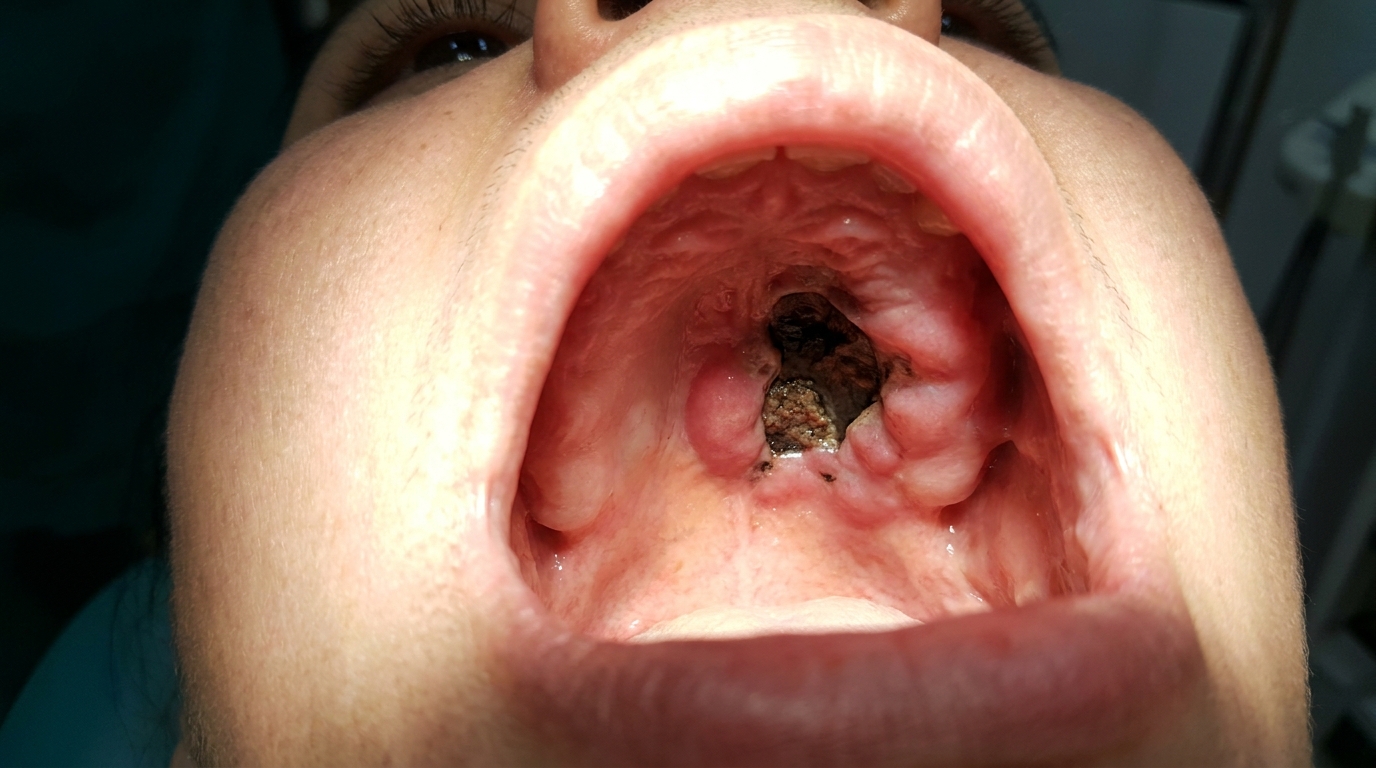
Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker , Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | Aspirin burn, pizza burn, chemical injury of oral mouth lining (mucosa), thermal mucosal burn, contact stomatitis |
How urgent? | 🟢 Usually harmless, most heal on their own within 7 to 14 days, but persistent or large burns deserve a check |
Common or rare? | Common, particularly thermal food burns and aspirin burns |
Who it affects | Both adults and children; aspirin burns are mostly in adults trying to ease toothache, food burns affect everyone |
Who treats it | General dentist, specialist input rarely needed unless the burn is large or caustic |
Based on | Regezi, Neville, Cawson, Laskaris |
What is it?
