
Gum
Disease
Healthy gums protect more than just your teeth.
Bleeding gums, swelling, or bad breath might seem like small things, but they can be early signs of gum disease. Left untreated, it doesn’t just affect your teeth, it can impact your overall health too. The good news? When caught early, gum disease is very treatable. At ArtSmiles in Southport, we help Gold Coast patients take control before things get worse.
What Is
Gum Disease?
Common Warning Signs
- Bleeding when brushing or flossing
- Swollen, red, or tender gums
- Persistent bad breath (halitosis)
- Gum recession or receding gums
- Loose or shifting teeth
- Visible pus around teeth
How Gum Infection
Affects Your Body
Managing oral health is one part of reducing overall inflammatory burden — and it starts with early assessment.
some form of gum disease
moderate-to-severe periodontitis
don't know they have it
Sources: Eke et al. 2012, NHANES · Ha et al. 2020, Australian Dental Journal · CDC Oral Health
Book Your Periodontal Assessment
Share your details and our team will be in touch within 1 business day to confirm your appointment.
Prefer to call? Reach us on (07) 5588 3677
Oral Inflammation and
Whole-Body Health
When gums are inflamed, bacteria from the mouth can enter the bloodstream. This triggers a low-level immune response throughout the body, the same kind of persistent inflammation linked to conditions like diabetes, heart disease, and respiratory problems.
Treating gum infection does not cure these conditions, but it helps reduce the overall inflammatory load on your body. Research continues to show that good oral health supports better general health outcomes.
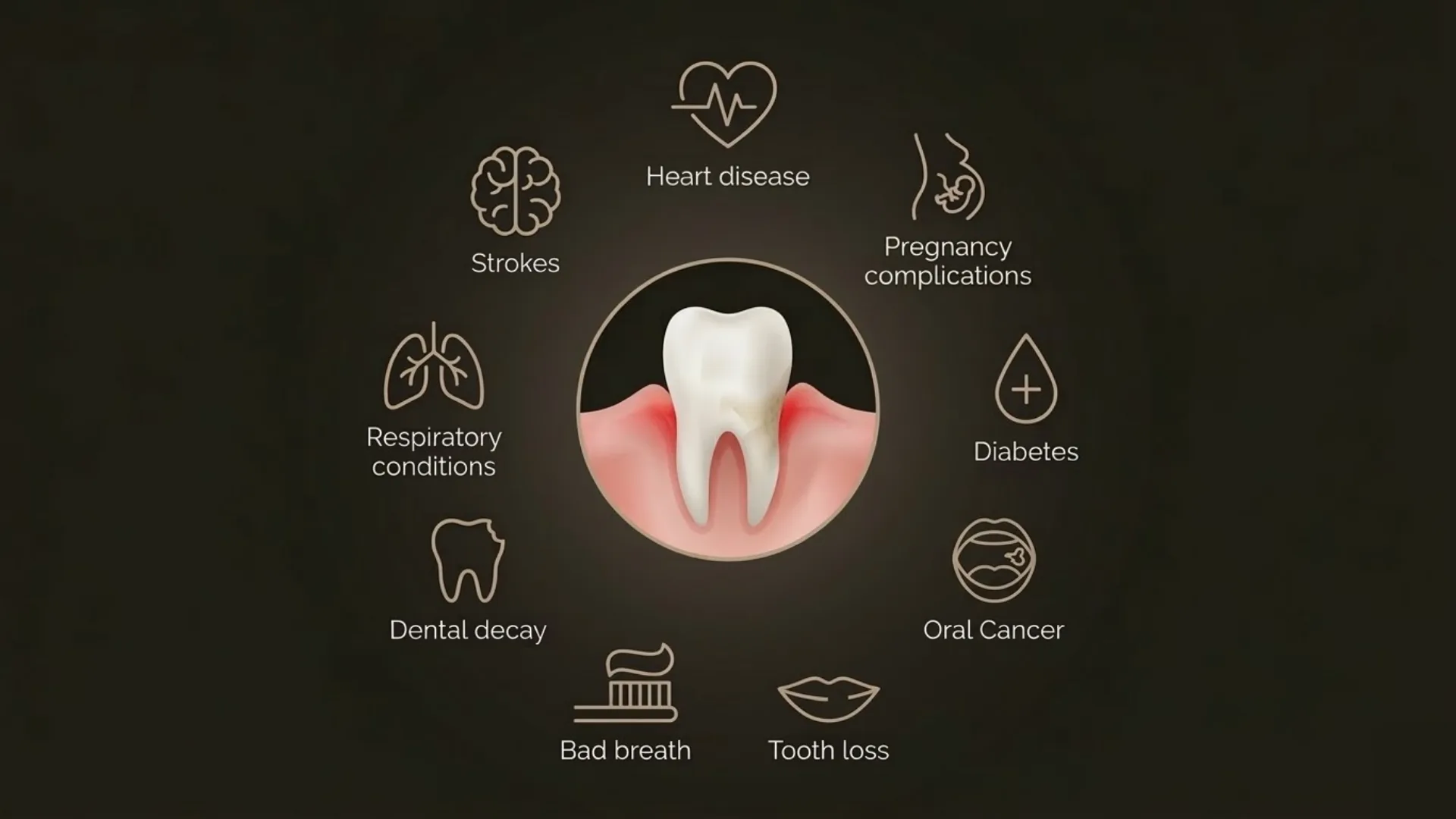
Gum Disease and Your Health
Periodontal disease is one of the most researched inflammatory conditions in dentistry. The table below summarises the strongest available evidence — all from peer-reviewed systematic reviews and clinical studies linking oral inflammation to systemic health.
