Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker , Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | Mucous cyst, mucous extravasation phenomenon, mucus escape reaction, mucous extravasation cyst, mucus retention cyst, sialocyst (when in the floor of the mouth: ranula) |
How urgent? | 🟡 Worth a check-up, most mucoceles are harmless, but a soft, bluish lump that lingers for more than two weeks should be examined to rule out other lesions |
Common or rare? | Very common, the most common cyst-like lesion of the oral soft tissues |
Who it affects | Most often children, teenagers and young adults, although it can appear at any age |
Who treats it | General dentist, sometimes with referral to an oral and maxillofacial surgeon for larger lesions or ranulas |
Based on | Regezi, Neville, Cawson, Laskaris |
What is it?
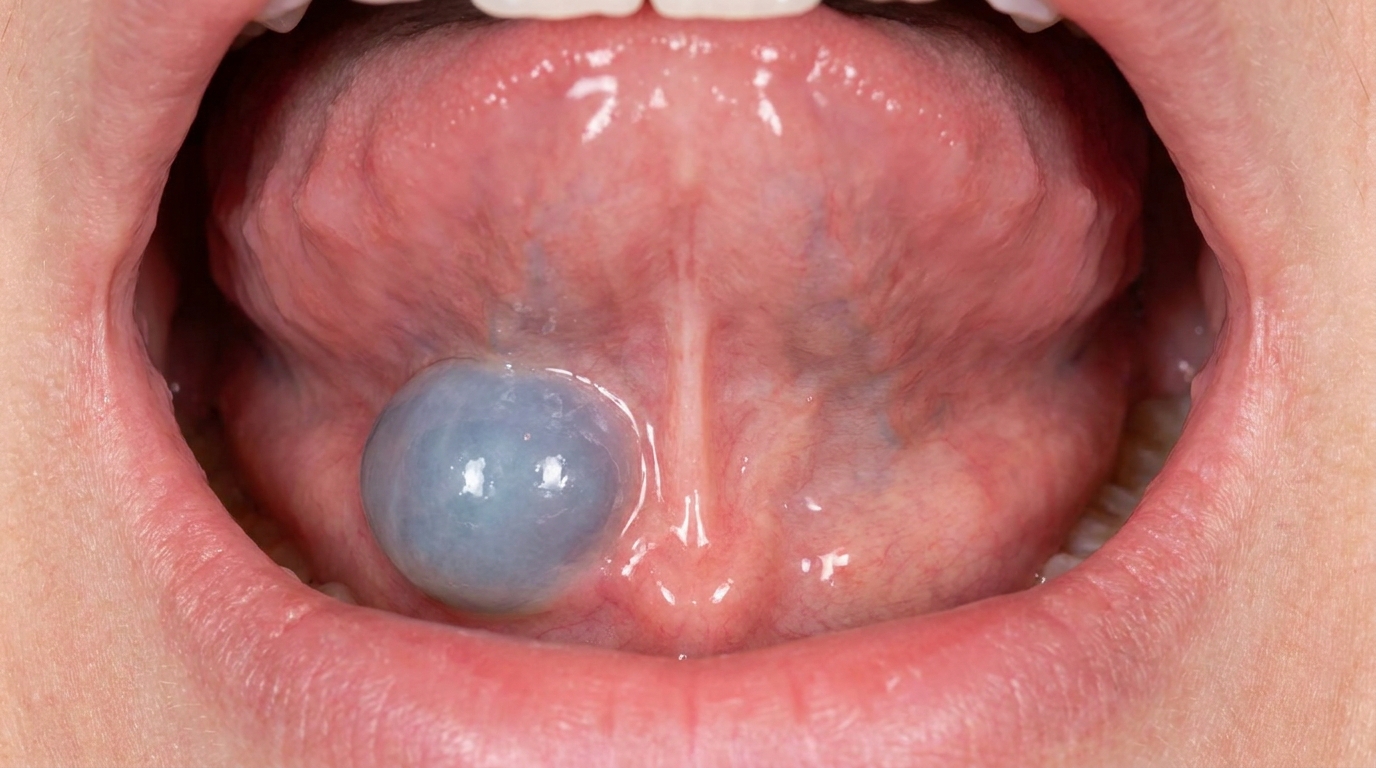
A mucocele is a small, soft, dome-shaped swelling that forms when one of the tiny saliva-producing glands in the lining of your mouth gets damaged and leaks. The leaked saliva pools just under the surface, creating a bubble-like lump that often looks bluish or translucent.
Most mucoceles turn up on the inside of the lower lip, but they can pop up on the cheek, the underside of the tongue, the floor of the mouth, or the soft palate. Although they look unusual, they are not cancerous and are not contagious.
Who tends to get it?
Mucoceles are one of the most common soft-tissue lesions in the mouth. They tend to appear in children, teenagers and young adults, with a peak in the second and third decades of life. This is partly because younger people are more likely to bite or knock their lips during everyday activities. That said, mucoceles can develop at any age, including in infants and older adults.