A chemical or thermal burn of the mouth is an injury where the lining of the mouth has been damaged by something hot, acidic, alkaline or otherwise irritating. The tissue dies on the surface, leaving a white film that peels away to reveal a red, raw area underneath.
These burns are reactive injuries, meaning they are simply the mouth's response to a one-off insult. They have no link to cancer, and once the offending agent is removed, the tissue almost always heals on its own.
Who tends to get it?
Anyone can get one. There are some patterns worth knowing about.
Aspirin burns are most often seen in adults who hold an aspirin tablet (or powder) directly against the gum next to a sore tooth, hoping it will numb the pain. The textbooks note that this practice is becoming less common as people learn that aspirin only works once it is swallowed and absorbed, but the injury still turns up in dental clinics.
Pizza burns and other thermal food burns are seen across all ages. Children and adults alike scald the roof of the mouth on hot melted cheese, microwaved fillings that are cool on the outside but molten inside, and very hot tea or coffee.
Iatrogenic burns, those caused during a dental procedure, can affect any patient. They occur when materials such as etching gel, tooth-whitening peroxide, phenol-containing cavity dressings, sodium hypochlorite endodontic (root canal) irrigant or hot impression material come into contact with the soft tissues for too long.
Caustic chemical burns are seen in patients who place strong household products (bleach, denture cleaners, hydrogen peroxide mouthrinses, alcohol-heavy folk remedies) directly on the gums, often hoping to treat an ulcer or sore spot. Children can sustain accidental burns by drinking from a container holding a household chemical.
What causes it?
The two big categories are heat and chemicals.
Thermal causes include hot pizza, melted cheese, microwaved foods that hide a molten core, freshly made tea or coffee, and hot soups. The textbooks note that microwave cooking has increased thermal burn frequency because food can feel cool to the touch on the outside while being scalding inside. Electronic cigarettes have also been linked to thermal injuries, the heating element can reach 100 to 250°C, and there have been reports of devices overheating or even exploding in the mouth.
Chemical causes the books describe in detail include:
Aspirin held against the gum next to a painful tooth.
Hydrogen peroxide, even dilute concentrations (1% and above) can damage the lining if held against it.
Tooth-whitening products containing peroxide or carbamide peroxide, particularly when strips or trays leak.
Phenol, found in some over-the-counter "canker sore" gels and in dental cavity medicaments.
Silver nitrate, sometimes used as an old-school cautery (burning the surface to seal it) for ulcers.
Endodontic materials such as sodium hypochlorite, formocresol, paraformaldehyde and calcium hydroxide if they leak from the root canal during treatment.
Acid etchants used during fillings and orthodontic bonding.
Caustic household agents like bleach, denture cleaners, trichloroacetic acid and other concentrated cleaners.
Concentrated alcohol or alcoholic iodine solutions held in the mouth as a folk remedy for toothache.
Cocaine rubbed on the gums to test purity, the textbooks describe this as a recognised cause of localised mucosal tissue death (necrosis).
In short: anything strong enough to denature protein (break down its structure), whether hot or chemically aggressive, can do it.
How does it develop?
The lining of the mouth is a thin sheet of cells designed for warm, moist food, not boiling cheese or concentrated acid. When something too hot or too caustic stays in contact with the tissue, the surface cells die in a process called coagulative necrosis. Think of it like a fried egg: the protein in the white changes from clear and flexible to opaque and rubbery the moment it hits the hot pan.
In the mouth, this gives the dead surface a white, wrinkled appearance. The dead layer stays in place for a day or two, then sloughs away, leaving a raw, red, sometimes bleeding patch underneath. A yellowish fibrin film (a natural healing film) then forms over the raw area, and new lining cells grow in from the edges to close it.
Mucosa firmly bound down to bone (such as the hard palate and attached gum) is keratinised (the firm, leathery type of lining) and a bit tougher, so it resists damage longer. The thin, mobile lining of the cheeks, floor of the mouth and underside of the tongue is destroyed more quickly.
