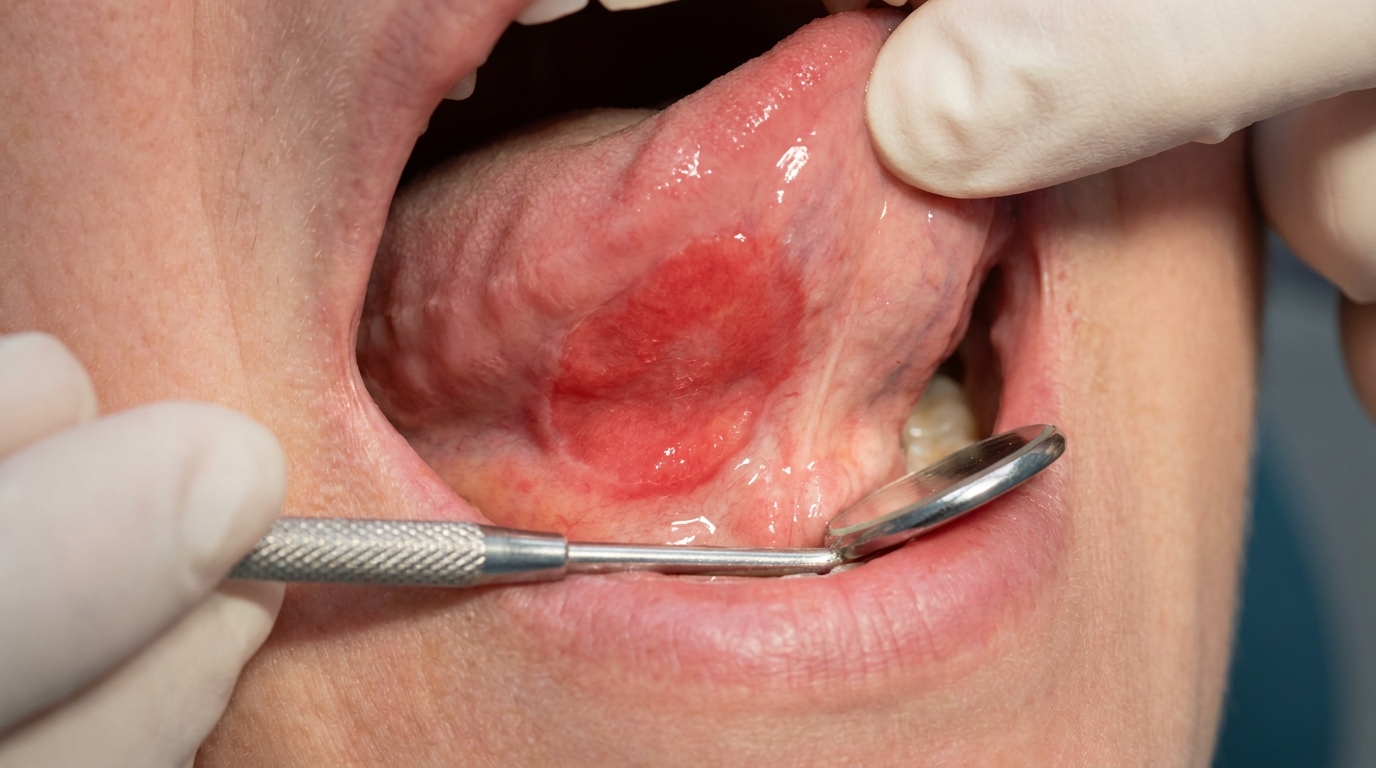
Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker, Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | Cheek chewing, habitual cheek biting, chronic cheek nibbling; related forms include morsicatio labiorum (lip) and morsicatio linguarum (tongue) |
How urgent? | 🟢 Not urgent, benign and reversible once the biting habit stops |
Common or rare? | Common; often under-recognised because patients are not aware of the habit |
Who it affects | Adults of any age, more often in people who are anxious, focused or stressed; sometimes linked with malocclusion or bruxism (habitual teeth grinding or clenching) |
