Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker , Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | Allergic contact stomatitis, stomatitis venenata, oral contact allergy, allergic gingivostomatitis |
How urgent? | 🟡 Worth a check-up, usually settles once the trigger is identified, but persistent burning or ulceration deserves an assessment |
Common or rare? | True allergic reactions are uncommon overall, but cinnamon-flavour and toothpaste reactions are encountered fairly regularly in practice |
Who it affects | Adults more than children; both sexes affected, with a slight female predominance reported in diagnosed cases |
Who treats it | General dentist usually identifies and manages it; allergist or oral medicine referral is helpful for stubborn cases |
Based on | Neville, Regezi, Cawson and Laskaris |
What is it?
Contact stomatitis is a reaction in your mouth that happens when the lining touches something it has become sensitive to, a flavouring in your toothpaste, an ingredient in chewing gum, a metal in a filling, or a chemical used in dentistry. The mouth lining (mucosa) goes red, sore, sometimes white and patchy, sometimes ulcerated, and the burning often eases off once the trigger is removed.
Think of it as your mouth's version of contact dermatitis on the skin, the same kind of immune reaction, just in a slightly more forgiving environment.
Who tends to get it?
Allergic contact stomatitis can affect both adults and children, but most diagnosed cases are in adults, with a noticeable female predominance in both the acute and chronic patterns. A large prospective study of more than 13,000 dental patients identified only seven acute and fifteen chronic cases of allergic reaction to dental materials, which gives some idea of how uncommon a true mucosal allergy is, even though the list of substances that could trigger one is long.
Certain patterns have their own demographics:
Cinnamon-flavour reactions can occur at any age, often in people who chew flavoured gum daily, use cinnamon-flavoured candy, or switch to a strongly flavoured toothpaste.
Lichenoid contact reactions to amalgam fillings tend to appear in adults with older, corroded restorations.
Plasma cell gingivitis (a related allergic gingival pattern) was famously linked to a chewing gum ingredient in the 1970s and is now seen sporadically with herbal toothpastes, mints, and certain cooking spices.
What causes it?
The oral mucosa is actually less sensitive than the skin, saliva dilutes allergens, the surface is constantly bathed and renewed, and contact times are usually short. So a true allergic reaction in the mouth needs both a sensitising substance and a person who has already become reactive to it.
The usual culprits include:
Toothpaste and mouthwash ingredients, cinnamon and mint flavours, anti-tartar additives, sodium lauryl sulphate, fluoride formulations, herbal extracts, and preservatives.
Cinnamon flavouring in gum, candy, breath mints, soft drinks and even dental floss. Concentrations in artificial cinnamon products can be up to a hundred times higher than the natural spice.
Dental restorative materials, amalgam (mercury, silver, tin, copper), nickel-containing alloys, gold, beryllium, chromium, cobalt and, less commonly, composite resins.
Acrylic denture base material, usually from residual unpolymerised methylmethacrylate monomer rather than the cured plastic itself.
Eugenol, used in temporary fillings, periodontal dressings and root canal sealers.
Topical medicaments and antiseptics, iodine, essential oils, topical antibiotics and steroids, aluminium chloride retraction cord.
Latex in gloves and rubber dam, especially in healthcare workers, atopic patients, and people with multiple childhood surgeries.
Foods and food additives, chocolates, cocoa, peanuts, dairy, eggs, citrus, monosodium glutamate, tartrazine and other colourings.
Atopic individuals (people who already have hay fever, asthma, eczema or other allergies) are more likely to develop a contact reaction to dental materials, but anyone can become sensitised over time.
How does it develop?
Most oral contact reactions are a type IV, or delayed, hypersensitivity reaction. That just means the immune system needs time to recognise the trigger and decides to over-react on the next exposure rather than the first.
Here's the everyday version: the first time your mouth meets the substance, say, a new cinnamon-flavoured gum, nothing happens, but a small population of immune cells quietly memorise it. The next time you chew that gum, those cells recognise the flavour molecule, send out chemical signals, and recruit a small army of lymphocytes (immune cells) to the lining where the gum sits. The result is the redness, swelling and burning you feel.
With dental amalgam, the corrosion process slowly releases tiny amounts of metal ions, which bind to surface proteins on the mouth's lining cells. The immune system can mistake this combination for a threat and launch a chronic, lichen-planus-like reaction directly under the filling.
What might you notice?
