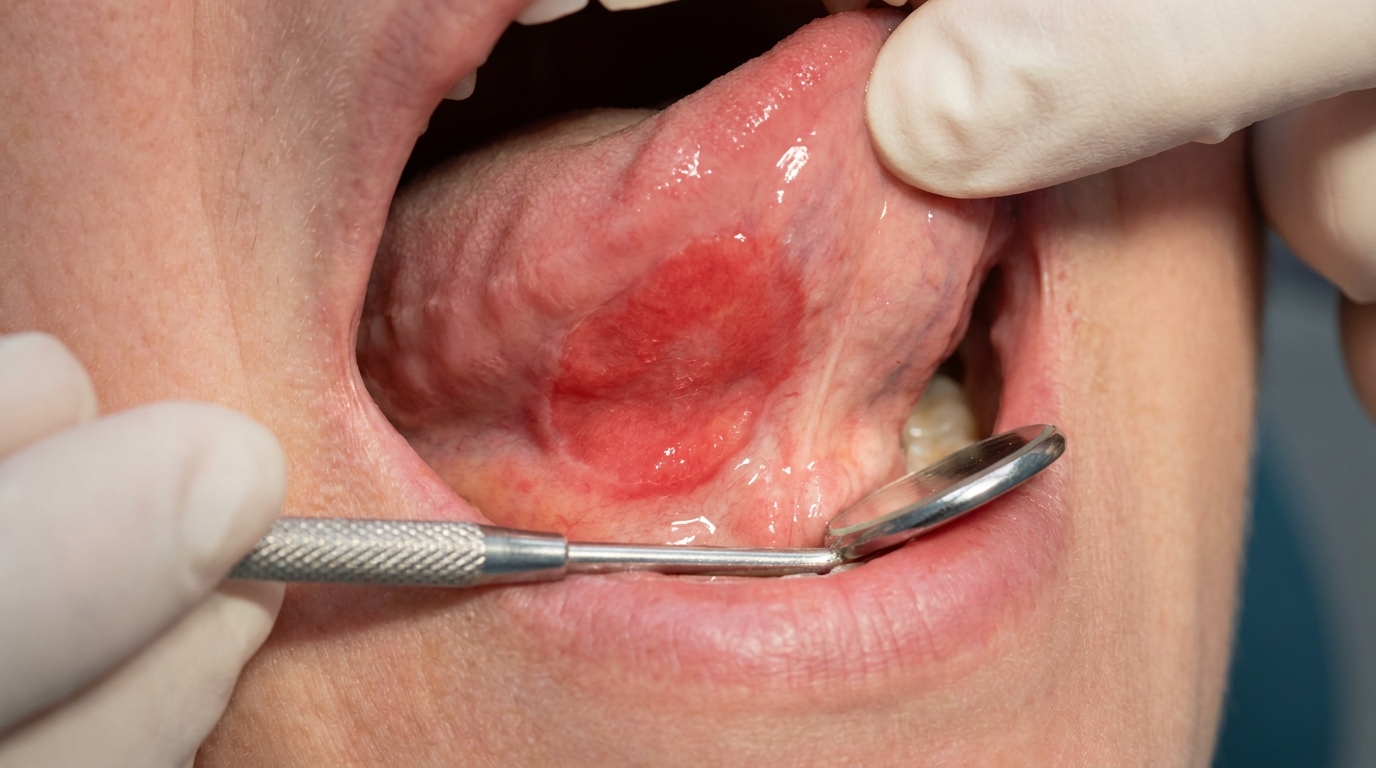
Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker , Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | Ackerman's tumour, snuff dipper's cancer, oral florid papillomatosis (older term) |
How urgent? | 🔴 See a dentist promptly, verrucous carcinoma is a low-grade form of oral cancer that can quietly destroy nearby bone if left alone |
Common or rare? | Uncommon, accounts for roughly 1 to 16% of oral squamous cell carcinomas, depending on local tobacco habits |
Who it affects | Adults, usually over 60 years of age, with a male predominance |
Who treats it | Specialist referral, diagnosis and surgical management typically involve an oral medicine specialist or oral and maxillofacial surgeon, often guided by your general dentist |
Based on | Regezi, Neville, Cawson, Laskaris |
What is it?