Who treats it | General dentist for diagnosis and management; psychologist or GP for stress and anxiety; orthodontist if malocclusion is a major driver |
Based on | Neville, Cawson and Regezi |
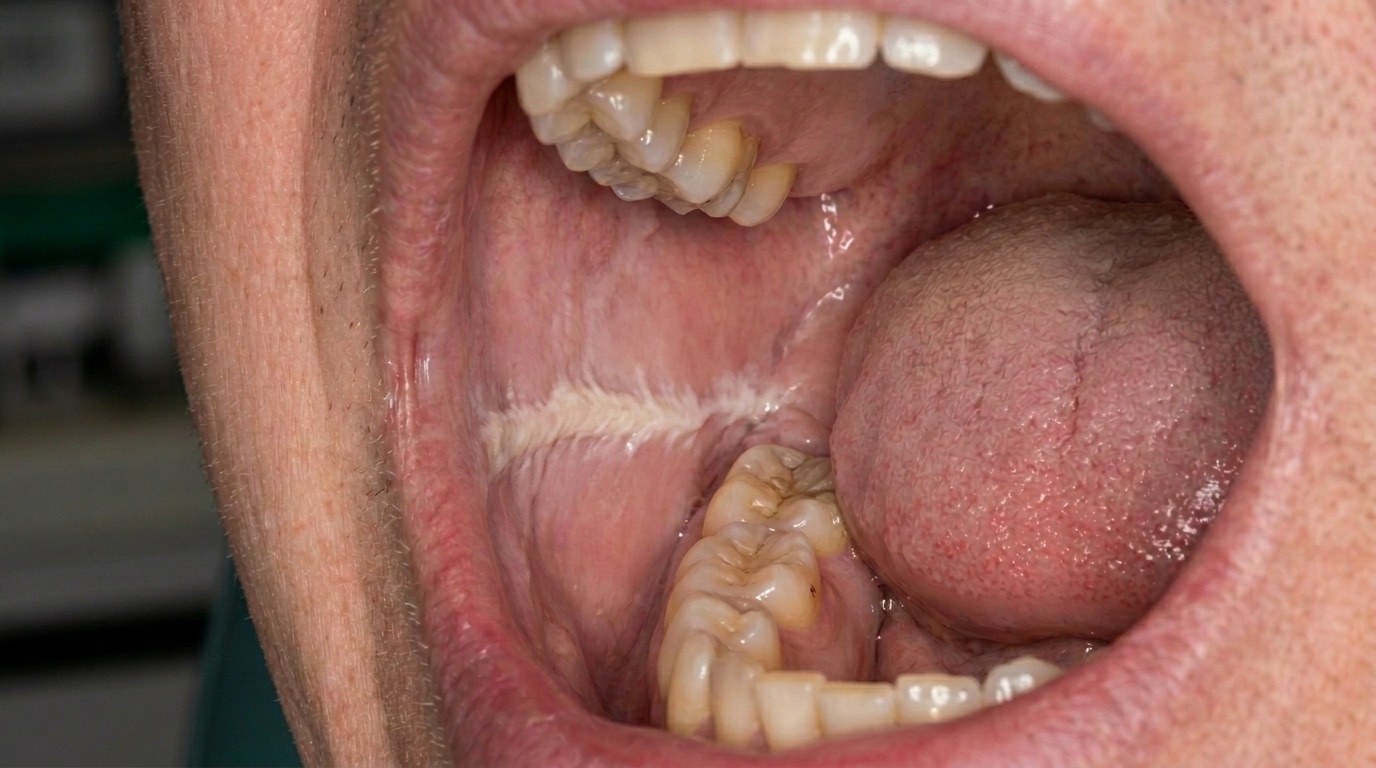
If you frequently catch yourself biting or nibbling the inside of your cheek, especially when stressed, anxious, concentrating or watching television, you may have noticed a slightly fluffy white area on the lining of the cheek. The medical term for this benign change is morsicatio buccarum, from the Latin for cheek-biting.