What it looks like
The appearance is genuinely variable, that's part of why it can be tricky to diagnose. Common patterns:
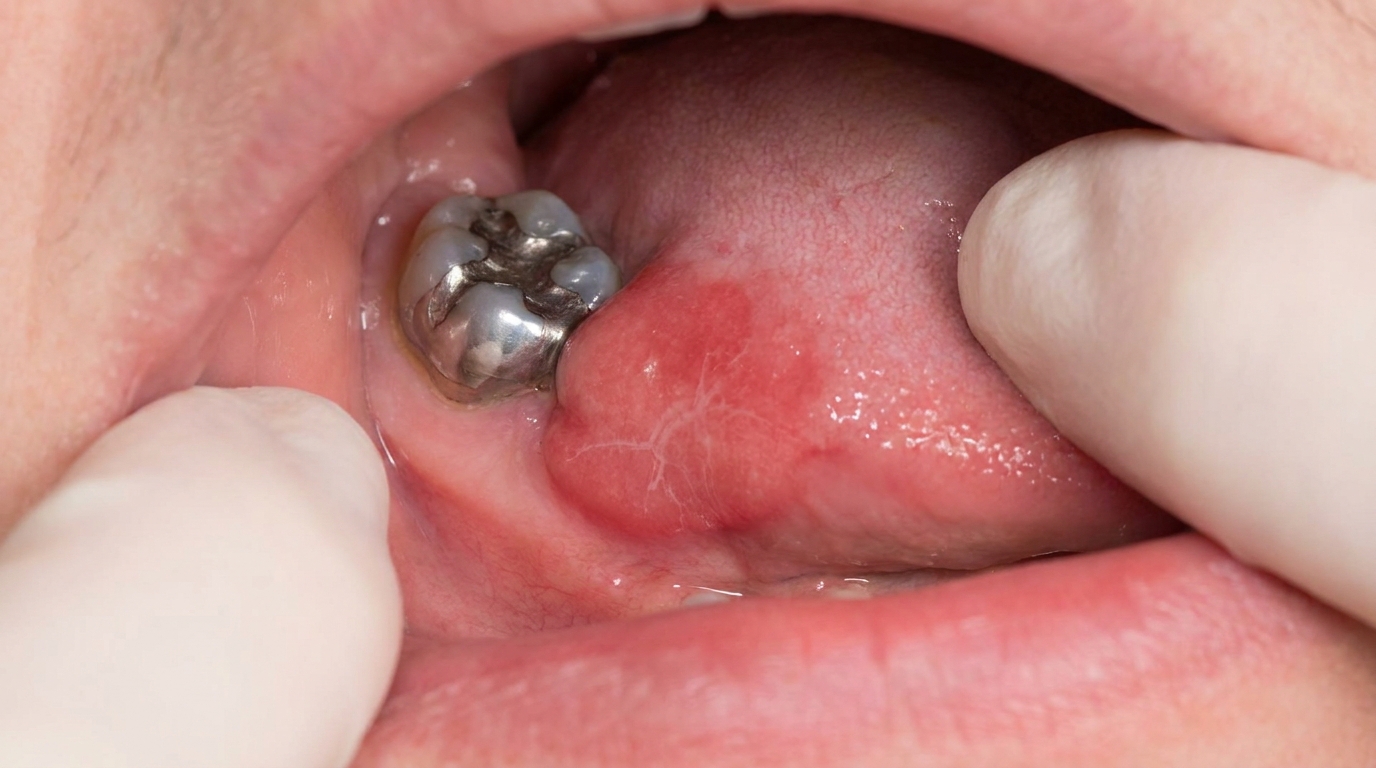
Bright red, glossy patches wherever the substance touches the mucosa.