Verrucous carcinoma is a slow-growing, low-grade variant of oral squamous cell carcinoma, the most common form of mouth cancer. Although it is technically a cancer, it behaves quite differently from the more aggressive form: it grows outwards rather than burrowing deeply, and it almost never spreads to other parts of the body. It usually appears as a thick, white, warty patch inside the mouth.
The lesion was first described in detail in 1948 by an American pathologist called Lauren Ackerman, which is why some clinicians still call it "Ackerman's tumour".
Who tends to get it?
Verrucous carcinoma is largely a disease of older adults. The average age at diagnosis is around 65 to 70 years, and most affected people are over 50. Men are more commonly affected than women, although in communities where women regularly use dry snuff the gender pattern can flip.
The most common sites in the mouth are:
The mandibular vestibule, the gum-and-cheek fold along the lower jaw
The buccal mucosa, the inner lining of the cheeks (more than half of all cases)
The gingiva, the gums, with a slight preference for the lower gums
The tongue
The hard palate
The location often matches exactly where a person has habitually placed smokeless tobacco. In overall numbers, verrucous carcinoma is uncommon, only about one to three new oral cases are diagnosed per million people each year in Western countries.
What causes it?
The strongest known risk factor is tobacco, particularly smokeless tobacco such as chewing tobacco, snuff, and betel quid (paan). The lesion typically develops in the exact spot where tobacco has been held against the cheek or gums for years.
Other contributing factors documented in the source textbooks include:
Smoked tobacco use
Combined habits, smokeless tobacco together with smoking and alcohol
A pre-existing high-risk white patch called proliferative verrucous leukoplakia (PVL), from which verrucous carcinoma can develop over time
Human papillomavirus (HPV) types 6, 11, 16 and 18 have been detected in a small minority of cases, but a clear cause-and-effect relationship has not been established. Some lesions appear in people with no identifiable risk factors at all.
It's worth saying clearly: this is not about blame. Many people who develop verrucous carcinoma picked up tobacco habits decades ago when the risks weren't well understood. The point of identifying the cause is to remove the trigger, not to judge the patient. If you have a long tobacco history and want a soft-tissue check, our general dental services team can examine the area and arrange a specialist referral if anything looks suspicious.
How does it develop?
Think of the lining of the mouth as a layered cake of cells, with new cells made at the bottom and older keratin (the same protein that makes up fingernails) shed from the top. When tobacco chemicals sit against this lining for years, they slowly damage the DNA of the cells underneath, and the tissue begins to overproduce keratin and pile up in folds.
In many cases the mucosa first develops a flat white patch (leukoplakia) or a tobacco pouch keratosis. Over months and years, the patch may thicken, develop a corrugated or warty surface, and eventually meet the criteria for verrucous carcinoma. The cancerous cells push outwards in broad, blunt fronts rather than sending invasive fingers down into the tissue, which is why the lesion stays superficial and rarely spreads through the bloodstream or lymphatic system.
It's a slow process. Patients often have the lesion for two to three years before a definitive diagnosis is made.
What might you notice?
