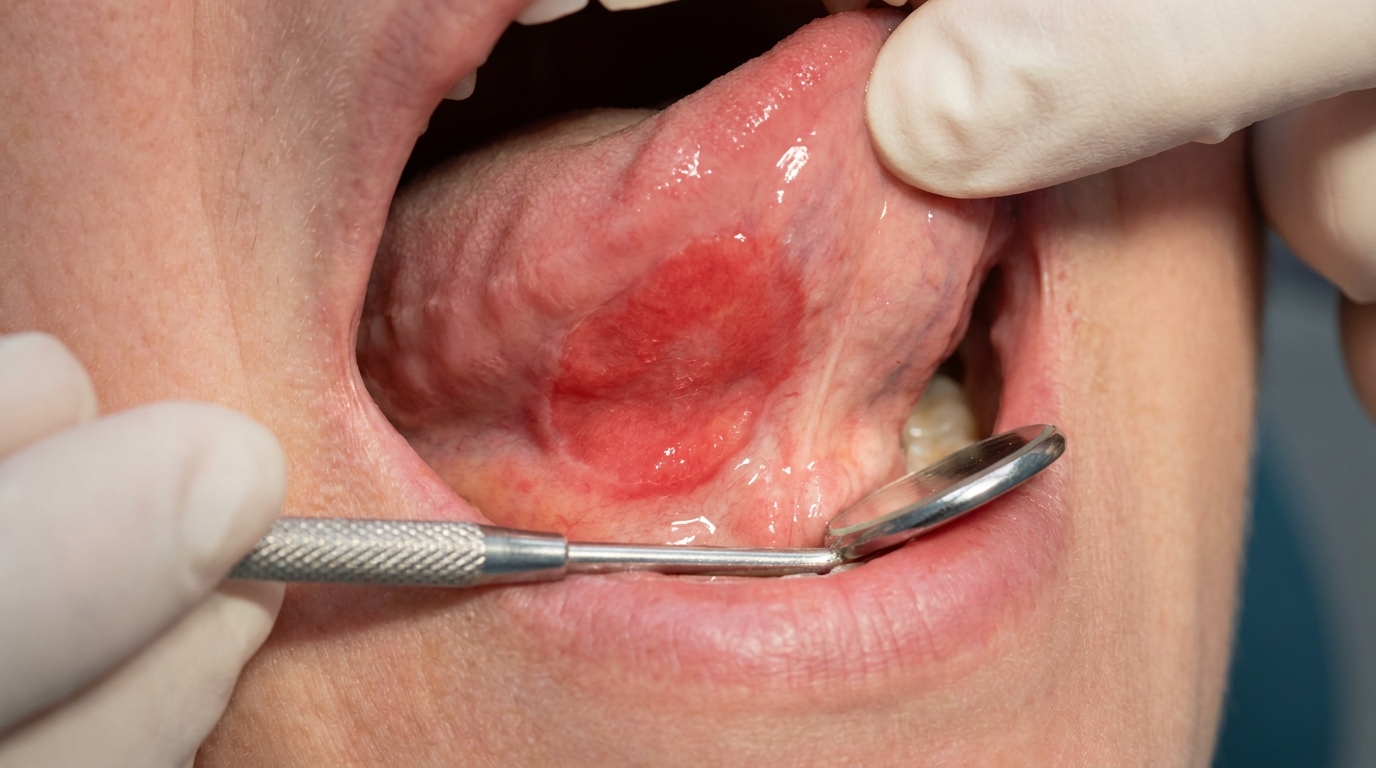
Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker, Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | Smoker's palate, stomatitis nicotina, pipe-smoker's palate |
How urgent? | 🟡 The hard-palate form is generally low-risk and reversible with cessation, but reverse-smoking form is potentially malignant and needs prompt review |
Common or rare? | Uncommon in modern populations, almost always seen in long-term pipe, cigar or heavy cigarette smokers |
Who it affects | Adults, most often men, with long-standing smoking habits; striking in reverse smokers who hold the lit end inside the mouth |
Who treats it | General dentist for diagnosis, cessation support and surveillance; oral medicine specialist if the change persists after cessation or in reverse smokers |
Based on | Neville, Cawson and Regezi |
