Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker , Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | Acute pericoronitis, operculitis, wisdom tooth infection |
How urgent? | 🔴 See a dentist promptly, the swelling and trismus (difficulty opening the mouth, from muscle spasm) can spread into the deeper tissues of the face and neck if left untreated |
Common or rare? | Very common in young adults with partially erupted lower wisdom teeth |
Who it affects | Mostly young adults in their late teens to late twenties, when the wisdom teeth are coming through |
Who treats it | A general dentist initially; an oral surgeon may be involved if the wisdom tooth needs removing |
Based on | Neville, Cawson, Regezi |
What is it?
Pericoronitis is an inflammation of the gum tissue that sits over and around a tooth that is only partly through the gum. It happens most often around a lower wisdom tooth that has erupted only halfway, leaving a flap of gum covering part of the crown. Bacteria and food debris become trapped under that flap, the area becomes red and swollen, and the gum can feel sore, tender and sometimes very painful.
Who tends to get it?
Pericoronitis is mainly a condition of young adults. It usually develops at the age when the wisdom teeth, the third molars, are trying to erupt, which is typically the late teens through to the late twenties. The lower wisdom teeth are the most common site, because they are often slightly tilted, crowded, or do not have enough room to come through fully. People who have had supernumerary (extra) teeth or other partially erupted teeth can also be affected, but this is much less common.
What causes it?
A wisdom tooth that only partly erupts creates a stagnation area under the surrounding gum flap, called the operculum. This little pocket is almost impossible to clean properly, so bacterial plaque and food