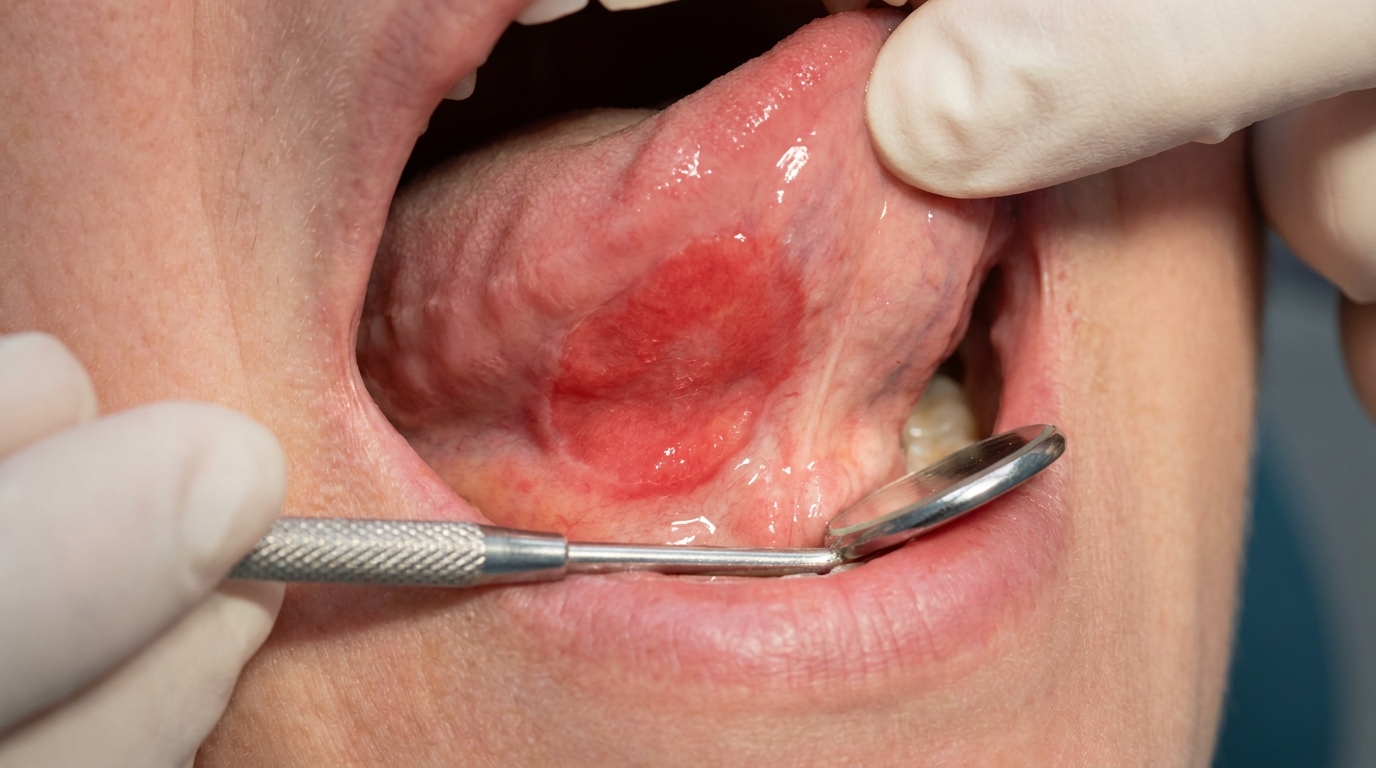
Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker , Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | Cannon's disease, white sponge nevus, familial white folded dysplasia (microscopic changes that can signal an increased cancer risk) |
How urgent? | 🟢 Not dangerous, benign, hereditary, and does not progress to cancer |
Common or rare? | Uncommon, but distinctive enough that it is usually recognised once it has been seen |
Who it affects | Anyone with the inherited keratin (the protective protein in the surface lining) gene change, typically present from birth or early childhood and stable into adulthood; affected people often have a family history |
Who treats it | General dentist for diagnosis and reassurance; no treatment is required |
Based on | Cawson, Laskaris, with cross-references in Neville |
What is it?