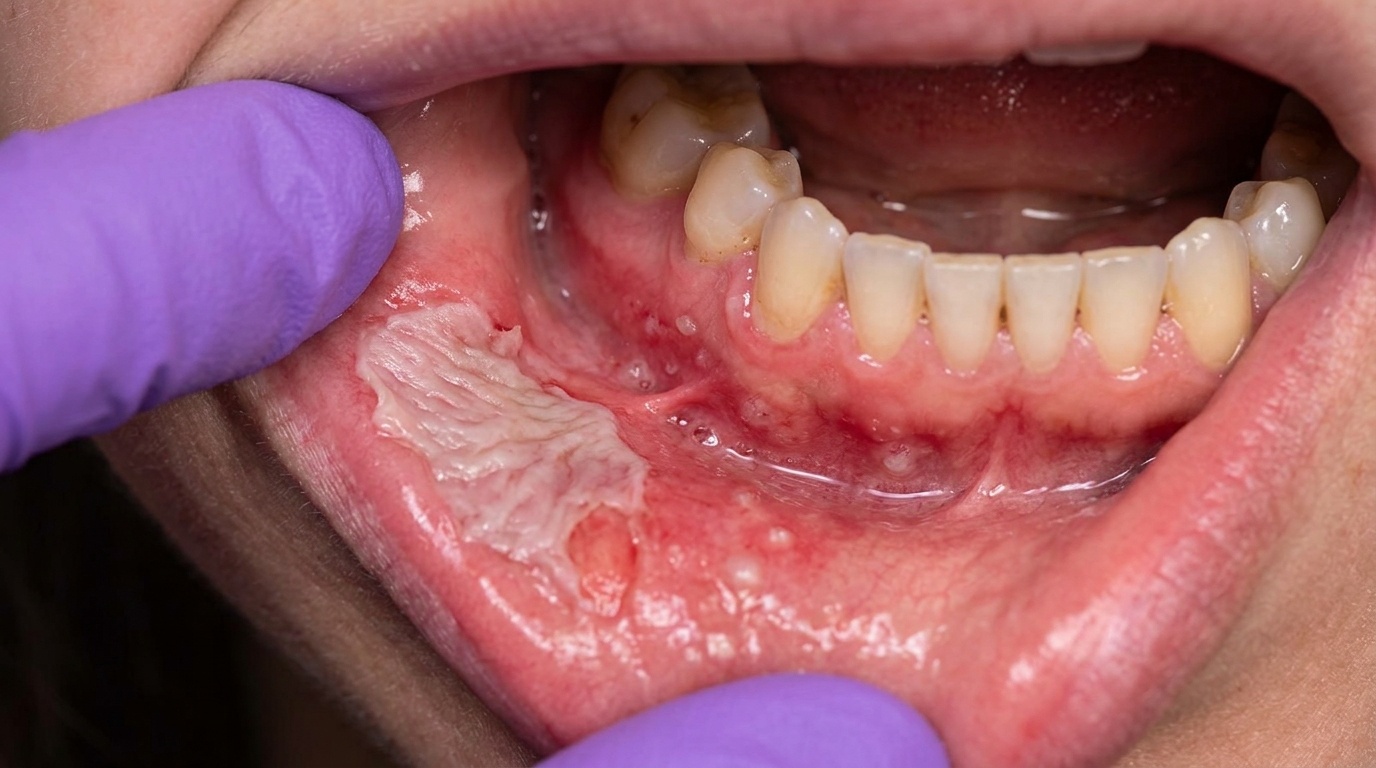
White, slightly thickened or shaggy patches on the cheeks or tongue (especially with cinnamon gum), sometimes streaked with redness.
Diffuse redness with peeling of the surface layer when toothpaste is the trigger, the inside of your cheeks and gums look raw.
Swollen, fiery red gums that bleed easily, with loss of the normal stippled texture (this is the plasma cell gingivitis pattern).