particles build up underneath. The infection that results is a mixed one, mostly involving the anaerobic bacteria (bacteria that thrive without oxygen) that thrive in low-oxygen pockets.
Several things make pericoronitis more likely to flare up:
Plaque and food trapped under the gum flap
An upper tooth biting down on the flap and traumatising it during chewing
Stress
An upper respiratory tract infection, especially tonsillitis or pharyngitis
Less commonly, an episode of acute necrotising ulcerative gingivitis in the same area
How does it develop?
Think of the gum flap over a half-erupted wisdom tooth as a small hood. Bristles cannot reach underneath it, so plaque slowly accumulates against the crown of the tooth and the inside of the hood. The body responds with the usual signs of inflammation, redness, swelling and tenderness, and the flap itself starts to enlarge. Once swollen, the flap drains even more poorly, which lets the bacterial population grow further and the cycle accelerates.
If the upper wisdom tooth bites down on the swollen flap each time the jaws close, the tissue is further bruised and irritated, which keeps the inflammation going. In more severe episodes, pus can form within the pocket, producing an abscess. From there, the infection can track backwards along the deeper tissues of the face and neck.
What might you notice?
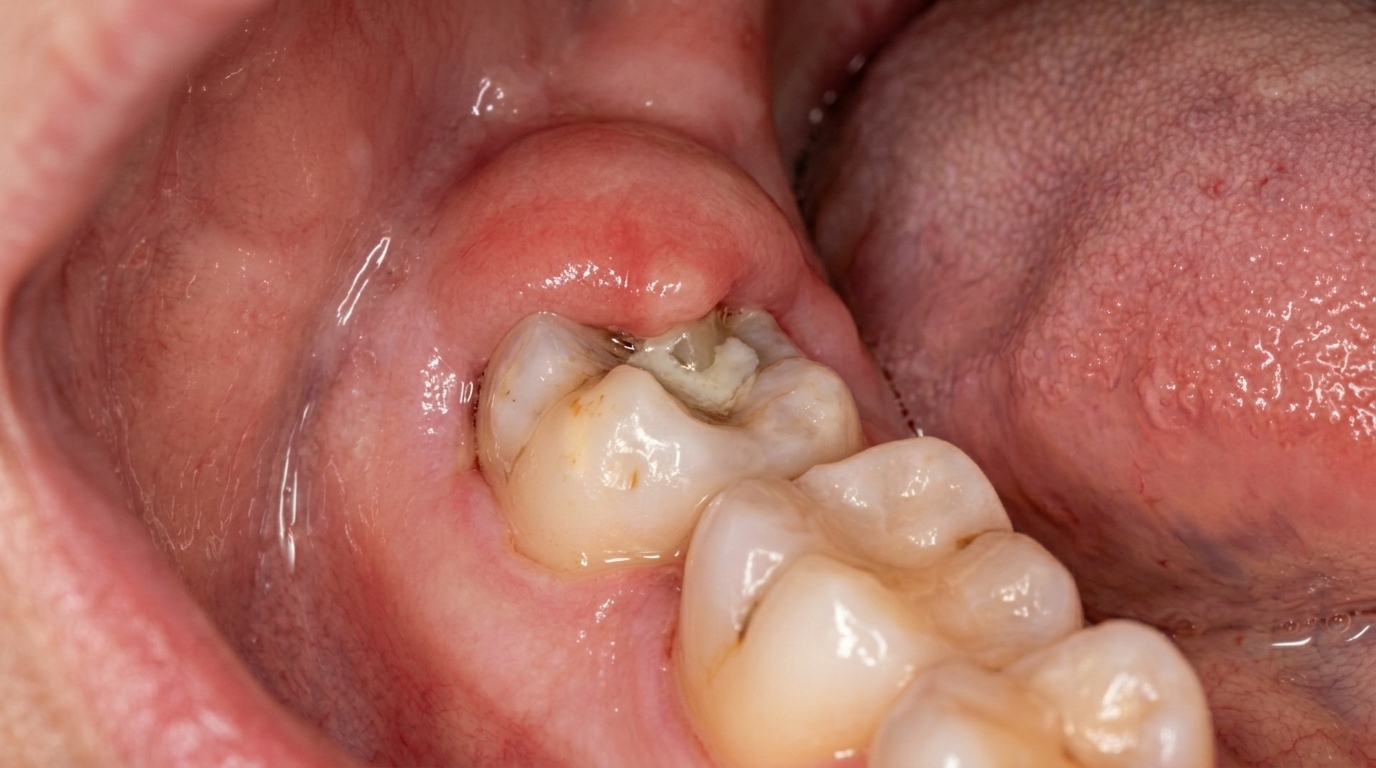
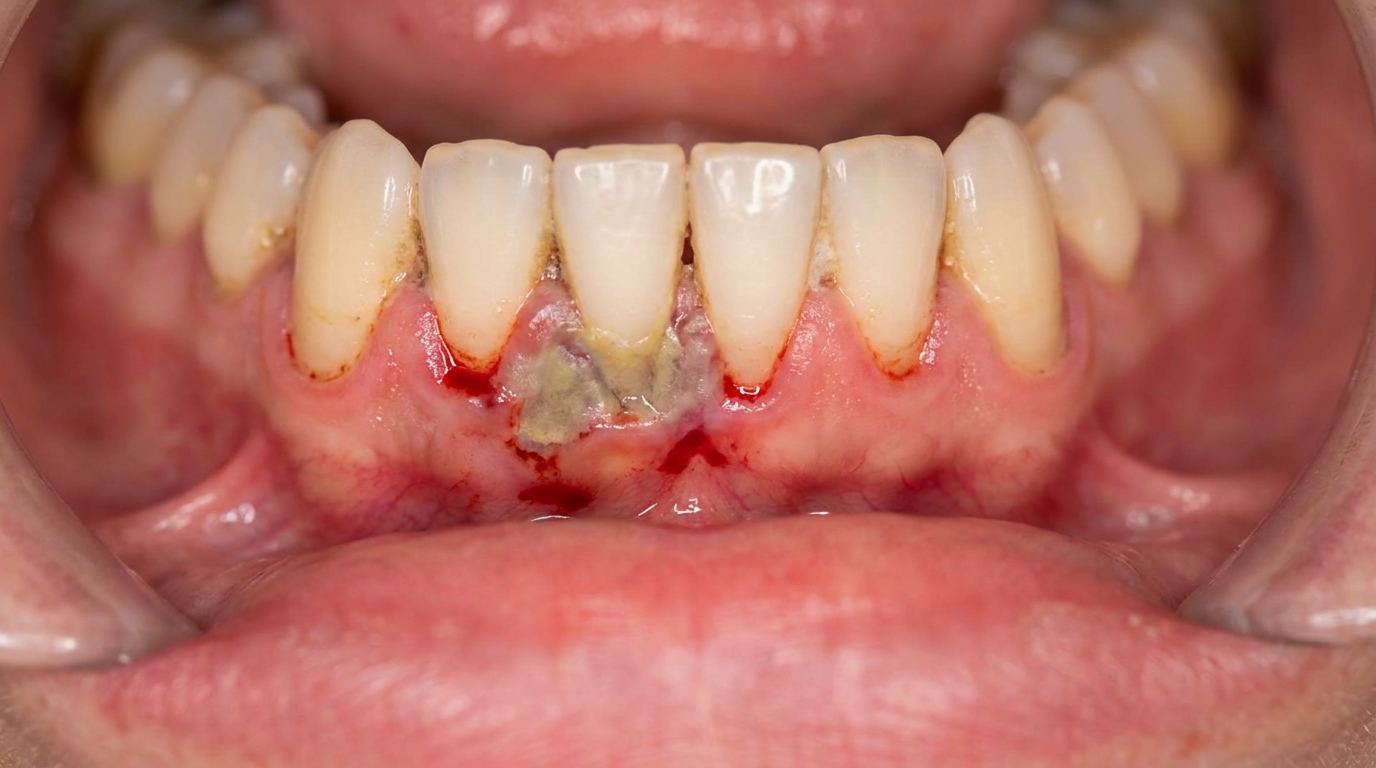
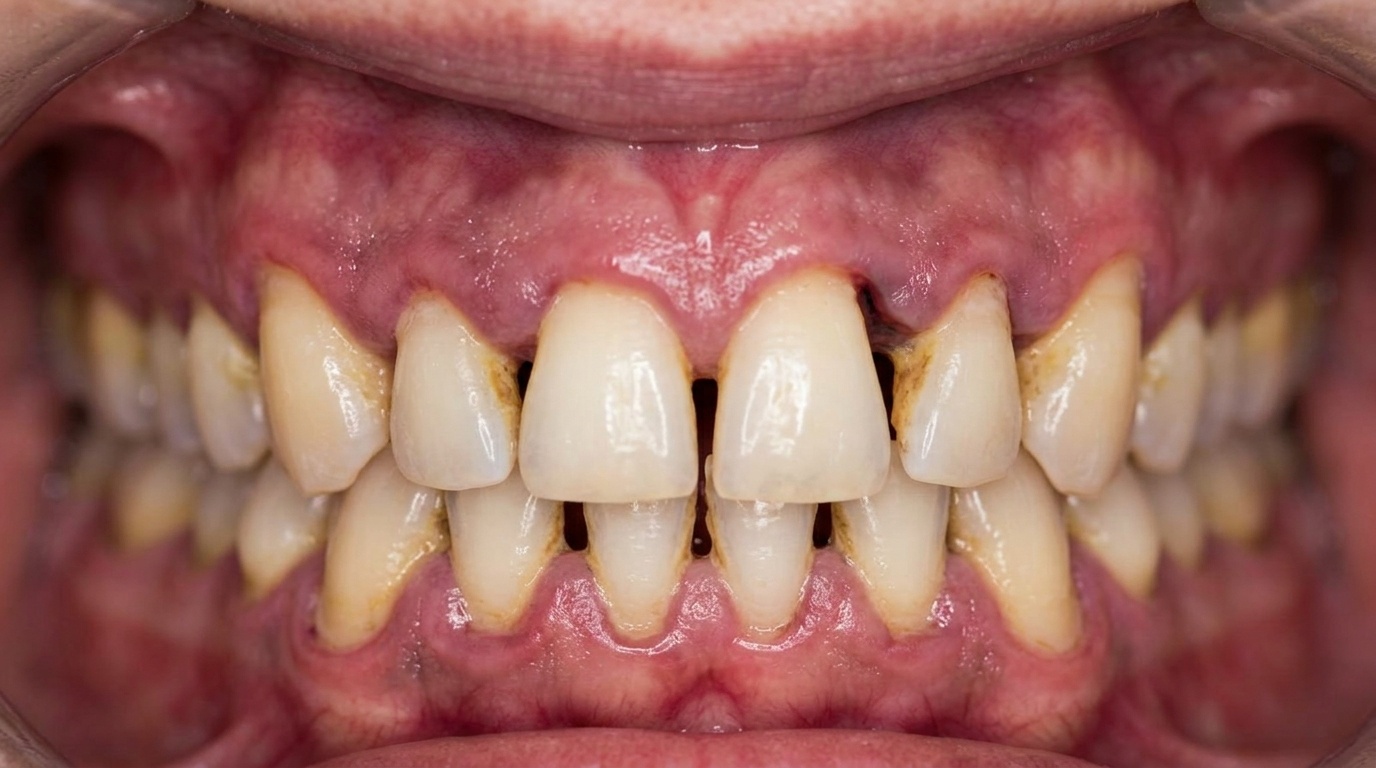
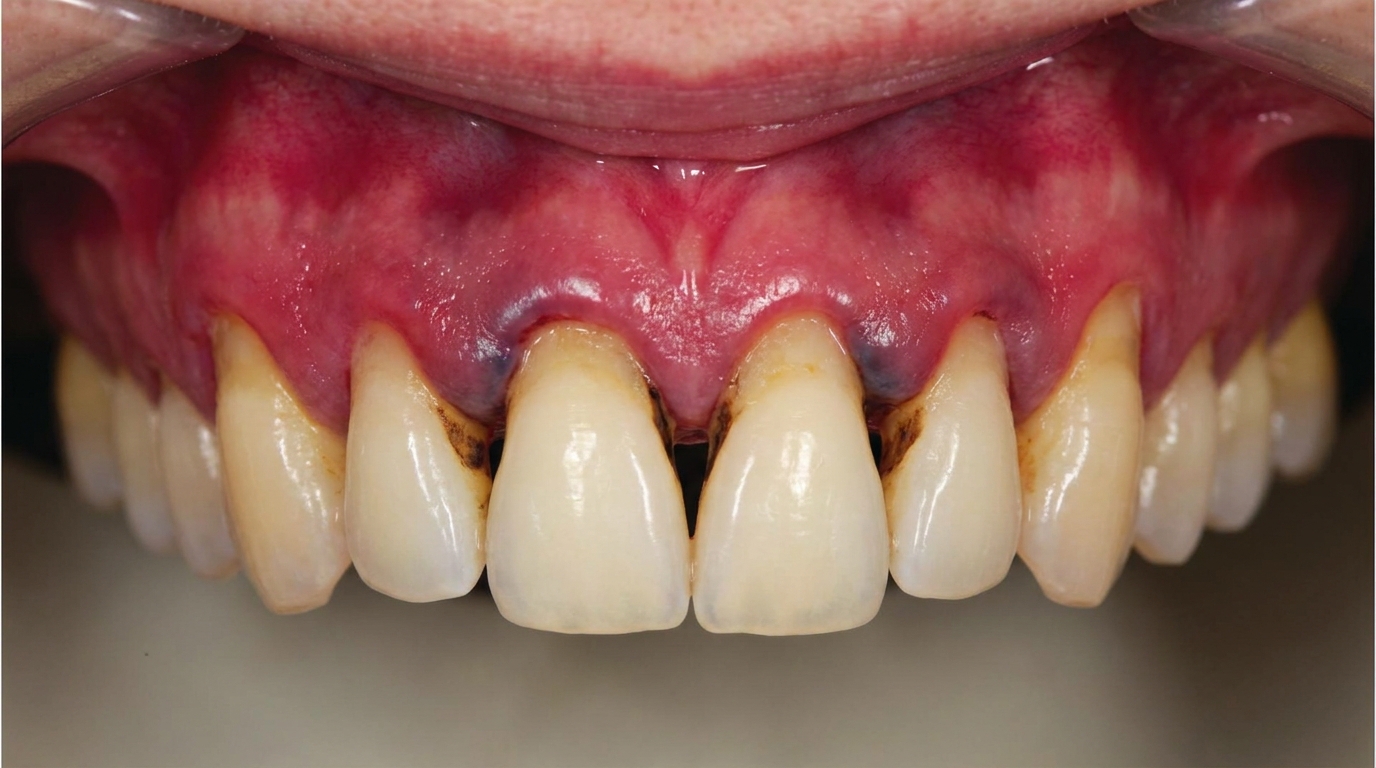
What it looks like
The gum behind the last lower tooth on one side often appears red, puffy and shiny. There may be a visible flap of swollen tissue partly covering the crown of the wisdom tooth. Sometimes a yellowish discharge can be expressed from underneath the flap. The lymph nodes under the jaw on the affected side may feel enlarged and tender.
