Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker , Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | Candidal leukoplakia, chronic hyperplastic candidosis |
How urgent? | 🟡 Worth checking, usually painless but persistent; biopsy is needed to distinguish it from other white patches and to assess for any associated dysplasia (microscopic changes that can signal an increased cancer risk) |
Common or rare? | Less common than other forms of oral candidiasis but well recognised |
Who it affects | Most often middle-aged or older adults, particularly men, with smoking, denture wear, dry mouth or iron deficiency as common contributors |
Who treats it | General dentist for diagnosis, biopsy and antifungal therapy, sometimes in coordination with an oral medicine specialist |
Based on | Cawson, Neville, with cross-references in Regezi |
What is it?
Chronic hyperplastic candidiasis is a long-standing form of Candida infection of the mouth that produces a tough, adherent white patch rather than the wipeable creamy plaque seen in ordinary thrush. The textbooks describe it as the form of candidiasis that is hardest to distinguish from a true oral leukoplakia, in fact, the older term "candidal leukoplakia" reflects exactly that overlap. Diagnosis depends on biopsy showing fungal hyphae (long branching threads of the yeast) growing within the keratin of the epithelium, and treatment is based on antifungal therapy plus addressing the underlying factors that allowed the infection to take hold.
Who tends to get it?
The textbooks describe a fairly recognisable clinical group:
Adults of middle age or older, with men slightly more often affected than women.
People who smoke, by far the most common single contributing factor.
People who wear dentures, particularly when the denture is worn at night or is poorly cleaned.
People with dry mouth (xerostomia), dry mouth, whether from medications, salivary gland disease or radiotherapy.
People with iron deficiency anaemia, B12 or folate deficiency.
People with diabetes mellitus, particularly when poorly controlled.
People taking inhaled corticosteroids (such as preventer inhalers for asthma) without rinsing the mouth afterwards.
People with weakened immunity, including HIV infection, organ transplant recipients, and patients on long-term systemic corticosteroids or chemotherapy.
Rarely, young patients with chronic mucocutaneous candidiasis, a rare immune disorder that produces persistent skin, nail and mouth candidiasis from early life.
What causes it?
The cause is well established:
Persistent infection by Candida albicans (or, less commonly, related Candida species) in the surface of the mouth.
A combination of host and local factors that allow the infection to take hold and remain. These include:
Smoking, alters the surface of the mucosa and impairs local immunity.
Denture wear, provides a sheltered, often dry environment under the denture for yeast to multiply.
Reduced saliva flow, saliva normally flushes out and limits Candida.
Nutritional deficiencies, particularly iron, B12 and folate.
Endocrine conditions, diabetes mellitus, hypothyroidism, hypoparathyroidism.
Immunosuppression, local (inhaled steroids) or systemic (HIV, transplant medications, chemotherapy).
The textbooks discuss whether Candida itself drives the white patch or simply colonises a pre-existing leukoplakia. Both situations occur in practice. What matters clinically is that confirming Candida and treating it often improves or fully clears the patch.
How does it develop?
The yeast invades the surface keratin of the mouth's lining, growing as long branching threads (hyphae) that extend into the upper layers of the epithelium. The textbooks describe these hyphae as embedded in the parakeratin (the upper protective layer of mouth lining) and rarely penetrating into the deeper, viable cell layers unless the patient is severely immunocompromised (with a weakened immune system). The host responds with thickening of the keratin layer (hyperkeratosis), thickened keratin layer, elongation of the deeper rete ridges (the finger-like projections of surface tissue into the underlying connective tissue), and a chronic inflammatory infiltrate beneath. In some patients there is also dysplasia, abnormal cell change that signals the lesion may carry an extra cancer risk over time. The patch appears clinically as a tough, white plaque that does not wipe off, although fragments can sometimes be detached with firm scraping.
What might you notice?