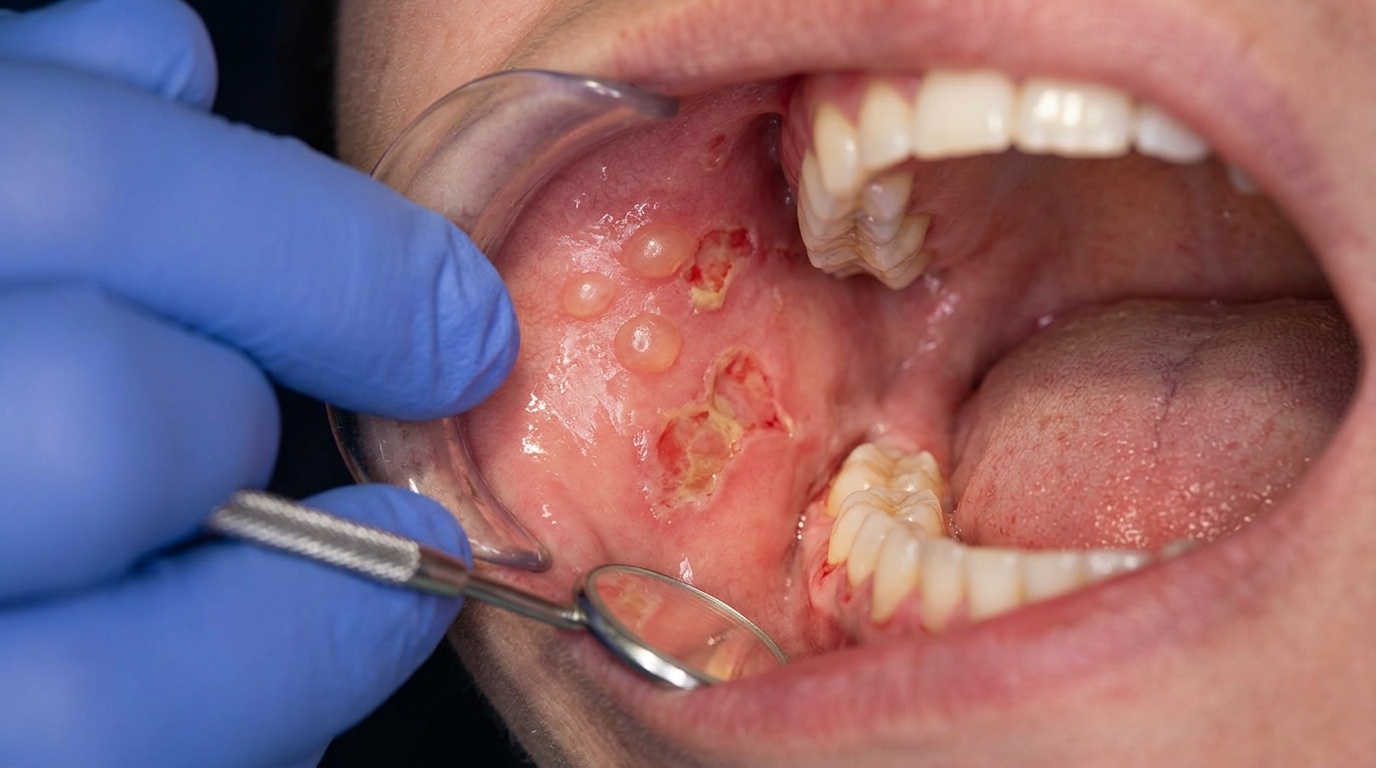
Small ulcers or erosions in the affected zone.
Lacy white striae around an old filling, the lichen-planus-like (lichenoid) contact reaction pattern.
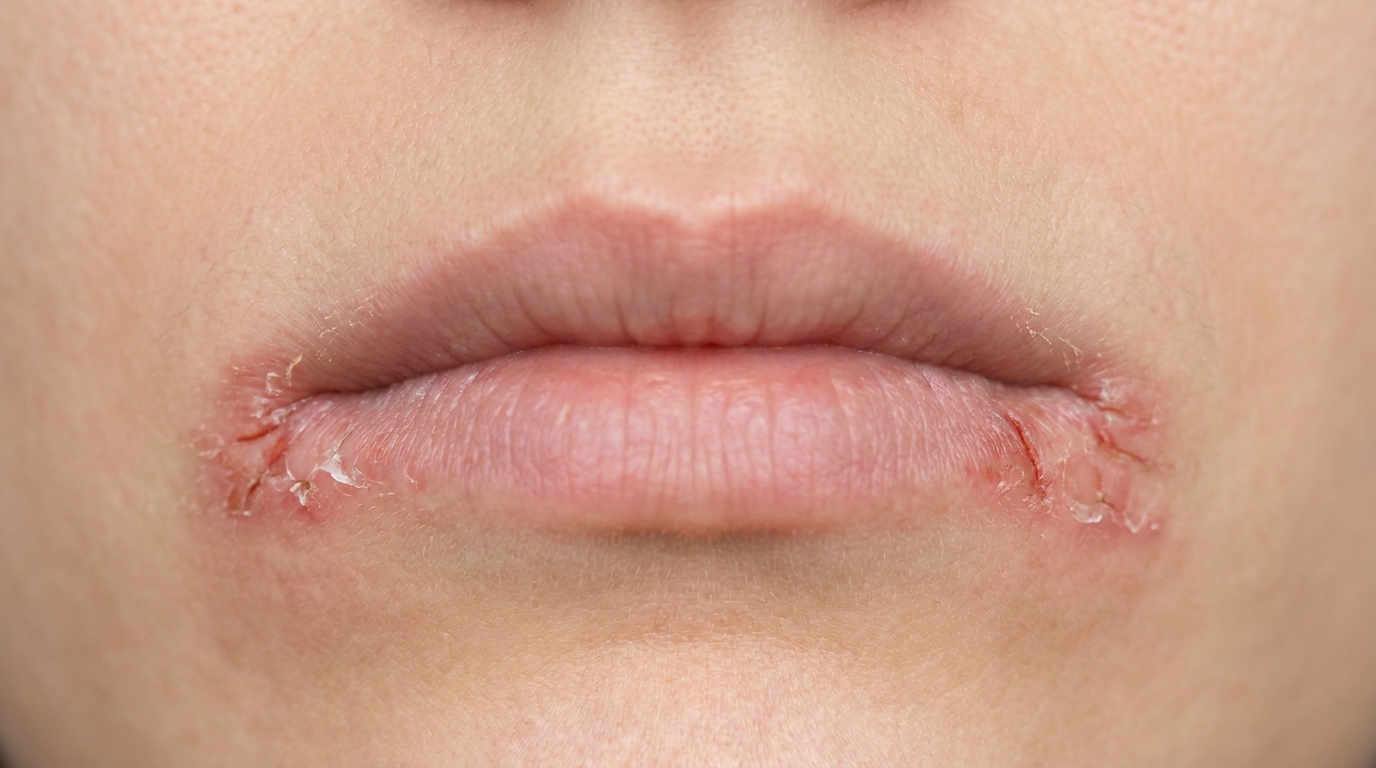
Cracked, dry, fissured lips and angles of the mouth when toothpaste, lipstick or sunscreen is the trigger (allergic contact cheilitis).
The reaction sits where the substance sat. Cinnamon-gum lesions famously appear as oblong patches along the line where your teeth meet, on the inside of the cheeks and the sides of the tongue.
What it feels like
Burning is the most consistent symptom, patients often describe a hot, raw, stinging quality rather than the sharp pain of an ulcer. You may also notice:
Itching, tingling or a prickly sensation
Mild swelling that makes the lining feel tight
Soreness when eating spicy, acidic or hot foods
Sometimes nothing at all, particularly with chronic lichenoid reactions next to fillings, these can sit there silently for years
What an X-ray might show
Nothing relevant. Contact stomatitis is a soft-tissue reaction; X-rays don't help with the diagnosis. They might be taken for other reasons during your visit, such as checking the integrity of an old filling.
What happens at the dentist?
At ArtSmiles, most contact reactions are sorted out by careful detective work rather than dramatic testing. A typical pathway:
A thorough history. Your dentist will ask what you brush with, what gum or mints you use, what you've recently changed, when symptoms started, and whether the soreness sits in one spot or moves around. The temporal link, symptoms appearing within days of a new toothpaste, or always after chewing a particular gum, is often the strongest clue.
