Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker, Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | Leukoplakia of the floor of mouth, ventrolateral (the side and underside of the tongue) tongue leukoplakia, U-zone white patch |
How urgent? | 🔴 Important, a white patch in this high-risk zone deserves prompt biopsy and follow-up |
Common or rare? | Uncommon, but a high-risk subtype with malignant transformation reported up to 25 to 35% in some series |
Who it affects | Adults over 40, more often men, particularly heavy smokers and those who combine smoking with alcohol |
Who treats it | General dentist for identification and urgent referral; oral medicine specialist or oral and maxillofacial surgeon for biopsy and ongoing surveillance |
Based on | Neville, Cawson and Regezi |
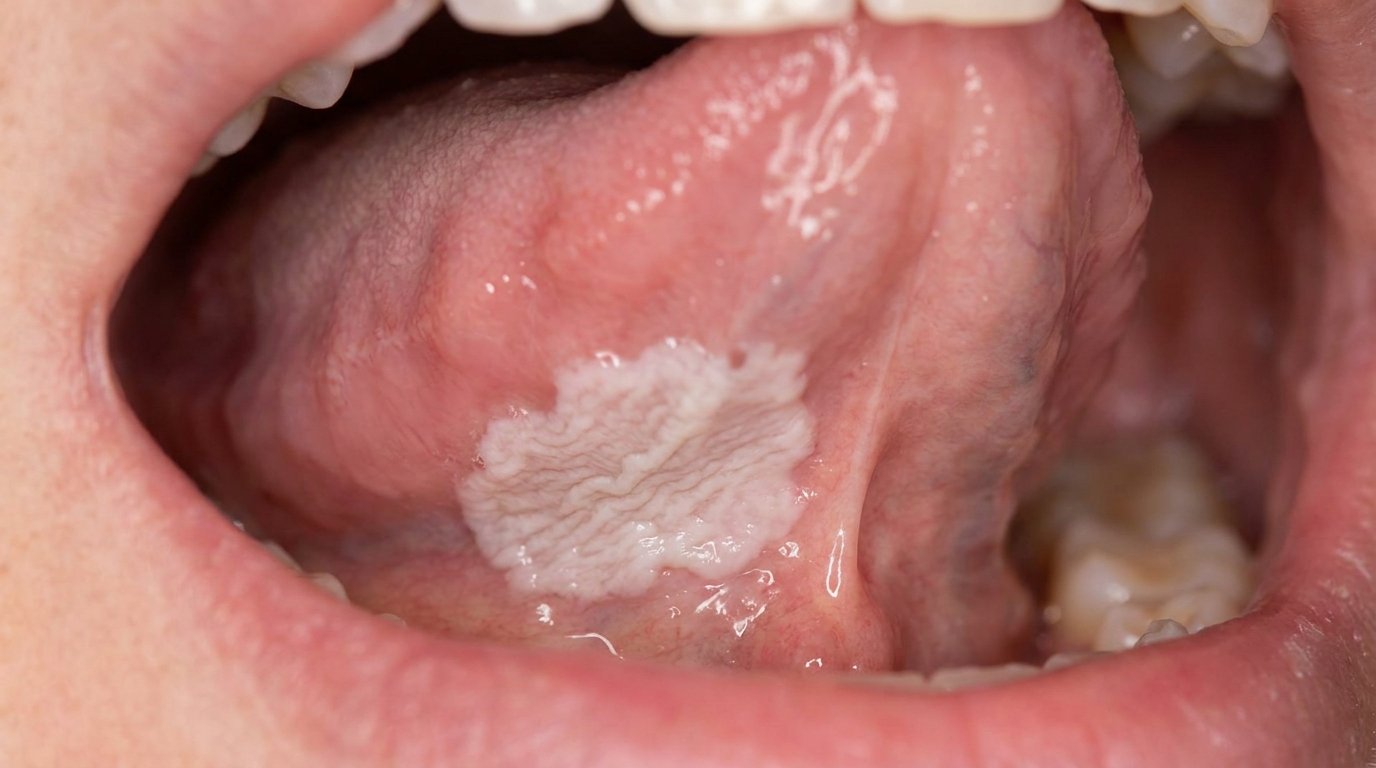
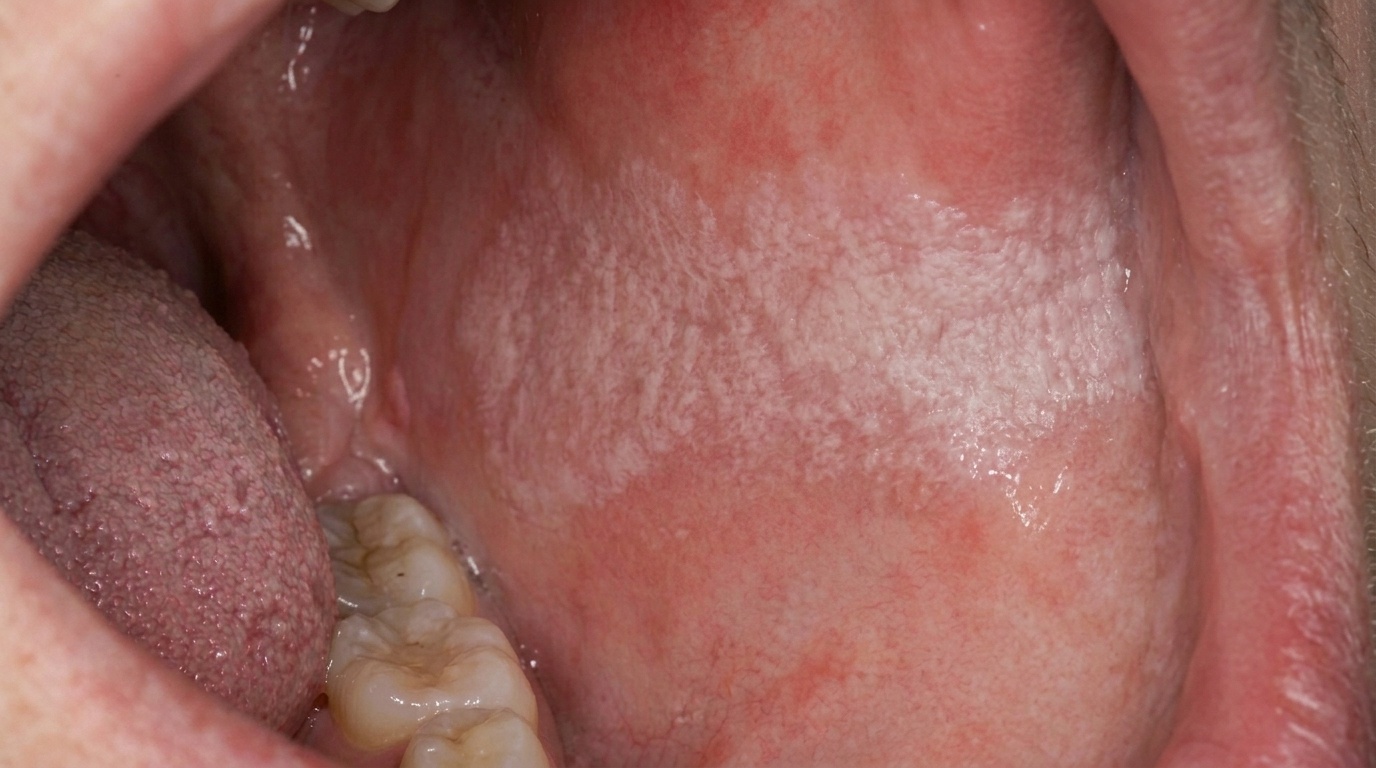
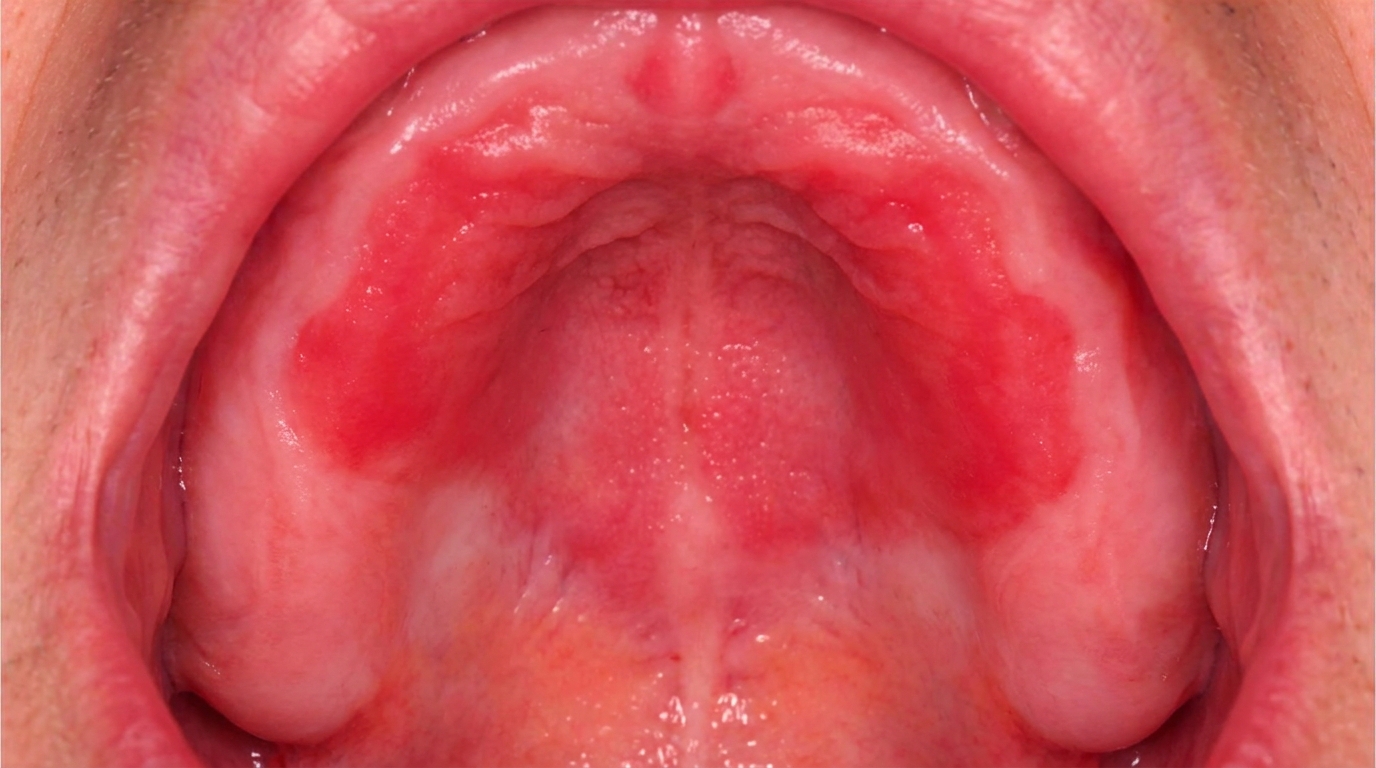