How We Address
Gum Infection
Every case is assessed individually. Treatment is planned based on disease staging, pocket depth, bone levels, and your personal risk factors — not performed automatically.
Periodontal Assessment
A thorough assessment is the essential first step. We measure and record all relevant clinical data before recommending any treatment for bleeding gums or deeper gum infection.
- —Full pocket charting (six points per tooth)
- —Bleeding index scoring
- —Radiographic bone level analysis
- —Risk factor identification (smoking, diabetes, systemic conditions)
 Step 01 · ArtSmiles
Step 01 · ArtSmilesReady to take the next step?
Book a consultation to discuss your personalised plan.
Risk-Based
Assessment Model
Based on the Periodontal Risk Assessment (PRA) model. Lang & Tonetti, 2003
Stages of Gum Disease
The earlier the condition is caught, the simpler the treatment. Bone loss from periodontitis cannot be reversed, but progression can be halted with structured care.
 Routine Clean
Routine CleanHealthy
No inflammation, no bleeding, no pocket depth beyond normal. Maintained with regular check-ups and professional cleaning.
 Routine Clean
Routine CleanGingivitis
Reversible inflammation with redness and bleeding. No bone loss yet. Early intervention prevents progression.
 Deep Cleaning
Deep CleaningEarly Periodontitis
Bone loss begins. Pockets deepen beyond 4 mm. Deep cleaning at this stage is highly effective at halting progression.
 Deep Cleaning
Deep CleaningModerate Periodontitis
Deeper pockets, increased mobility risk, and visible bone loss. Ongoing maintenance becomes essential for stability.
 Surgery
SurgeryAdvanced Periodontitis
Significant bone loss and tooth mobility. Complex rehabilitation or extraction planning may be required. Surgical intervention is typically needed.
Stages 1 and 2 are managed with routine check-ups and professional cleaning. Deep cleaning (scaling and root planing) is indicated for Stages 3 and 4. Stage 5 typically requires periodontal surgery.
Bleeding Gums? Let’s Check.
The earlier you get your gums checked, the simpler the treatment. Book a consultation and we’ll take a thorough look at what’s going on.
Ready to get started?
Prefer to call? (07) 5588 3677
Understand Your
Oral Health Risk
This assessment provides a general indication only. A definitive evaluation requires an in-person consultation with our Southport team.
- —Decay risk — dietary habits, saliva quality, and bacterial balance
- —Gum health risk — inflammation patterns, bone support, and hygiene effectiveness
- —Grinding & clenching risk — bite forces, wear signs, and jaw tension
Start Your Assessment
Takes less than 2 minutes. No obligation.
Why Bleeding Gums Treatment
Should Not Wait
Consequences of Delayed Treatment
Progressive Bone Loss
Pockets deepen and attachment loss accelerates with each cycle of reinfection. Once bone is lost, it rarely regenerates without surgical intervention.
Tooth Mobility
As supporting bone recedes, teeth gradually loosen. Increased mobility compromises chewing function and may eventually make teeth non-restorable.
Tooth Loss
In advanced cases, extraction becomes unavoidable. Severely compromised teeth pose ongoing infection risk to adjacent teeth and bone.
Compromised Implants
Active infection dramatically increases the risk of peri-implant disease and implant failure. The condition must be controlled before any implant treatment can proceed safely.
Systemic Inflammatory Exposure
Ongoing bacterial burden and elevated inflammatory markers are linked to cardiovascular, diabetic, and respiratory health complications.
