Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker , Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | Sublingual mucocele; plunging or cervical ranula (when it extends into the neck) |
How urgent? | 🟡 Worth assessing, usually painless but can grow large enough to interfere with speech and swallowing; surgical treatment is often needed |
Common or rare? | Uncommon overall, but the most common kind of mucocele in the floor of the mouth |
Who it affects | Most often children and young adults, with no strong sex predilection |
Who treats it | General dentist for assessment, with referral to an oral and maxillofacial surgeon for definitive treatment |
Based on | Cawson, Neville, Laskaris |
What is it?
A ranula is a soft, fluid-filled swelling in the floor of the mouth that develops when saliva escapes from the sublingual salivary gland (the saliva-producing gland that sits under your tongue) into the surrounding tissues. It is a special type of mucocele (a soft swelling that forms when saliva leaks or becomes trapped under the lining of the mouth), distinguished from ordinary mucoceles of the lip mainly by its location and its tendency to grow much larger. The name comes from the Latin "rana", meaning frog, because the swelling can resemble a frog's translucent underbelly. When the spilled saliva pushes through the floor of the mouth and tracks down into the neck, the lesion is called a plunging ranula or cervical ranula.
Who tends to get it?
Dentists typically see:
Children and young adults are most often affected, although a ranula can occur at any age.
No strong difference between males and females.
A previous knock or injury in the floor of the mouth is sometimes recognised, but in many cases there is no obvious trigger.
Patients with previous oral surgery in the floor of the mouth are at slightly higher risk.
People with anatomical variations in the way the sublingual gland drains saliva may be slightly more prone to develop a ranula.
What causes it?
Two main mechanisms produce a ranula:
Damage to the duct of the sublingual gland (the small tube that normally carries saliva into the mouth) tears, saliva leaks out, and the surrounding tissue forms a layer of squashed, scar-like connective tissue around it. Most ranulas are this kind of extravasation mucocele (a swelling caused by saliva leaking out of the duct into the surrounding tissue).
Less commonly, partial obstruction of one of the small ducts of the sublingual gland, saliva builds up inside a stretched duct, forming a true retention cyst (a closed sac of saliva with its own thin inner cell lining).
The sublingual gland is particularly prone to forming a ranula because it produces a steady flow of thick, mucus-rich saliva even between meals. Once a duct is damaged or obstructed, the saliva keeps coming, and the swelling enlarges until pressure equalises or the saliva escapes elsewhere.
How does it develop?
The classic ranula starts as a small, soft swelling under the tongue. Over weeks or months, more saliva accumulates and the swelling enlarges, often visibly lifting the tongue. The thin lining of the mouth (called the mucosa) stretches over the swelling, and the thick saliva inside (known as mucin, the thick protein in saliva) gives the lesion its translucent, bluish look. The body's response surrounds the spilled saliva with a layer of squashed, scar-like tissue, but without a proper inner cell lining in most cases.
In the plunging variant, the saliva tracks downward through or around the mylohyoid muscle (a sheet of muscle that forms the floor of the mouth) and produces a soft swelling in the neck. Sometimes the part inside the mouth is small or not visible at all, and the person comes in with what looks like an isolated swelling in the neck.
What might you notice?