What might you notice?
What it looks like
Most burns go through two stages.
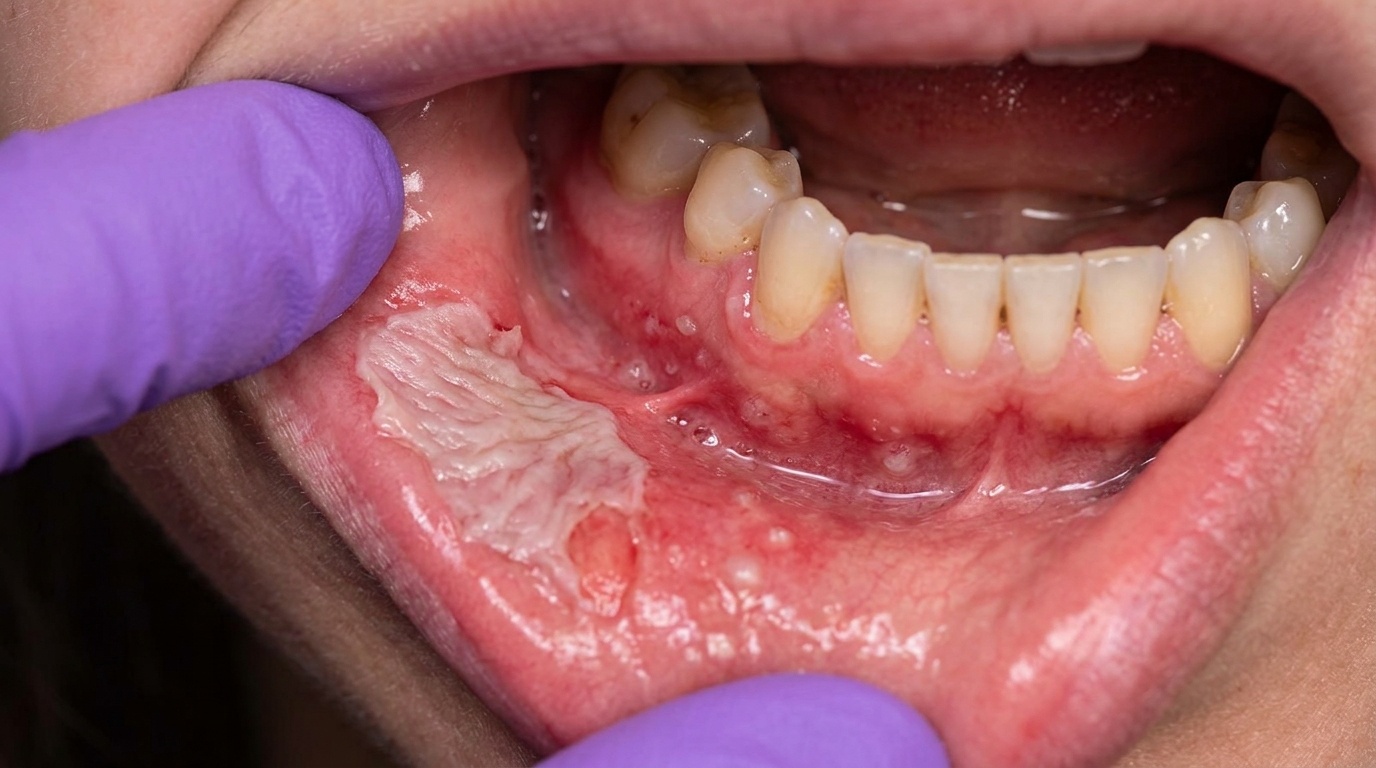
In the first day or so, the affected area looks white, wrinkled and slightly raised, almost as though a piece of tissue paper has been stuck onto the gum or palate. The white film is sharply demarcated from healthy pink mucosa around it.