Men and women are affected equally. The lower lip is by far the most common site, in one large series, about 82 per cent of mucoceles were found there. Other typical sites include the floor of the mouth (where they are called ranulas), the underside of the tongue, the cheek, and occasionally the palate. They almost never form on the upper lip; a swelling there is more likely to be a salivary gland tumour and warrants careful assessment.
What causes it?
The usual culprit is minor trauma to one of the small saliva ducts that drain the mucous glands of your lip or cheek. Common triggers include:
Accidentally biting the inside of the lip or cheek
A knock to the lip from a sporting incident or a fall
Habitual lip-chewing or sucking on the lower lip
Sharp edges from broken teeth, restorations or dental appliances
Holding objects between the lips (a classic example is a referee biting on a whistle)
There are two main types of mucocele, and they form in slightly different ways:
Mucous extravasation cyst, accounts for around 80–90 per cent of cases. The duct of a small salivary gland is torn, and saliva spills into the surrounding tissue. This is not a true cyst because it has no proper lining; it is walled off only by compressed connective tissue.
Mucous retention cyst, much less common. Here, the duct is partly blocked (sometimes by a tiny salivary stone, called a sialolith) rather than torn. Saliva backs up inside the duct and balloons it outwards. This type does have a thin layer of duct lining cells, making it a true cyst.
Many people have no memory of any specific injury, which is normal, the trauma can be minor enough to go unnoticed.
How does it develop?
Think of a minor salivary gland as a tiny grape with a fine straw (the duct) that carries saliva into the mouth. If that straw is snapped or pinched, saliva still keeps being made, it just has nowhere to go. The escaped saliva collects under the lining of the mouth and pushes the surface upwards into a soft, fluid-filled dome.
The body recognises the spilled mucus as something that does not belong and sends in cleanup cells (macrophages) to mop it up. Over time, a wall of granulation tissue forms around the pool of saliva. As long as the gland keeps producing saliva and the duct stays damaged, the bubble keeps refilling. That is why mucoceles often burst, deflate and then come back again days or weeks later.
What might you notice?
What it looks like
A mucocele usually appears as a smooth, rounded, dome-shaped swelling, anywhere from a few millimetres up to a couple of centimetres across. When the pool of saliva sits close to the surface, the lump often takes on a soft bluish or translucent hue, a bit like a tiny water blister. Deeper mucoceles may look the same colour as the surrounding pink mucosa.
Many people first notice the lump after waking, after a meal, or after biting their lip. It might appear suddenly and reach its full size within a day or two.
What it feels like
Mucoceles are typically painless. They feel soft, fluctuant (squishy and fluid-filled) when gently pressed, although some are firmer. Larger ones can feel awkward when speaking or chewing because the tongue and teeth keep bumping into them. Some lesions burst on their own, releasing a thick, clear, sticky fluid, and then quietly refill over the following days.
A particular variant called a superficial mucocele sits very close to the surface and looks like a tense little blister, often on the soft palate or back of the cheek. These pop easily and leave a shallow ulcer that heals within a few days, but they can keep recurring in the same spot.
What an X-ray might show
A standard mucocele is a soft-tissue lesion and does not show up on dental X-rays. Imaging is usually only needed for ranulas (especially the plunging type) or to look for an underlying salivary stone. In those situations, ultrasound, CT or MRI scans may be used to map the lesion before treatment.
What happens at the dentist?
At ArtSmiles, most mucoceles can be diagnosed by a careful clinical examination. Your dentist will ask about how long the lump has been there, whether it has come and gone, and whether you remember any injury. They will then look at the lump in good light and gently feel it to assess size, softness and depth.
If the diagnosis is straightforward and the lesion is small, simple removal is often the next step. Because other lesions, including some salivary gland tumours, can mimic a mucocele, any tissue that is removed should be sent for microscopic examination to confirm what it is. This is especially important for any lump on the upper lip, hard palate or floor of the mouth, where a salivary gland tumour is more of a concern.
For a swelling under the tongue or in the floor of the mouth, your dentist may recommend referral to an oral and maxillofacial surgeon. Imaging may be requested to see how deep the lesion goes, particularly if a plunging ranula is suspected.
Is this serious?
🟢 Usually harmless. Mucoceles are benign, non-cancerous lesions. They will not spread or turn into anything sinister. A small mucocele can sometimes burst and heal on its own without treatment.
That said, they are often persistent, and many will keep refilling until the underlying damaged gland is dealt with. Larger ranulas in the floor of the mouth can interfere with speech, chewing and swallowing, and a plunging ranula can extend into the neck, so these warrant timely care.
The main reason to have any persistent lump checked is that other, more serious conditions can occasionally look like a mucocele. A professional examination is the safest way to be sure.
If you've noticed any of these signs for more than two weeks, it's worth booking an assessment.
Could it be something else?
Several other lesions can produce a similar soft, bluish or dome-shaped swelling. Your dentist will work through these possibilities during the examination.
Salivary duct cyst (mucus retention cyst / sialocyst), looks almost identical clinically, but is a true epithelium-lined cyst. It tends to appear in older adults and is differentiated under the microscope after excision.