Related Articles
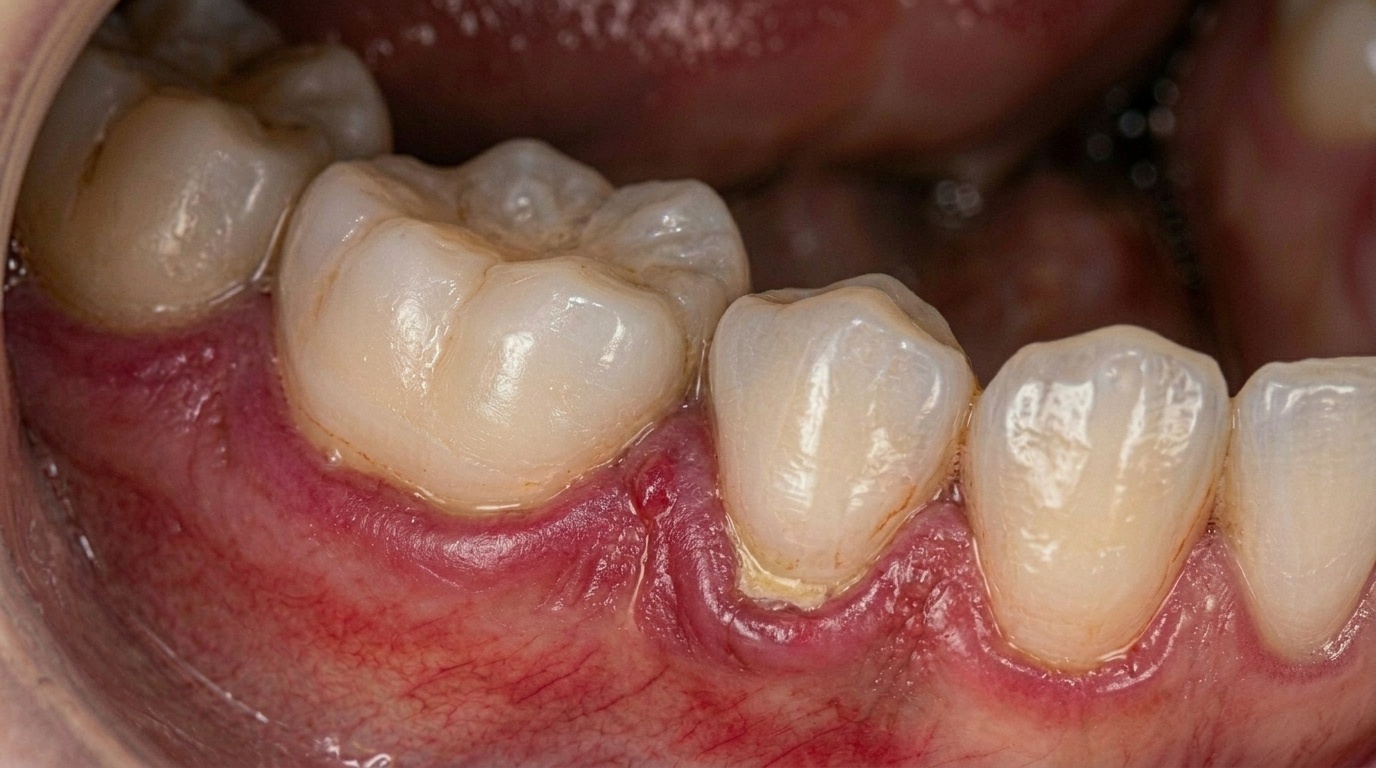
How to Treat Bleeding Gums: Causes, Solutions, and When to See a Dentist
Updated 17 May 2026
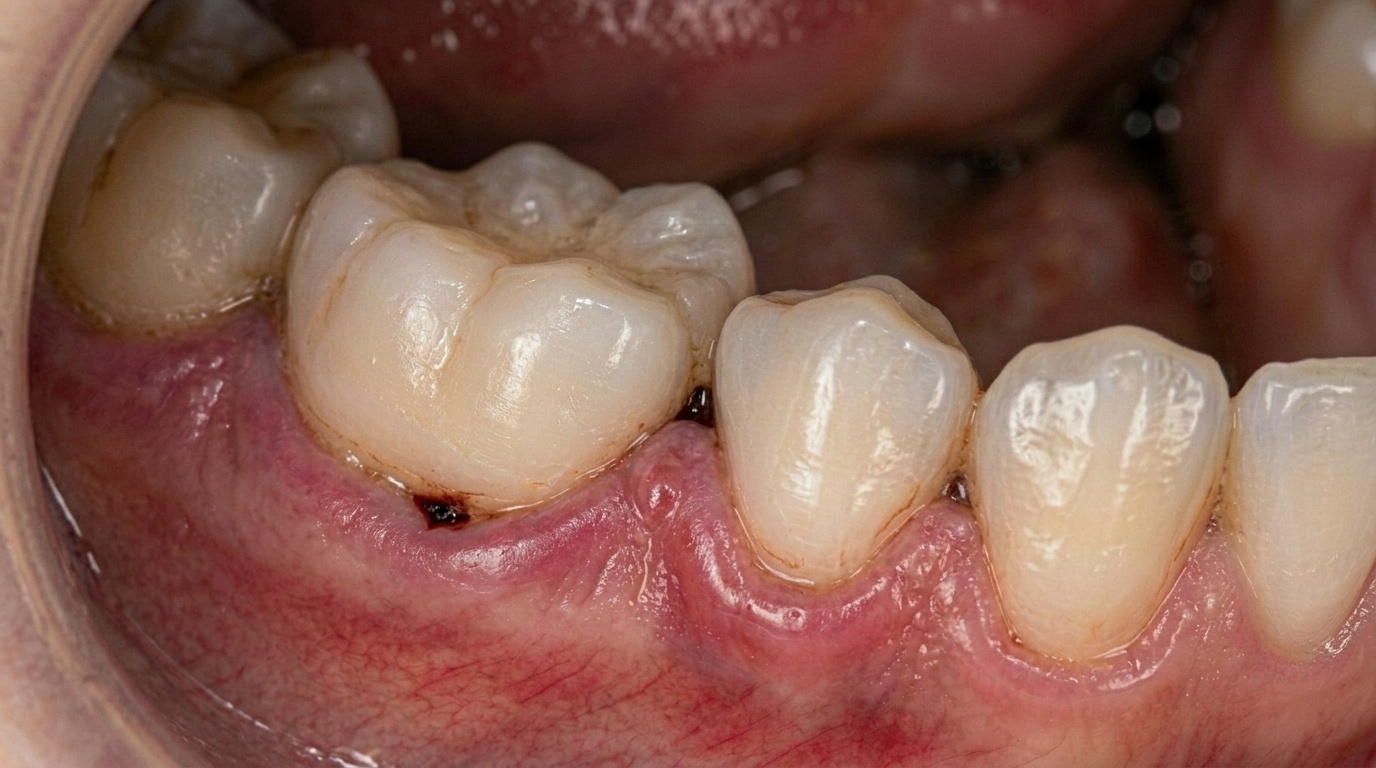
Bleeding Gums Are Not Normal: What Your Body Is Trying to Tell You
Updated 17 May 2026
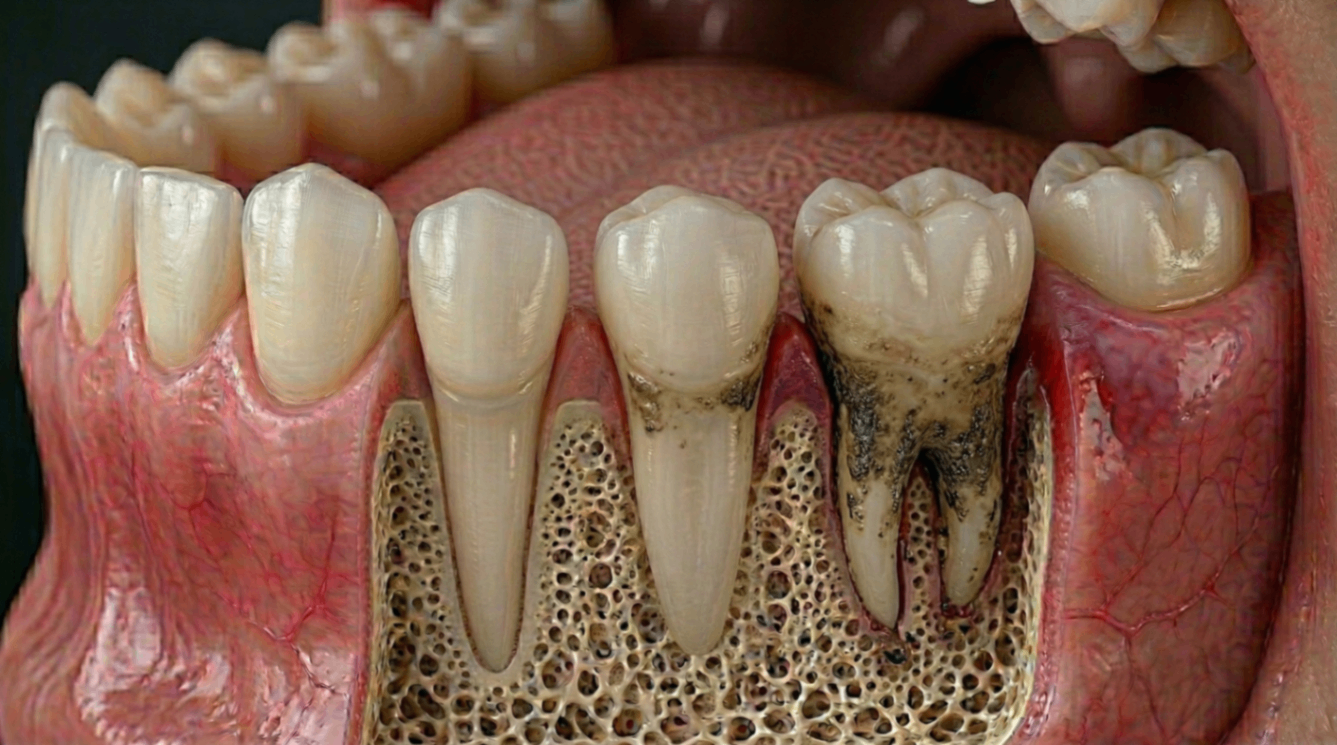
When Gum Disease Stops Hurting: Why Silence Does Not Mean Safety
Updated 17 May 2026
Noticing Your Teeth Moving? Here's Why It Happens as We Age
Updated 25 April 2026
Frequently Asked
Questions
What is the difference between gingivitis and periodontitis?
Gingivitis is the early, reversible stage — inflammation in the gum tissue without bone loss. Periodontitis is more advanced, involving irreversible bone loss around teeth. Gingivitis can progress to periodontitis if left untreated, which is why early assessment matters.
Is gum disease painful?
It is often painless, particularly in early and moderate stages. This is one of the reasons it frequently goes undetected until significant damage has occurred. Bleeding during brushing is often the only early warning sign.
What is scaling and root planing?
Scaling and root planing is a deep cleaning procedure that removes plaque and calculus from below the gumline. It reduces the bacterial load within periodontal pockets and smooths the root surface to promote healing. It is the primary non-surgical treatment for periodontitis.