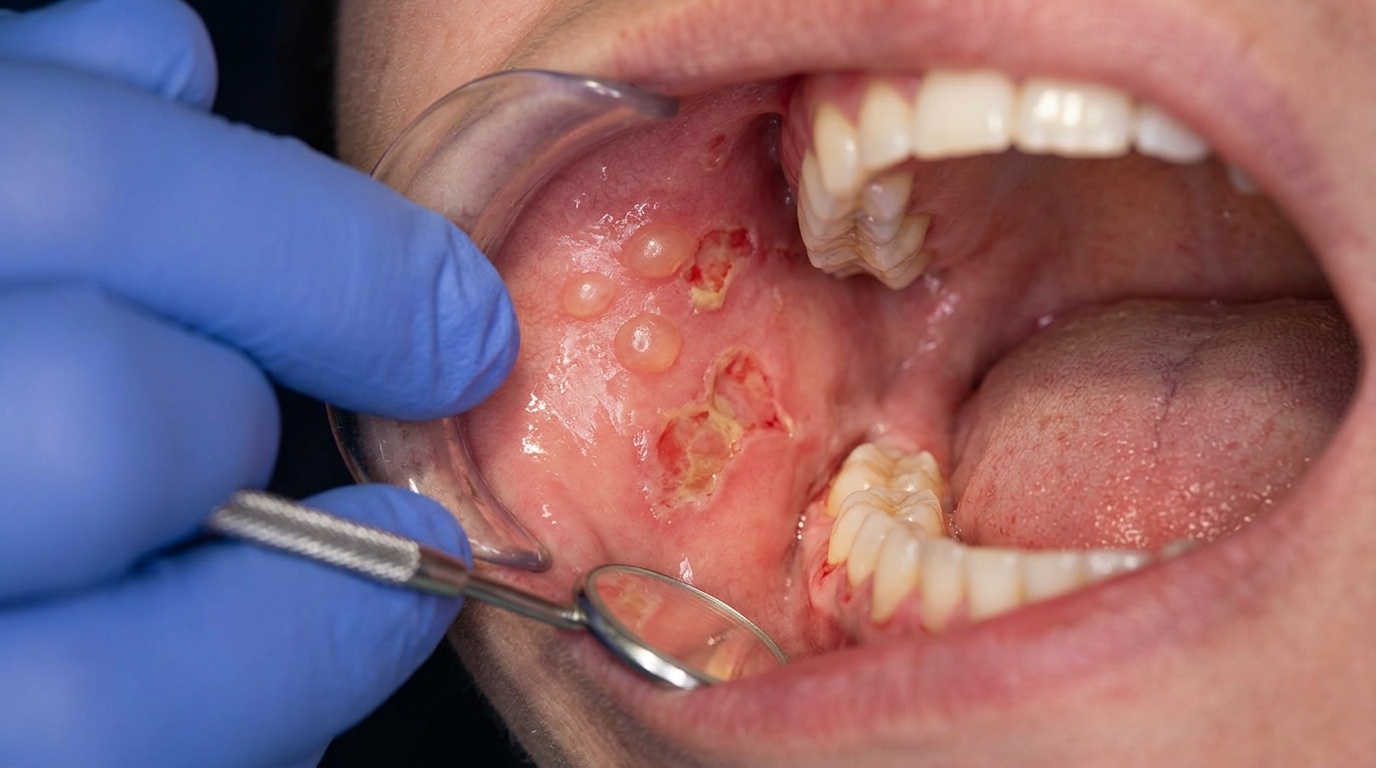
Within a few days, that white slough (dead surface tissue that lifts off) peels off, often in flakes if you brush your teeth or eat. Underneath you will see a red, raw, sometimes bleeding ulcer that may then develop a yellow fibrin coating as it begins to heal.
For an aspirin burn, the white patch is classically right next to the tooth the patient was trying to treat. Pizza burns most often sit on the hard palate or back of the cheek. Tooth-whitening burns trace the outline of the strip or tray on the gum line. Phenol or endodontic-irrigant burns sit around the tooth being treated.
