Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker, Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | BP, autoimmune subepidermal blistering disease |
How urgent? | 🔴 See a doctor or dentist promptly, this is an autoimmune blistering condition that needs medical management, especially if widespread or painful. |
Common or rare? | The most common autoimmune blistering disease overall, but uncommon in the general population (around ten new cases per million people per year). Oral involvement is uncommon within the disease itself. |
Who it affects | Adults, predominantly older adults (most cases occur between 75 and 80 years of age, with peak incidence in the seventh and eighth decades) |
Who treats it | Dermatologist usually leads care; your dentist may be the first to notice oral lesions and works alongside the medical team for any mouth involvement |
Based on | Regezi, Neville, Cawson, Laskaris |
What is it?
Bullous pemphigoid is a long-term autoimmune blistering condition that mostly affects the skin in older adults. The body's immune system mistakenly targets the proteins that help glue the top layer of skin to the layer beneath, causing tense, fluid-filled blisters to form. The mouth can be involved too, but usually plays a supporting role rather than the lead.
Who tends to get it?
Bullous pemphigoid is the most common of the autoimmune blistering conditions. It tends to develop in older people, with most patients between 75 and 80 years of age, and a peak incidence in the seventh and eighth decades of life.
There is no clear racial predilection, and reports on gender vary. Some sources note no sex preference, while others suggest men may be slightly over-represented when you adjust for the higher proportion of women in older age groups. Laskaris, in contrast, reports a female-to-male ratio of around 1.7 to 1, with a mean age of onset of 65 years. Childhood cases have been described but are very rare.
When it comes to the mouth, oral involvement happens in roughly 10 to 20 per cent of patients in some series, and up to about 40 per cent in others. Either way, the mouth is rarely where the story starts, only around 6% of patients have their first lesion in the oral cavity. In about a third of cases, mouth lesions appear alongside the skin disease.
What causes it?
Bullous pemphigoid is an autoimmune condition. That means the immune system, which normally protects you from infection, produces antibodies that attack a part of your own body, in this case, the very thin layer (called the basement membrane) that anchors your top layer of skin to the connective tissue below.
The specific targets are two proteins called BP180 and BP230, essentially the bolts inside tiny rivets (hemidesmosomes) that hold the skin's surface layer onto the layer beneath. When the antibodies bind to these proteins, they kick off a chain reaction involving the complement system (a group of proteins that helps the immune response) along with mast cells, neutrophils, and eosinophils (different types of inflammatory cells). The end result is that the top layer of skin separates from the layer beneath, and a blister forms.
Most cases are idiopathic, meaning no clear trigger can be identified. A small number of cases have been linked to certain medications, with the antibiotic vancomycin mentioned in the literature as a possible association for related blistering diseases. Genetics, ageing of the immune system, and certain neurological conditions have all been studied as possible contributing factors, but for most patients the cause remains uncertain.
How does it develop?
Think of your skin as a stack of two layers held together by tiny press-studs. In bullous pemphigoid, the immune system targets those press-studs. Once enough of them are damaged, the upper layer lifts away from the lower layer, and the gap fills with fluid, that is the blister.
Because the split happens deep down (beneath the entire surface layer of skin), the resulting blisters tend to be tense and dome-shaped, with a thick roof. They feel firm to the touch and don't pop easily. This is one of the most useful clinical clues, because in pemphigus vulgaris (a different autoimmune blistering disease), the split happens higher up within the skin's surface layer, and the resulting blisters are flaccid (soft and floppy), fragile, and rupture almost as soon as they form.