This article from the team at ArtSmiles, reviewed by Dr Cristian Dunker, explains what morsicatio buccarum is and how to address the underlying habit.
What is it?
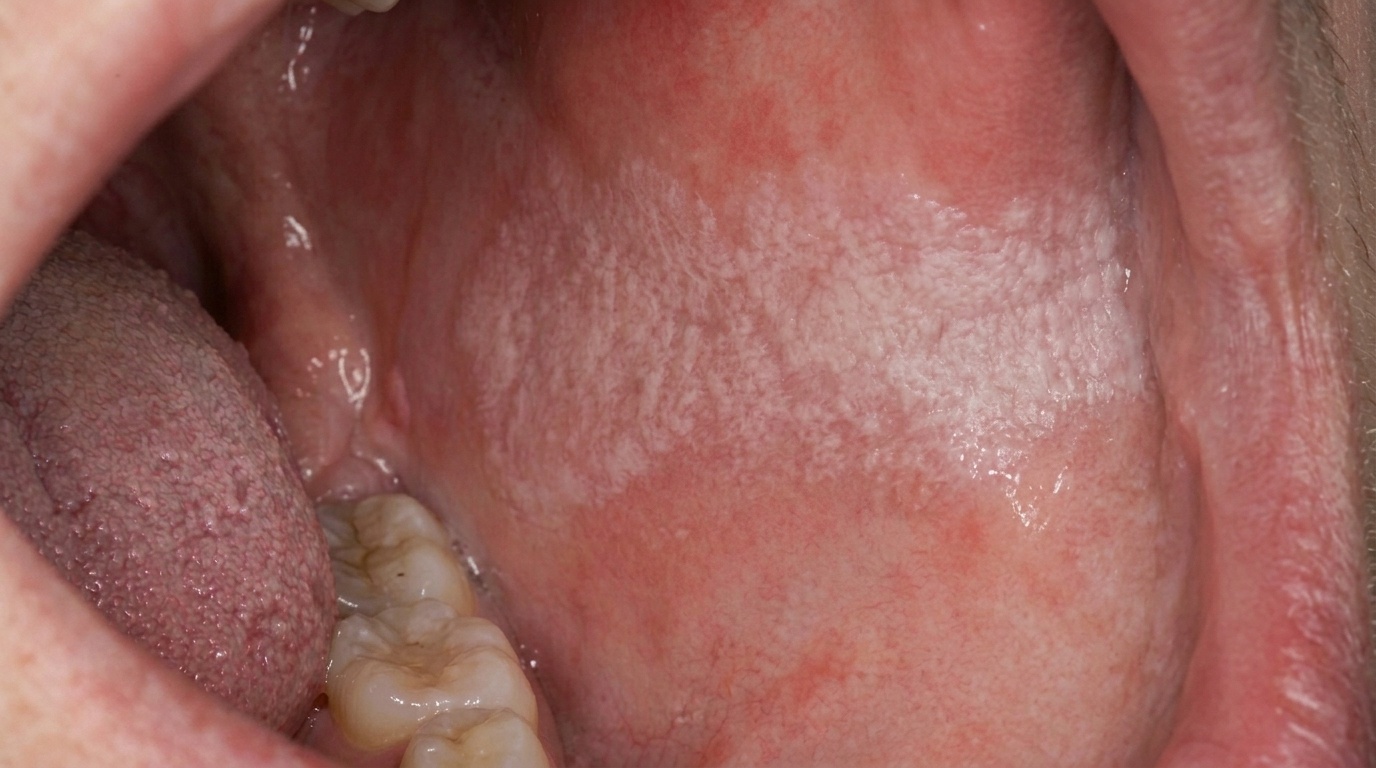
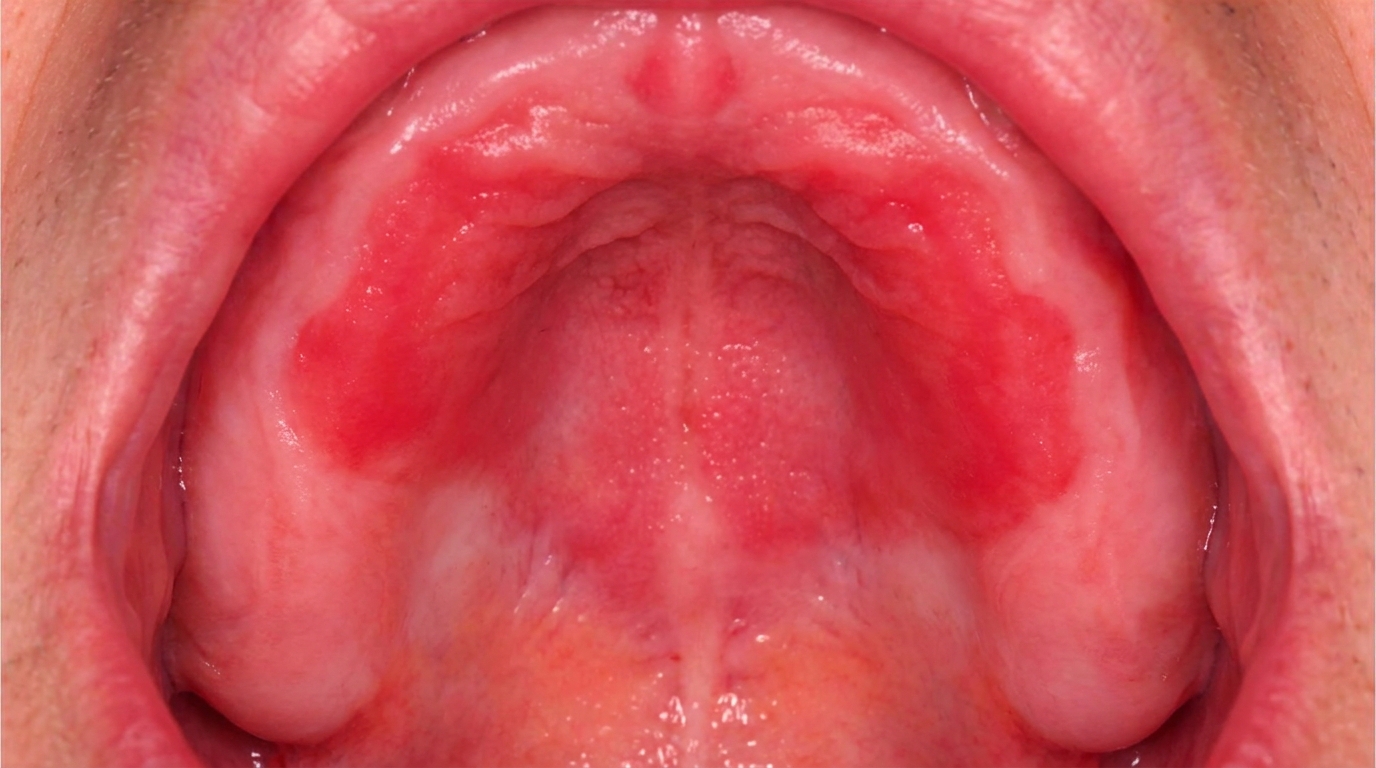
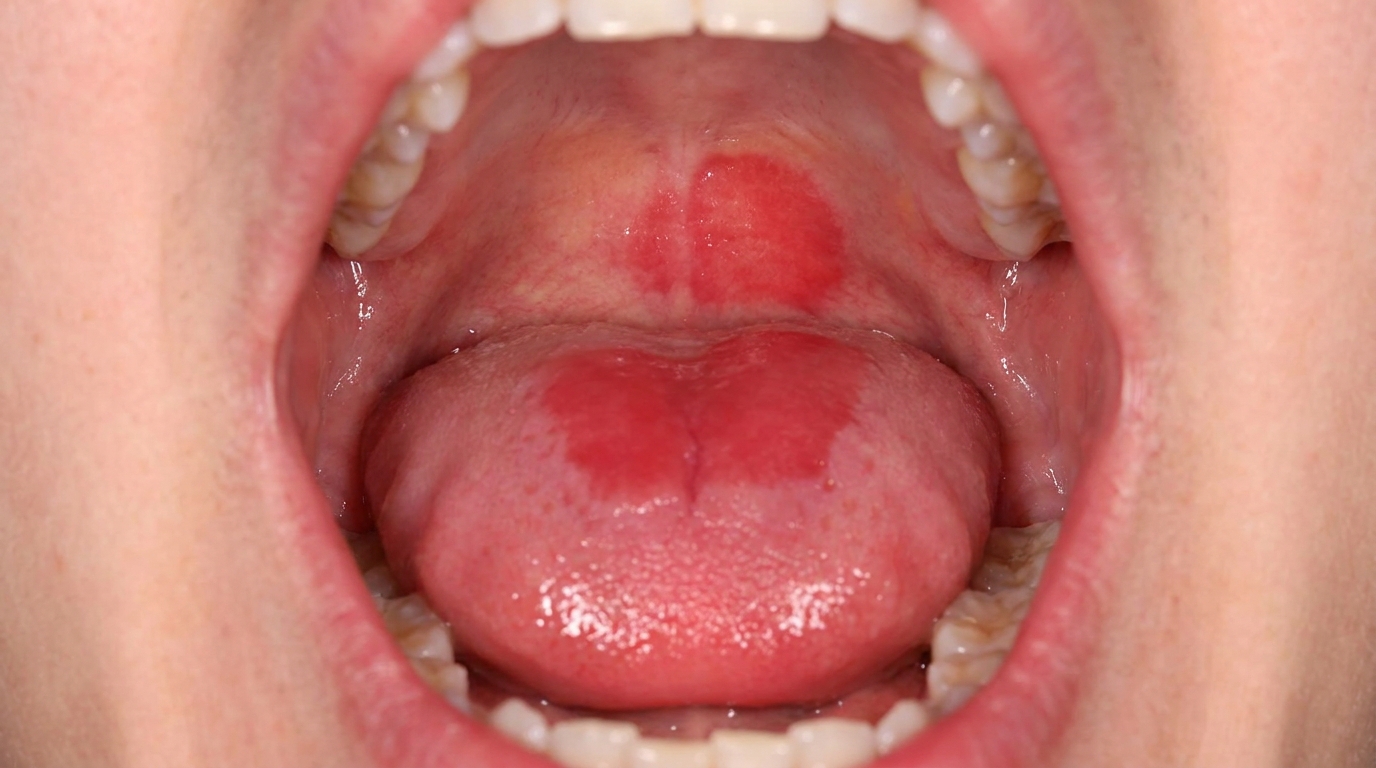
Morsicatio buccarum is a chronic frictional keratosis of the cheek lining caused by repeated chewing or biting. The lining responds to constant low-grade injury by becoming thicker, paler and frayed. Common features include:
A fluffy, shaggy or shredded white surface, often described as having a "pulled apart" appearance.
Located along the occlusal line, where the upper and lower teeth meet.
Bilateral in many patients, sometimes more pronounced on one side.
Soft to touch, with small loose tags of lining that can be felt with the tongue or fingernail.
No pain, although some areas can be slightly tender.
Two related conditions exist on neighbouring sites:
Morsicatio labiorum, chronic biting of the lip lining.
Morsicatio linguarum, chronic biting of the side of the tongue.
Who tends to get it?
Morsicatio buccarum is mostly seen in:
Adults with a long-standing cheek-biting habit, often unconscious.
People prone to anxiety or stress.
Those with high focus or concentration jobs, where biting becomes an unconscious habit.
Children and adolescents in some cases, though it is more often diagnosed in adults.
Patients with malocclusion (crooked teeth) where the cheek can catch between the teeth.
What causes it?
The trigger is mechanical injury from chronic biting. The cheek lining responds by:
Producing more keratin (the protective protein layer).
Forming irregular surface tears as small bits of lining are nibbled.