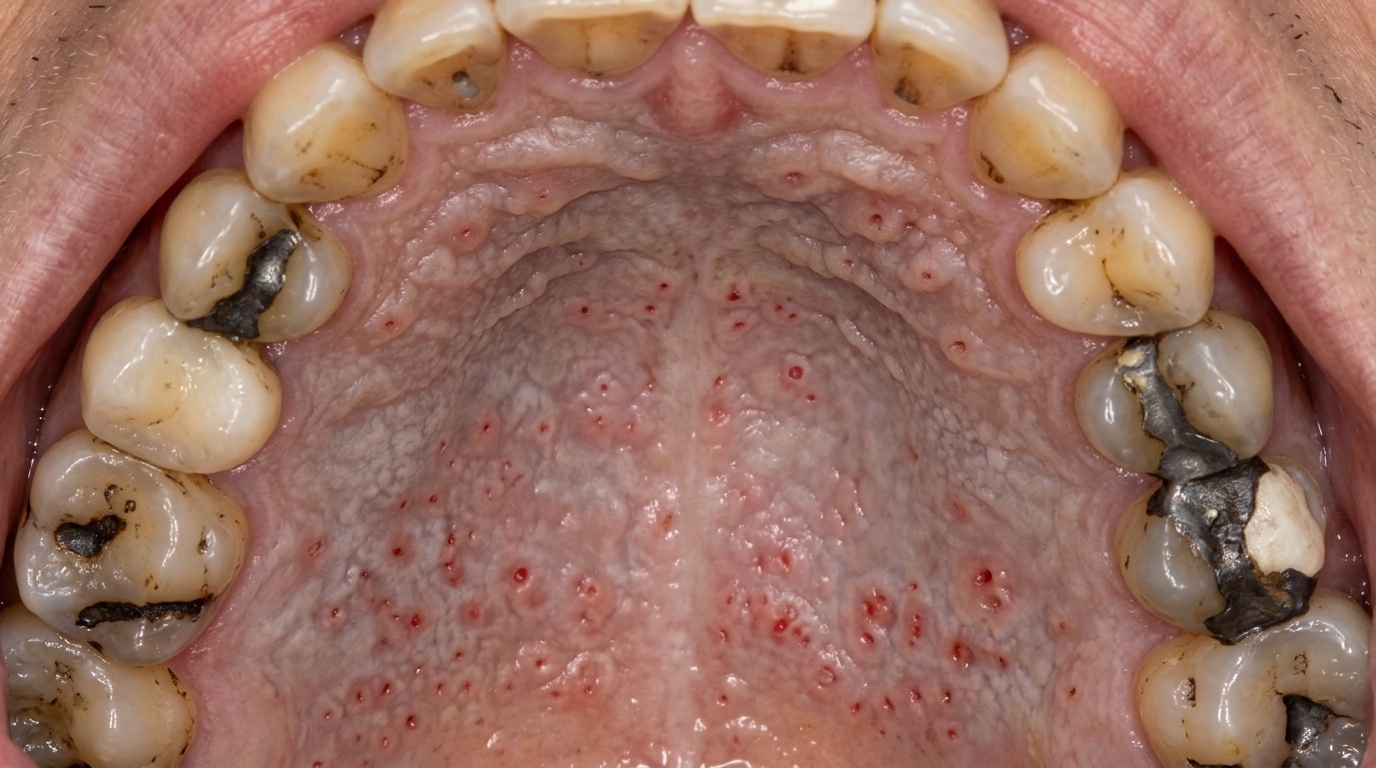
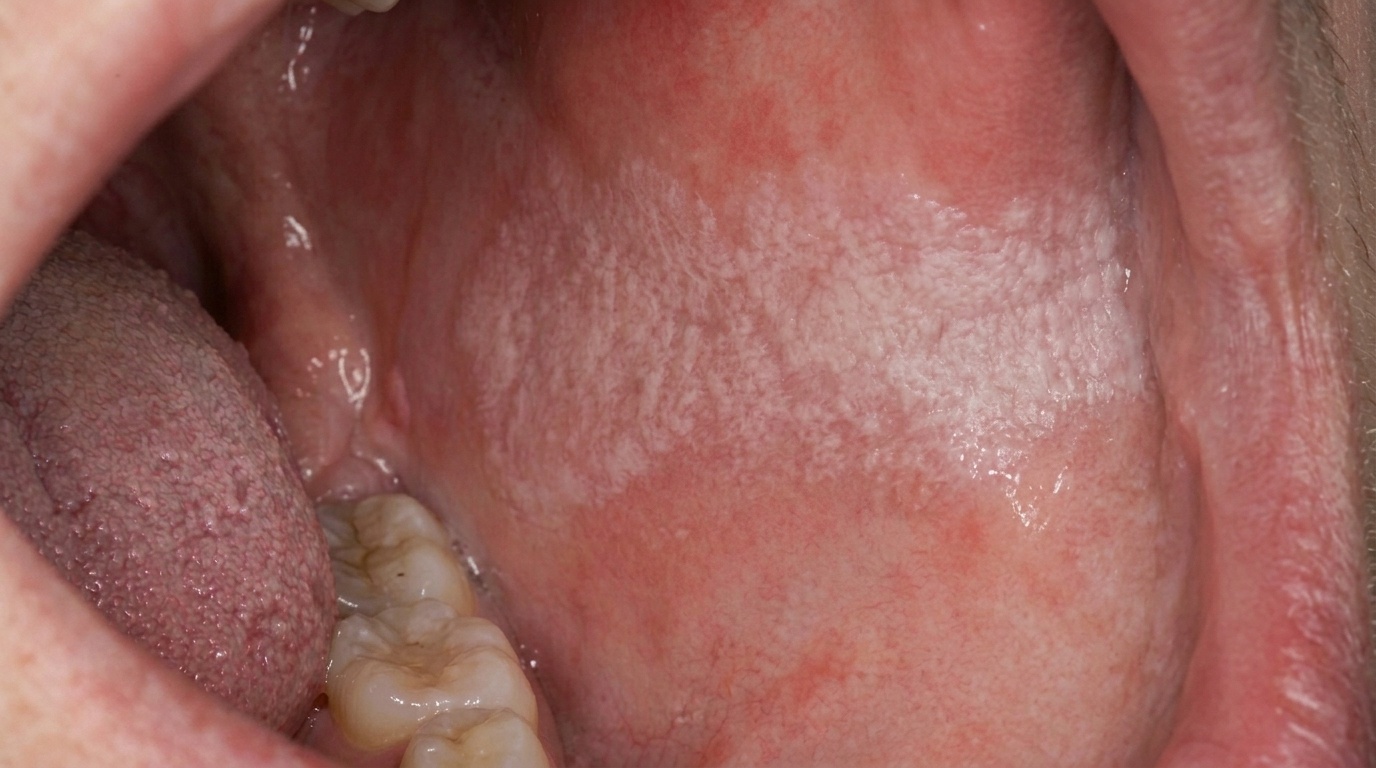
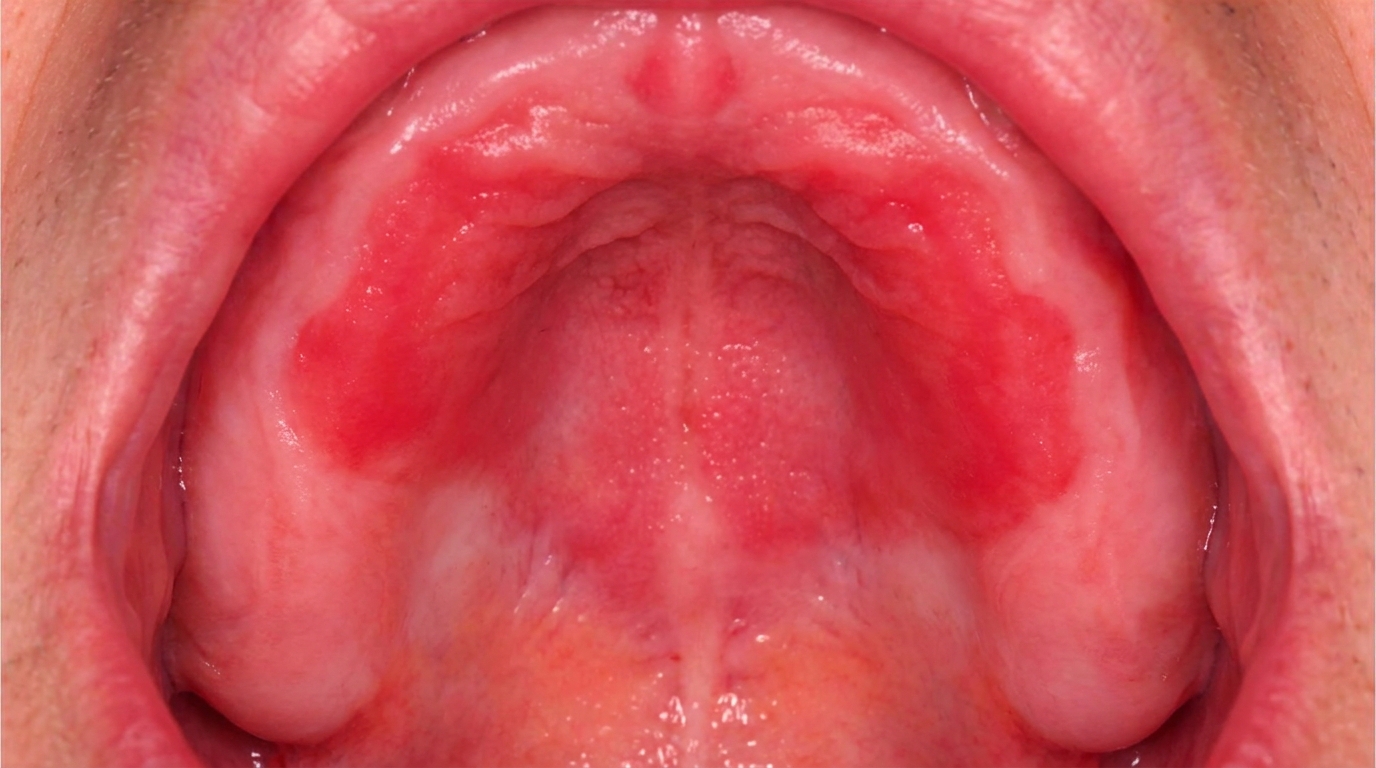
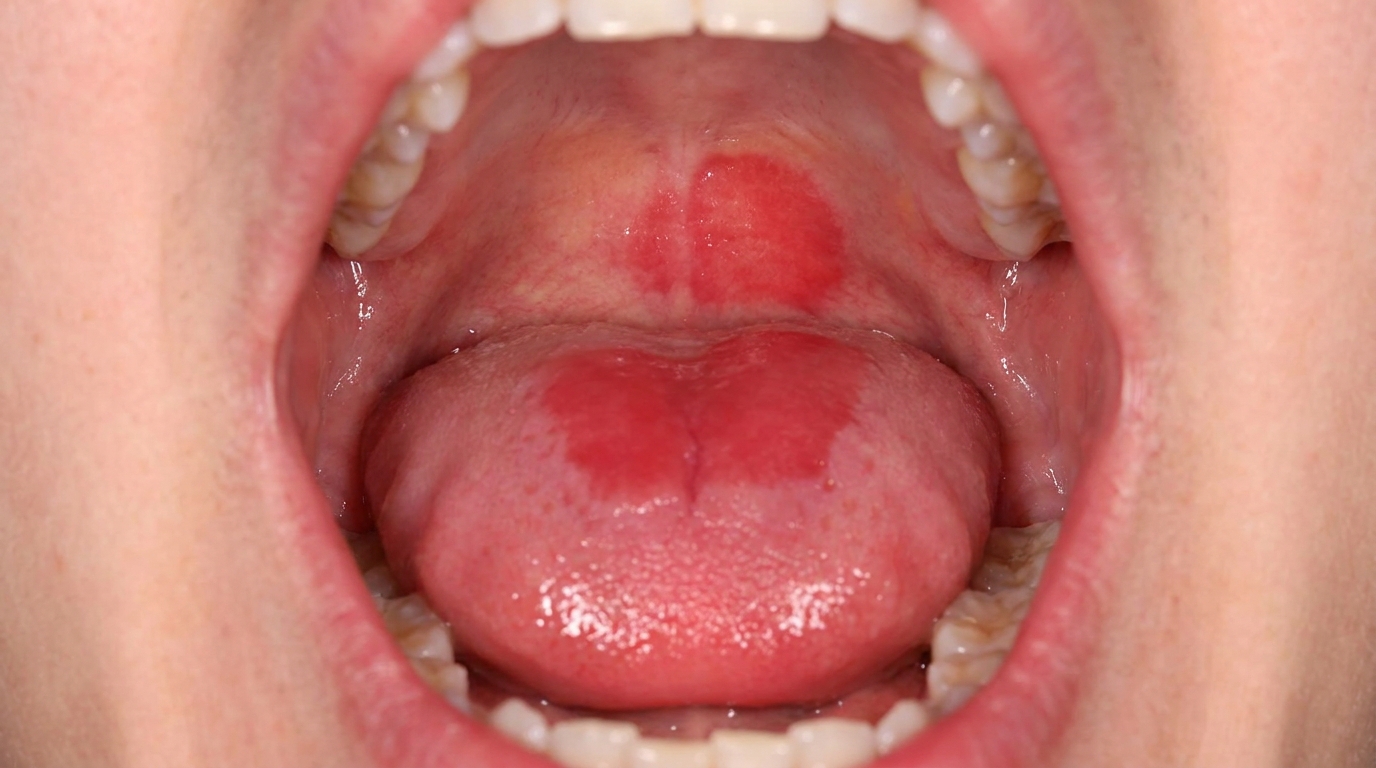
A pale, slightly thickened palate dotted with tiny red spots is one of the classic mouth changes seen in long-term smokers. It is called nicotinic stomatitis, also widely known as smoker's palate or stomatitis nicotina. While the appearance can be striking, it is usually a localised reaction to the heat of smoke rather than a dangerous disease in its own right, and on the hard palate, it generally settles after smoking stops.
This article from the team at ArtSmiles, reviewed by Dr Cristian Dunker, explains what nicotinic stomatitis is, why it happens, and how a dental check-up fits into the wider picture of smoking and oral health.
What is it?