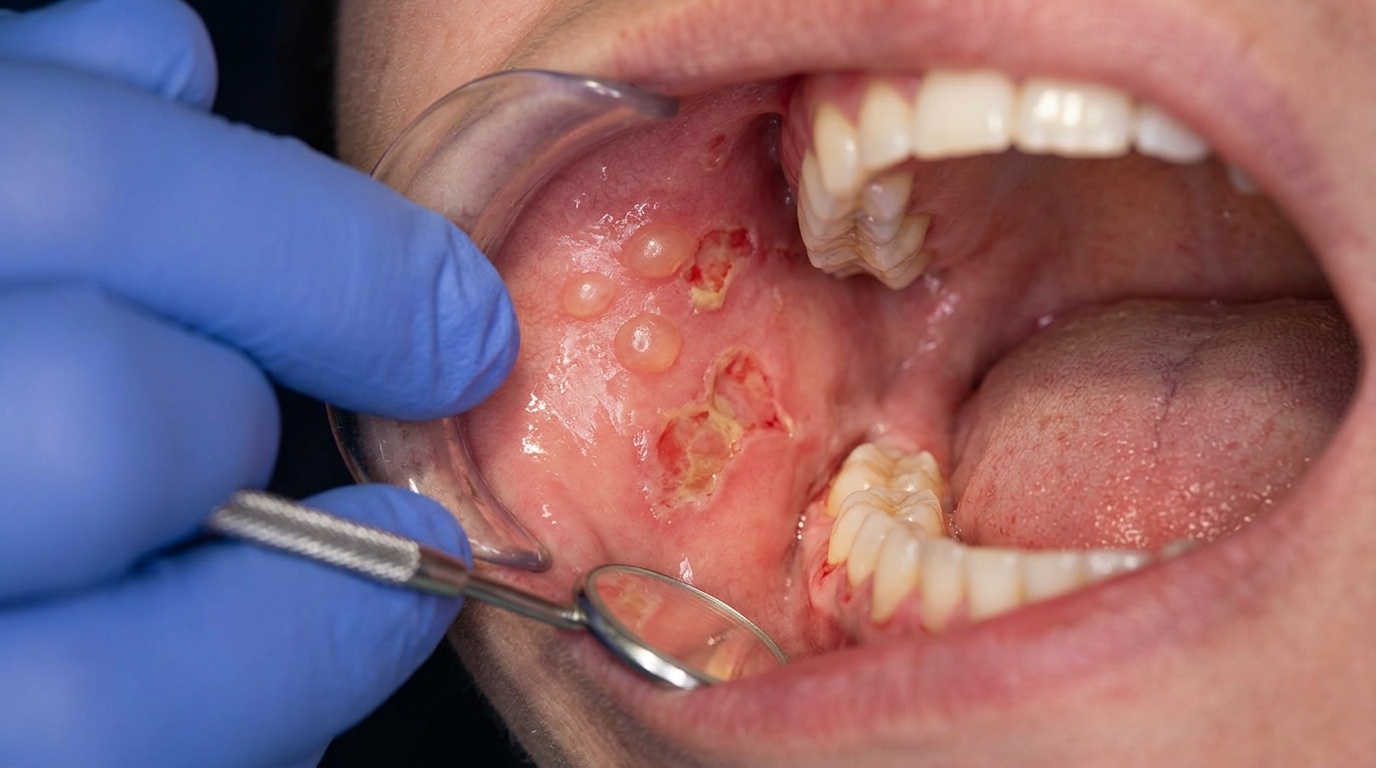
In the mouth, the same process occurs but the constant low-grade trauma from eating, talking, and tooth contact means the blisters rupture much sooner. By the time you or your dentist notice them, you usually see large, shallow ulcerations with smooth, distinct margins rather than intact bullae (unbroken blisters).
What might you notice?
What it looks like
On the skin, lesions begin as multiple tense bullae, firm, fluid-filled blisters that sit on either normal-looking skin or on a patch of redness. They are typically distributed over the trunk, arms, and legs. After a few days, the blisters rupture, leaving raw or crusted areas that go on to heal without scarring. Many patients describe an itchy, hive-like or red rash that comes before the blisters appear.