What it looks like
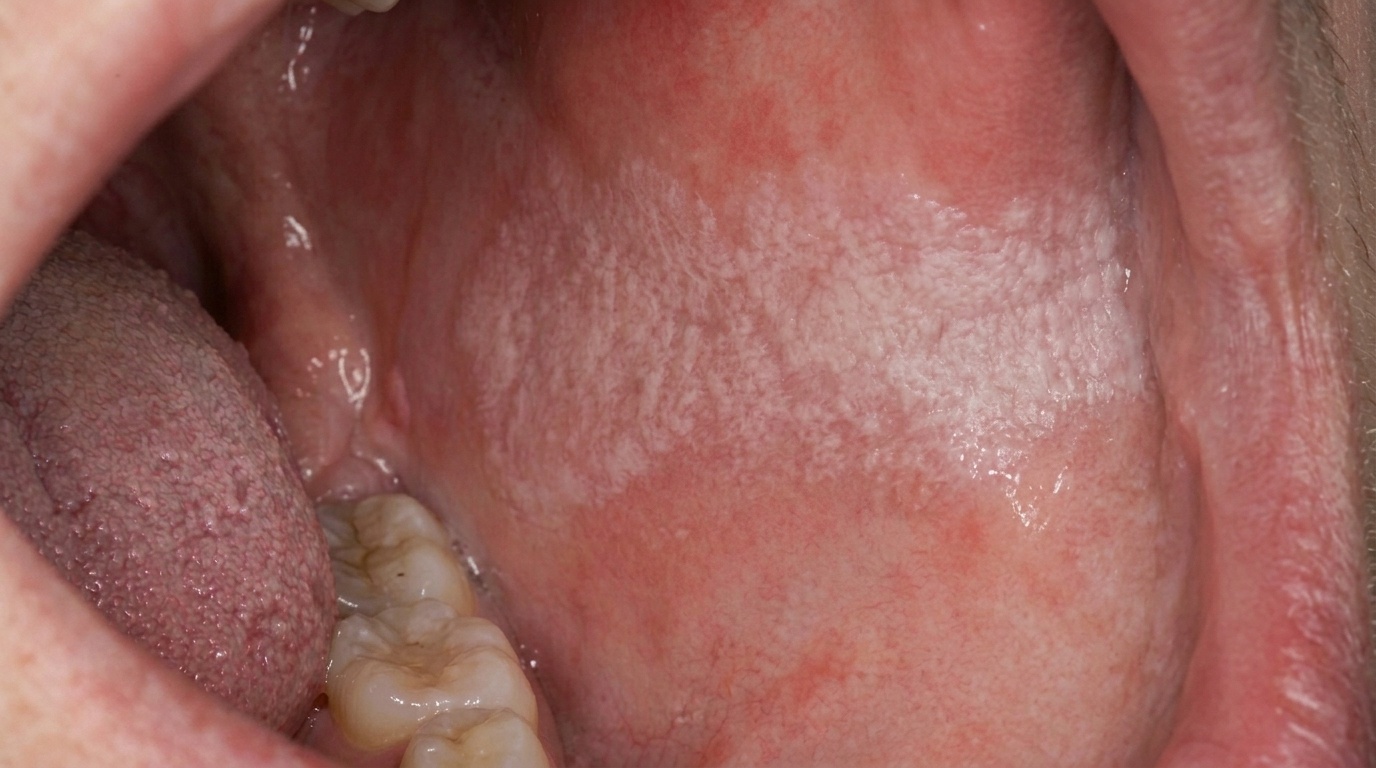
In its early stages, verrucous carcinoma may look like an ordinary white patch, a thin, slightly corrugated area that could easily be mistaken for leukoplakia or even a small papilloma.