Nicotinic stomatitis is a chronic change of the palate caused by repeated exposure to hot smoke. It involves two related features:
Diffuse white thickening (keratosis (thickened keratin layer of the surface)) of the hard palate, the front, bony part of the roof of the mouth.
Small red dots scattered through the white area, each marking the inflamed opening of a small palatal salivary gland duct (each surrounded by a slight pale ring).
The combination gives the palate a characteristic cobblestoned or dotted appearance.
The condition affects the hard palate where heat is most concentrated. The soft palate at the back is usually spared, except in heavy smokers, where it may also become slightly white.
Who tends to get it?
Nicotinic stomatitis is mostly seen in:
Pipe and cigar smokers, in whom heat is especially intense.
Heavy cigarette smokers of long duration.
Men more often than women, mirroring the historic pattern of pipe smoking.
People who hold a cigarette in the mouth without removing it, allowing heat to reach the palate.
Reverse smokers, those who hold the lit end of the cigarette inside the mouth (a practice in some communities). This form is much higher risk and is discussed separately.
What causes it?
The main trigger is heat from smoking, with a contribution from chemicals in the smoke. Heat dries the surface lining of the palate, prompting the body to lay down a thicker, keratinised (with a thicker protective surface layer) layer in protection. The salivary gland duct openings become inflamed because saliva flow is interrupted as it tries to reach the heated surface.
Things that contribute to severity include:
The temperature of the smoke (pipe and cigar smoke are hotter at the palate level).
The duration of the smoking habit.
The frequency of smoking through the day.
Holding the smoke in the mouth before exhaling.
Drinks consumed at very high temperatures (extremely hot tea or coffee) can produce a similar but milder appearance and may add to the picture.
How does it develop?
The course is gradual:
With repeated heat exposure, the palate produces a thicker keratin layer to protect itself.
Small salivary gland ducts in the palate become inflamed, producing the central red dots.
Over months to years, the appearance becomes more pronounced and the white area expands.
After smoking stops, the palate gradually returns to normal, usually within a few weeks for milder cases, occasionally longer for heavy long-term smokers.
What might you notice?
In many patients, nicotinic stomatitis causes no symptoms at all. Common observations include:
A pale, white roof of the mouth that does not look like the rest of the lining.