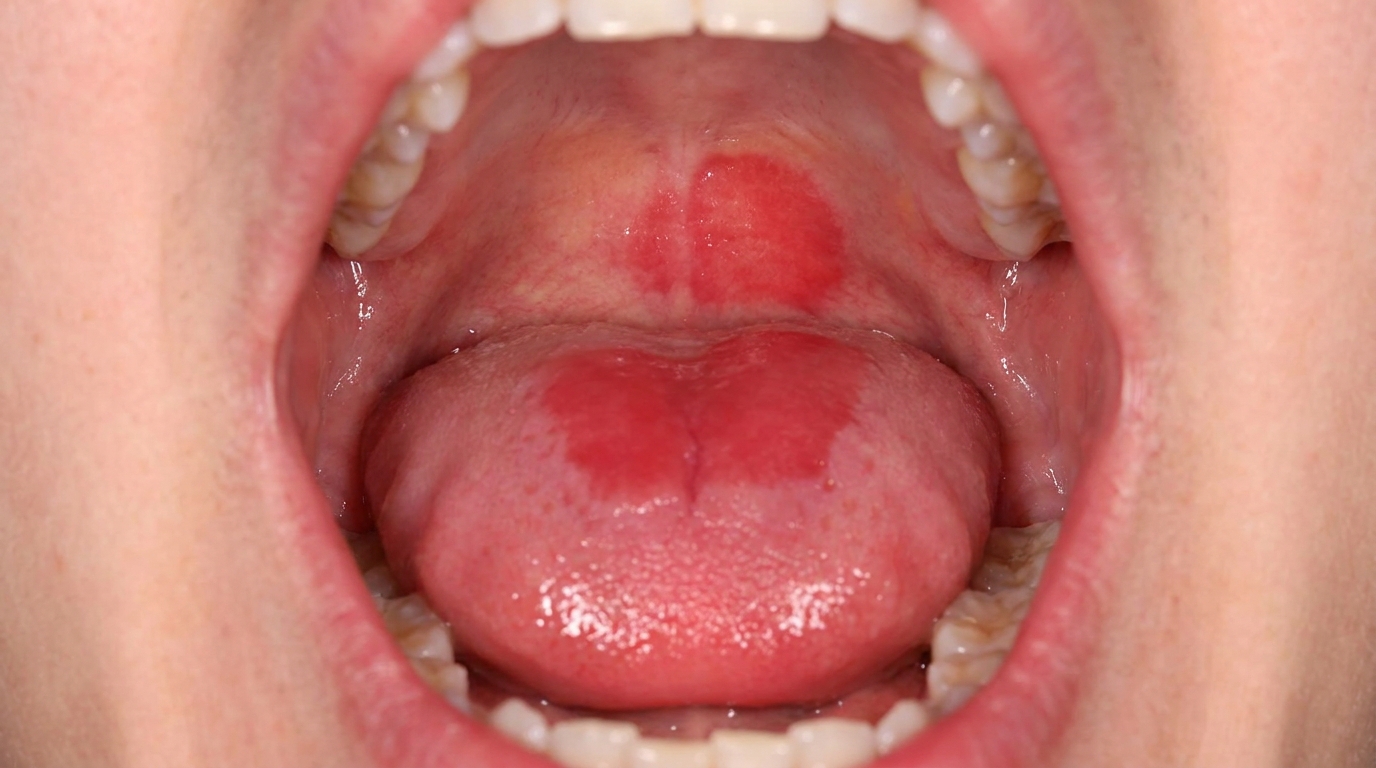
A small, white, slightly wrinkled patch on the underside of the tongue or on the floor of the mouth often goes unnoticed, but it is one of the most important findings a dentist can identify. Sublingual keratosis is a white patch in this high-risk zone, and it carries one of the highest rates of progression to oral cancer of any oral lesion.
This article from the team at ArtSmiles, reviewed by Dr Cristian Dunker, explains what sublingual keratosis is, why the location matters so much, and what to expect at a dental visit.
What is it?
Sublingual keratosis is a particular pattern of oral leukoplakia (a persistent white patch that cannot be rubbed off) located in the sublingual region, the floor of the mouth and the underside of the tongue. The classic features include:
A white, well-defined plaque that may be flat or slightly raised.
