Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker , Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | PVL, proliferative leukoplakia |
How urgent? | 🔴 Serious, multiple slowly growing white patches with a high lifetime risk of progression to oral cancer; warrants specialist assessment and long-term surveillance |
Common or rare? | Rare and probably under-recognised; most pathology services see only a handful of cases each year |
Who it affects | Most often elderly women, with a male-to-female ratio of about 1:4; many patients are non-smokers, unusual for leukoplakia |
Who treats it | General dentist working with an oral medicine specialist or oral and maxillofacial surgeon for biopsies, treatment and lifelong surveillance |
Based on | Cawson, Neville, with cross-references in Regezi |
What is it?
Proliferative verrucous leukoplakia (PVL) is a particularly aggressive form of oral leukoplakia characterised by multiple, slowly spreading white patches that develop a rough, warty (verrucous) surface over time and tend to involve more than one site in the mouth. The textbooks describe PVL as inexorably progressive, the patches rarely regress with treatment and most cases eventually transform into oral squamous cell carcinoma. Because of this very high transformation rate, PVL is considered the highest-risk form of oral leukoplakia, even though it is rare overall.
Who tends to get it?
The textbooks describe a distinctive demographic profile that helps separate PVL from ordinary leukoplakia:
Elderly patients, typically over 60 at diagnosis.
Strong female predominance, Neville reports a male-to-female ratio of about 1:4. Cawson notes that "patients are elderly and mostly female".
Many patients are non-smokers, unlike most other forms of leukoplakia, where tobacco is the main driver. Tobacco association is minimal in PVL.
Multiple sites involved, common sites include the gingiva (gums), the buccal mucosa (inside of the cheek) and the tongue.
Long pre-existing history, patients often describe white patches in the mouth that have been present for years, sometimes decades, before diagnosis.
The cause of the female and non-smoker predominance is not well understood. Some studies have suggested a possible role for human papillomavirus (HPV), but the textbooks do not consider this proven.
What causes it?
The cause is unknown. Possible contributors discussed in the textbooks include:
Genetic susceptibility, accumulating molecular changes in the surface cells over many years.
Possible viral involvement, human papillomavirus (HPV) has been investigated as a potential factor, but the role is not yet clear.
Lack of strong tobacco association, unlike ordinary leukoplakia, where smoking and smokeless tobacco are major drivers, PVL frequently develops in non-smokers, which makes the disease particularly difficult to prevent.
Genuinely idiopathic in most cases, the textbooks describe PVL as "rather poorly defined" with no single, reproducible cause that explains all cases.
How does it develop?
The textbooks describe a slow, multistep evolution:
Phase 1, Simple flat hyperkeratosis (thickened keratin layer). The lesion begins as a flat, white patch that is microscopically indistinguishable from ordinary homogeneous leukoplakia.
Phase 2, Spread to multiple sites. Over years, additional white patches appear in different parts of the mouth. The original lesions persist and slowly enlarge.
Phase 3, Surface change. The patches develop rough, warty, papillary (with finger-like surface projections) or verrucous surfaces. The previously flat lesions now look exophytic (raised and projecting from the surface), raised and projecting.
Phase 4, Verrucous carcinoma. Some lesions go through a stage that is microscopically indistinguishable from verrucous carcinoma, a slow-growing form of squamous cell carcinoma that does not typically metastasise (spread to distant parts of the body).
Phase 5, Squamous cell carcinoma. Many lesions eventually transform into ordinary, frankly invasive squamous cell carcinoma. Neville notes that this often happens within 8 years of initial PVL diagnosis. Multiple separate primary carcinomas can develop in the same patient over many years.
The disease essentially keeps moving forward even when individual lesions are excised, with new lesions appearing at fresh sites.
What might you notice?