White sponge naevus is a benign, inherited condition in which the lining of the mouth (and sometimes other mucosal surfaces) develops a thick, soft, spongy white appearance. The textbooks describe it as a developmental anomaly inherited as an autosomal dominant (passed from parent to child with a 50% chance each pregnancy) trait, caused by mutations in keratin genes (chiefly K4 and K13) that affect how the surface cells of the mouth's lining hold together. The condition is also called Cannon's disease after the doctor who first reported it. Despite the dramatic appearance, white sponge naevus does not turn into cancer, does not cause discomfort, and does not need any specific treatment.
Who tends to get it?
The textbooks describe a fairly tight clinical group:
Anyone with the inherited keratin gene change. As an autosomal dominant trait, each child of an affected parent has a 50% chance of being affected.
Typically present from birth or early childhood, with the appearance becoming more obvious during adolescence.
Progressive until early adulthood and then stable for the rest of life.
Affects both sexes equally with no strong ethnic predilection.
Often noticed in multiple family members when one is identified, a strong family history is highly suggestive.
May also affect other mucosal surfaces such as the vagina, rectum and anal canal, although the mouth is the most commonly involved site.
What causes it?
The cause is well established:
Mutations in keratin genes K4 and K13. These genes code for the keratin proteins that are specific to the surface cells of the oral, vaginal, oesophageal and anal lining. When the proteins are abnormal, the cells do not stack and bind together as tightly as they should, producing the spongy, thickened appearance.
Autosomal dominant inheritance. The condition is passed down from parent to child with a 50% chance per pregnancy. New (sporadic) mutations also occur but are uncommon.
No environmental cause. White sponge naevus is not caused by smoking, biting, infection, food, oral hygiene or any habit. Once present, it is not affected by these factors either.
How does it develop?
The genetic change is present from conception, but the white sponge appearance develops gradually as the lining of the mouth matures. Typically the first changes are noticed in early childhood, with the lesions