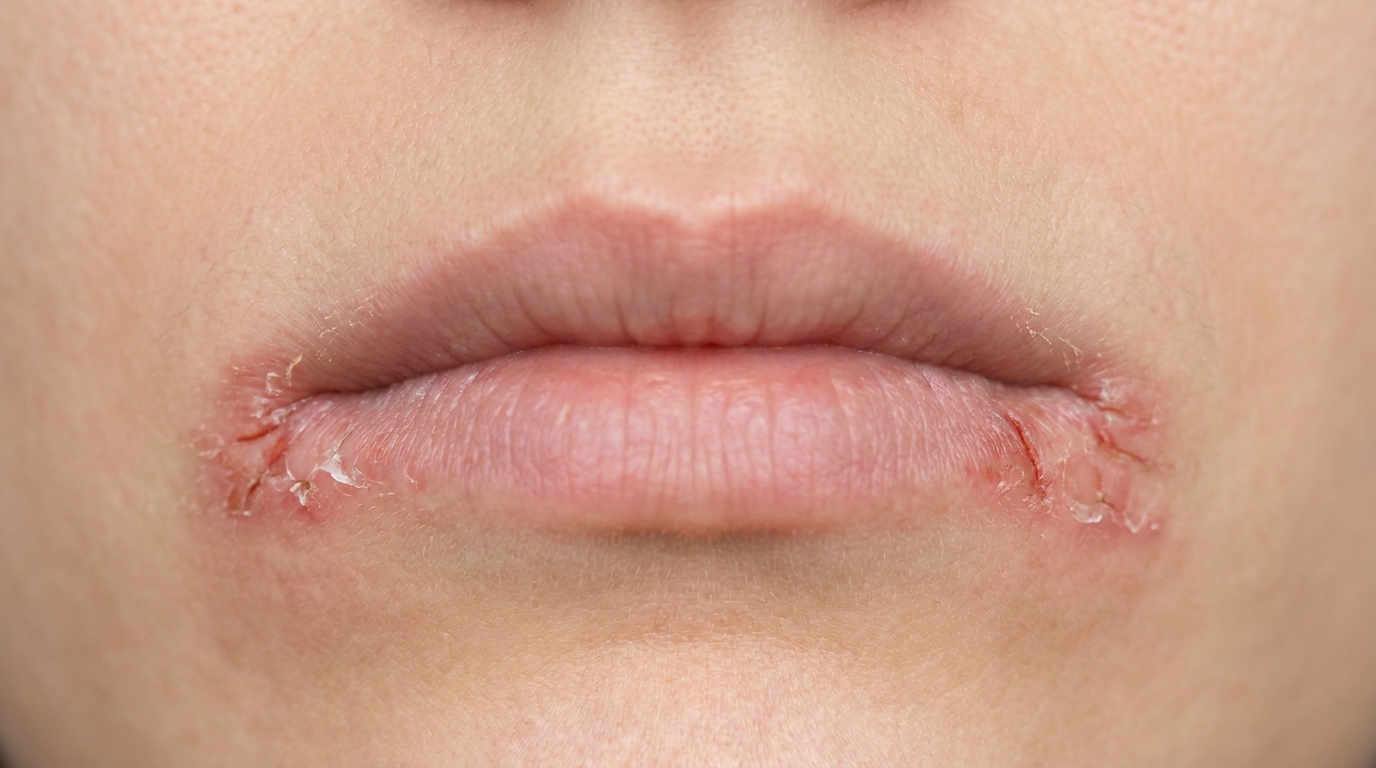
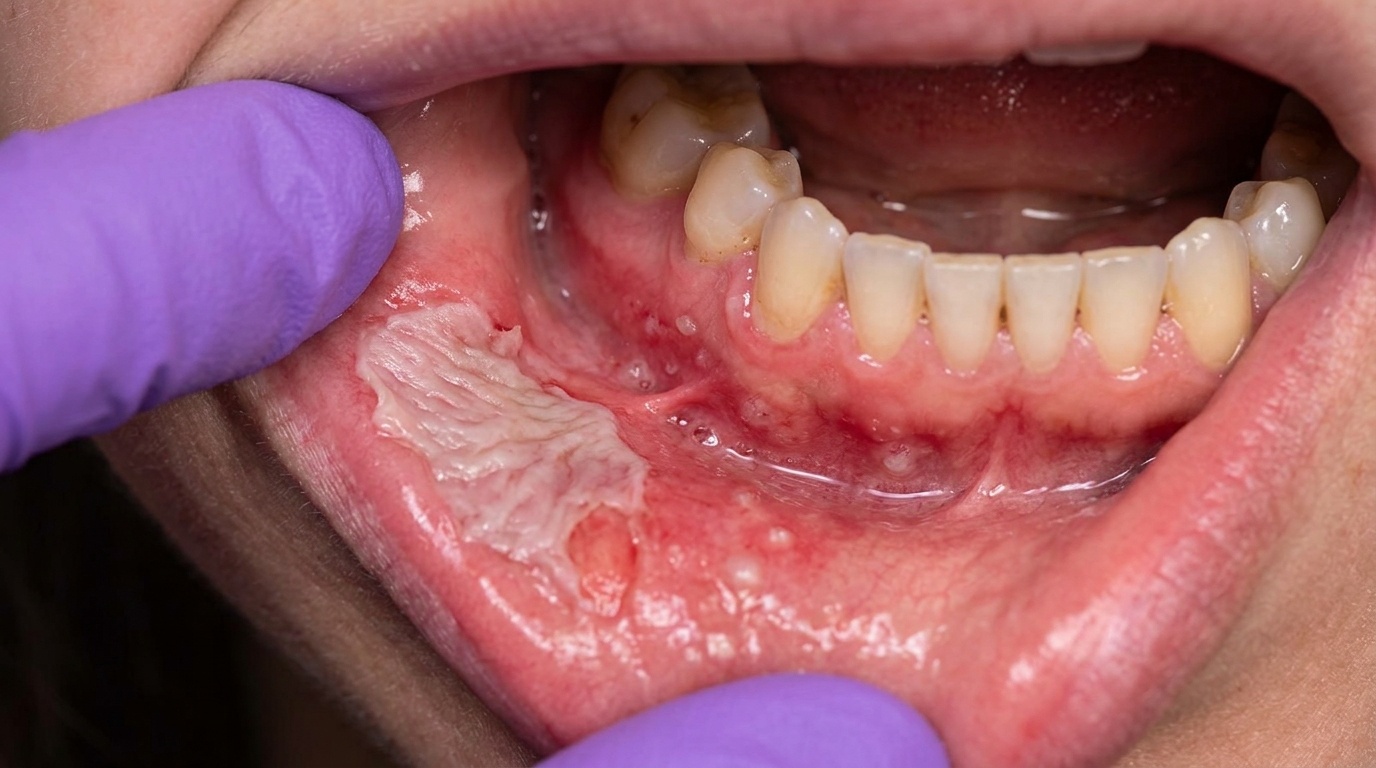
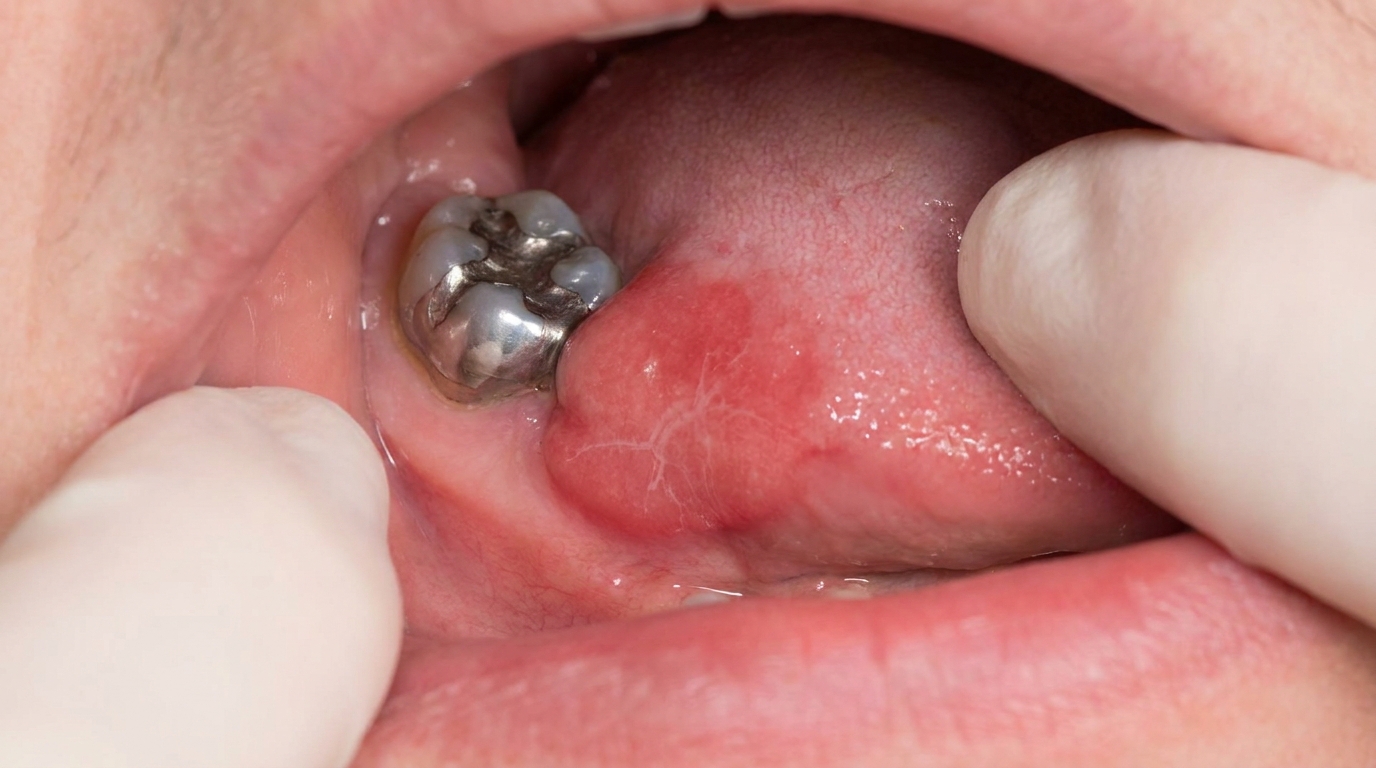
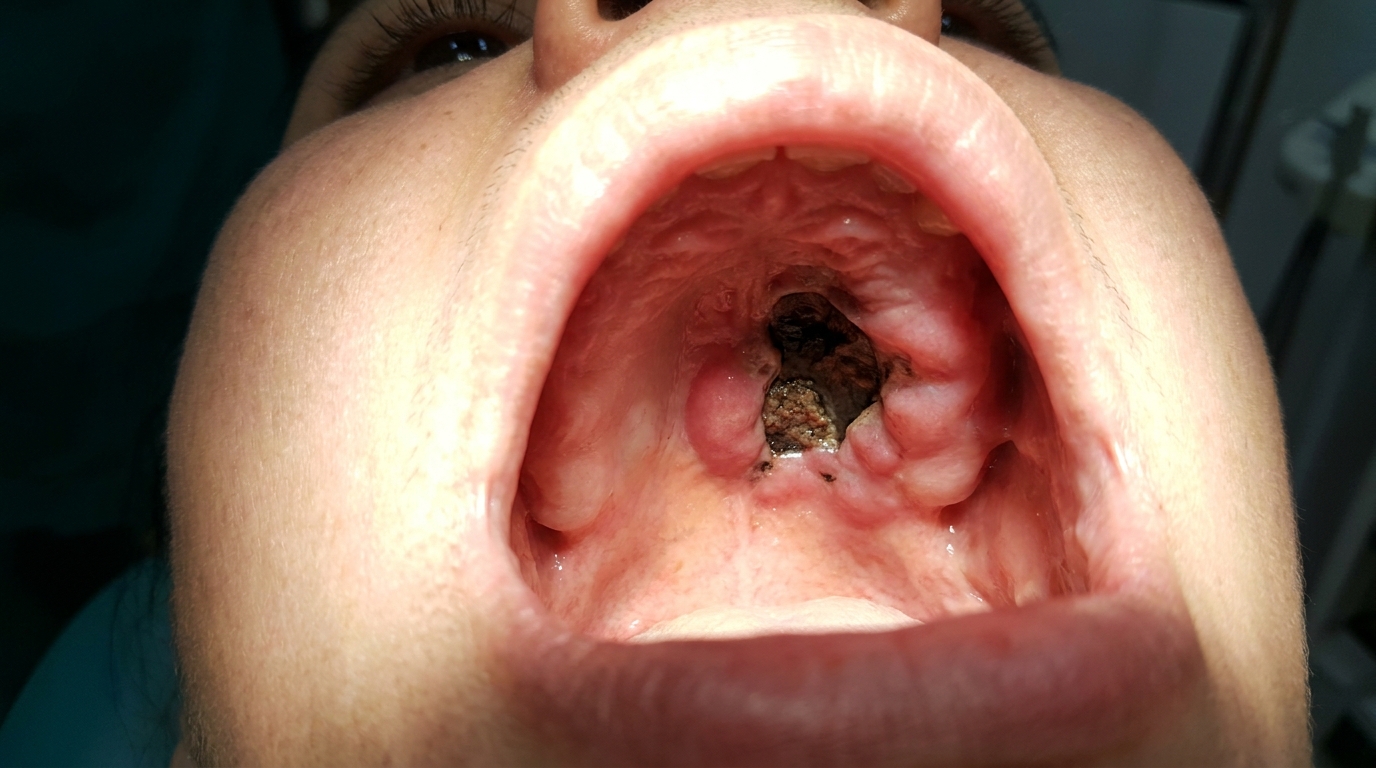
In the mouth, you may notice large, shallow ulcerations with smooth borders, most commonly on the soft palate, the inside of the cheeks, the tongue, the lower lip, or the gums. Occasionally the gums look red, raw, and peeling, a pattern dentists call desquamative gingivitis (the gum surface peels and reddens, looking sore and raw).
What it feels like