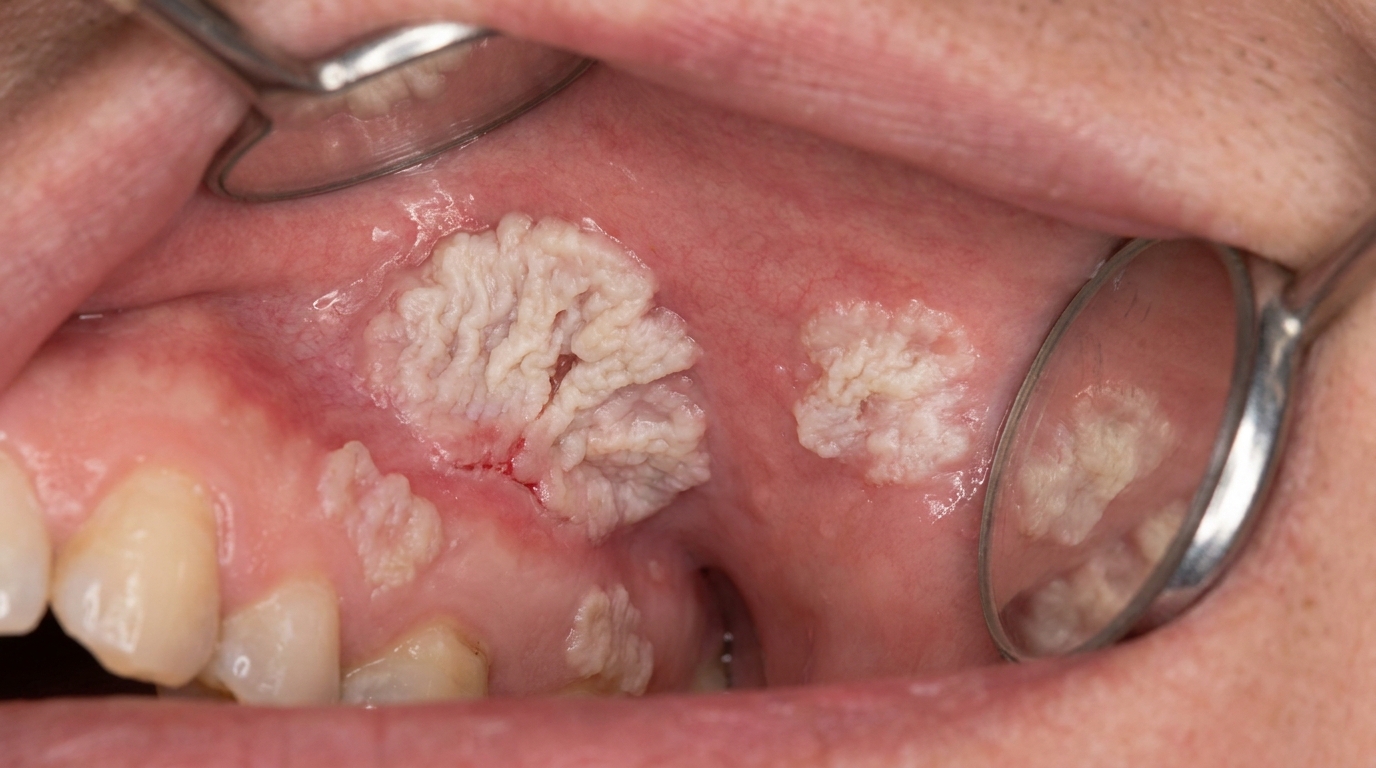
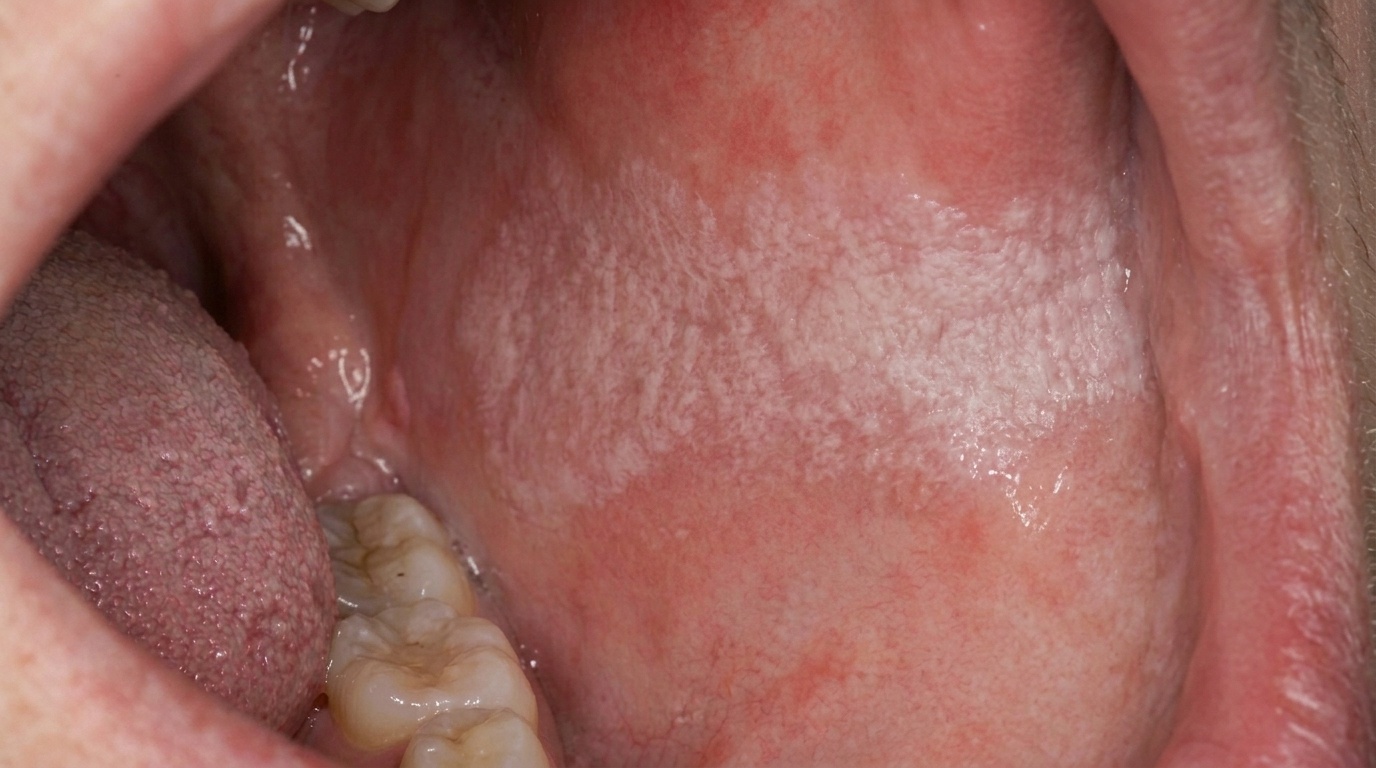
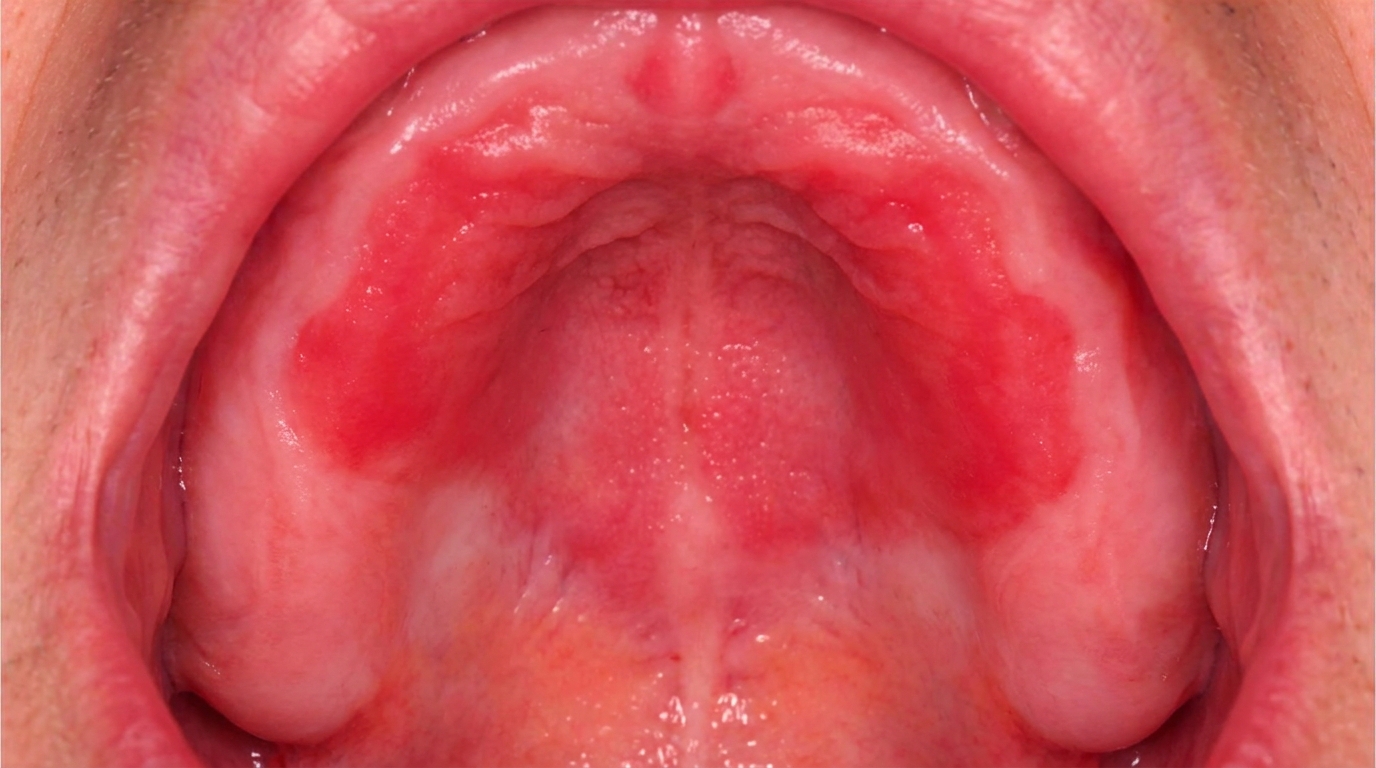
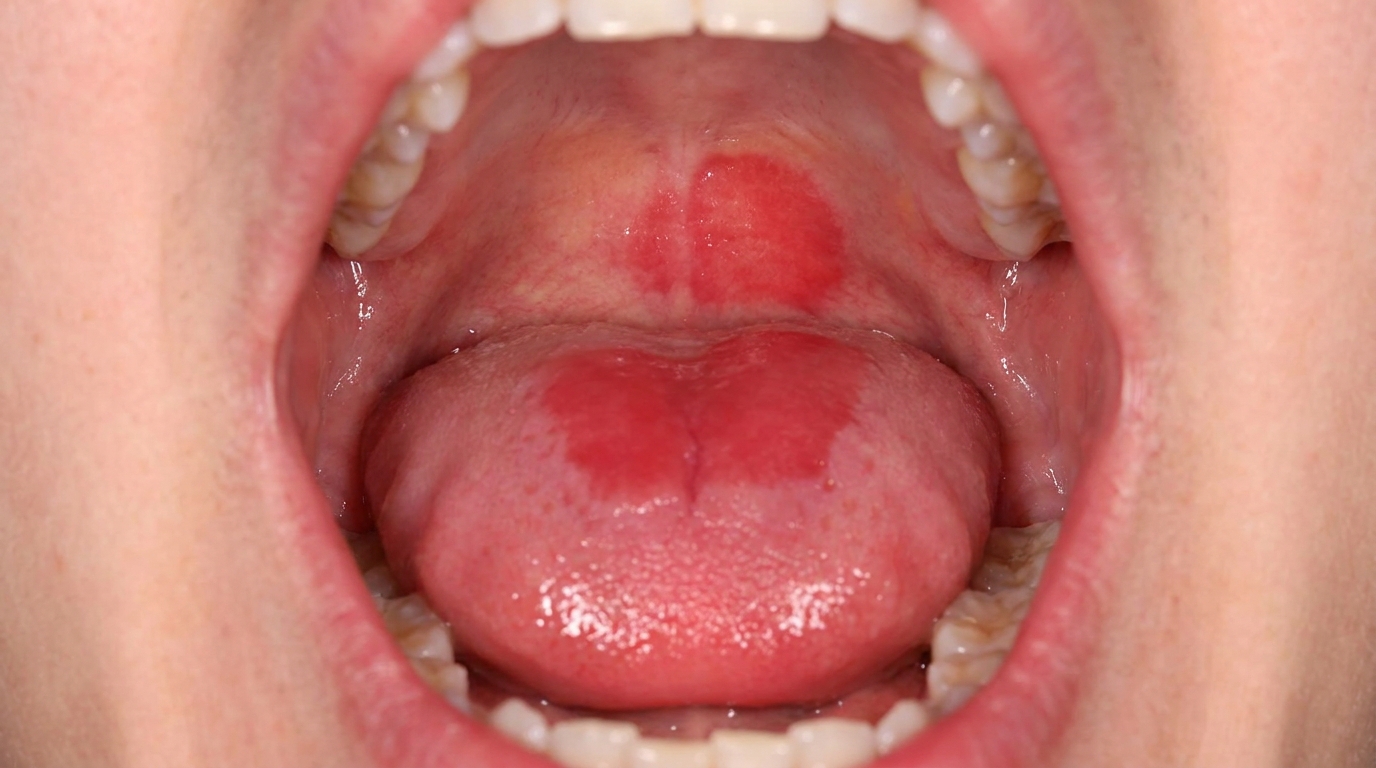
What it looks like
The textbooks describe a fairly recognisable clinical picture:
Multiple white patches in different parts of the mouth, rather than a single isolated lesion.
Surface texture that begins flat and gradually becomes wrinkled, warty or cauliflower-like over the years.
Common sites include the gums (gingiva), the inside of the cheeks, and the tongue. The gum involvement is often a useful clue, as ordinary leukoplakia less commonly affects the gingiva so extensively.
Slow but persistent growth, the patches enlarge gradually over months and years rather than rapidly over weeks.
Mixed appearances are common, different patches in the same mouth may be at different stages, with some flat and white, others thick and verrucous.