A clinical examination. The dentist will map out where the redness or white change sits and look at whether it lines up with a specific filling, denture, gum-chewing habit or toothpaste foam pattern.
A trial of removal. The most reliable diagnostic test is to eliminate the suspected trigger and see whether the mouth clears. Cinnamon reactions usually settle within about a week of stopping the product; reintroducing it often brings symptoms back within 24 hours.
Patch testing, performed by a dermatologist or allergist, can be useful when the trigger is unclear or when a dental material is suspected. It is not perfect, patients with obvious oral cinnamon reactions may test negative on the skin, and not everyone with a positive patch test reacts in the mouth.
Biopsy (a small tissue sample sent to the lab for testing), taken under local anaesthetic, may be recommended if the lesion is extensive, atypical, doesn't clear with trigger removal, or needs to be distinguished from lichen planus or another mucosal disease.
Replacing one suspect filling with an inert alternative, see our service page on white dental fillings, is sometimes done as a diagnostic step when a lichenoid reaction sits directly against an amalgam. If the lining clears in that spot, the other suspicious fillings can be replaced too.
Is this serious?
🟡 In most cases, no. Contact stomatitis is uncomfortable and sometimes alarming to look at, but it isn't dangerous and almost always settles once the trigger is identified and removed.
There are a few situations that warrant prompter attention:
Acute swelling of the lips, tongue or throat, breathing difficulty, or hives spreading rapidly after a dental visit, this can represent a true immediate (anaphylactic) reaction, which is a medical emergency.