What it looks like
The classic appearance is well described:
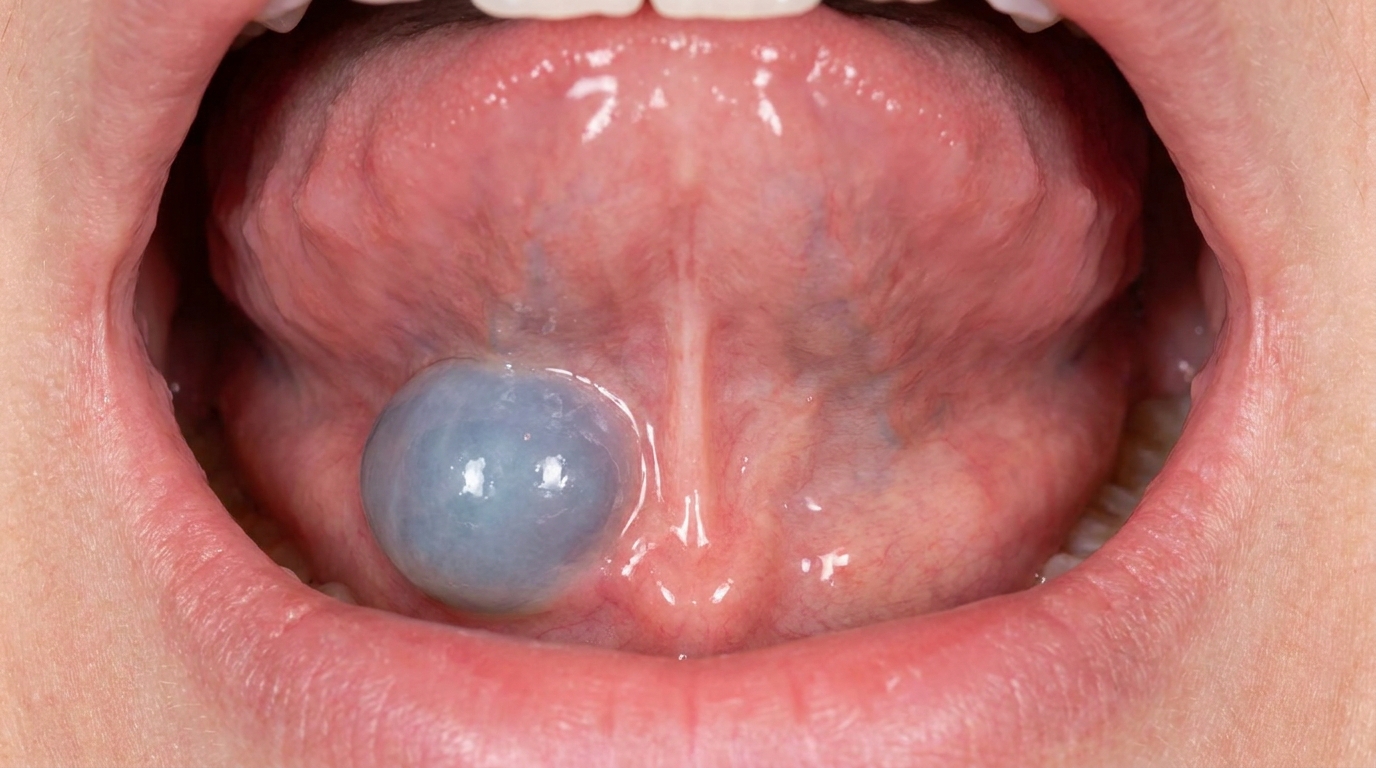
A soft, dome-shaped swelling in the floor of the mouth, usually lateral to the midline (one side or the other rather than directly in the centre).
Bluish or translucent colour, often described as pale blue through the thin overlying mucosa.
Fluctuant to touch, it feels like a soft, fluid-filled balloon when pressed.
Lifts the tongue when large.
Size varies from 1-2 cm in early lesions to several centimetres in long-standing cases.
A plunging ranula may show a soft swelling in the neck, with or without a swelling in the mouth.
What it feels like
Most ranulas are painless, particularly in the early stages. As they enlarge, symptoms may include:
A fullness or pressure under the tongue.
Difficulty speaking or eating, particularly when the lesion is large.
An obvious bump noticed by the patient with the tongue.
Periodic rupture and re-formation, the lesion can leak its contents into the mouth, partially deflate, and then refill over days to weeks.
Discomfort or visible swelling in the neck if the ranula has plunged.
What an X-ray might show
Imaging is more helpful for ranulas than X-rays alone:
Plain X-rays show only the soft tissue outline and are rarely diagnostic.
Ultrasound is widely used and can show the fluid-filled cavity and its relation to the sublingual gland.
CT or MRI scans are particularly useful for plunging ranulas, where the extension into the neck and the relationship to the mylohyoid muscle need to be mapped out.
Sialography (a special X-ray of the salivary ducts using a contrast dye) is occasionally used but is rarely needed for diagnosis.
What happens at the dentist?
A ranula is most often noticed by the patient or picked up at a routine dental check-up and clean at ArtSmiles. The dentist will typically:
Examine the floor of the mouth with the patient's tongue lifted, noting the size, colour, location and consistency of the swelling.
Take a careful history about how long the swelling has been present, whether it has changed size, whether it has ever ruptured, and any past trauma or surgery in the area.
Distinguish a ranula from other floor-of-mouth swellings by clinical examination.
Refer to an oral and maxillofacial surgeon (a specialist surgeon for the mouth, jaws and face) for further imaging and treatment, particularly for larger or plunging ranulas.
Reassure that the lesion is not cancer and that effective treatment is available.
Is this serious?
🟡 A ranula is benign and not cancerous. However, it tends to grow over time, can interfere with speech, swallowing and tongue movement, and can be cosmetically obvious. Plunging ranulas can produce a noticeable neck swelling and may be confused with other neck masses if the intraoral component is small. With timely treatment, the outlook is very good.
