Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker , Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | Chronic apical periodontitis, dental granuloma, apical granuloma |
How urgent? | 🟡 Worth a check-up, usually painless, but it signals an infected, non-vital (with a dead nerve) tooth that needs treatment to stop it growing or flaring up |
Common or rare? | Very common, one of the most frequently encountered findings on dental X-rays |
Who it affects | Adults of any age; uncommon in the first decade of life |
Who treats it | General dentist, often in partnership with an endodontist (root canal specialist, a dentist who specialises in this treatment) for complex cases |
Based on | Regezi, Neville, Cawson |
What is it?
A periapical (at the tip of a tooth root) granuloma is a small ball of inflamed healing tissue that forms at the very tip of a tooth root when the nerve inside that tooth has died. Despite the scary-sounding name, it is not a tumour and not a true "granuloma" in the way doctors use that word for diseases like tuberculosis. It is simply your body's long-term reaction to a dead, infected tooth nerve, walled off in a neat little package against the jawbone.
In most people, it sits quietly at the root tip and is only spotted on a routine dental X-ray as a small dark circle.
Who tends to get it?
Periapical granulomas are extremely common, they make up the majority of all small dark spots dentists see at the apex of teeth on radiographs. They are far less common in young children, partly because deep decay and trauma severe enough to kill a tooth nerve take time to develop. From the teens onwards, they can occur at any age.
There is no strong gender or ethnic pattern. The condition follows the tooth, not the person, any non-vital tooth in any patient can develop one.
What causes it?
A periapical granuloma is almost always the late stage of an infected tooth. The most common pathway looks like this:
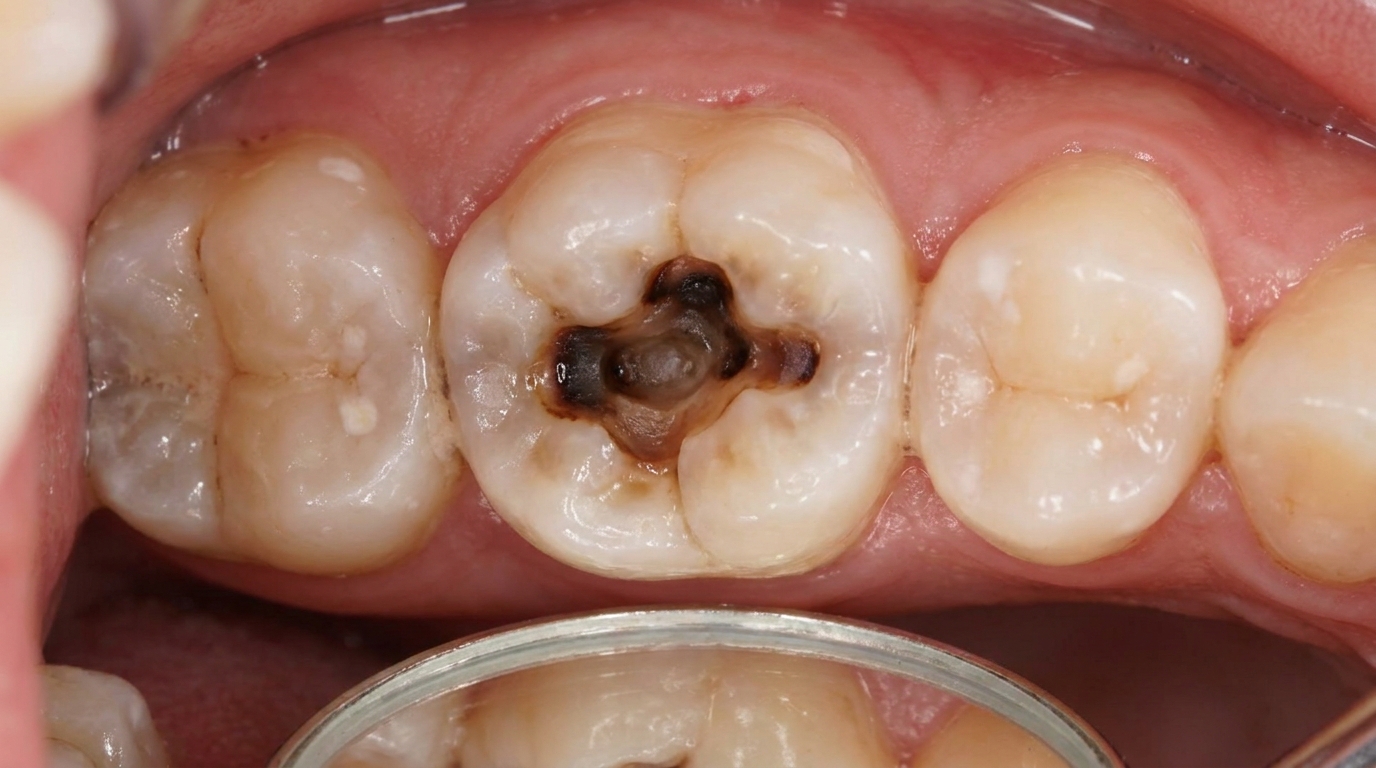
Deep tooth decay that reaches the nerve chamber
Cracks or fractures that let bacteria into the pulp
Trauma, a blow to a front tooth that quietly kills the nerve, sometimes years before the granuloma appears
Failed previous treatment, a root-filled tooth where bacteria have re-colonised the canal
Very deep fillings or repeated dental work that has stressed the pulp over time
Less often, irritation from instruments, antiseptics or filling materials pushed beyond the root tip during root canal treatment can keep the inflammation going.