becoming more obvious through adolescence and reaching their stable adult appearance by the early twenties. Microscopically, the lining of the mouth is much thicker than normal, with abundant pale, swollen cells in the upper layers and a characteristic "basket-weave" pattern of intracellular oedema (fluid swelling inside the cells). Despite this dramatic-looking change under the microscope, there is no dysplasia, no inflammation, and no risk of malignant transformation.
What might you notice?
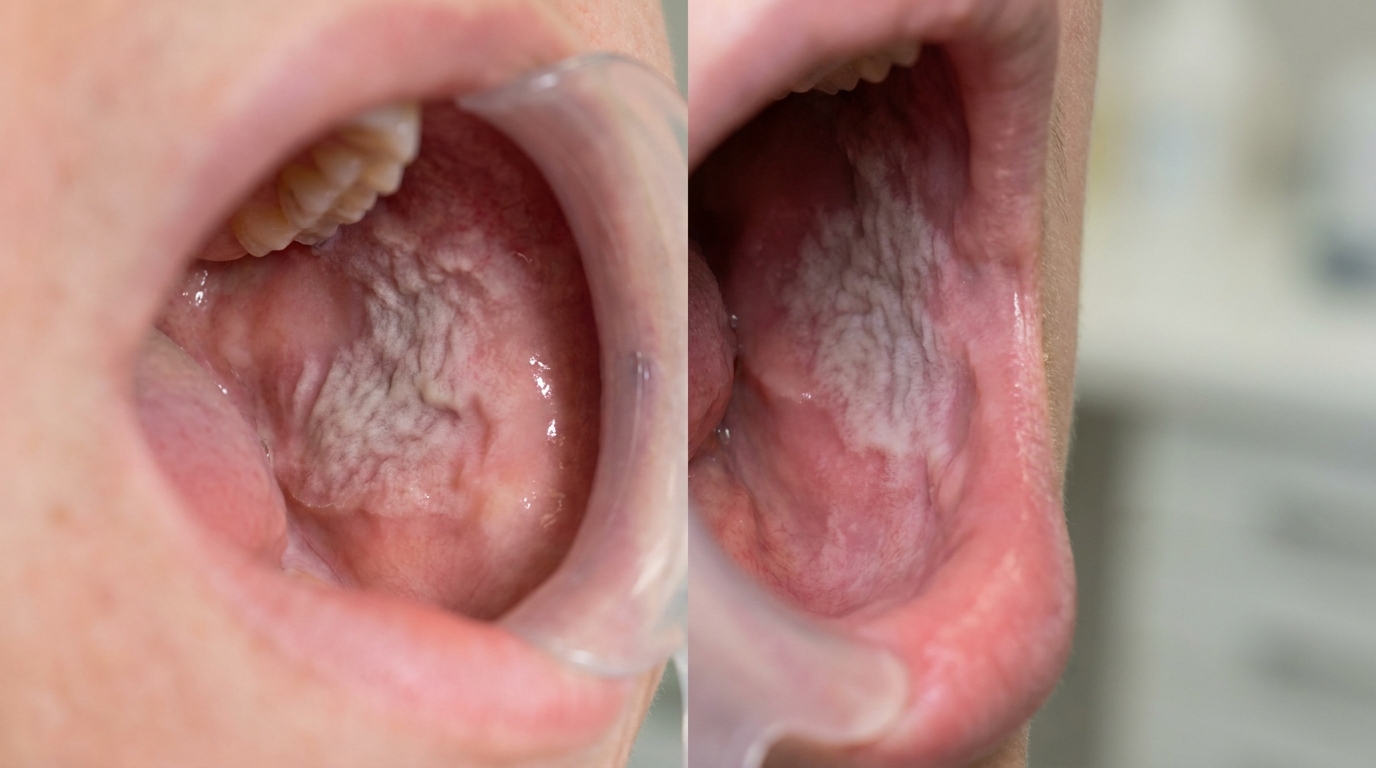
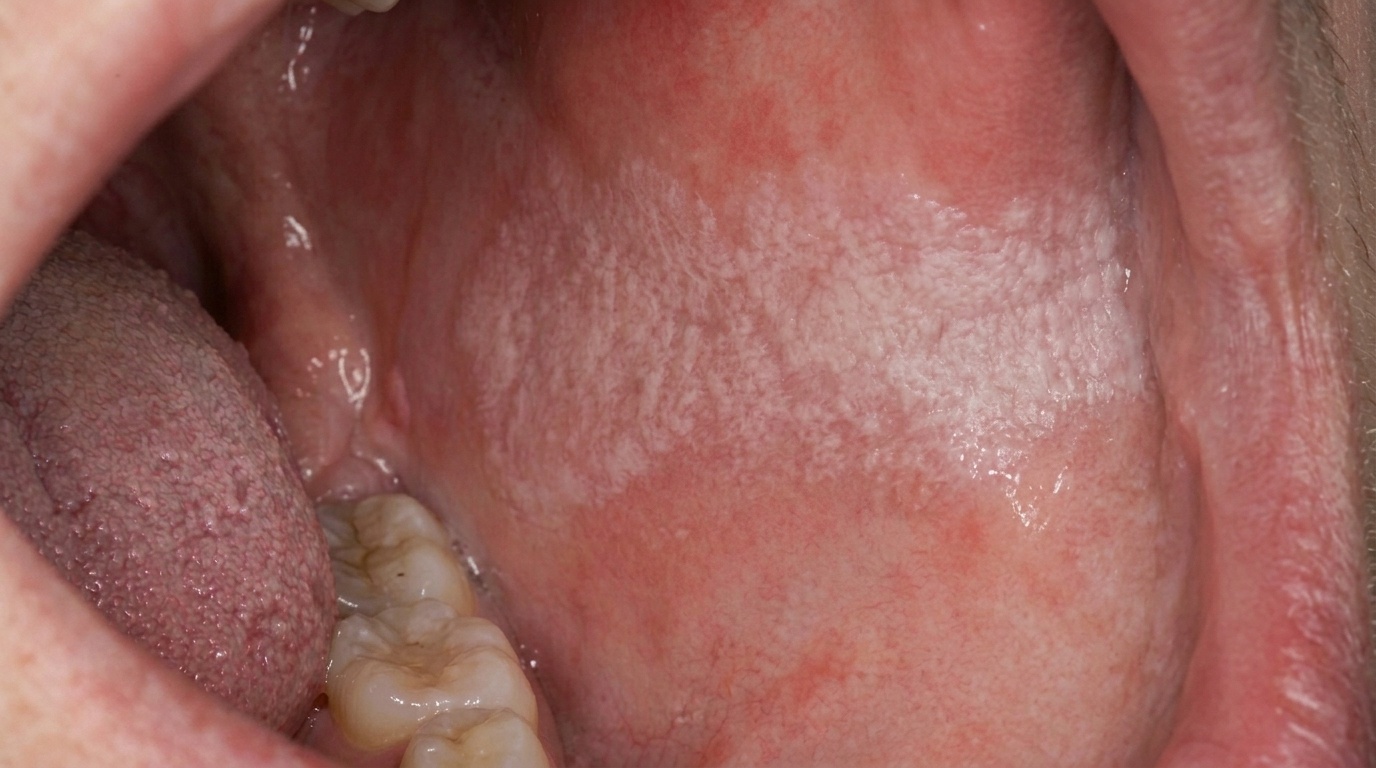
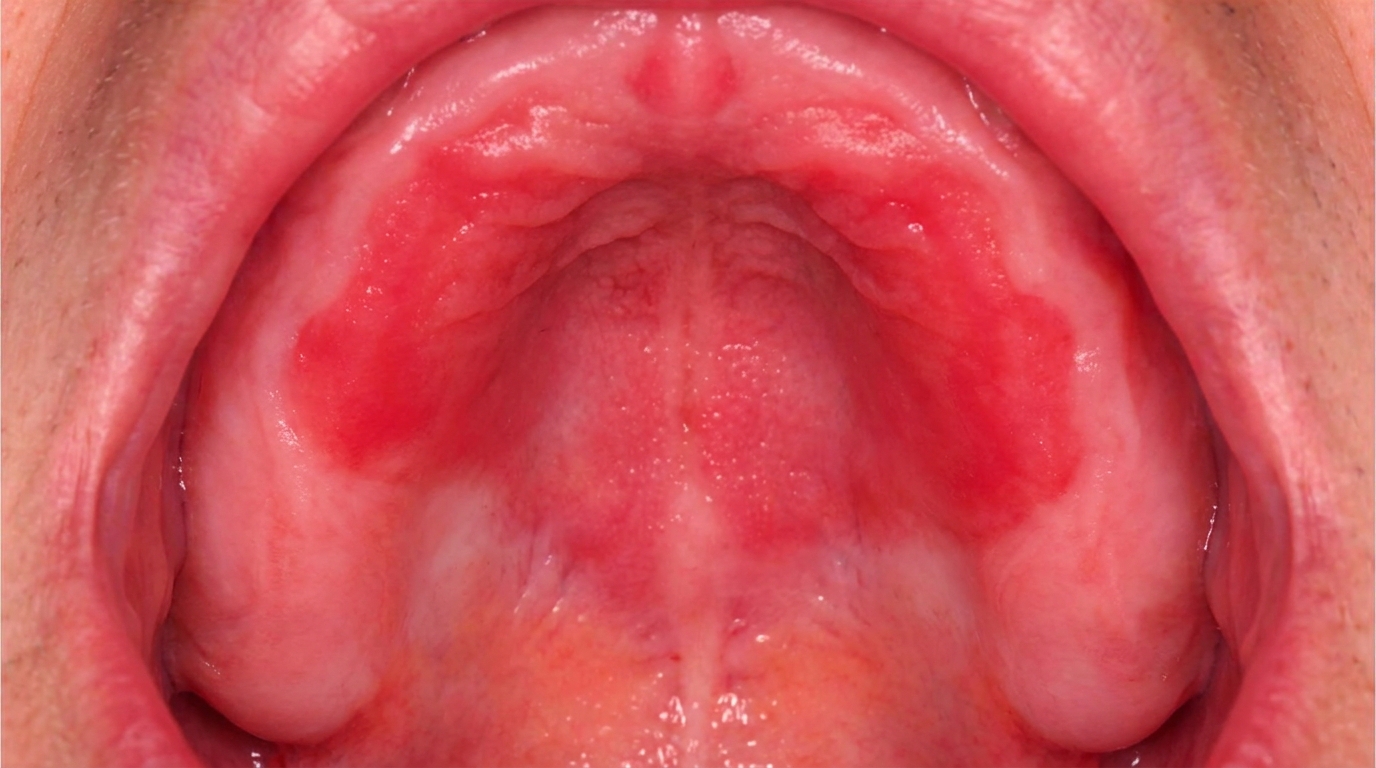
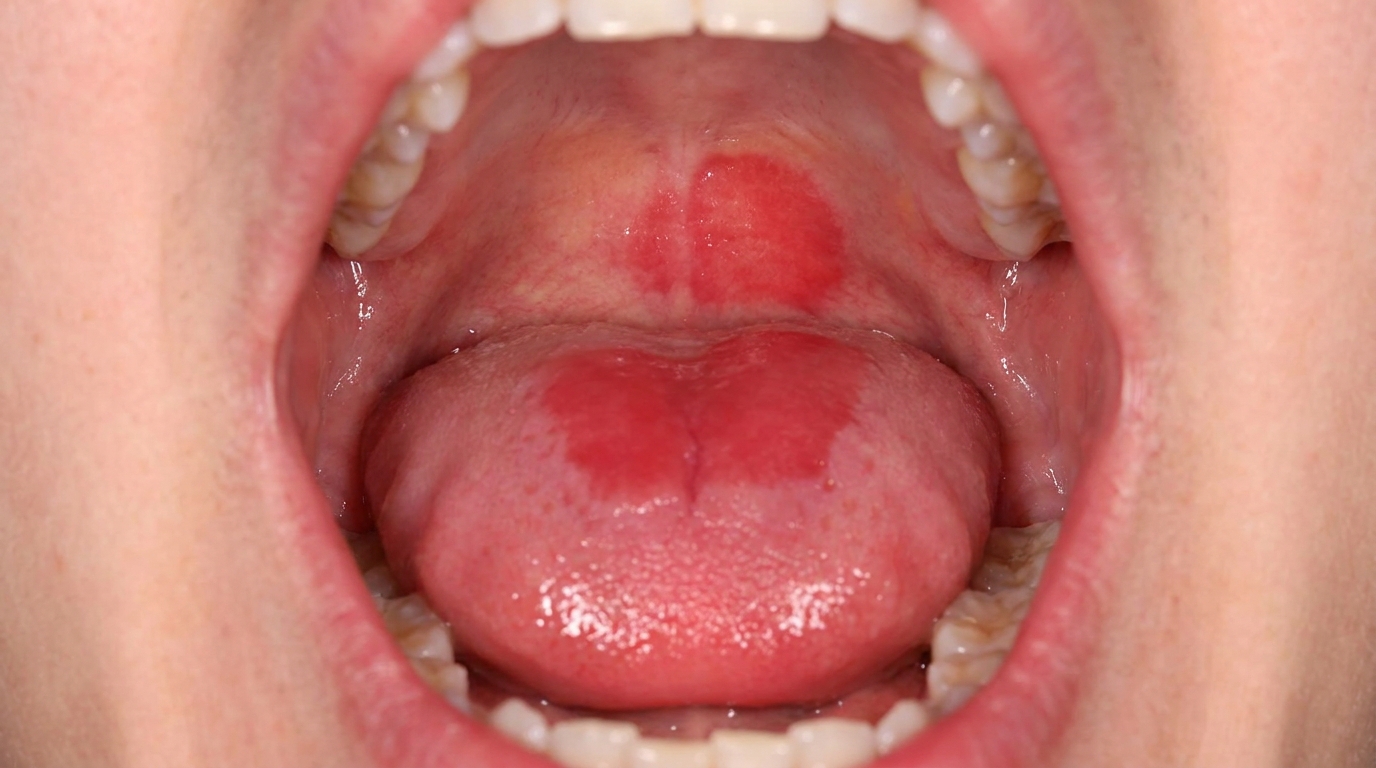
What it looks like
The textbooks describe a very distinctive appearance:
Soft, white, irregularly thickened lining of the mouth.