Tiny red spots scattered throughout the white area.
A rough or stippled feel when the tongue is pressed against the palate.
Slight burning with hot food or drink.
Stained teeth and breath odour, both linked to the same smoking habit.
What an X-ray might show
Nicotinic stomatitis is a surface change of the palate lining and does not show on X-rays. Imaging is reserved for ruling out bone involvement if a suspicious mass or ulcer is found alongside.
What happens at the dentist?
When a smoker comes in for a check-up, the visit usually involves:
A thorough mouth examination, with attention to the palate, lips, gums, tongue, floor of mouth and back of throat.
A discussion of smoking habits, including duration, type and any reverse smoking patterns.
A photograph of the palate for the record so we can monitor change over time.
A check for related conditions, leukoplakia, erythroplakia, oral cancer, smoker's melanosis, candidiasis.
A simple test, if the change is on the hard palate alone and matches the typical pattern, no biopsy is needed. If anything is unusual, particularly white patches that do not match the heat-exposure pattern, a small sample may be taken.
Cessation support. With your permission, we discuss simple steps and refer you to your GP, the Quitline or pharmacy-based support if you would like help.
Is this serious?
For most patients, nicotinic stomatitis on the hard palate is considered a relatively low-risk change in itself. It is reversible with smoking cessation. The reasons it still deserves attention are:
Marker for risk. It is the visible sign of a much larger smoking habit that affects the whole body.
Other oral cancer sites. The same smoking that causes nicotinic stomatitis also raises the risk of cancer in the floor of mouth, lateral tongue, lip and oropharynx (the back of the mouth and throat), sites that need separate examination.
Reverse smoking. When the lit end is held inside the mouth, the palate change is considered a potentially malignant disorder (a condition that carries a real risk of progressing to cancer), and biopsy and close follow-up are indicated.
Persistence after stopping. A white palate change that does not fade after several weeks of cessation is investigated further with biopsy.
Could it be something else?
Other conditions can produce a white or red palate. Considerations include:
Leukoplakia, a white patch unrelated to heat or smoking, with potential to progress.
Candidiasis (oral thrush), a creamy or red palatal change, often linked to dentures or immune suppression.
Lichen planus of the palate, usually with characteristic lacy white streaks.
Reverse smoker's palate, a much more aggressive change with red, ulcerated and white areas; treated as potentially malignant.
Frictional keratosis, white change from a denture or repeated rubbing.
Squamous cell carcinoma of the palate, usually firmer, ulcerated and not following the typical heat pattern.
A specialist examination and, when needed, biopsy are the way to tell these apart.
How is it treated?
The cornerstone of management is smoking cessation:
Stopping smoking allows the palate to return close to normal in most patients.
No medical or surgical treatment is directed at the palatal change itself in standard cases.
Reverse smokers are referred for specialist review and possible biopsy.
A persistent change after cessation is investigated.
Regular dental review continues, with attention to the rest of the mouth.
We can discuss cessation support options at any visit. Combining counselling with nicotine replacement, varenicline or bupropion (under medical supervision) is the most successful approach for many patients.
What's the long-term outlook?
For nicotinic stomatitis itself, the outlook is excellent, it fades with cessation and does not, in standard cases, transform into cancer. For the smoking habit that caused it, the outlook depends on whether smoking continues. Each year of cessation lowers the risk of oral cancer, lung cancer, heart disease and many other smoking-related conditions.
If you have noticed a white change on the roof of your mouth, please book a visit. We can confirm the diagnosis, talk through cessation, and check the rest of your mouth thoroughly at the same time.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
The cover image above is an AI-generated illustration based on the most common visible features of this condition described in clinical pathology references. It is not a photograph of a real case and should not be used to diagnose or rule out the condition in your own situation. If you are concerned about something you have noticed, please book an assessment with a registered dental practitioner.
References
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2016). Oral and maxillofacial pathology (4th ed., Ch. 10: Epithelial Pathology, Nicotine Stomatitis). Elsevier.
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed., Ch. 16: Premalignant Conditions). Elsevier.
Regezi, J. A., Sciubba, J. J., & Jordan, R. C. K. (2017). Oral pathology: clinical pathologic correlations (7th ed., Ch. 3: Red and White Lesions). Elsevier.