What it feels like
It depends on the stage. While the white slough is intact, the area can feel oddly numb or just slightly tight. Once the slough peels off and exposes the raw surface, the area becomes sore, stinging and very sensitive to hot, salty, acidic or spicy foods. Toothpaste can sting. Talking and eating may be uncomfortable for a few days.
In an electronic-cigarette burn or a hot-liquid burn that has been swallowed, there can be swelling further down the throat, and the books warn that breathing difficulty is a red flag needing urgent medical care.
What an X-ray might show
Not relevant for the soft-tissue surface burn itself. X-rays are only used if a dentist suspects deeper damage, for example, if a strong endodontic chemical has leaked into the bone around a tooth, or if an electrical or e-cigarette injury may have damaged the jaw.
What happens at the dentist?
The diagnosis is usually a clinical one made on the day, and the history is the giveaway. Your dentist at ArtSmiles will ask:
Have you held anything against that area recently, a tablet, a gel, an ulcer treatment?
Have you eaten something very hot in the past day or two?
Have you had a recent dental procedure (filling, whitening, root canal)?
Do you use mouthrinses, peroxide products or whitening strips?
They will then examine the mouth, looking at the size, shape, location and stage of the white or red area. A burn is typically sharply demarcated, sits in a location consistent with the reported insult (next to the offending tooth, on the palate after a hot meal, along the gum line for whitening), and matches the timeline.
A biopsy (a small tissue sample sent to the lab for testing) is rarely needed for a clear-cut burn. It may be considered if the lesion is unusual, has not healed within two weeks, or if there is doubt about the diagnosis. Where a biopsy is taken, the textbooks describe coagulative necrosis of the surface lining (epithelium) with mixed inflammation underneath.
Referral to a specialist is uncommon but appropriate for very large caustic burns, suspected airway involvement, electrical or e-cigarette injuries with deeper tissue damage, or burns that fail to heal as expected.
Is this serious?
🟢 Most chemical and thermal burns of the mouth are mild and self-limiting. Superficial areas of necrosis typically resolve completely without scarring within 10 to 14 days once the offending agent is removed. The textbooks describe these as having no malignant potential, they do not turn into cancer.
There are situations where a burn deserves more attention:
🟡 Large or deep burns from caustic agents (concentrated bleach, paraformaldehyde, strong acids).
🟡 Iatrogenic burns from leaked endodontic chemicals, these can damage underlying bone.
🔴 Burns associated with swallowed hot liquids, electrical injuries or e-cigarette explosions, especially if there is throat swelling, breathing difficulty or blood loss.
If you've noticed any of these signs for more than two weeks, it's worth booking an assessment.
Could it be something else?
Several other conditions can produce a white patch or a tender ulcer in the mouth. The books list these as the main differentials:
Aphthous ulcer, round or oval ulcers with a yellow base and red halo. Aphthae have no associated white slough peeling off, no clear chemical or hot-food trigger, and tend to recur in the same patient over years.
Traumatic ulcer, caused by mechanical injury (a sharp tooth, denture, cheek bite). The shape often matches the offending object and there is no white slough phase.
Herpes simplex (cold sore inside the mouth), starts as small clustered blisters that pop into shallow ulcers, usually on the gum or palate. There is often a tingling prodrome (early warning sensation) and the patient may feel generally unwell, neither of which features in burns.
Oral candidiasis (pseudomembranous thrush, a wipe-off white film), produces white patches that wipe off, but the pattern is patchier and more spread out, the underlying mucosa is red rather than raw, and there is usually a predisposing factor like steroid inhalers, antibiotics or dry mouth.
Oral lichen planus, creates lacy white lines or patches, but these do not peel away to reveal an ulcer in the way a burn slough does, and the pattern is bilateral and chronic.
Leukoplakia (white patches) / leukoedema, persistent white patches that do not wipe off and have no clear acute trigger.
Necrotising sialometaplasia, a benign palatal ulcer that mimics cancer; develops over weeks rather than appearing acutely after a hot meal.