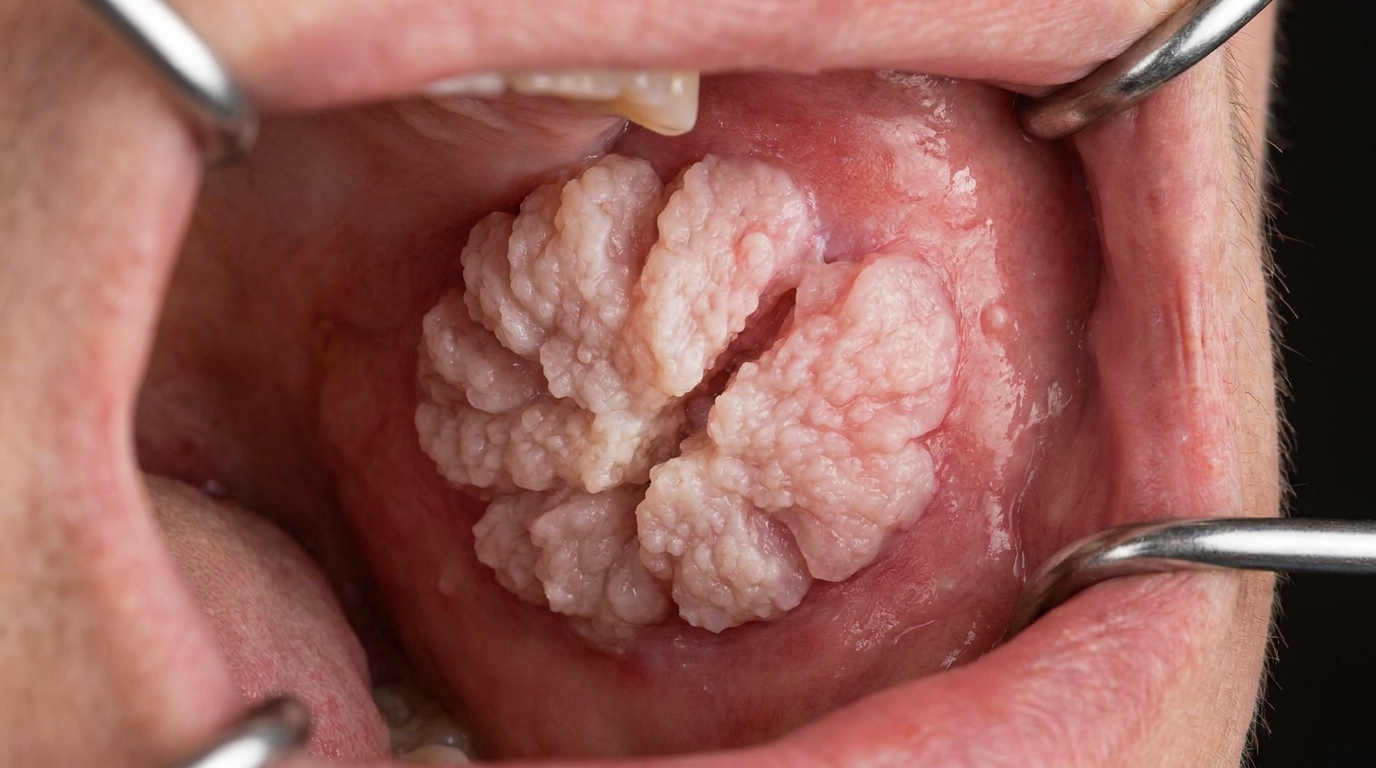
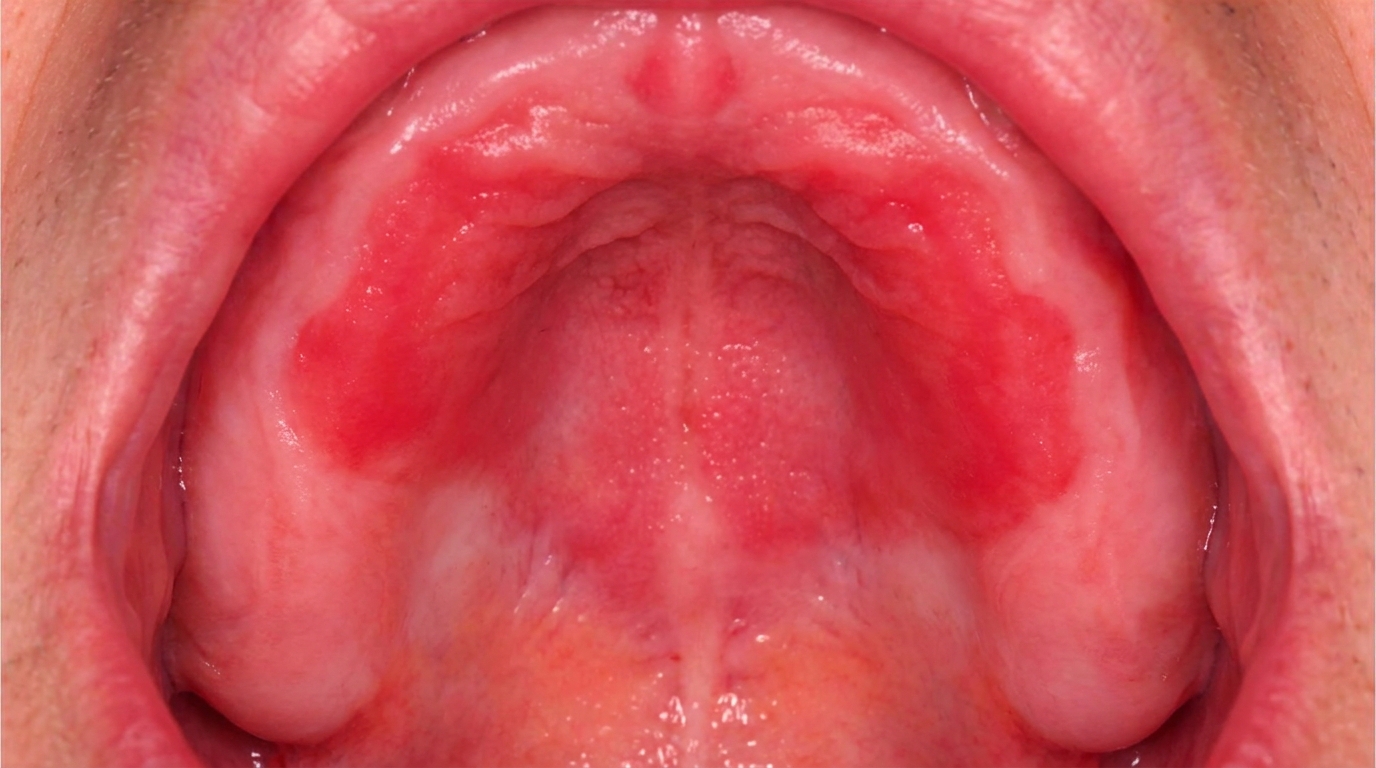
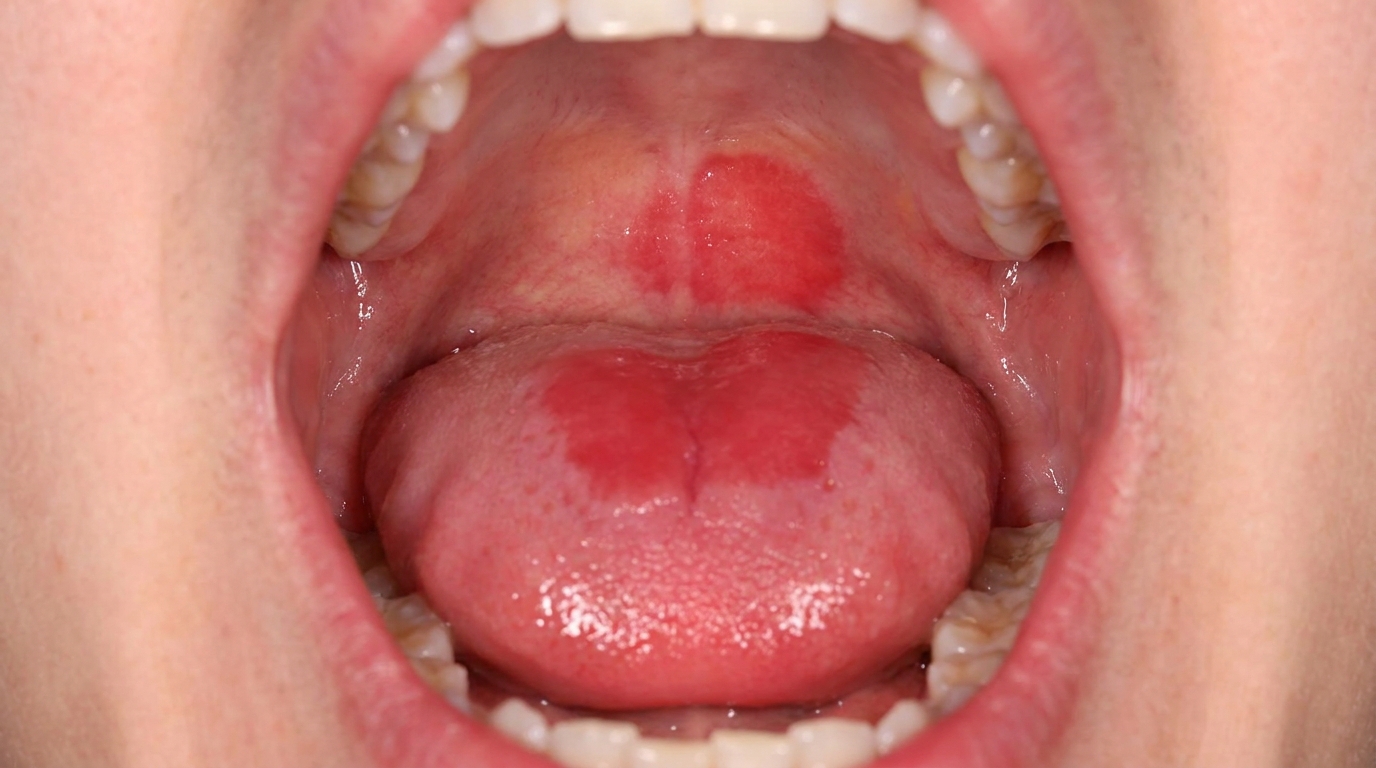
As it develops it becomes more characteristic: a broad-based, painless, thick plaque with papillary or verruciform (warty) surface projections. The lesion is usually white, but depending on how much keratin it produces and how much inflammation surrounds it, it can also appear pink, grey or even faintly red. The surface is often described as shaggy, pebbly or cauliflower-like, and the borders become irregular and feel firm to the touch.
When the lesion involves the gum, it tends to become fixed to the underlying bone over time.
What it feels like
Verrucous carcinoma is most often painless, which is part of what makes it so easy to ignore. People may notice a rough patch when running their tongue over the area, or feel that something is "in the way" of their cheek or denture. Discomfort, soreness or bleeding usually only appear in advanced lesions or where a denture rubs against the patch.