Can gum disease affect overall health?
Research has linked periodontal inflammation to conditions including diabetes, cardiovascular disease, respiratory conditions, and adverse pregnancy outcomes. The shared mechanism is chronic inflammation. Managing oral health is one part of reducing the body's overall inflammatory burden.
Can gum disease affect dental implants?
Yes. Active infection significantly increases the risk of peri-implant disease — the implant equivalent of periodontitis. The condition should be stabilised before implant placement and monitored closely afterwards.
When should I see a dentist about my gums?
If you notice bleeding, swelling, recession, persistent bad breath, or any changes around your teeth, book an assessment as soon as possible. The earlier the condition is caught, the simpler and more predictable the treatment.
What causes gum disease?
The primary cause is bacterial plaque that accumulates along and beneath the gum line. Risk factors that increase susceptibility include smoking, poorly controlled diabetes, genetic predisposition, certain medications, stress, and inadequate oral hygiene.
Can gum disease be cured?
Gingivitis is fully reversible with professional treatment and improved home care. Periodontitis cannot be cured, but it can be stabilised. With structured treatment and ongoing maintenance, progression can be halted and teeth maintained long term.
How often do I need periodontal maintenance?
This depends on your disease stage and response to treatment. Most patients with a history of periodontitis require maintenance every three to four months, which is more frequent than the standard six-month recall.
Is the relationship between gum disease and diabetes real?
Yes, and it works in both directions. Diabetes increases susceptibility to gum infection, and active periodontal inflammation can worsen glycaemic control. Managing oral health is considered an important part of diabetes care.
Does smoking worsen gum disease?
Significantly. Smoking impairs blood flow to the gums, suppresses immune response, masks bleeding (making early detection harder), and substantially reduces the effectiveness of treatment. It is one of the strongest modifiable risk factors.
Still have questions?
Our team is here to help. Book a consultation to discuss your options.
This page has been clinically reviewed by Dr. Cristian Dunker, BDSc, MBA, Principal Dentist at ArtSmiles.