A shaggy, spongy or velvety texture, often with shallow folds and ridges.
The change is bilateral and symmetrical, both cheeks usually affected.
The borders are not sharply defined, the white patches fade gradually into normal-appearing mucosa.
The most commonly affected sites are the inside of the cheeks (buccal mucosa) and the underside of the tongue, although any non-keratinised (without the usual thicker protective surface layer) lining can be involved.
Peeling of the surface in fine sheets sometimes occurs, particularly with rubbing or after a meal.
Similar lesions may be present in the vaginal, rectal or anal mucosa in some patients.
What it feels like
White sponge naevus is essentially asymptomatic. Most patients:
Are unaware of the condition until a dentist or doctor points it out.
Notice no pain, soreness or discomfort.
May find that small flakes of soft white tissue come off when brushing, this is harmless surface peeling.
Have no taste change, no bleeding, and no functional limitation.
What an X-ray might show
X-rays are not used to diagnose white sponge naevus, the condition is confined to the soft-tissue lining and the diagnosis is made on appearance, family history and, where needed, biopsy.
What happens at the dentist?
White sponge naevus is most often picked up at a routine dental check-up and clean at ArtSmiles, sometimes at the patient's first visit, sometimes after years of being unnoticed. The dentist will typically:
Examine the mouth carefully, noting the bilateral and symmetrical pattern, the spongy texture, and the lack of sharp borders.
Take a careful history, asking when the patient first noticed the appearance and whether any close family members have similar findings.
Offer a biopsy in the rare cases where the diagnosis is unclear, particularly if the patient has no family history or if the lesion looks slightly different from the classic appearance. Biopsy reliably distinguishes white sponge naevus from idiopathic leukoplakia and other white patches.
Reassure that the condition is benign, hereditary, and does not progress to cancer.
Document the appearance with photographs as a baseline, particularly in younger patients where the appearance may evolve.
Is this serious?
🟢 White sponge naevus is benign. The textbooks specifically note that there is no dysplasia, no inflammation and no risk of malignant transformation. Reassurance is the central piece of management. Many patients have lived with the appearance for years without realising what it is, and clear explanation often comes as a relief.
If you have noticed soft white patches inside your mouth that have been present since childhood, particularly if other family members have a similar appearance, it is worth booking an assessment so the diagnosis can be confirmed and you can be reassured about what it is.
Could it be something else?
Several conditions can produce white patches in the mouth, and white sponge naevus is one of the more readily distinguished. The textbooks list these as the main differentials:
Idiopathic oral leukoplakia, usually appears later in life, in smokers, often as a single localised patch with sharper borders.
Leukoedema, a faint, milky-white change in the inside of the cheeks that disappears or fades when the cheek is stretched. The change in white sponge naevus persists with stretching.
Oral lichen planus, typically has fine white lacy lines (Wickham striae) and may be tender; usually develops later in life.