Intense itch is often one of the earliest skin symptoms, sometimes appearing weeks before any blister is visible. Once the blisters develop and rupture, the affected skin can be tender or sore, especially when clothing rubs against it.
Mouth lesions tend to be uncomfortable to painful, particularly when eating spicy, acidic, or hot foods. Brushing can also feel sore if the gums are involved. Some people find it harder to maintain their usual oral hygiene routine because of this discomfort.
What an X-ray might show
Dental X-rays do not show bullous pemphigoid, it is a soft-tissue, immune-mediated disease and leaves no signature on imaging. Diagnosis depends on the clinical appearance plus laboratory tests on a small biopsy sample.
What happens at the dentist?
Your dentist at ArtSmiles may be one of the first health professionals to spot oral changes, especially if mouth ulcers appear before any obvious skin disease. The assessment usually starts with a careful look at the lips, gums, palate, cheeks, and tongue, along with questions about how long the lesions have been there, whether the skin is also affected, and whether you have noticed any itching elsewhere.
If an autoimmune blistering disease is suspected, a small biopsy (a tissue sample taken with local anaesthetic and sent to the lab) of the affected mucosa is usually recommended.
A blood test called indirect immunofluorescence (a blood test for the same antibodies) may also be requested, which can detect circulating autoantibodies (antibodies travelling in the bloodstream) in 50% to 90% of cases. Your dentist will typically refer you to a dermatologist or oral medicine specialist for ongoing management, while continuing to look after the dental side of things, gentle hygiene, monitoring for medication side effects, and managing any flare-ups that affect the gums.