What it looks like
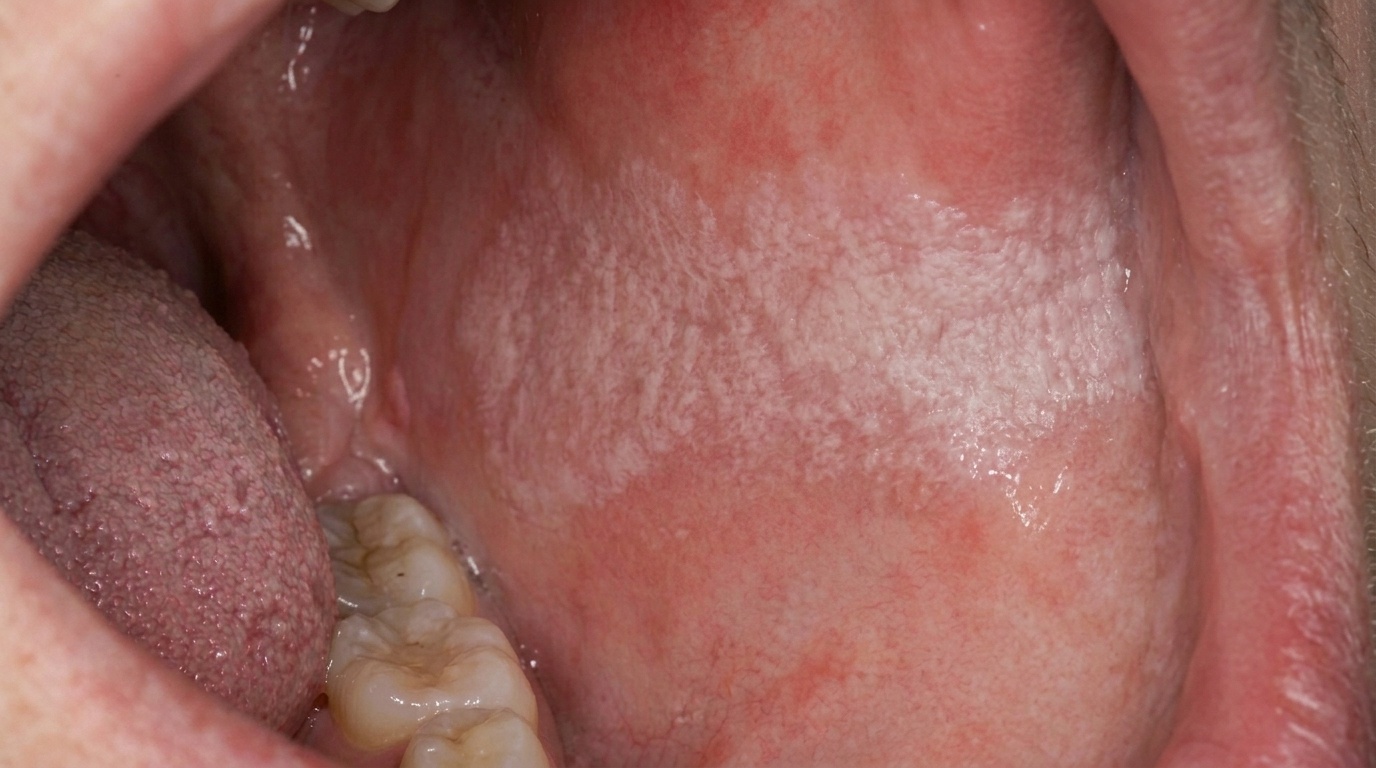
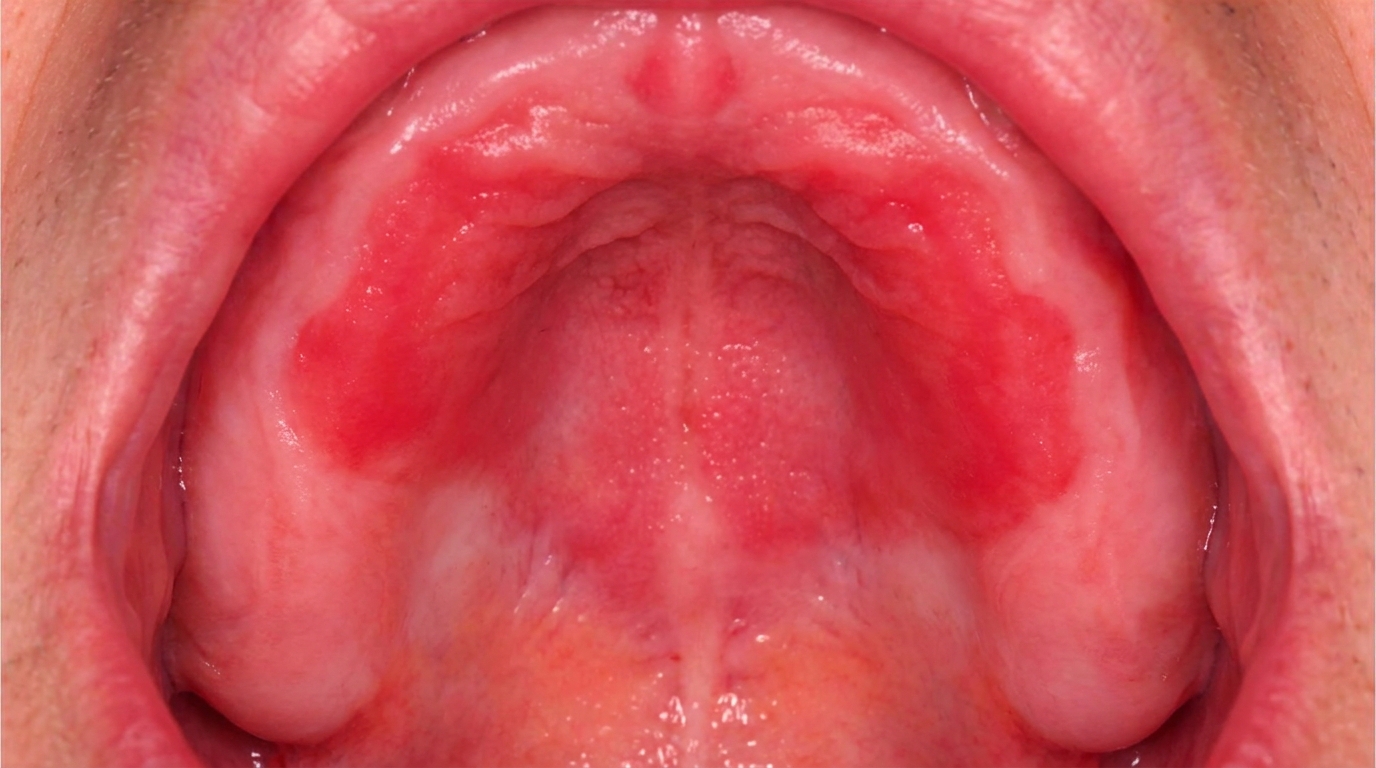