What it feels like
The most common feelings are soreness and tenderness around the partially erupted tooth, along with a constant dull ache that can build into a throbbing pain. The pain can radiate forward into the jaw, up to the ear, into the floor of the mouth, or back into the throat. A bad or foul taste from the area is typical, and many people find it harder to open their mouth fully, a symptom called trismus, which is caused by spasm in the chewing muscles near the inflamed area. Some people develop a fever and feel generally unwell, with swollen lymph nodes in the neck.
What an X-ray might show
An X-ray, often a panoramic image of the lower jaw, is usually taken to assess the position of the wisdom tooth, how it is angled, how close its roots are to the nerve in the lower jaw, and its relationship to the second molar. In long-standing or recurrent cases, the X-ray may show extensive bone loss around the wisdom tooth and its neighbour.
What happens at the dentist?
At ArtSmiles, a dentist will usually identify pericoronitis from the history and a careful look at the back of the mouth. They will check for the partially erupted tooth, the swollen operculum (the flap of gum sitting over a partly erupted tooth), the presence of pus, the size of the local lymph nodes and whether the patient has a fever. The position of the affected tooth, its relationship to the second molar, and any complicating factors are then assessed with a radiograph.
If the swelling and trismus (difficulty opening the mouth, from muscle spasm) are severe enough that the area cannot be examined comfortably, the dentist may focus first on settling the acute infection before doing a full assessment. In some cases, particularly when the swelling is spreading, the patient is unwell, or there are signs of a deeper infection, a referral to an oral and maxillofacial specialist or to hospital may be appropriate.
Is this serious?
🔴 Pericoronitis should be taken seriously and assessed promptly. In most cases the infection stays local and settles with treatment, but pus can track backwards from the operculum into the deeper tissue spaces of the face and neck. Serious fascial space (the connective-tissue plane between muscles where infection can spread) infections, cellulitis (a spreading bacterial infection through the soft tissues) and, more rarely, osteomyelitis (infection of the jawbone itself) can follow. Before antibiotics were available, infection from pericoronitis was a relatively common cause of death in young adults, a useful reminder that this is not just a minor nuisance.
In people with sickle cell disease, an acute pericoronitis can even precipitate a sickling crisis, so prompt treatment is especially important. Both treated and untreated acute episodes can also become chronic if the operculum is not addressed, leading to recurrent flare-ups and ongoing bone loss around the wisdom tooth and its neighbour.
If you have noticed any of these signs for more than two weeks, it is worth booking an assessment.
Could it be something else?
Several other conditions can cause pain, swelling or a bad taste at the back of the mouth, and a dentist will work through these to be sure of what is going on:
Periodontal (lateral) abscess, also produces a localised, painful, tender swelling of the gum, but it usually arises from a deep periodontal pocket alongside an existing tooth rather than from the gum flap of a partially erupted one.
Acute apical periodontitis, pain from a dying or dead tooth nerve can also be severe and localised, but the affected tooth is typically very tender to bite on, and the pain often follows a history of a deep cavity, a large filling or a previous dental injury.
pulpitis (inflammation of the pulp), inflammation inside the tooth itself causes sharp pain triggered by hot or cold, rather than the constant aching, swelling and trismus typical of pericoronitis.
Acute necrotising ulcerative gingivitis, produces sore, bleeding, ulcerated gums with a characteristic foul breath, but the ulceration tends to follow the gum margins around several teeth rather than concentrating around one wisdom tooth.
HIV-associated necrotising gingivitis or periodontitis, can look similar in the early stages but is typically more generalised and rapidly destructive, and usually occurs in someone with known immune compromise.
Inflamed dentigerous cyst, a fluid-filled cyst around the crown of an unerupted tooth can cause swelling and discomfort. It is usually visible on a radiograph as a well-defined area of bone loss around the crown, which pericoronitis alone does not produce.
Paradental cyst (buccal bifurcation cyst), an inflammatory cyst that can develop alongside a partially erupted lower molar with a history of repeated pericoronitis. It is distinguished radiographically and at biopsy after the acute infection has settled.
Primary herpetic gingivostomatitis, a viral infection causing widespread mouth ulcers, sore gums and fever. The pattern of small, blistering ulcers across many areas of the mouth, rather than swelling around a single wisdom tooth, helps tell them apart.