Is this serious?
🔴 Bullous pemphigoid is a serious condition that needs prompt medical attention, but for most patients it is controllable rather than dangerous in itself.
The skin disease is generally responsive to treatment, and many patients experience long periods of remission. The clinical course in bullous pemphigoid is typically marked by periods of relapse and remission rather than steady worsening.
The more concerning issue is that the condition mostly affects older adults, and the immunosuppressive medications (drugs that dampen down the immune system) used to treat it can carry their own risks in this age group. Larger studies have noted higher mortality rates in patients with bullous pemphigoid compared with age- and sex-matched populations, with the medications and the patient's overall health both playing a role. This is why treatment is usually individualised, balancing disease control against medication-related risks.
If you've noticed any of these signs for more than two weeks, it's worth booking an assessment.
Could it be something else?
Several other conditions can produce blisters or ulcers that look similar to bullous pemphigoid. Your dentist or doctor will work through these as part of the diagnostic process.
Mucous membrane pemphigoid (MMP), closely related, with the same kind of subepithelial split and similar immunofluorescence pattern, and sometimes indistinguishable from bullous pemphigoid in the mouth alone. The key difference is distribution: MMP is mucosa-dominant (mouth, eyes, genitals) with little or no skin involvement, runs a more protracted and progressive course, and can cause scarring of the eye that risks blindness if untreated.
Pemphigus vulgaris, also produces blisters and oral ulcers, often with the mouth as the first site involved. The blisters in pemphigus vulgaris are flaccid (not tense) because the split is intraepithelial (within the surface lining) rather than subepithelial (beneath the surface lining). Direct immunofluorescence shows IgG bound between the cells of the epithelium, not along the basement membrane.
Dermatitis herpetiformis, an itchy, blistering skin disease linked to gluten sensitivity. Typically affects younger and middle-aged adults rather than the elderly, lesions are grouped and intensely itchy on the elbows, knees, and buttocks, and immunofluorescence shows granular IgA at the tips of the dermal papillae (a different antibody pattern in the skin) rather than a linear IgG/C3 band.
Linear IgA disease, another subepithelial blistering condition that often involves both skin and mucous membranes. Distinguished by a linear band of IgA (rather than IgG and C3) along the basement membrane on direct immunofluorescence.
Epidermolysis bullosa acquisita, a rare autoimmune blistering disease where blisters form at sites of mechanical trauma and heal with scarring. Distinguished on biopsy by IgG deposits below the basement membrane and antibodies to type VII collagen.
Erythema multiforme, a blistering, ulcerative condition that can affect mouth and skin, but usually appears in younger adults, has an acute onset linked to herpes simplex infection or certain drugs, and shows characteristic target-shaped skin lesions rather than tense bullae.
Erosive lichen planus, a chronic inflammatory disease that can produce oral erosions and desquamative gingivitis. Distinguished by fine, lace-like white lines (white lacy striae) alongside the raw, eroded patches, a different biopsy appearance, and the absence of the linear IgG/C3 band on direct immunofluorescence.
Discoid lupus erythematosus, can cause oral ulcers and is sometimes considered alongside autoimmune blistering diseases. Distinguished by its characteristic skin lesions, autoantibody profile on blood tests, and a different immunofluorescence pattern.
How is it treated?
Bullous pemphigoid is usually managed by a dermatologist, with your dentist involved if the mouth is affected. Treatment is tailored to how widespread and severe the disease is.
For mild or localised disease, treatment may include strong topical corticosteroid preparations applied to the affected skin or, when the mouth is involved, topical steroid gels or rinses used under dental supervision. Custom flexible mouth trays are sometimes made to hold topical medication against the gums.
