Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker , Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | Aphthous ulcers, recurrent aphthae, canker sores, RAS, RAU, aphthous stomatitis |
How urgent? | 🟢 Usually harmless, but persistent or unusually severe ulcers deserve a check-up to rule out other causes |
Common or rare? | Very common, among the most common conditions of the oral mouth lining (mucosa), affecting roughly 5,60% of people at some point |
Who it affects | Children and young adults most often, with first episodes typically before age 30; women slightly more than men |
Who treats it | General dentist for most cases; specialist referral if ulcers are severe, persistent, or part of a wider condition |
Based on | Regezi, Neville, Cawson, Laskaris |
What is it?
Recurrent aphthous stomatitis (RAS) is the medical name for the small, painful mouth ulcers many people simply call canker sores or aphthous ulcers. They appear on the soft, movable lining of the mouth, the inside of the lips and cheeks, the floor of the mouth, the underside or sides of the tongue, and the soft palate at the back. They tend to come back from time to time, heal on their own, then return weeks or months later.
Three clinical patterns are recognised: minor, major, and herpetiform. They sit on the same disease spectrum and differ mainly in size, depth, and number rather than in cause.
Who tends to get it?
RAS is one of the most common oral mucosal conditions. Reported prevalence varies widely, from around 5% to as high as 66% of people, depending on the population studied, with most estimates clustering around 20%. It is more often reported in non-smokers and in white-collar or professional groups.
Most people experience their first episode before the age of 30, and the frequency of attacks usually peaks in adolescence and early adulthood before gradually easing later in life. Women are affected slightly more often than men. Recurrent aphthae are uncommon in older adults, particularly those who wear full dentures, and a new onset later in life should always prompt a check for other underlying causes.
Family history matters. Around 40% of affected people have a first-degree relative who is also affected, and a child with two affected parents has roughly a 90% chance of developing aphthae themselves.
What causes it?
The exact cause is still unknown, and the honest summary from the pathology literature is that the trigger appears to be "different things in different people". The mucosal damage itself is driven by an immune reaction in which T lymphocytes (a type of white blood cell) and the inflammatory signalling molecule TNF-alpha play a major role.
A range of factors have been linked to triggering or worsening attacks in individual subgroups of patients:
Local trauma, minor knocks from a toothbrush bristle, a sharp food edge, accidental cheek bite, or rough cusp
Stress, both mental and physical
Hormonal changes, some women notice a flare in the days before menstruation
Stopping smoking, aphthae are almost exclusively a problem of non-smokers, and may even start when someone quits
Nutritional deficiencies, iron, folate, zinc, and B-group vitamins (B1, B2, B6, B12)
Foods and food chemicals, chocolate, nuts, gluten, cheese, coffee, cow's milk, strawberries, tomatoes, dyes, flavourings, and preservatives have all been reported as triggers
Toothpaste ingredients, sodium lauryl sulfate (a common foaming agent) is mentioned as a possible trigger
Certain medications, non-steroidal anti-inflammatories (NSAIDs), some beta-blockers, angiotensin receptor blockers, bisphosphonates, and nicorandil among others
Underlying systemic conditions, coeliac disease, Crohn's disease, ulcerative colitis, immune deficiencies, and some hereditary inflammatory syndromes
Genetic predisposition
HIV-positive patients can experience more severe and prolonged aphthous-like ulcers. Outside of these specific associations, most people with recurrent aphthae are otherwise completely well.
How does it develop?
Think of the mouth lining as a protective wallpaper. The non-keratinised parts (the soft, movable lining), inside the cheeks, lips, and under the tongue, have thinner, more delicate "wallpaper" than the tougher mucosa over the gums and hard palate. In people prone to RAS, the immune system seems to misread something on or near this thinner lining as a threat.
T cells gather in the tissue and release inflammatory signals (including TNF-alpha) that direct cytotoxic T cells (immune cells that destroy other cells) to attack the surface lining cells. The lining breaks down, leaving a small crater covered by a yellow-white fibrin layer (a protein the body uses to form a temporary seal over a wound) with a red rim of inflammation around it. Over a week or two, healing reverses the process and the lining grows back.
This explains two consistent observations: the ulcers almost always appear on the soft, movable mucosa rather than on gum or hard palate, and small triggers like a toothbrush poke or a salty crisp can tip the area into a full ulcer in someone already predisposed.
What might you notice?