Chronic lichenoid reactions that won't clear after the suspected metal is removed deserve closer follow-up, because some investigators believe a small minority can change over time, and other lookalike conditions need to be ruled out.
Persistent ulceration in one spot for more than two weeks should always be assessed.
If you've noticed any of these signs for more than two weeks, it's worth booking an assessment.
Could it be something else?
Lots of conditions can produce a sore, red, white or ulcerated mouth. The differentials your dentist will keep in mind include:
Oral lichen planus, produces lacy white striae and erosions that look almost identical to a lichenoid contact reaction. The key difference is distribution: true lichen planus is usually bilateral, symmetrical and migrates over time, whereas a contact reaction sits stubbornly against the offending filling and clears when it is removed.
Lupus erythematosus (oral), can cause red, atrophic, sometimes ulcerated patches with white radiating striae. Usually accompanied by skin or systemic features and specific blood findings.
Erythematous (atrophic) candidiasis, produces a smooth, red, sore mucosa, often under a denture or after antibiotics. A swab or trial of antifungal treatment helps tell them apart.
Denture-induced stomatitis, bright red mucosa exactly outlining the denture-bearing area; usually caused by candida and poor denture hygiene rather than allergy to the acrylic itself.
Traumatic ulcer, caused by a sharp tooth, rough filling, or accidental bite. Usually a single, well-defined sore that heals once the source of trauma is smoothed.
Perioral (periorificial) dermatitis, a rash of small red papules around the lips, nose and eyes, classically with a thin spared zone right next to the lip border. Linked to overuse of topical steroids and heavy facial cosmetics.
Allergic contact cheilitis, chronic dryness, scaling, fissuring and cracking of the lip vermilion. Triggers include lipsticks, sunscreens, toothpaste residues and dental floss flavours.
Plasma cell gingivitis, closely related allergic gingival pattern with diffuse, fiery red, swollen gums; often a reaction to a flavoured toothpaste, gum, mint or spice.
Burning mouth syndrome, burning sensation, often of the tongue, with a normal-looking mucosa and no clear trigger. The visible lesions of contact stomatitis distinguish it.
Erythema multiforme and other drug reactions, can cause widespread oral redness, erosions and crusted lips, but usually with a more dramatic and systemic onset.
Geographic tongue (erythema migrans), red patches with a white border that move around the tongue; pattern and migration help separate it.
Oral hairy leukoplakia or early dysplasia, hyperkeratotic (thickened, white) cinnamon lesions on the side of the tongue can look unsettlingly similar; biopsy (a small tissue sample sent to the lab for testing) and a trial of cinnamon avoidance help clarify.
Foreign body gingivitis, focal red and white gingival changes from microscopic restorative debris embedded during dental work; needs biopsy to confirm.
Orofacial granulomatosis, persistent lip and facial swelling, sometimes triggered by cinnamon and benzoate; biopsy shows non-caseating granulomas (small clusters of immune cells without the cheesy decay seen in tuberculosis).
Latex or impression-material allergy, typically presents as facial or perioral redness, hives or swelling soon after a dental appointment; intraoral changes may be minimal.
How is it treated?
The core of treatment is straightforward: identify the trigger and remove it. Almost everything else is comfort care while the lining settles.
What you can do at home:
Switch to a bland toothpaste, plain baking soda or a flavour-free, preservative-free toothpaste is often recommended during the investigation period.
Avoid cinnamon-flavoured products of any kind: gum, mints, candy, mouthwash, breath sprays, even cinnamon-flavoured floss.
Cut out other common triggers temporarily, strong mouthwashes, chewing gum, mints, chocolate, carbonated drinks, and very salty, spicy or acidic foods.
Keep a brief diary of what goes into your mouth and when symptoms flare; the pattern often reveals itself.
What a dentist may recommend:
Removing or replacing a suspect filling, especially when a lichenoid reaction sits directly against an old amalgam. Inert alternatives (materials less likely to provoke a reaction) such as glass ionomer, porcelain or porcelain-fused-to-metal restorations are usually preferred.
Smoothing, polishing or recontouring an existing restoration first, since plaque accumulation around a rough surface can mimic an allergic reaction.
Topical corticosteroid gels, pastes or rinses to settle stubborn inflammation while the trigger is being identified.
Topical anaesthetics or antihistamines for symptom relief in more severe acute reactions.