What it feels like
PVL is generally painless in the early phases. Symptoms tend to develop later and may include:
Mild discomfort when eating spicy or acidic foods.
Roughness felt with the tongue, particularly over the verrucous areas.
Bleeding or ulceration in areas where transformation to cancer has occurred, these are warning signs that warrant urgent reassessment.
Loose teeth if PVL has caused or coexists with cancer involving the gums and underlying bone.
What an X-ray might show
PVL itself is a soft-tissue condition, so X-rays do not show the white patches directly. Imaging may be relevant if a transformed area extends into the underlying bone, where bone destruction can be seen.
What happens at the dentist?
A patient with PVL typically presents in one of two ways: a single white patch that has not gone away, or a more obvious set of multiple persistent patches. A dentist at ArtSmiles, typically as part of a dental check-up and clean, will commonly:
Examine every area of the mouth carefully under good light, photographing and mapping any white or rough areas.
Review the timeline, when the patches were first noticed, how they have changed, what risk factors are present.
Take multiple biopsies from representative areas. PVL is rarely diagnosed from a single biopsy because different parts of the same lesion may be at different stages.
Refer to an oral medicine specialist or oral and maxillofacial surgeon for confirmation of the diagnosis and ongoing care.
Plan long-term surveillance with frequent reviews, typically every 3-6 months, often supported by photographs taken at each visit.
Coordinate with general health practitioners for any associated conditions and risk factor management.
The textbooks emphasise that PVL diagnosis is often only definitively made retrospectively, when the pattern of multiple progressive lesions has become clear over years. This means careful documentation from the first encounter is particularly important.
Is this serious?
🔴 PVL is the most aggressive of the leukoplakia variants. Although the lesions themselves do not cause acute symptoms, the long-term outlook is sobering: the great majority of cases eventually transform into squamous cell carcinoma, often at multiple sites and sometimes despite repeated surgical removal. With early identification and structured surveillance, individual cancers are usually caught at a stage where they can be effectively treated. Without surveillance, the disease can present with advanced cancer. The key practical message is that PVL is a chronic condition requiring lifelong dental and specialist follow-up.