What it looks like
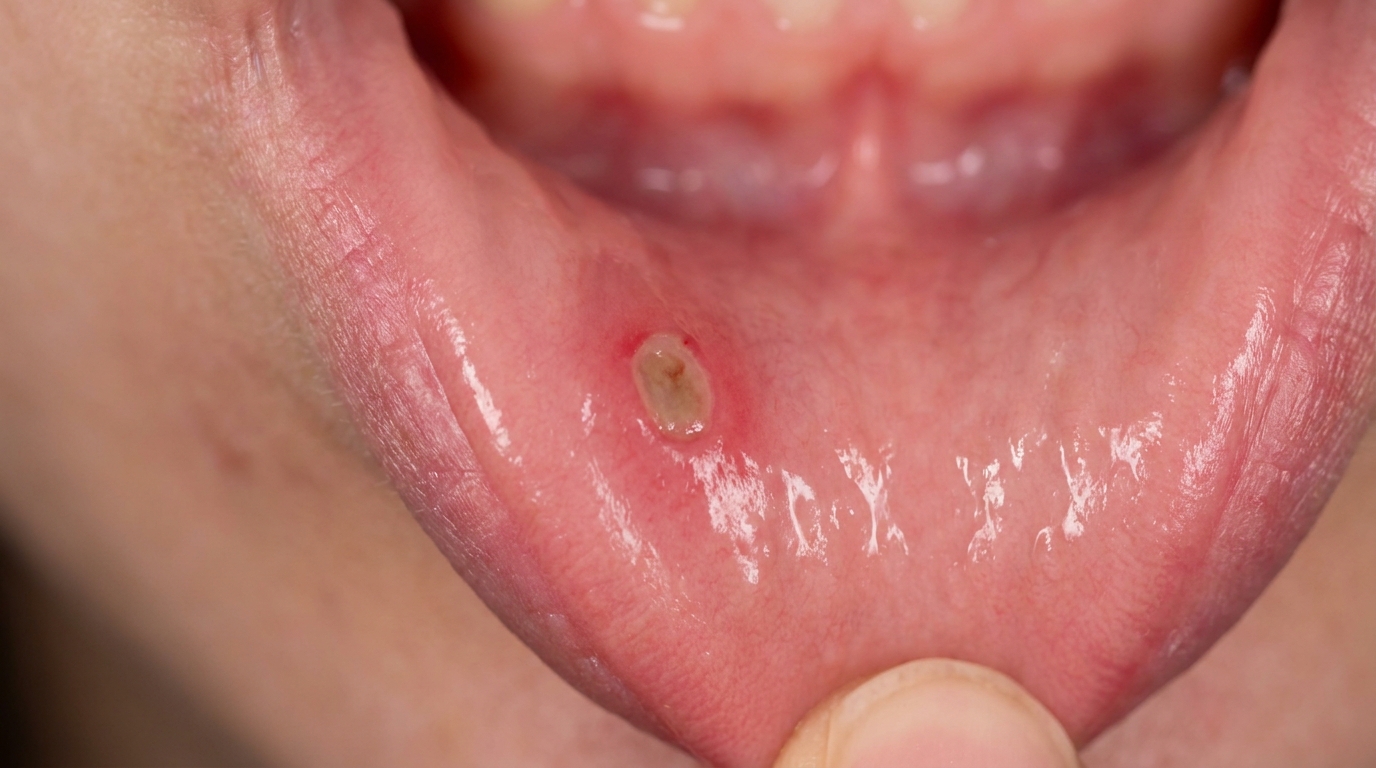
A classic minor aphthous ulcer is a small, round or oval crater, usually 3,10 mm across, with a creamy yellow or yellow-white floor and a thin bright-red halo around the edge. Most episodes show one to five ulcers at a time, on the inside of the cheek or lip, the underside of the tongue, the floor of the mouth, the mucobuccal fold (the crease where the inner lip meets the gum), or the soft palate. They heal in 7,14 days without leaving a scar.
Major aphthous ulcers (sometimes called Sutton disease or periadenitis mucosa necrotica recurrens) are larger and deeper, usually 1,3 cm across, often with a ragged, crater-like appearance. They take longer to heal, from two to six weeks, and may leave a small scar. They tend to favour the lip lining, soft palate, and the area around the tonsils.
Herpetiform aphthae appear as crops of many tiny pinhead ulcers, each only 1,3 mm across. There can be 10 to 100 at a time, sometimes coalescing into larger irregular patches. Despite the name, they are not caused by the herpes virus, the resemblance is purely visual.
What it feels like
Most people first notice a tingling, burning, or stinging spot in the mouth a day or two before the ulcer appears. Once the ulcer forms, it is usually surprisingly painful for its size, especially when the tongue, salty or acidic foods, hot drinks, or toothbrush bristles brush against it. Speaking, eating, and brushing can all become uncomfortable. Major ulcers, in particular, can interfere with eating and may affect sleep and general wellbeing during a flare.
Fever and feeling generally unwell are not typical of straightforward RAS, if these are present, another diagnosis should be considered.
What happens at the dentist?