Alveolar osteitis (dry socket), severe, throbbing pain at the back of the lower jaw a few days after a tooth is removed. The history of a recent extraction, rather than a partially erupted tooth still in place, is the key difference.
submasseteric (under the main chewing muscle of the cheek) or other fascial space abscess, a deeper infection that produces profound trismus and facial swelling. This may actually start as a pericoronitis that has spread, and a dentist will look carefully for the original source.
Herpes zoster (shingles) of a facial nerve branch, can cause severe, aching, toothache-like pain, but a tell-tale rash usually appears within a few days, and there is no swollen flap or pus to find.
How is it treated?
While waiting to be seen, gentle warm saltwater rinses several times a day, careful brushing of the area, and over-the-counter pain relief can help calm the symptoms a little. They will not, however, resolve the underlying problem.
In the dental chair, treatment usually follows a step-by-step plan:
Local cleaning of the area. The dentist may gently irrigate under the gum flap with saline or an antiseptic to flush out food debris and bacteria.
Pain relief and home care advice. Warm saltwater rinses are often recommended several times a day, and the patient is usually asked to return for review within a day or two.
Antibiotics in selected cases. If there is a fever, swollen lymph nodes, spreading swelling or signs that the infection is moving beyond the local area, an antibiotic such as penicillin (sometimes combined with metronidazole) may be prescribed.
Adjusting an opposing tooth. If an upper tooth is biting on and traumatising the gum flap, the dentist may smooth the cusps of the upper tooth, or in some cases recommend that the upper tooth itself be removed, particularly if the lower wisdom tooth is also going to be taken out.
Removing the gum flap (operculectomy). If the wisdom tooth is in a reasonable position and worth keeping, the gum flap can be surgically removed once the acute infection has settled, followed by thorough cleaning of the area to prevent further build-up.
Removing the wisdom tooth. If the radiograph shows that the tooth is poorly positioned, impacted, decayed, or unlikely to ever come through fully, removal is generally recommended once the acute infection has settled. Extraction during the acute stage is usually avoided, because the infection can spread more easily at that point.
Hospital referral. If the patient is very unwell, has high fever, marked trismus or signs of a spreading fascial space infection, urgent referral to a hospital oral and maxillofacial team is appropriate.
What's the long-term outlook?
For most people, an episode of pericoronitis settles within several days once the area has been cleaned and the underlying cause addressed. The longer-term outlook depends on what happens to the wisdom tooth itself. If the tooth is removed, or if it eventually erupts fully so that it can be cleaned properly, recurrences are unlikely. If the operculum is left in place over a tooth that will never fully erupt, the inflammation often becomes chronic, with repeated acute flare-ups and gradual bone loss around both the wisdom tooth and the second molar in front of it.
