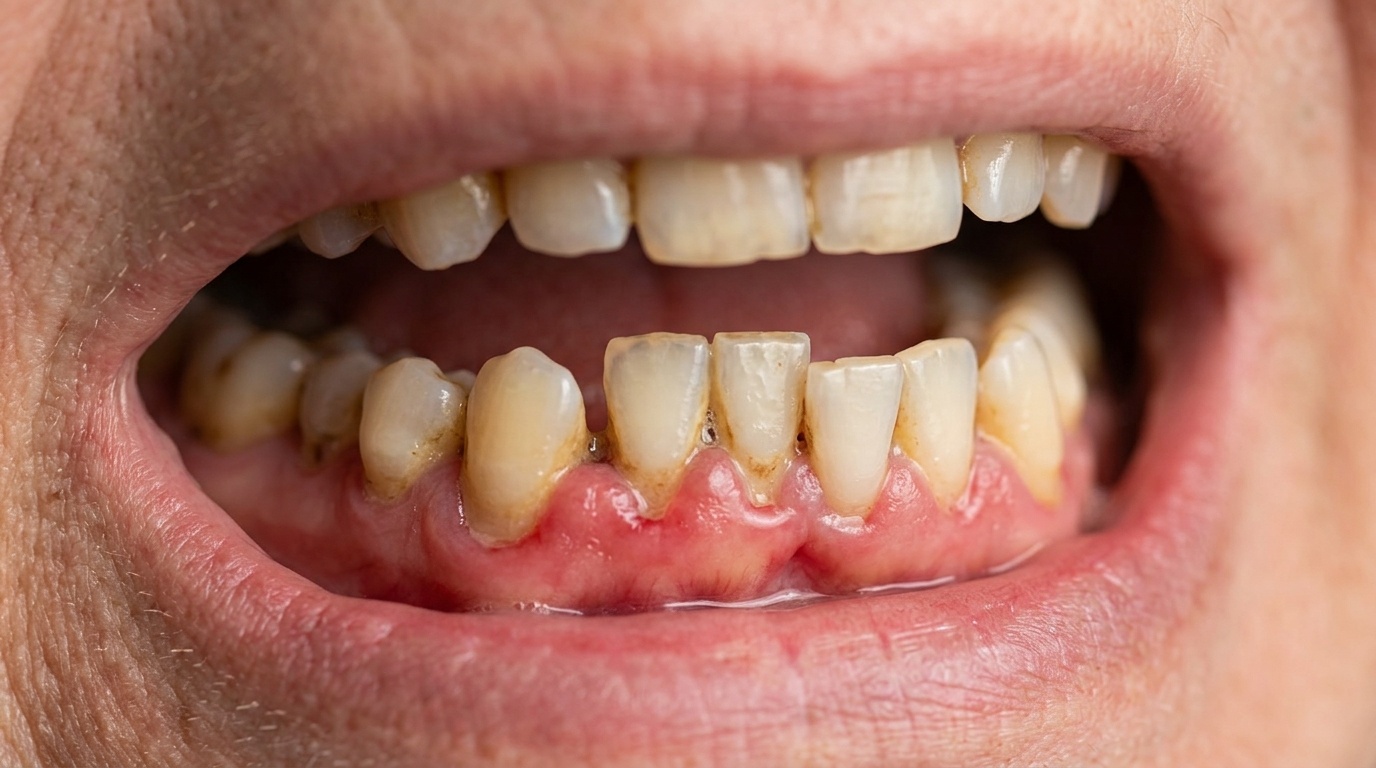
Loose Teeth: Why It Happens and When You Should Worry
Updated 19 April 2026
Frequently Asked
Questions
What is periodontal surgery?
Also called gum surgery, it is a surgical approach to treating advanced gum disease when non-surgical methods have not achieved sufficient pocket reduction. The procedure gives the clinician direct access to root surfaces and bone for thorough decontamination.
Is periodontal surgery painful?
Local anaesthetic is used throughout, so the procedure itself should be comfortable. Afterward, mild to moderate discomfort, swelling, and tenderness are common and typically well-managed with prescribed medication and cold compresses.