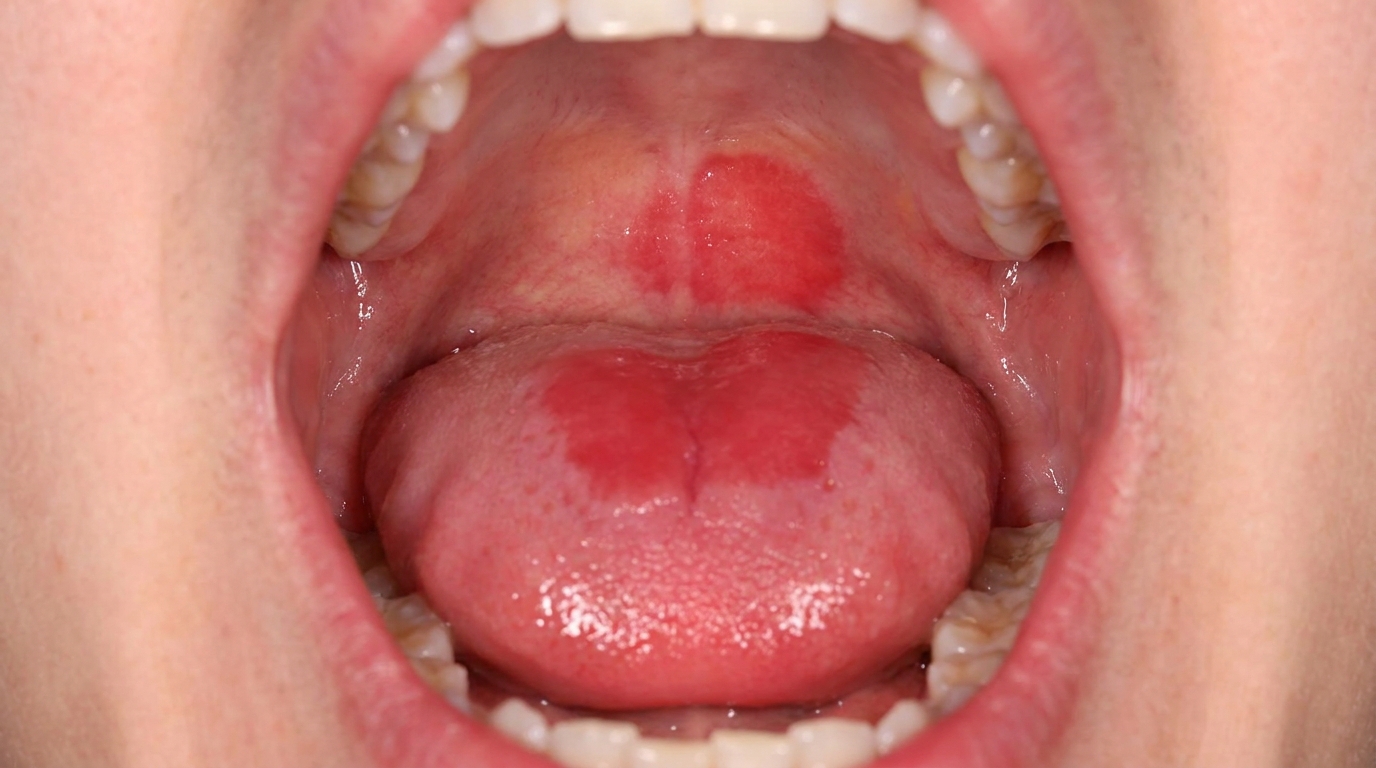
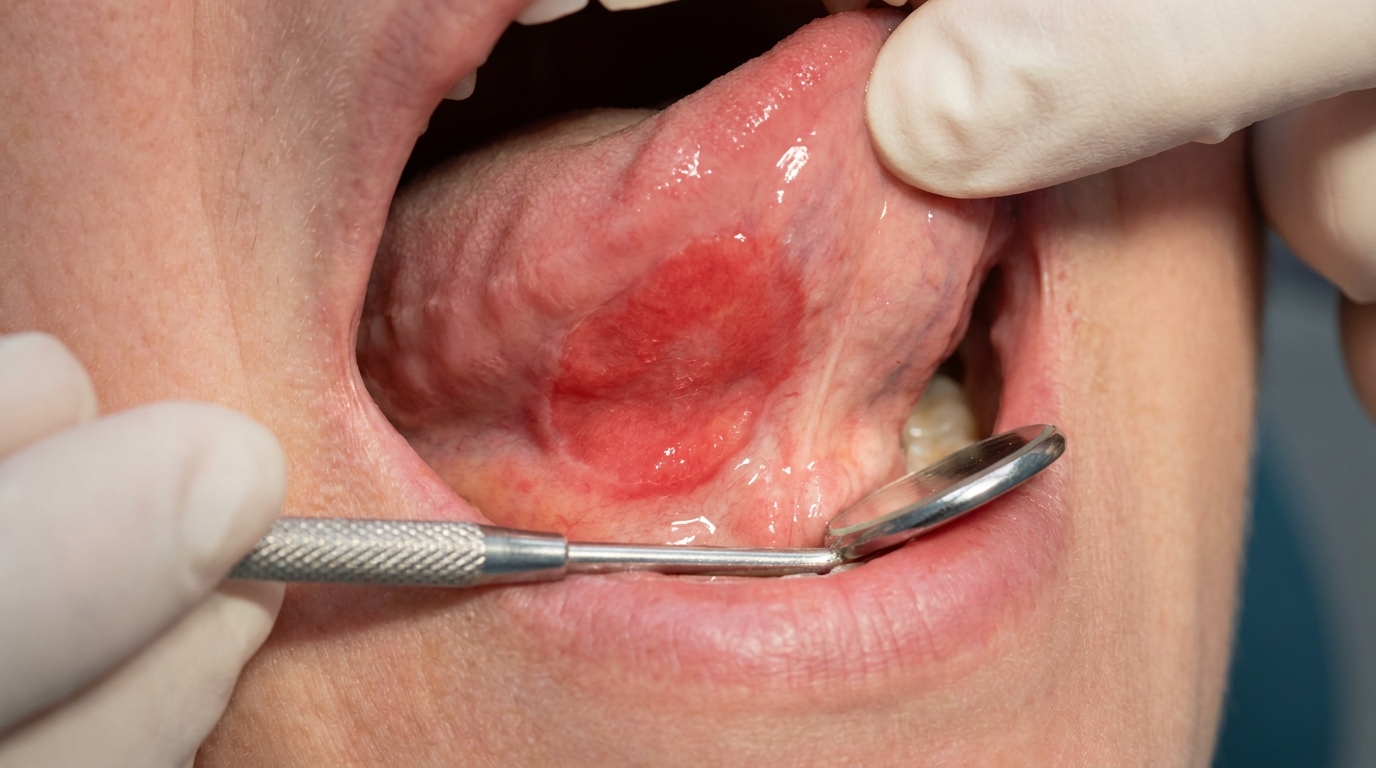
The classic appearance has several recognisable features:
A white plaque that is tough and adherent, does not rub off with gauze.