There is no single laboratory test that confirms RAS. Diagnosis is made from the history (recurrent ulcers since childhood or adolescence, healing between attacks) and clinical appearance (typical sites, typical look). At ArtSmiles, a dentist will usually:
Ask about the pattern and frequency of attacks, family history, diet, medications, smoking status, gut symptoms, skin or eye involvement, and any genital ulcers
Examine the mouth carefully to confirm the appearance and rule out look-alike conditions
For ulcers that have not healed within 2,3 weeks, or that look unusual, recommend a biopsy (a small tissue sample sent to the lab for testing) to exclude other causes
Order blood tests where appropriate, full blood count, ferritin (a marker of body iron stores), folate, vitamin B12, particularly if symptoms started later in life, are severe, or are getting worse
Refer to a specialist (oral medicine, dermatology, or gastroenterology) if Behçet disease, inflammatory bowel disease, coeliac disease, or another underlying condition is suspected
Biopsy of an aphthous ulcer is rarely needed for diagnosis because the microscopic features are non-specific. Its main role is to exclude other diseases, particularly when a single ulcer is solitary, persistent, or has unusual features.
Is this serious?
🟢 In the great majority of cases, recurrent aphthous stomatitis is a benign, self-limiting condition. The ulcers are uncomfortable rather than dangerous, they heal on their own, and they do not turn into cancer.
🟡 A check-up is worthwhile when:
A first episode occurs after the age of 30
Ulcers become more frequent, larger, or more painful than before
Healing takes longer than 2,3 weeks
There are other symptoms, eye irritation, genital ulcers, skin rashes, joint pain, persistent diarrhoea, weight loss, or fatigue
Ulcers are interfering significantly with eating, drinking, or sleep
If you've noticed any of these signs for more than two weeks, it's worth booking an assessment.
Major aphthae can be genuinely disabling during a flare and rarely, in long-standing severe cases, the scarring may restrict mouth opening. Persistent severe RAS in adulthood can also signal an underlying condition, such as a haematinic deficiency (low iron, vitamin B12 or folate, the nutrients needed to make healthy blood), coeliac or Crohn's disease, an immune disorder, or Behçet's disease, that benefits from being identified and treated.
Could it be something else?
A number of conditions can produce mouth ulcers that look similar to RAS. The dentist's job is to spot the features that point one way or the other.
Recurrent (secondary) herpes simplex infection, also produces recurrent oral ulcers, but typically appears on the attached gum or hard palate, is preceded by small fluid-filled blisters, and tends to come in clusters of tiny ulcers that merge. RAS, by contrast, occurs on movable mucosa and is not preceded by blisters.
Primary herpetic gingivostomatitis, a first herpes infection in children and young adults, causing widespread painful ulcers with fever, swollen lymph nodes, and inflamed gums; RAS is recurrent and not associated with systemic illness.
Hand, foot and mouth disease, viral illness with mouth ulcers plus a rash on the palms, soles, and sometimes buttocks; usually self-limits within a week and patients are systemically unwell.
Herpangina, viral infection with small ulcers concentrated at the back of the mouth and soft palate, accompanied by sore throat and fever.
Traumatic ulcer, caused by a sharp tooth, denture, cheek bite, or hot food; usually a single ulcer that heals within days once the cause is removed.
Behçet's disease, a multisystem inflammatory disease causing recurrent oral aphthae plus genital ulcers, eye inflammation, skin lesions, and sometimes joint, vascular, gastrointestinal, or neurological involvement; the oral ulcers themselves can be indistinguishable from RAS.
Reactive arthritis (Reiter syndrome), oral ulcers similar to minor aphthae, alongside urethritis, conjunctivitis, and arthritis, often after a gut or sexually transmitted infection.
Crohn's disease, can produce aphthous-like ulcers along with mucosal fissures and "cobblestone" nodules (firm bumps that give the cheek lining a paved-stone look); biopsy of the nodules shows characteristic granulomas (small clusters of immune cells).
Coeliac disease, gluten-sensitive enteropathy (where gluten damages the lining of the small bowel) that can present with aphthous-like ulcers, often via secondary folate or iron deficiency.
Cyclic neutropenia, a periodic dip in white blood cells producing recurrent ulcers in a strict cyclical pattern, usually with fever.
PFAPA syndrome (periodic fever, aphthous stomatitis, pharyngitis, cervical adenitis), a childhood syndrome with recurrent fever, sore throat, swollen neck nodes, and aphthous ulcers.
MAGIC syndrome (mouth and genital ulcers with inflamed cartilage), a rare overlap of Behçet-type ulcers with relapsing polychondritis (a condition in which the immune system attacks cartilage).
HIV-associated aphthous ulcer formation, major aphthae are a recognised feature of advancing HIV disease, often more severe and more frequent than typical RAS.
Pemphigus vulgaris, autoimmune blistering disease in which fragile blisters break down to leave persistent ulcers on any oral surface; biopsy with direct immunofluorescence (a special lab stain that highlights immune-system markers in tissue) is diagnostic.