What types of gum surgery are available?
Options include flap surgery (open debridement) for deep pocket access, osseous recontouring for irregular bone, regenerative procedures using bone grafts and GTR membranes, and soft tissue grafting for gum recession. The choice depends on each patient's clinical presentation.
Can gum surgery reverse bone loss?
In favourable defect patterns, regenerative techniques can partially restore lost bone. However, not all damage is reversible. The primary objective is halting further progression and creating a stable, maintainable environment.
What are the risks of gum surgery?
All surgical procedures carry some risk. Potential complications include swelling, bruising, short-term sensitivity, tissue recession during healing, and rare instances of infection or incomplete graft integration. Risks are discussed in detail before any procedure.
When is surgery recommended over deep cleaning?
Surgery is considered when deep cleaning alone cannot reduce pockets to a manageable depth, when bone defects are too complex for non-surgical access, or when regenerative treatment is clinically appropriate.
How do smoking and diabetes affect outcomes?
Both are significant risk factors. Smoking impairs blood flow and slows wound healing. Poorly controlled diabetes increases infection risk and delays tissue repair. Addressing these factors before and after surgery improves predictability.
What aftercare is needed following gum surgery?
Careful oral hygiene, a soft diet for the first week, prescribed medication, and attending all scheduled follow-up appointments. Long-term, periodontal maintenance every 3 to 6 months is essential to protect surgical outcomes.
How much does gum surgery cost?
Fees vary based on the number of sites treated, the type of procedure, whether bone graft or regenerative materials are used, and the surgical time involved. A detailed periodontal assessment is required before providing a treatment plan and cost estimate.
Can gum recession be treated with surgery?
Yes. Soft tissue grafting can cover exposed roots, reduce sensitivity, and restore gum contour in cases of recession. The technique and expected outcome depend on the extent of recession and the quality of surrounding tissue.
Why would I need gum surgery?
It may be recommended if pockets remain deep after scaling and root planing, if infection continues despite initial therapy, or if bone defects require reshaping or regeneration to improve long-term prognosis.
How long does periodontal surgery take?
A single area is usually completed within 60 to 120 minutes. If multiple sites require treatment, procedures may be staged across separate appointments to allow adequate healing between sessions.
What is regenerative periodontal surgery?
It involves placing bone graft materials, barrier membranes, or biologic growth factors into selected bone defects to encourage new tissue formation. Success depends on defect shape, oral hygiene, and systemic health.
What is the recovery time after gum surgery?
Soft tissue healing typically occurs within 1 to 2 weeks, during which a modified diet and gentle oral hygiene are recommended. Full tissue maturation and bone integration (in graft cases) may take 3 to 6 months.
Will my gums grow back after surgery?
Swollen, inflamed tissue will tighten as healing occurs, which may make teeth appear longer. This is a normal sign that infection is resolving. Where gum grafting is performed, tissue coverage can improve over time.
Can antibiotics replace gum surgery?
No. Antibiotics cannot remove hardened deposits or reshape bone. They may be prescribed alongside surgical treatment to support healing, but they are not a substitute for mechanical debridement.
Do I need to see a periodontist for gum surgery?
Depending on case complexity, treatment may be provided by a dentist with advanced periodontal training or by a specialist periodontist. At ArtSmiles, our team assesses each case individually and refers to a periodontist when appropriate.
What happens if I delay treatment?
Untreated advanced gum disease can lead to progressive structural damage, increased tooth mobility, complications around existing dental work, and eventual tooth loss. Earlier intervention typically results in simpler, more predictable treatment.
How much does a dental bone graft cost in Australia?
Bone graft costs depend on the type of graft material used, the size of the defect, and whether guided tissue regeneration membranes are required. A clinical examination and imaging are needed to determine suitability and provide an accurate estimate.
Still have questions?
Our team is here to help. Book a consultation to discuss your options.
Our Other Periodontal
Services
This page has been clinically reviewed by Dr. Cristian Dunker, BDSc, MBA, Principal Dentist at ArtSmiles.