Adjustments to denture design, polishing, or remaking the denture with a fully polymerised acrylic when residual monomer is suspected.
Referral to an allergist for patch testing (a skin allergy test where small amounts of suspected allergens are applied to the skin) or to an oral medicine specialist for chronic, recurrent or unclear cases.
For the rare immediate (anaphylactic-type) reaction with airway swelling, urgent medical care with adrenaline (epinephrine), antihistamines and corticosteroids is required.
What's the long-term outlook?
The outlook is generally very good. Once the offending trigger is identified and removed, the mucosa usually returns to normal within one to two weeks. Cinnamon-related lesions typically clear within a week of stopping the product, and reintroduction usually brings symptoms back within a day, which is itself a useful diagnostic confirmation.
Lichenoid contact reactions next to a filling resolve in most patients within a couple of weeks of replacing the restoration. Plasma cell gingivitis settles when the responsible allergen (often a toothpaste, mint or chewing gum ingredient) is removed, although a small subset is more stubborn and may need topical corticosteroid management.
The main long-term consideration is avoidance: once your mouth has reacted to a particular substance, future exposures are likely to produce the same reaction, so the trigger generally needs to be left out for good. Patients who continue to be exposed without realising it (for example, switching brands but not realising the new toothpaste contains the same flavouring) often have grumbling, recurrent symptoms that puzzle them for months until the connection is finally made.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
The cover image above is an AI-generated illustration based on the most common visible features of this condition described in clinical pathology references. It is not a photograph of a real case and should not be used to diagnose or rule out the condition in your own situation. If you are concerned about something you have noticed, please book an assessment with a registered dental practitioner.
References
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2023). Oral and maxillofacial pathology (5th ed.). Elsevier. Chapter 9, Allergies and Immunologic Diseases (Allergic Contact Stomatitis; Contact Stomatitis from Artificial Cinnamon Flavoring; Lichenoid Contact Reaction from Dental Restorative Materials), pp. 342,347; Chapter 4, Periodontal Diseases (Plasma Cell Gingivitis), pp. 152,154.
Regezi, J. A., Sciubba, J. J., & Jordan, R. C. K. (2017). Oral pathology: Clinical pathologic correlations (7th ed.). Elsevier. Chapter 2, Ulcerative Conditions (Contact Allergy / Drug Reactions), pp. 49,50; Chapter 4, Red-Blue Lesions (Plasma Cell Gingivitis; Drug Reactions and Contact Allergies), pp. 130,131.
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 13, Diseases of the Oral Mucosa: Non-infective Stomatitis ('Allergic' Stomatitis), pp. 236,237; Chapter 25, Allergy and Autoimmune Disease (Latex allergy; Allergy to mercury and other metals), pp. 362,364.
Laskaris, G. (1994). Color atlas of oral diseases (2nd ed.). Thieme. Chapter 10, Allergy to Chemical Agents Applied Locally (Allergic Stomatitis due to Acrylic Resin; Allergic Stomatitis due to Eugenol), pp. 83,84.
Frequently asked questions
What is contact stomatitis?
Contact stomatitis is inflammation of the lining of the mouth caused by direct contact with a substance the immune system has become sensitised to. The reaction looks like redness, ulceration, white lichenoid lines, swelling and a burning sensation, usually at the site of contact (cheek next to an amalgam filling, lips after lipstick, palate after a denture).
What are common triggers?
Common triggers include dental amalgam (mercury, silver, palladium, copper), gold, nickel and other dental alloys, acrylic monomers in dentures, denture adhesives, toothpaste flavours (cinnamon, mint), preservatives (parabens, sodium lauryl sulfate), foods (mango skin, nuts, certain fruit), lip balms, lipsticks, cosmetic peels, latex and orthodontic materials.
How is it diagnosed?
The pattern of redness or ulceration corresponding to the contact site is the most important clue. A detailed history of new products, foods or restorations helps narrow the possibilities. Patch testing (skin or oral) confirms the specific allergen. Biopsy may be needed to rule out lichen planus, lichenoid drug reactions or autoimmune blistering disease.
How is contact stomatitis treated?
Treatment is by identifying and removing the trigger — switching toothpaste, replacing the suspected restoration with an alternative material, changing denture base material, avoiding the offending food or cosmetic. Topical corticosteroids and barrier rinses help during the healing phase. Most cases resolve in 1-4 weeks after the trigger is removed.