Maintaining a constantly thickened, scarred-looking surface.
Common drivers of the habit include:
Stress and anxiety.
Boredom or focus during reading, watching, computer use.
Malocclusion that allows the cheek to slip between teeth.
Sleep-related cheek biting in some patients with bruxism.
Tic-like behaviour in some neuropsychiatric conditions.
How does it develop?
The course is gradual. Once the biting habit is established, the lining develops the typical shredded white appearance over weeks to months. The change persists as long as the habit continues. Once the habit stops, for example after wearing an occlusal splint, the lining returns to normal within a few weeks.
What might you notice?
Common observations include:
A fluffy white area on the inside of one or both cheeks.
A feeling of small loose pieces of lining that the tongue can pull at.
No pain, but sometimes a feeling of dryness or irritation.
A worsening pattern during stressful periods.
An awareness of the habit when looking for it.
What an X-ray might show
Morsicatio buccarum is confined to the surface lining of the cheek and does not show on X-rays.
What happens at the dentist?
When morsicatio buccarum is identified at ArtSmiles, the visit usually involves:
A look at the affected area to confirm the typical appearance.
A history conversation about the habit, when it occurs, and any associated stress or anxiety.
A check for malocclusion or sharp tooth edges contributing to cheek catching.
A discussion of strategies to break the habit, see below.
No biopsy in straightforward cases, the appearance is usually distinctive enough.
Reassurance that the lining is benign and reversible.
Is this serious?
Morsicatio buccarum is not serious in itself. It does not turn into cancer. Reasons it can deserve attention include:
Confirmation of diagnosis, since other white patches need to be excluded.
Identifying underlying anxiety or stress that may benefit from broader support.
Addressing malocclusion that drives the habit.
Comfort, patients sometimes find the rough surface bothersome.
Could it be something else?
Other white changes that can be confused with morsicatio buccarum include:
Linea alba, a smooth horizontal white line, not shredded.
Frictional keratosis from a sharp tooth, localised, not bilateral.
Leukoedema, a soft grey-white film, not shredded.
Lichen planus, lacy white streaks, often with other features.
White sponge naevus, hereditary, present from young age.
Leukoplakia, persistent white patch with potential malignant change.
The "pulled apart" or shaggy appearance combined with a confirmed biting habit is usually distinctive.
How is it treated?
Treatment is directed at the habit, not at the lining:
Awareness. Many patients are unaware of how often they bite. Becoming conscious of the habit is the first step.
Occlusal splint (night guard). A simple acrylic splint covering the teeth physically blocks cheek-biting and helps the lining heal.
Stress management. Breathing exercises, mindfulness, exercise and structured stress reduction can reduce the habit.
Cognitive behavioural therapy for patients in whom the habit is driven by anxiety.
Treatment of malocclusion by orthodontics in selected cases.
Smoothing of any sharp tooth edge that catches the cheek.
Avoiding triggers identified by the patient.
What's the long-term outlook?
The outlook is excellent. Once the habit stops, the cheek lining returns to a normal appearance within a few weeks. Some patients have a recurring pattern during stressful periods and a quiet period when life is calmer. Long-term, the condition itself does not cause harm.
If you have noticed a fluffy white area on the inside of your cheek, or are aware that you bite your cheek a lot, please book a visit. We can confirm the diagnosis and discuss simple strategies to break the cycle.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
The cover image above is an AI-generated illustration based on the most common visible features of this condition described in clinical pathology references. It is not a photograph of a real case and should not be used to diagnose or rule out the condition in your own situation. If you are concerned about something you have noticed, please book an assessment with a registered dental practitioner.
References
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2016). Oral and maxillofacial pathology (4th ed., Ch. 10: Epithelial Pathology, Morsicatio Buccarum). Elsevier.
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed., Ch. 16: Premalignant Conditions, cross-reference). Elsevier.
Regezi, J. A., Sciubba, J. J., & Jordan, R. C. K. (2017). Oral pathology: clinical pathologic correlations (7th ed., Ch. 3: Red and White Lesions). Elsevier.