With timely treatment, serious complications such as deep facial space infection, cellulitis or osteomyelitis are uncommon. The key is not to let repeated mild episodes drift on without an assessment, because each flare-up adds to the underlying tissue and bone changes around the tooth.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
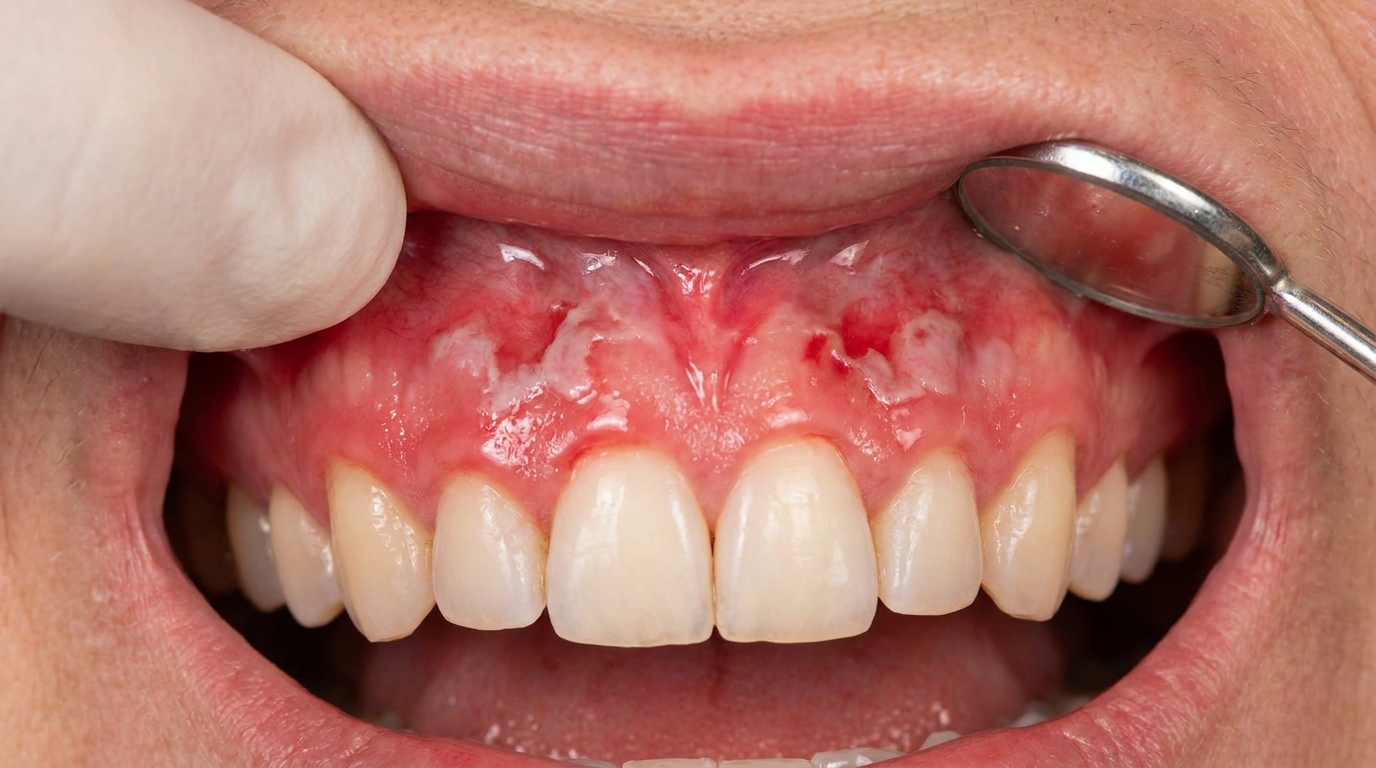
The cover image above is an AI-generated illustration based on the most common visible features of this condition described in clinical pathology references. It is not a photograph of a real case and should not be used to diagnose or rule out the condition in your own situation. If you are concerned about something you have noticed, please book an assessment with a registered dental practitioner.
References
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2023). Oral and maxillofacial pathology (5th ed.). Elsevier. Chapter 4, Periodontal Diseases, pp. 165 to 167; Chapter 2, Abnormalities of Teeth, pp. 73 to 81; Chapter 15, Odontogenic Cysts and Tumors, pp. 704 to 705.
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 5, Gingivitis and Periodontitis, pp. 91 to 92; Chapter 11, Disorders of the Temporomandibular Joints and Periarticular Tissues, p. 192; Chapter 22, Sickle cell disease, p. 338; Chapter 34, Pain, Anxiety, Neurological and Psychogenic Disorders, p. 432.
Regezi, J. A., Sciubba, J. J., & Jordan, R. C. K. (2017). Oral pathology: Clinical pathologic correlations (7th ed.). Elsevier. Chapter 8, Halitosis (oral infection causes).
Frequently asked questions
Why does pericoronitis usually affect wisdom teeth?
Pericoronitis develops when a flap of gum partially covers an erupting tooth, trapping food and bacteria. Lower wisdom teeth are by far the most common site because they often erupt incompletely or at an awkward angle, leaving a gum flap (operculum) that is hard to clean.
What does pericoronitis feel like?
Typical features include a swollen, tender gum behind the last tooth, pain on chewing or biting (sometimes the upper tooth catches on the inflamed gum), bad taste or smell from trapped food, and in some cases facial swelling, fever or trismus (limited mouth opening). Symptoms can flare and settle repeatedly.
How is pericoronitis treated?
Treatment depends on whether the wisdom tooth is functional. If the tooth is in a useful position, the gum is cleaned, irrigated and a short course of antibiotics may be given. If the tooth is impacted or repeatedly flaring, removal is the definitive treatment. Soft diet, warm salt-water rinses and pain relief help in the acute phase.
Is pericoronitis a dental emergency?
Localised pericoronitis is an urgent rather than emergency problem and can usually be managed by a dentist within 24-48 hours. Significant facial swelling, trouble swallowing, fever or difficulty opening the mouth is a warning sign that the infection is spreading and warrants emergency care.