The surface is often irregular, rough or slightly nodular.
Sometimes a mixed red-and-white (speckled) appearance, areas of redness within the white patch. These speckled lesions carry a higher risk of dysplasia.
The most common sites are the inside of the cheeks just behind the corners of the mouth (the post-commissural buccal mucosa) and the upper surface of the tongue.
Angular cheilitis, soreness and cracking at the corners of the mouth, may be present at the same time and is often a useful clue toward Candida.
What it feels like
Most chronic hyperplastic candidiasis patches are mildly symptomatic at most. When symptoms occur they may include:
A mild burning or soreness, particularly with hot or spicy foods.
A rough sensation felt with the tongue.
An altered taste in some patients.
Cracking or soreness at the corners of the mouth if angular cheilitis is associated.
Severe pain, ulceration or rapid change in size are not typical of chronic hyperplastic candidiasis and should prompt urgent reassessment.
What an X-ray might show
X-rays are not used to diagnose chronic hyperplastic candidiasis, the diagnosis depends on clinical examination plus biopsy and microbiology.
What happens at the dentist?
A persistent white patch always warrants careful assessment. A dentist at ArtSmiles, typically as part of a dental check-up and clean, will commonly:
Examine the patch carefully, note its location, surface, edges, and whether it wipes off.
Take a careful history of smoking, denture wear, inhaler use, recent illnesses, medications, dry mouth, and any nutritional or endocrine conditions.
Perform a fungal swab or smear to confirm the presence of Candida.
Take a biopsy from the patch, since this is the only reliable way to distinguish chronic hyperplastic candidiasis from idiopathic oral leukoplakia and to assess for dysplasia.
Investigate underlying factors, including blood tests for iron, B12, folate and blood glucose where appropriate, often through your GP.
Assess and clean any denture that may be harbouring Candida, including checking the fit and the patient's denture-cleaning routine.
Refer to an oral medicine specialist for cases that do not respond to first-line treatment, where dysplasia is identified, or where the patient has more complex underlying conditions.
Is this serious?
🟡 Chronic hyperplastic candidiasis is benign in most cases and clears with combined antifungal and supportive treatment. However, the textbooks all stress that there is a small but real risk of malignant change, particularly in speckled lesions and those with dysplasia on biopsy. The exact level of risk is debated and probably lower than for ordinary leukoplakia, but it is not zero. For this reason, biopsy at diagnosis and follow-up after treatment matter.
If you have a tough white patch in the mouth that has been present for two to three weeks and does not wipe off, particularly if it is in the cheek near the corner of the mouth, on the tongue or under a denture, it is worth booking an assessment so the right tests can be arranged.
Could it be something else?
Several conditions can produce a similar tough white patch in the mouth. The textbooks list these as the main differentials:
Idiopathic oral leukoplakia, a white patch with no specific cause, distinguished from chronic hyperplastic candidiasis on biopsy and by the absence of fungal hyphae.
Pseudomembranous oral candidiasis (thrush), a creamy-white plaque that wipes off, leaving red mucosa underneath.
Hairy leukoplakia, a corrugated white patch on the side of the tongue caused by Epstein-Barr virus, usually in the context of immunosuppression.