What an X-ray might show
Verrucous carcinoma typically does not destroy bone in the way conventional oral cancer does. At most, an X-ray may show gentle pressure resorption of the underlying bone, the bone smoothly thinned out beneath the lesion rather than "moth-eaten". In long-standing cases that have been left untreated, more substantial bone destruction can occur, especially in the maxilla or mandible.
What happens at the dentist?
If your dentist sees a persistent, thick, white, warty patch in your mouth, they will take it seriously. At ArtSmiles, the clinical examination usually includes:
Careful inspection and palpation (gentle feeling) of the lesion and the surrounding mucosa
Examination of the rest of the mouth for other white or red patches, since verrucous carcinoma can arise alongside leukoplakia or PVL
Examination of the lymph nodes in the neck, although enlarged nodes in verrucous carcinoma usually represent reactive inflammation rather than spread of the cancer
A discussion of tobacco, alcohol and betel quid history
Because verrucous carcinoma can look deceptively benign under the microscope, a generous incisional biopsy is essential, a small slice that includes the full thickness of the surface and a piece of the underlying connective tissue. A superficial shave biopsy is not enough. The pathologist needs to see the architectural pattern of the broad, pushing rete ridges (the finger-like projections of surface tissue into the underlying connective tissue) to make the diagnosis with confidence.
Adequate sampling matters for another reason too: in up to 20% of verrucous carcinomas, a focus of conventional (more aggressive) squamous cell carcinoma is hiding within the lesion. Catching that changes the treatment plan.
Imaging may be ordered if the lesion sits over bone or extends deeply, and a referral to an oral medicine specialist or an oral and maxillofacial surgeon is the standard pathway, coordinated by your general dentist.