Pseudomembranous reaction to chemotherapy or radiotherapy (mucositis), looks similar but develops in the context of cancer treatment.
Erythroplakia (a persistent red velvety patch), a persistent red velvety patch, usually painless, that warrants biopsy because of malignant potential. Burns are painful and acute.
Squamous cell carcinoma, a non-healing ulcer or red-and-white patch that persists beyond a few weeks. The key distinguisher is that burns heal; cancer does not.
Factitious (self-inflicted) ulceration, bizarre patterns in accessible areas, often with an inconsistent history. Cawson notes the history is rarely matched by the clinical picture.
The single most useful distinguisher across all of these is the history: a clear story of an aspirin tablet, a hot pizza, a whitening strip, or a recent dental procedure pointing at the right spot at the right time.
How is it treated?
The textbooks are unanimous: the best treatment is prevention, and the next-best is removing the cause and letting the body heal itself.
At home, you can help things along by:
Stopping whatever caused the burn, discard the aspirin habit, pause whitening products, avoid the offending mouthrinse.
Letting hot food and drink cool before eating.
Rinsing with warm salt water several times a day.
Eating soft, cool, bland foods while the area is raw.
Avoiding spicy, salty, acidic, alcoholic and carbonated foods and drinks until healed.
Using a soft toothbrush and being gentle around the area.
A dentist may suggest:
A topical anaesthetic to numb the area for short-term comfort.
A protective emollient paste or hydroxypropyl cellulose film (a thin protective film) placed over the area to shield it.
Simple paracetamol for pain (rather than aspirin held in the mouth).
A bland mouthrinse such as dilute saline or chlorhexidine if there is concern about secondary infection.
For larger or deeper burns, debridement (gentle removal of dead tissue) of the dead tissue and a short course of antibiotics may be considered.
For burns linked to a recent dental procedure (etchant, peroxide, endodontic irrigant), the dentist will identify and modify the cause to prevent it happening again.
Most patients are comfortable again within a few days, even before the area is fully healed.
What's the long-term outlook?
For everyday aspirin burns, pizza burns, whitening-strip burns and most accidental chemical contact burns, the outlook is excellent. The mouth has remarkable healing capacity. The textbooks describe complete resolution within 7 to 14 days without scarring once the offending agent is removed.
There is no malignant potential, chemical and thermal burns are reactive injuries, not pre-cancerous lesions. They do not increase your risk of mouth cancer.
Larger or deeper caustic burns (from concentrated bleach, paraformaldehyde, strong acids, leaked endodontic chemicals) can take longer to heal and occasionally leave scarring or, rarely, underlying bone necrosis. Electrical burns from biting through a live wire, most often seen in young children, can cause scarring of the mouth opening (microstomia) and may require splinting and surgical reconstruction.
Recurrence is entirely preventable: avoid the trigger and the burn does not return. If burns keep happening at the same site, that is a useful signal that a habit (aspirin under the tongue, very hot drinks, a particular mouthrinse) is worth changing.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
The cover image above is an AI-generated illustration based on the most common visible features of this condition described in clinical pathology references. It is not a photograph of a real case and should not be used to diagnose or rule out the condition in your own situation. If you are concerned about something you have noticed, please book an assessment with a registered dental practitioner.
References
Regezi, J. A., Sciubba, J. J., & Jordan, R. C. K. (2017). Oral pathology: Clinical pathologic correlations (7th ed.). Elsevier. Chapter 2, Ulcerative Conditions, pp. 23 to 26.
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2023). Oral and maxillofacial pathology (5th ed.). Elsevier. Chapter 8, Physical and Chemical Injuries, pp. 276 to 280.
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 13, Soft Tissue Disease (Chemical burn), p. 238; Chapter 35, Complications of Systemic Drug Treatment (Chemical burns), p. 443.
Laskaris, G. (2006). Pocket atlas of oral diseases (2nd ed.). Thieme. Chapter 5, Oral Lesions due to Chemical Agents, pp. 56 to 63; Chapter 6, Oral Lesions due to Smoking and Heat, pp. 64 to 66.