Frictional hyperkeratosis, a white thickening from chronic biting, rubbing or denture pressure that resolves when the cause is removed.
Oral lichen planus, typically has fine white lacy lines (Wickham striae), usually symmetrical and on both cheeks.
Speckled (non-homogeneous) leukoplakia or erythroplakia, high-risk lesions distinguished on biopsy.
Squamous cell carcinoma in situ or invasive cancer, biopsy is essential to rule out malignancy in any non-healing white patch.
How is it treated?
Treatment is based on confirming the diagnosis, treating the Candida, and addressing the factors that allowed the infection to persist.
At-home measures and habits:
Stop smoking. This is the single most important step.
Clean dentures thoroughly every day, brushing both the fitting surface and the remaining teeth. Soak the denture overnight in a chlorhexidine solution or denture cleaner, and ideally do not wear the denture overnight.
Address dry mouth, sip water often, use saliva substitutes if needed, and review any medications with your GP that may be contributing.
Rinse the mouth with water after using inhalers, particularly preventer inhalers containing corticosteroids.
Eat a balanced diet to limit deficiencies of iron, B12 or folate.
Manage diabetes carefully if you have it.
Professional steps your dentist may consider:
Biopsy of the patch to confirm chronic hyperplastic candidiasis and assess for any dysplasia.
Systemic antifungal therapy, typically fluconazole, often for several weeks to a few months. The textbooks specifically note that prolonged courses are sometimes needed, with the understanding that long-term antifungal use carries a small risk of resistance.
Topical antifungal therapy, clotrimazole troches, nystatin oral suspension or miconazole gel, especially for milder cases or as adjunctive treatment.
Treating angular cheilitis if present, often with a combined antifungal-corticosteroid cream.
Addressing iron, B12 or folate deficiency through your GP.
Reassessment after treatment, the textbooks specifically note that surgical excision alone is "of little value", since the infection often recurs in the same site. The aim is to clear the Candida and the predisposing factors.
Long-term review, particularly when dysplasia has been documented, with re-biopsy of any persistent white change.
A patient-centred approach matters here too. Many patients are surprised that a "white patch" can be infectious, and clear explanation of what is being treated, why long courses of antifungal are sometimes needed, and what changes in habit will help the most is itself part of effective care, values that sit at the heart of our clinical philosophy.
What's the long-term outlook?