Is this serious?
🔴 Yes, this is one to act on.
The good news first: verrucous carcinoma rarely metastasises (spreads to distant parts of the body) (spreads to distant sites), and once diagnosed and treated, the long-term outlook is excellent. Around 90% of patients are disease-free five years after surgery.
The sober news: it is still a cancer. Left untreated, it gradually invades and destroys neighbouring tissues, periosteum (the thin layer of tissue covering bone), bone, cartilage, muscle and salivary glands. And because conventional squamous cell carcinoma can develop within the lesion in up to one in five cases, what looks like a stable warty patch can occasionally harbour a more dangerous tumour. A small proportion of long-standing verrucous carcinomas do progress to invasive squamous cell carcinoma, which can then metastasise.
If you've noticed a thickening white or warty patch in your mouth for more than two weeks, especially in the cheek pouch or along the gum, it's worth booking an assessment.
Could it be something else?
Several other oral lesions can mimic verrucous carcinoma. The source textbooks list a wide range of conditions in the differential diagnosis, and only a biopsy can reliably tell them apart.
Conventional squamous cell carcinoma, the more aggressive form of mouth cancer. It can also appear as a white or mixed white-and-red patch, but tends to grow more rapidly, ulcerates more readily, feels indurated (firm and hardened) (hardened) deeper down, and is more likely to spread to neck lymph nodes.
Papillary squamous cell carcinoma, looks like verrucous carcinoma on the surface but is less differentiated under the microscope. A dentist or pathologist distinguishes it by its more infiltrative growth pattern, greater cellular atypia (cells that look microscopically abnormal) and faster clinical progression.
Carcinoma cuniculatum, another well-differentiated squamous cell carcinoma variant. The surface looks subtly papillary or cobblestone-like, but unlike verrucous carcinoma it burrows deeply into bone and creates branching keratin-filled tunnels visible on biopsy and "moth-eaten" lytic changes on X-ray.
Verrucous hyperplasia, a benign thickened white lesion that is the precursor to verrucous carcinoma. It can look identical clinically; the pathologist tells them apart by whether the lesion grows downward into the connective tissue (verrucous carcinoma) or only upward above the surrounding mucosa (verrucous hyperplasia).
Proliferative verrucous leukoplakia (PVL), a high-risk white patch disorder that causes multiple, persistent, slowly enlarging warty plaques. PVL can be indistinguishable from verrucous carcinoma at one stage, and verrucous carcinoma can develop directly out of PVL. Long-term clinical follow-up and serial biopsies are how clinicians track the difference.
Leukoplakia (homogeneous and non-homogeneous), flat or slightly textured white patches that cannot be wiped off. Early verrucous carcinoma can be initially mistaken for leukoplakia; biopsy and the development of a more warty, exophytic (raised and projecting from the surface) surface point to verrucous carcinoma.
Squamous papilloma, a small, soft, finger-like benign growth caused by HPV. Papillomas are usually solitary, pedunculated and small (under a centimetre), whereas verrucous carcinoma is broad-based and progressively enlarging.
Condyloma acuminatum, another HPV-associated wart-like growth. It tends to be smaller, softer, often multiple, and typically affects younger patients with sexual transmission as the route of infection.
Verruciform xanthoma, a rare benign pebbly lesion that can appear yellow-white or red and stays small. Histology, not clinical examination, is the only reliable distinguisher.
White sponge naevus, a hereditary spongy white thickening of the cheek mucosa, usually present from childhood and bilateral, in contrast to the unilateral, acquired and progressive nature of verrucous carcinoma.
Keratoacanthoma, a fast-growing keratin-filled lesion of sun-exposed skin and lips that develops over weeks rather than years and often regresses spontaneously, unlike the relentlessly progressive verrucous carcinoma.
How is it treated?
At home, the most important step is removing the trigger. That means stopping all forms of tobacco, smoked, chewed, snuffed and in betel quid, and reducing alcohol. Your dentist or GP can help connect you with cessation support.