If you have multiple persistent white patches in the mouth, particularly if they have been slowly growing over years and especially if they involve the gums, it is worth booking an assessment so that the right biopsies and surveillance plan can be put in place.
Could it be something else?
Several conditions can produce multiple white or warty patches in the mouth. The textbooks list these as the main differentials:
Ordinary oral leukoplakia, usually a single patch with less aggressive course. PVL is distinguished by the multifocal, progressive pattern over years.
Verrucous carcinoma, a slow-growing form of squamous cell carcinoma that can develop within PVL. Distinguished on biopsy.
Squamous cell carcinoma, invasive cancer can arise within PVL or mimic it. Biopsy is essential.
Multiple oral squamous papillomas, small wart-like growths from HPV; usually well-demarcated and not associated with surrounding white change.
Reticular oral lichen planus, produces lacy white patterns, often symmetrical, and follows a different course.
Chronic hyperplastic candidiasis, can produce a thick adherent plaque, particularly at the corner of the mouth, distinguishable on biopsy.
How is it treated?
PVL is one of the more difficult oral conditions to manage because the lesions resist treatment and continually appear in new sites. The textbooks describe a multifaceted approach:
At-home measures and habits:
Maintain meticulous oral hygiene, including thorough brushing, flossing, and gentle tongue care.
Avoid all forms of tobacco, including smoking and smokeless tobacco, even if PVL is not strongly tobacco-related.
Limit alcohol to reduce overall mucosal stress.
Eat a balanced diet with plenty of fruit and vegetables to support general mucosal health.
Photograph any new or changing patches if you have been advised to monitor.
Attend every scheduled review. With PVL, the timing of review visits is crucial, missed appointments are the single biggest avoidable risk.
Professional steps your dentist may consider:
Multiple biopsies from representative areas, both at diagnosis and at intervals over time.
Surgical excision of dysplastic or thickened lesions. This is the mainstay of treatment for individual lesions, although the textbooks note that lesions are "difficult or impossible to eradicate surgically and recur or spread to new sites".
Laser ablation as an alternative to surgical excision, particularly for more accessible lesions.
Photodynamic therapy in selected centres.
Long-term specialist surveillance with examinations every 3-6 months for life, including photographs and selected re-biopsy.
Prompt management of any cancer that develops, with conventional oncological treatment.
A patient-centred approach is particularly important here. PVL is a long-term diagnosis that asks a great deal of patience and trust. Honest, ongoing discussion of what to expect, when to come back, and what change should prompt urgent review is itself part of effective care, values that sit at the heart of our clinical philosophy.
What's the long-term outlook?
The outlook for PVL is the most challenging of the leukoplakia variants. Most patients eventually develop squamous cell carcinoma at one or more sites, often within 8 years of initial diagnosis. With careful long-term surveillance, however, the cancers that arise are usually caught early, when treatment outcomes are far better. With strong patient engagement, regular review, and prompt management of any new or changing lesion, many patients live with PVL for decades while maintaining good function and quality of life. The single most important factor, more than any specific treatment, is consistent, ongoing dental and specialist follow-up.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
The cover image above is an AI-generated illustration based on the most common visible features of this condition described in clinical pathology references. It is not a photograph of a real case and should not be used to diagnose or rule out the condition in your own situation. If you are concerned about something you have noticed, please book an assessment with a registered dental practitioner.
References
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 16, Oral Premalignancy: Proliferative Verrucous Leukoplakia, with elderly female predominance, non-smokers and high transformation rate, p. 265.
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2023). Oral and maxillofacial pathology (5th ed.). Elsevier. Chapter 10, Epithelial Pathology: Proliferative Verrucous Leukoplakia (PVL), with female predilection (1:4 male-to-female ratio) and squamous cell carcinoma transformation often within 8 years, pp. 384 to 385.
Regezi, J. A., Sciubba, J. J., & Jordan, R. C. K. (2017). Oral pathology: Clinical pathologic correlations (7th ed.). Elsevier. Chapter 6, Premalignant and Malignant Soft Tissue Lesions: PVL as a verrucous carcinoma precursor.