For moderate to severe or widespread disease, a doctor may recommend systemic corticosteroids such as prednisone, often starting at moderate daily doses and tapering to alternate-day therapy once the disease is controlled. If steroids alone are not enough, or if side effects become a concern, additional steroid-sparing medications may be added. These can include azathioprine, methotrexate, mycophenolate mofetil, dapsone, or in resistant cases, the monoclonal antibody rituximab (a targeted antibody-based treatment that calms the misbehaving immune cells). The combination of tetracycline (or doxycycline) and niacinamide is also reported to be helpful for some patients, particularly those who cannot tolerate stronger immunosuppressants.
At home, supportive measures include gentle skin care, avoiding trauma to blistered areas, and maintaining careful oral hygiene if the mouth is affected. Soft-bristled toothbrushes, alcohol-free mouthwashes, and avoiding spicy or acidic foods during flares can all help. Regular dental review is important, both to monitor the oral lesions and to look out for medication side effects such as oral thrush (a fungal infection in the mouth).
What's the long-term outlook?
The outlook for skin disease in bullous pemphigoid is generally good. Many patients respond well to treatment and experience remissions, and lesions typically heal without scarring. The course is usually one of relapses and remissions rather than continuous worsening.
That said, it is a chronic condition, and most people will need long-term medical follow-up. The biggest long-term risks come not from the disease itself but from the immunosuppressive medications used to treat it, especially in older adults. Working closely with both a dermatologist and your dentist helps balance disease control with overall health.
When the mouth is involved, oral lesions often respond well alongside the skin disease, and unlike mucous membrane pemphigoid, scarring of the mucosa is generally not a feature. Keeping up with regular dental check-ups during treatment helps catch flare-ups early and supports comfortable, healthy oral function over the long term.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
References
Regezi, J. A., Sciubba, J. J., & Jordan, R. C. K. (2017). Oral pathology: Clinical pathologic correlations (7th ed.). Elsevier. Chapter 1, Vesiculobullous Diseases (Bullous Pemphigoid), pp. 17,20.
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2023). Oral and maxillofacial pathology (5th ed.). Elsevier. Chapter 16, Dermatologic Diseases (Bullous Pemphigoid), pp. 779,781.
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 13, Diseases of the Oral Mucosa: Non-Infective Stomatitis (Subtypes of Pemphigoid, Appendix 13.3, Bullous Pemphigoid), p. 243.
Laskaris, G. (2003). Color atlas of oral diseases (3rd ed.). Thieme. Chapter 22, Skin Diseases (Bullous Pemphigoid), pp. 210,212.
Frequently asked questions
What is bullous pemphigoid?
Bullous pemphigoid is an autoimmune blistering disease that mainly affects elderly people. Antibodies attack proteins (BP180 and BP230) at the basement membrane of the skin, producing large, tense, fluid-filled blisters on red, itchy skin. Oral involvement is uncommon (about 10-30% of cases) but when it occurs causes ulcers and erosions on the lining of the mouth.
How is it different from pemphigus vulgaris?
Pemphigus vulgaris almost always involves the mouth first and produces fragile, easily ruptured blisters because the split is high in the epithelium. Bullous pemphigoid mainly affects the skin, produces large tense blisters because the split is deeper (subepithelial), and the mouth is less commonly involved. Direct immunofluorescence and serology distinguish the two reliably.
How is it diagnosed?
Diagnosis combines characteristic clinical features (tense blisters, elderly patient), biopsy of perilesional tissue for routine histology and direct immunofluorescence (showing linear IgG and C3 along the basement membrane), and serum testing for BP180 and BP230 antibodies (indirect immunofluorescence or ELISA).
How is bullous pemphigoid treated?
Treatment is shared between the dermatologist and the dentist if the mouth is involved. Mild cases respond to potent topical corticosteroids. Moderate-to-severe cases need systemic corticosteroids (prednisolone), often combined with steroid-sparing agents (azathioprine, methotrexate, mycophenolate, dapsone) or biologics (rituximab) in resistant cases. Oral lesions usually improve with the systemic treatment but may need topical steroids and bland mouthrinses for symptomatic relief.