The outlook is generally good when the diagnosis is made and the predisposing factors are addressed. Many lesions clear completely with antifungal therapy and removal of contributing factors. Some require long-term intermittent antifungal treatment because the infection tends to recur. Lesions that persist after treatment, or that show dysplasia on biopsy, warrant ongoing review and re-biopsy. Across all cases, the most important factor in a good outcome is consistent dental review and consistent management of the patient's smoking, denture care and general health.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
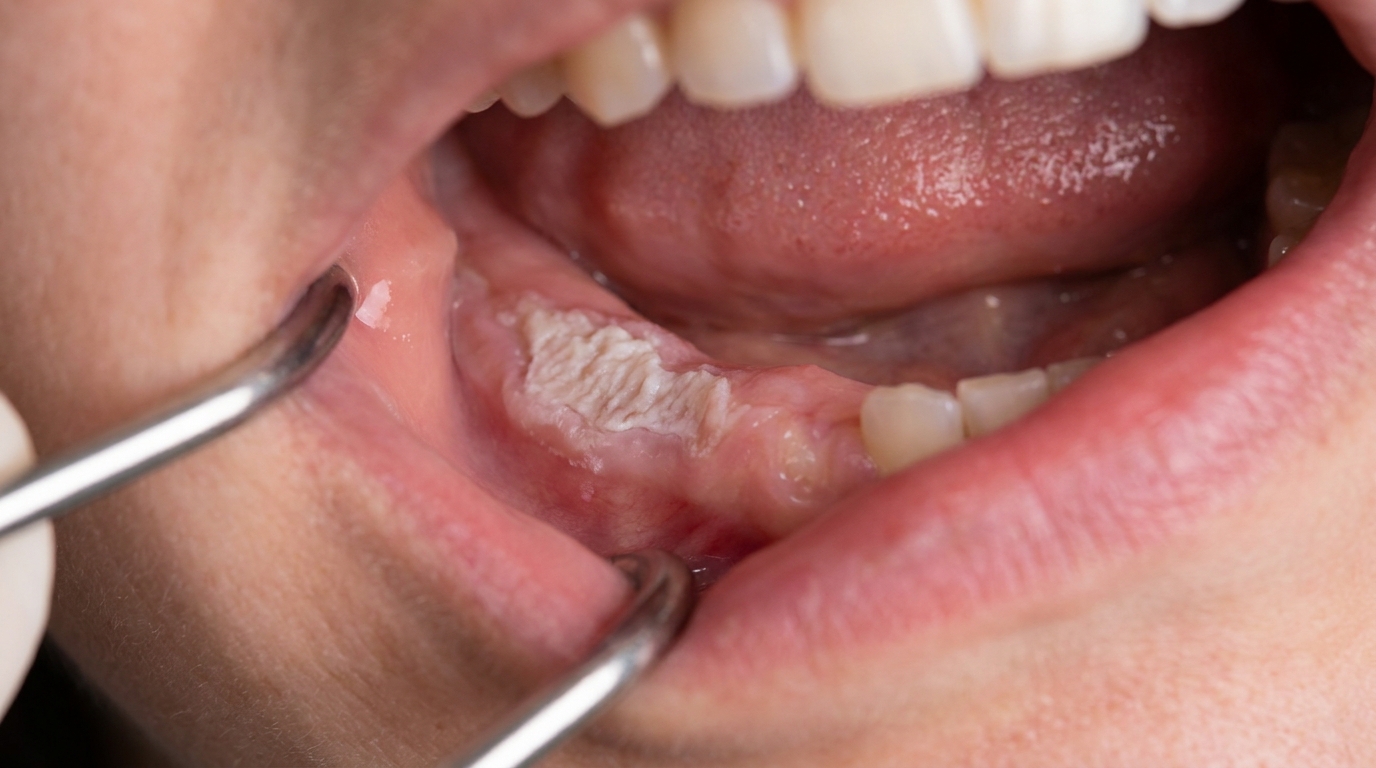
The cover image above is an AI-generated illustration based on the most common visible features of this condition described in clinical pathology references. It is not a photograph of a real case and should not be used to diagnose or rule out the condition in your own situation. If you are concerned about something you have noticed, please book an assessment with a registered dental practitioner.
References
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 16, Oral Premalignancy: Chronic Hyperplastic Candidosis (Candidal Leukoplakia), with treatment by systemic antifungal and management of contributing factors, pp. 267 to 268.
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2023). Oral and maxillofacial pathology (5th ed.). Elsevier. Chapter 6, Fungal and Protozoal Diseases: Chronic Hyperplastic Candidiasis (Candidal Leukoplakia), pp. 206 to 208.
Regezi, J. A., Sciubba, J. J., & Jordan, R. C. K. (2017). Oral pathology: Clinical pathologic correlations (7th ed.). Elsevier. Chapter 3, White Lesions: hyperplastic candidiasis as a key differential of leukoplakia.
Frequently asked questions
What is chronic hyperplastic candidiasis?
Chronic hyperplastic candidiasis is a long-standing infection of the mouth lining by Candida (a yeast), producing a thickened white patch that does not wipe off, most often at the corner of the cheek behind the corners of the mouth. Unlike the easily-wiped-off pseudomembranous form (thrush), this form is firmly attached and cannot be removed with gauze.
Is chronic hyperplastic candidiasis dangerous?
It deserves attention because the chronic Candida infection has a small but recognised potential to harbour or develop into dysplastic (pre-cancerous) changes within the patch. The lesion itself is not cancer, but it should be biopsied to assess the underlying tissue and to direct treatment. Smoking is a major risk factor and should be addressed.
How is it treated?
Treatment combines long-course topical antifungal medication (such as miconazole gel) and sometimes oral systemic antifungals, with strict control of contributing factors: smoking cessation, treatment of denture stomatitis, fixing ill-fitting dentures, and managing diabetes or iron deficiency where present. The lesion is followed and biopsied if it persists or changes.
Will it come back after treatment?
Recurrence is common if the underlying triggers (smoking, denture wear overnight, immune issues) are not addressed. Successful long-term control combines clearing the active infection, treating contributing factors and regular dental review every few months.