Hereditary benign intraepithelial dyskeratosis, a rare similar genetic condition that affects both the mouth and the eye, traditionally described in a North Carolina population. White sponge naevus does not affect the eye.
Frictional hyperkeratosis (cheek-biting line), a localised white line where the teeth contact the cheek, with a clear cause and asymmetrical distribution.
Pachyonychia congenita, a rare genetic condition with thickened nails, palmar,plantar keratoderma and oral white plaques.
How is it treated?
The textbooks all agree: white sponge naevus needs no specific treatment. The main management step is reassurance.
At-home measures and habits:
Continue normal oral hygiene, brushing twice a day with fluoride toothpaste and flossing daily.
No need to avoid any food, drink or habit because of the white sponge naevus itself.
Do not pick or scrape at the surface, although small flakes will sometimes come off, vigorous scraping is not necessary and may cause minor discomfort.
Professional steps your dentist may consider:
Confirming the diagnosis by clinical examination and family history. A biopsy is offered in the rare case where the diagnosis is uncertain.
Reassuring the patient that the condition is benign and stable.
Documenting the appearance with photographs, particularly in young patients, as a baseline for future reviews.
Genetic counselling for patients planning a family who would like to understand the inheritance pattern. Because the condition is autosomal dominant, each child has a 50% chance of inheriting it, and affected children will have a similar mild appearance with no health implications.
Continuing routine dental care without modification.
A patient-centred approach matters. People sometimes worry for years about a condition that turns out to be entirely benign. Calm, clear explanation of the genetic basis, the lack of risk, and the simple plan of "no treatment, just routine review" is itself part of effective care, values that sit at the heart of our clinical philosophy.
What's the long-term outlook?
The outlook is excellent. White sponge naevus is a stable, harmless, lifelong condition. The appearance reaches its adult pattern by early adulthood and then changes very little. There are no long-term consequences for general or oral health, and no special review is needed beyond routine dental check-ups. For patients who have lived for years wondering what the white patches in their mouth might mean, identifying white sponge naevus is usually the most important, and reassuring, step.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
The cover image above is an AI-generated illustration based on the most common visible features of this condition described in clinical pathology references. It is not a photograph of a real case and should not be used to diagnose or rule out the condition in your own situation. If you are concerned about something you have noticed, please book an assessment with a registered dental practitioner.
References
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 15, Soft Tissue Disease: White Sponge Naevus, with key features in Box 15.3, p. 256.
Laskaris, G. Pocket atlas of oral diseases. Thieme. Chapter 3, Genetic Diseases: White Sponge Nevus (Cannon's disease), with detailed clinical features and differential diagnosis, pp. 14 to 15.
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2023). Oral and maxillofacial pathology (5th ed.). Elsevier. Chapter 10, Epithelial Pathology: white sponge nevus listed as a key differential of leukoplakia.
Frequently asked questions
What is white sponge naevus?
White sponge naevus is a rare, inherited (autosomal dominant) condition where the lining of the mouth develops thick, white, spongy, folded patches. It usually appears in childhood or adolescence and affects multiple sites — most commonly the cheeks (buccal mucosa), tongue and floor of the mouth, often symmetrically.
Is white sponge naevus serious?
No. White sponge naevus is completely benign. It does not turn into cancer and does not cause pain or other health problems. The main concern is cosmetic and the worry it can cause when a patient or new dentist sees the patches for the first time.
How is it diagnosed?
Diagnosis is usually clinical based on the look and family history. A biopsy may be done to rule out other white patches like leukoplakia, lichen planus or hereditary benign intraepithelial dyskeratosis. Genetic testing for keratin gene mutations (KRT4, KRT13) can confirm the diagnosis in unclear cases.
Does white sponge naevus need treatment?
No specific treatment is needed because the condition is harmless. Some patients with troublesome secondary infection have reported improvement with tetracycline mouthwashes, but for most patients reassurance and routine dental check-ups are all that's required.