A surface texture often described as "ebbing tide", finely corrugated, with shallow lines that resemble sand left behind by a receding wave.
Soft to mildly leathery consistency, not warty or verrucous.
Asymptomatic in most cases, patients are not in pain and may have noticed nothing.
Located in the U-shaped high-risk zone of the mouth.
The microscopic features can range from simple thickening of the keratin layer (low risk) through to severe dysplasia (microscopic changes that can signal an increased cancer risk) or carcinoma in situ (early cancer confined to the surface layer) (high risk). The clinical appearance alone does not tell us where on this spectrum a particular lesion lies, that is why biopsy is essential.
Who tends to get it?
Sublingual keratosis can occur in any adult but is more common in:
Older adults, with most cases diagnosed after 40 years of age.
Men more often than women, in some series.
Smokers, particularly long-term and heavy smokers.
Patients with significant alcohol intake, especially when combined with smoking.
Patients with previous oral cancer or pre-cancer.
Patients with chronic mucosal conditions such as oral lichen planus.
What causes it?
The condition results from chronic injury to the lining of the floor of the mouth and underside of the tongue, typically from one or more of:
Tobacco in any form.
Alcohol, particularly with concurrent smoking.
Areca nut and betel quid in some communities.
Chronic irritation from sharp teeth, fillings or partial dentures.
Oncogenic HPV strains in some cases.
Genetic susceptibility in patients without obvious lifestyle risk factors.
The thin, non-keratinised (without the usual protective keratin layer) lining of this area is particularly susceptible to chemical and mechanical injury. The result is a white change that, in some patients, becomes the platform for cellular abnormality and eventual cancer.
How does it develop?
The course is typically slow:
Repeated injury or chemical insult activates the lining.
Cells in the area produce a thicker keratin layer in protection.
The patch becomes visible as a small, often unnoticed white area.
Over months and years, some patches enlarge, develop red components, ulcerate or become verrucous.
Dysplastic changes appear in the cells in some patients.
Without intervention, a proportion of these progress to squamous cell carcinoma.
Estimates of malignant transformation for sublingual keratosis run as high as 25 to 35% in some series, far higher than for white patches at most other oral sites, which is why aggressive surveillance is recommended.
What might you notice?
In many patients, nothing at all. The patch is found incidentally during a check-up or oral cancer screening. Some patients may notice:
A small white patch seen in the mirror under the tongue.
A rough or slightly different texture noticed by the tongue tip.
No pain, no ulceration in most early cases.
Mild discomfort or burning with spicy or acidic food in some patients.
A new red component appearing within or alongside a long-standing white patch (an important warning sign).
If a white patch in this area has been present for more than two weeks and cannot be wiped off, it should be examined by a dentist.
What an X-ray might show
Sublingual keratosis is confined to the surface lining and does not show on routine X-rays. Imaging may be considered if a transformed area extends into the floor of the mouth, the sublingual gland or the underlying bone.
What happens at the dentist?
When sublingual keratosis is identified at ArtSmiles, the visit usually involves:
A thorough history, including smoking, alcohol, areca nut use, occupational exposures and any previous oral pathology.
A careful intraoral examination of all soft tissues, with particular attention to the floor of mouth, ventral tongue, lateral tongue and soft palate.
Photography to document the appearance and size.
Identification of any contributing local factor (sharp tooth, ill-fitting denture).
Urgent referral to an oral medicine specialist or oral and maxillofacial surgeon for biopsy.
Communication with your GP as needed, particularly when smoking cessation or general health support is required.
A clear long-term plan built around the biopsy result.
Is this serious?
Sublingual keratosis is one of the more serious benign-appearing lesions of the mouth because:
High malignant transformation rate, among the highest of any oral leukoplakia subtype.
Often silent, patients have no symptoms and may not seek care for years.
Difficult location, the floor of the mouth is harder to see at home and is a common cancer site.