Professionally, surgical excision is the treatment of choice. Because verrucous carcinoma rarely metastasises and its borders are well demarcated, the surgery generally does not need to be as extensive as for conventional oral cancer of a similar size. The aim is complete removal with clear margins. Reconstruction may be needed for larger lesions, particularly those involving the gum or palate.
A neck dissection (removal of lymph nodes) may be considered if neck nodes are clinically enlarged, although these usually turn out to be reactive rather than truly involved. If the bone has been significantly invaded, a more extensive resection may be necessary.
Radiotherapy is an alternative for patients who can't tolerate surgery, although it provides poorer local control. Older concerns that radiation could cause the lesion to transform into a more aggressive cancer have been reassessed in recent literature and now appear less significant than once feared. Limited reports describe responses to chemotherapy, photodynamic therapy and combined chemoradiotherapy, but surgery remains the standard.
Long-term follow-up is essential because the same field of altered tissue that produced one verrucous carcinoma can produce another lesion later, a phenomenon called field cancerisation (a wider area of mucosa that carries the same risky changes).
What's the long-term outlook?
The prognosis for verrucous carcinoma is genuinely excellent, one of the most favourable outcomes of any oral cancer. Approximately 90% of patients remain disease-free five years after surgical treatment, and the cancer rarely spreads to other parts of the body.
That said, two long-term realities are worth knowing:
Local recurrence is possible if the original lesion was not fully excised, and some patients require at least one further procedure during the first few years.
New primary lesions can develop in the same field of tobacco-damaged mucosa, which is why ongoing dental review and continued tobacco cessation are so important.
With timely diagnosis, complete surgical removal and the abandonment of tobacco habits, most patients can expect a normal life expectancy and good function. The earlier the lesion is recognised and removed, the simpler the surgery and the better the long-term outcome.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
The cover image above is an AI-generated illustration based on the most common visible features of this condition described in clinical pathology references. It is not a photograph of a real case and should not be used to diagnose or rule out the condition in your own situation. If you are concerned about something you have noticed, please book an assessment with a registered dental practitioner.
References
Regezi, J. A., Sciubba, J. J., & Jordan, R. C. K. (2017). Oral pathology: Clinical pathologic correlations (7th ed.). Elsevier. Chapter 6, Verrucal-Papillary Lesions, pp. 154 to 158.
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2023). Oral and maxillofacial pathology (5th ed.). Elsevier. Chapter 10, Epithelial Pathology (Verrucous Carcinoma section), pp. 421 to 423.
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 17, Oral Cancer (Verrucous Carcinoma section), p. 289.
Laskaris, G. (2003). Color atlas of oral diseases (3rd ed.). Thieme. Chapter 31, Malignant Neoplasms (Verrucous Carcinoma), pp. 274 to 275.
Frequently asked questions
What is verrucous carcinoma?
Verrucous carcinoma is a low-grade variant of oral squamous cell carcinoma. It appears as a thick, white, warty or cauliflower-like patch, often in older patients with a long history of tobacco use (especially smokeless tobacco). It grows slowly outwards (exophytically) and rarely spreads to lymph nodes, but it is still cancer and needs treatment.
How is verrucous carcinoma different from leukoplakia?
Leukoplakia is a flat or slightly raised white patch with a thin keratin layer. Verrucous carcinoma is thicker, warty, and has a deeply furrowed or pebbled surface. Biopsy is the only reliable way to distinguish them, and any leukoplakia that becomes warty needs urgent reassessment.
How is it diagnosed?
Diagnosis requires biopsy, ideally a generous incisional or excisional sample, because superficial biopsies can underestimate the lesion and miss any deeper conventional carcinoma. Imaging is used to map the extent of large lesions before surgery.
How is verrucous carcinoma treated?
Surgical excision with clear margins is the treatment of choice. Because spread to lymph nodes is rare, neck dissection is usually not needed. Radiotherapy is generally avoided as it can transform verrucous carcinoma into a more aggressive cancer in some cases. Lifelong follow-up is essential.