Salivary gland tumour (such as a low-grade mucoepidermoid carcinoma or pleomorphic adenoma), can present as a slow-growing lump, especially on the upper lip or palate. Tumours usually feel firmer, do not fluctuate, and the diagnosis is confirmed by biopsy.
Lipoma, a soft fatty lump that can also feel squishy. Lipomas are usually yellow-tinted rather than blue, do not change in size suddenly, and feel smoother and more uniform.
Fibroma (traumatic fibroma), a firm, pink lump caused by chronic biting. Unlike a mucocele, a fibroma is solid (not fluid-filled) and does not change in size or burst.
Haemangioma or vascular malformation, bluish or purplish lesions that blanch (turn pale) when pressed because they are full of blood; mucoceles do not blanch.
Lymphangioma, a soft swelling caused by abnormal lymphatic vessels, usually present from a young age and often with a pebbly surface.
Venous varix, a small, soft, bluish dilated vein, more common in older adults and typically found under the tongue.
Dermoid cyst, a developmental cyst of the floor of the mouth that sits in the midline and feels doughy rather than fluctuant; helps distinguish it from a ranula, which is usually off to one side.
Lymphoepithelial cyst, a small, firm, yellowish nodule on the floor of the mouth or underside of the tongue; firmer and more clearly defined than a mucocele.
Abscess of the floor of the mouth, painful, red and warm, often with associated infection signs, unlike the painless mucocele.
Eruption cyst or gingival cyst, a bluish swelling over an erupting tooth or on the gum; the location and association with a tooth distinguish them.
Mucous membrane pemphigoid or other vesiculobullous disease, can look similar to multiple superficial mucoceles. A biopsy with special staining helps tell them apart.
How is it treated?
A few small mucoceles will rupture and heal on their own, particularly the very superficial ones. However, most lesions are persistent and tend to keep refilling, so professional treatment is usually recommended.
What you can do at home:
Avoid biting, sucking or playing with the lump, this only keeps the irritation going
Have any sharp tooth edges, broken fillings or rough denture surfaces smoothed by your dentist
Try not to chew on pens, lips or other objects out of habit
Professional treatment options that your dentist or oral surgeon may discuss include:
Surgical excision, the most common approach. The mucocele is removed under local anaesthetic, along with the small feeding salivary glands underneath. Removing the associated minor salivary glands is the key to preventing the lesion from coming back. The procedure is usually a short visit and the area heals over a couple of weeks.
Marsupialisation, used mainly for ranulas (mucoceles in the floor of the mouth). The roof of the cyst is opened and the edges are stitched back so the cavity drains and gradually flattens out. This can work well for small, superficial ranulas, but larger or deep ranulas often need removal of the underlying sublingual gland to stop them recurring.
Cryosurgery (freezing), sometimes used as an alternative to traditional excision for selected lesions.
Laser excision or vaporisation, another alternative technique for accessible lesions.
Referral to an oral and maxillofacial surgeon, recommended for ranulas, plunging ranulas (where the swelling extends into the neck), or any lesion where a salivary tumour is a possibility.
Whatever method is used, the removed tissue should always be sent for microscopic examination to confirm the diagnosis.
What's the long-term outlook?
The outlook for a typical mucocele is excellent. Once the lesion and its feeding salivary glands have been removed, the area heals well and most patients do not see any recurrence.
The main reason a mucocele comes back is that the original damaged minor salivary gland was not fully removed, so saliva continues to leak into the same spot. Mucoceles on the underside of the tongue (from the deeper Blandin–Nuhn glands) and ranulas in the floor of the mouth tend to have higher recurrence rates because of the more complex anatomy in those areas.
For superficial mucoceles, no treatment is usually needed because they rupture spontaneously and are short-lived, although they can recur in the same area over time.
The key takeaways are reassuring: mucoceles are benign, treatment is straightforward, and most people experience no long-term issues once the lesion is properly managed.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
The cover image above is an AI-generated illustration based on the most common visible features of this condition described in clinical pathology references. It is not a photograph of a real case and should not be used to diagnose or rule out the condition in your own situation. If you are concerned about something you have noticed, please book an assessment with a registered dental practitioner.
References
Regezi, J. A., Sciubba, J. J., & Jordan, R. C. K. (2017). Oral pathology: Clinical pathologic correlations (7th ed.). Elsevier. Chapter 8, Salivary Gland Diseases (Mucus Extravasation Phenomenon and Mucus Retention Cyst), pp. 185–189.
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2023). Oral and maxillofacial pathology (5th ed.). Elsevier. Chapter 11, Salivary Gland Pathology (Mucocele, Ranula and Salivary Duct Cyst), pp. 460–465.
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 18, Neoplastic and Non-neoplastic Diseases of Salivary Glands (Mucoceles and Cysts), pp. 292–294.
Laskaris, G. Color atlas of oral diseases. Chapter 14, Soft-Tissue Cysts (Mucocele and Ranula), pp. 108–109.