Coexisting risk factors are usually present, increasing background cancer risk.
The strong message is that any white patch in this location deserves prompt assessment, biopsy and follow-up, even if it looks innocent.
Could it be something else?
Other white changes that can occur in this area include:
Frictional keratosis from a sharp tooth or denture, which usually resolves once the irritant is removed.
Oral lichen planus, often with characteristic lacy striations elsewhere in the mouth.
Chronic hyperplastic candidiasis, often responsive to antifungal therapy.
White sponge naevus, a hereditary, soft and folded white change present from a young age.
Verrucous leukoplakia, with a wartier surface and possibly the same site.
Squamous cell carcinoma, which may present as a mixed white and red patch with ulceration.
Biopsy is the only reliable way to tell these apart.
How is it treated?
Treatment depends on the biopsy result and clinical features:
Mild to moderate dysplasia in a small lesion, surgical removal (excision or laser ablation), with regular follow-up.
Severe dysplasia or carcinoma in situ, surgical removal under specialist care.
Squamous cell carcinoma, managed by a head and neck cancer team with surgery and (sometimes) radiotherapy.
Lifestyle changes, smoking cessation, alcohol reduction, areca nut cessation, all strongly recommended.
Long-term follow-up at three- to six-month intervals with experienced clinicians.
Vitamin and antioxidant supplements have been studied but are not consistently effective.
The dentist's role is to identify the lesion, refer appropriately, support lifestyle changes and remain part of the long-term review team.
What's the long-term outlook?
The long-term outlook depends on the histology (the microscopic appearance of tissue) at biopsy and on whether risk factors can be reduced. Patients with low-grade lesions who stop smoking, limit alcohol and attend regular follow-up generally have good outcomes. Those who continue heavy smoking, do not reduce alcohol, or are lost to follow-up have a much higher chance of progression.
The most important step is the first appointment, early identification and biopsy. From there, a structured plan can keep the situation in hand.
If you have noticed a white patch under your tongue or in the floor of your mouth that has been there for more than two weeks, please book an appointment without delay. We will give you a clear picture and arrange the right specialist input quickly.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
The cover image above is an AI-generated illustration based on the most common visible features of this condition described in clinical pathology references. It is not a photograph of a real case and should not be used to diagnose or rule out the condition in your own situation. If you are concerned about something you have noticed, please book an assessment with a registered dental practitioner.
References
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2016). Oral and maxillofacial pathology (4th ed., Ch. 10: Epithelial Pathology, Leukoplakia). Elsevier.
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed., Ch. 16: Premalignant Conditions, Sublingual Keratosis). Elsevier.
Regezi, J. A., Sciubba, J. J., & Jordan, R. C. K. (2017). Oral pathology: clinical pathologic correlations (7th ed., Ch. 3: Red and White Lesions). Elsevier.
Frequently asked questions
What is sublingual keratosis?
Sublingual keratosis is a white patch on the underside of the tongue or floor of the mouth, with a sharply demarcated, slightly irregular, sometimes wrinkled surface. It belongs in the leukoplakia family but the floor-of-the-mouth location carries a particularly high cancer-change risk.
Why is the floor of the mouth a high-risk site?
The floor of the mouth and the underside of the tongue are the highest-risk sites for malignant transformation of white patches. Carcinogenic substances dissolved in saliva pool here, and the thin overlying lining offers less mechanical protection than the cheek. Any white patch in these sites should be biopsied.
How is it diagnosed?
Diagnosis requires a biopsy of the patch. Toluidine blue staining and brush biopsy can help target the most suspicious area within a larger lesion. Photographs and careful mapping are essential because lesions often recur.
How is sublingual keratosis treated?
Treatment depends on the histology. Lesions without dysplasia are usually monitored closely, with absolute cessation of smoking and alcohol. Dysplasia, especially moderate or severe, is treated with surgical excision or laser. Lifelong follow-up is recommended because recurrence is common.