If you have noticed a soft, bluish swelling in the floor of your mouth that has been present for more than a few weeks, particularly if it lifts your tongue or interferes with speech, it is worth booking an assessment so the diagnosis can be confirmed and the right treatment planned.
Could it be something else?
Several conditions can produce a swelling in the floor of the mouth. The main look-alike conditions are:
Dermoid cyst, a developmental cyst, often present from birth, that appears as a swelling in the middle of the floor of the mouth. Set apart from a ranula by its central position, it usually feels firmer and is not as bluish.
Lymphoepithelial cyst, a small, harmless cyst that arises from immune-system tissue, seen as a well-defined yellow-white lump, often in the floor of the mouth or under the tongue.
Sublingual abscess, a pocket of infection under the tongue, felt as a tender, hot, red swelling, often linked to a dental infection or a salivary gland stone.
Salivary gland tumour, a growth in a saliva-producing gland, felt as a firmer, persistent lump that does not feel fluid-filled and does not rupture; a biopsy (a small tissue sample sent to the lab) is essential.
Haemangioma or vascular malformation, a benign growth or unusual collection of blood vessels, seen as a long-standing reddish-blue lesion present for years that behaves differently from a ranula when pressed.
Lymphangioma (cystic hygroma), a soft, harmless growth made of dilated lymph channels, felt as a swelling with multiple small fluid-filled spaces, often present from infancy, that can affect the floor of the mouth or neck.
Sialolithiasis, a stone that forms inside the duct of a salivary gland, most often the gland under the jaw or under the tongue. It can cause swelling, usually with pain around meal times.
How is it treated?
Treatment is essentially surgical, with the specific approach depending on the size, location and whether the ranula is plunging.
At-home measures:
Avoid biting or pressing the swelling.
Eat softer foods if the lesion makes eating uncomfortable.
Stay well hydrated, although hydration does not cure the lesion, it supports general saliva and oral health.
Maintain good oral hygiene to keep the surrounding mouth as healthy as possible while awaiting surgery.
Professional steps your specialist may consider:
Marsupialisation, for smaller, superficial ranulas, the roof of the cyst is opened into the mouth and the edges of the cyst lining are stitched to the surrounding mouth lining. This converts the closed cavity into an open pouch and allows saliva to drain into the mouth, avoiding recurrence in many cases.
Removal of the feeding sublingual gland, for larger ranulas, ranulas that come back after earlier surgery, or plunging ranulas, the source sublingual gland on the affected side is removed. This is the most reliable option for preventing recurrence.
Combined approach, marsupialisation plus partial gland excision is sometimes used.
Imaging-guided drainage is occasionally used as a temporary measure but rarely cures the lesion.
Histopathological examination of any tissue removed at surgery (a pathologist examines it under a microscope), to confirm the diagnosis and rule out a true salivary duct cyst or other condition.
Long-term follow-up at 3-12 month intervals to confirm there is no recurrence.
Children and young adults can feel apprehensive about a procedure inside the mouth or neck, so calm, clear explanation of what the lesion is, what the surgery achieves and how recovery typically goes is part of the care we offer, in line with our clinical philosophy.
What's the long-term outlook?
The outlook is generally very good. Marsupialisation alone has a moderate recurrence rate, particularly for larger lesions. Removal of the feeding sublingual gland, with or without marsupialisation, is the most reliable way to prevent recurrence and is the standard approach for most ranulas, particularly plunging ranulas. Most patients return to normal function within a few weeks of surgery and have no long-term complications. The other salivary glands continue to provide normal saliva flow, so removing one sublingual gland generally has no lasting impact on dryness or function.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
The cover image above is an AI-generated illustration based on the most common visible features of this condition described in clinical pathology references. It is not a photograph of a real case and should not be used to diagnose or rule out the condition in your own situation. If you are concerned about something you have noticed, please book an assessment with a registered dental practitioner.
References
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2023). Oral and maxillofacial pathology (5th ed.). Elsevier. Chapter 11, Salivary Gland Pathology: Ranula, with detailed clinical features and the plunging ranula variant, pp. 463 to 464.
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 18, Neoplastic and Non-Neoplastic Diseases of Salivary Glands: Ranula, with marsupialisation as the preferred initial treatment, p. 293.
Laskaris, G. Pocket atlas of oral diseases. Thieme. Chapter 14, Soft-Tissue Cysts: Ranula, p. 108.