Mucous membrane pemphigoid, another autoimmune blistering disease, often involving the gum ("desquamative gingivitis", the gum surface peels and reddens, looking sore and raw) as well as ulcers; again confirmed by biopsy.
Erythema multiforme, sudden onset of widespread oral ulcers and crusted lips, often with target-shaped skin lesions, usually triggered by a recent infection or medication.
Chronic ulcerative stomatitis, a rare immune-mediated condition in older women, distinguished by specific findings on direct immunofluorescence.
Syphilitic chancre or mucous patches, usually a single painless ulcer (primary) or greyish patches (secondary); confirmed by serology (blood tests for antibodies) and history.
Nicorandil-induced ulceration, a heart medication that can produce ulcers resembling major aphthae but without the classic recurrent pattern; ulcers heal when the drug is stopped.
Squamous cell carcinoma (oral cancer), a single, persistent, often painless ulcer with raised, indurated (firm and hard) edges, usually in older smokers or drinkers; any solitary ulcer that fails to heal in 2,3 weeks needs urgent assessment and biopsy.
How is it treated?
For most people, RAS cannot be cured outright, but the ulcers can be made less frequent, less severe, and more tolerable. Treatment is tailored to the severity of the disease, and patients are best reassured that recurrent aphthae are common, not serious for general health, and usually settle eventually.
Self-care and prevention
Identify and avoid personal triggers, keeping a brief diary of ulcer episodes alongside foods, stress, and menstrual cycle can help
Switch to a sodium-lauryl-sulfate-free toothpaste if SLS appears to be a trigger
Use a soft toothbrush and brush gently to avoid mechanical trauma
Maintain a balanced diet and address any known nutritional deficiencies
Bland warm salt-water or sodium bicarbonate rinses can keep ulcers clean and comfortable
Professional treatment (always "may include…", never a fixed prescription):
Topical anaesthetics and protective gels, over-the-counter options that numb the ulcer and form a protective film
Topical antiseptic mouthrinses, chlorhexidine (a strong antiseptic mouthwash) at 0.2% used after meals can reduce duration and discomfort
Topical corticosteroids (strong anti-inflammatory gels, ointments or rinses applied directly to the ulcer), the mainstay of treatment for moderate disease; available as pellets, gels, ointments, sprays, or rinse-and-spit solutions, used judiciously they have minimal systemic effect
Tetracycline or doxycycline mouthrinses, particularly useful for herpetiform aphthae
Intralesional corticosteroid injection (a small injection of steroid directly into the ulcer), for individual stubborn major aphthae
Systemic corticosteroids (steroid tablets that work throughout the body), short courses for severe outbreaks under specialist supervision
Other systemic agents, colchicine, dapsone, pentoxifylline, azathioprine, and (in severe complex cases) thalidomide or biological anti-TNF agents (targeted antibody medications that block the inflammatory signal TNF-alpha) may be considered by a specialist
Treating an underlying cause, correcting a confirmed iron, folate, or B12 deficiency can dramatically reduce ulcers; managing coeliac, Crohn's, or other associated disease often helps too
Individual ulcers usually take 7,14 days to heal regardless of treatment; the goal of medication is to reduce pain and shorten that time, and where possible to space attacks further apart.
What's the long-term outlook?
Recurrent aphthous stomatitis is a long-term, benign condition for the great majority of people. Outcomes vary, but the typical pattern is recurrent crops of ulcers throughout adolescence and early adulthood, with attacks gradually becoming less frequent and milder later in life. Many people find that the disease eventually settles on its own.
Minor aphthae heal without scarring. Major aphthae can leave small scars and, very rarely after years of severe disease, contribute to restricted mouth opening. There is no transformation into oral cancer.
Identifying and addressing triggers, whether nutritional, mechanical, or related to an underlying systemic condition, can break the cycle and allow longer ulcer-free intervals. For patients with severe or complex aphthosis, ongoing specialist support helps keep the condition controlled and rules out the less common but more serious causes that share its appearance.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
References
Regezi, J. A., Sciubba, J. J., & Jordan, R. C. K. (2017). Oral pathology: Clinical pathologic correlations (7th ed.). Elsevier. Chapter 2, Ulcerative Conditions: Aphthous Ulcers, pp. 38,43.
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2023). Oral and maxillofacial pathology (5th ed.). Elsevier. Chapter 9, Allergies and Immunologic Diseases: Recurrent Aphthous Stomatitis, pp. 321,326.
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 13, Diseases of the Oral Mucosa: Non-Infective Stomatitis: Recurrent Aphthae, pp. 220,224.
Laskaris, G. Color atlas of oral diseases. Thieme. Chapter 20, Diseases with Possible Immunopathogenesis: Recurrent Aphthous Ulcers, pp. 177,179.