How does it develop?
When the nerve inside a tooth dies, bacteria and their toxins leak out through the tiny opening at the root tip into the surrounding bone. Your body responds the same way it would to a stubborn splinter it cannot quite remove, it sends in a steady stream of immune cells (lymphocytes, plasma cells and macrophages) to wall the irritation off.
Over weeks and months, these cells, along with new blood vessels and fibrous tissue, form a soft pink ball of granulation tissue (the soft pink healing tissue your body builds around an irritation) around the root tip. To make room, the body gently dissolves a small pocket of jawbone, which is why it shows up as a dark circle on the X-ray. As long as the bacteria keep dripping out of the root, the granuloma stays, it cannot heal on its own because the source of irritation is sealed inside the tooth.
Think of it as a bin liner the body has tied around a leaking pipe: the leak has not been fixed, but the mess has been contained.
What might you notice?
What it looks like
Usually, nothing at all from the outside. The tooth itself may look perfectly normal, although in some cases the crown can appear slightly darker or greyer than its neighbours, especially if the nerve died after an old knock to the face. There is rarely any visible swelling unless the lesion flares up acutely.
What it feels like
Most periapical granulomas are completely silent, no pain, no sensitivity, no aching. The tooth typically does not respond to hot, cold or electric pulp tests because the nerve inside is dead. Some people notice the tooth feels slightly different to bite on, or mildly tender if pressed.
If the lesion goes through an acute flare-up (sometimes called a "phoenix abscess"), pain can come on quickly, throbbing, well-localised to one tooth, and worse on biting.
What an X-ray might show
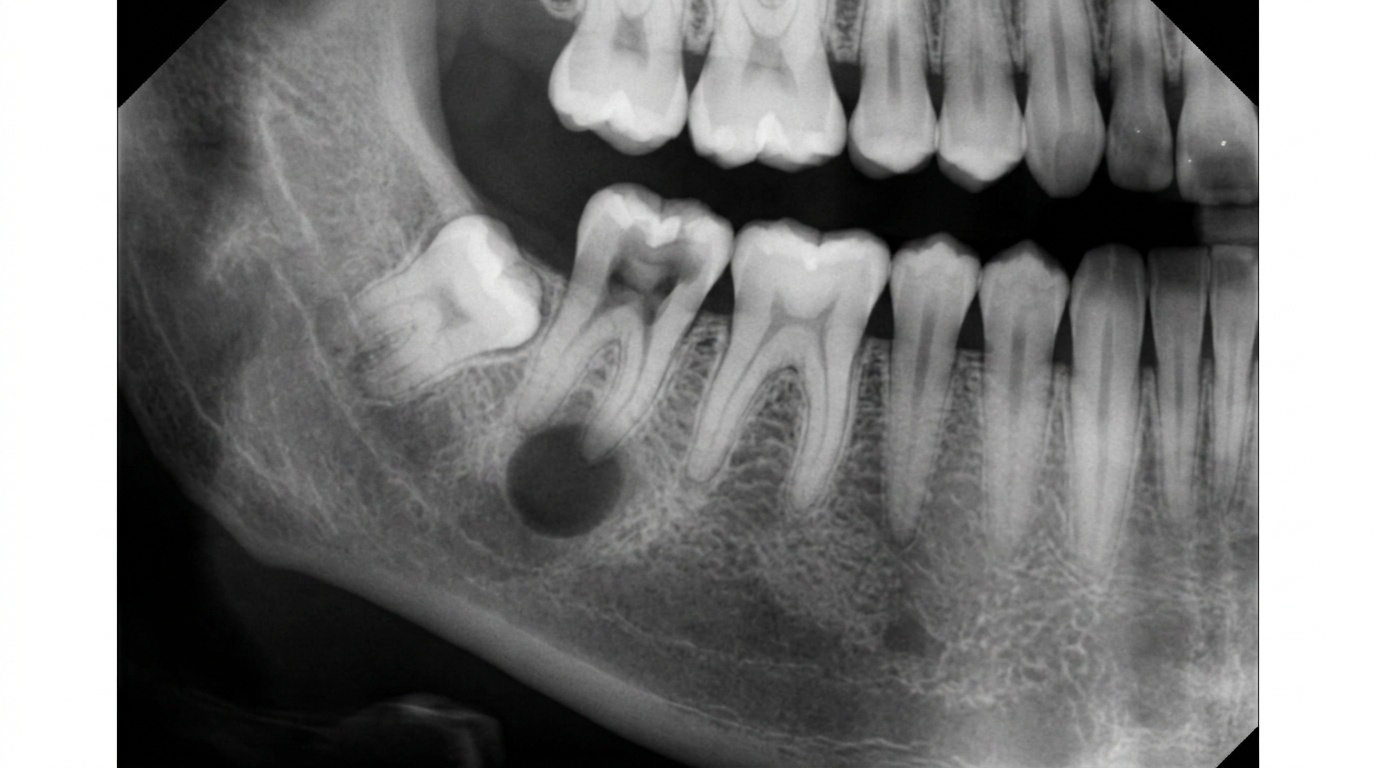
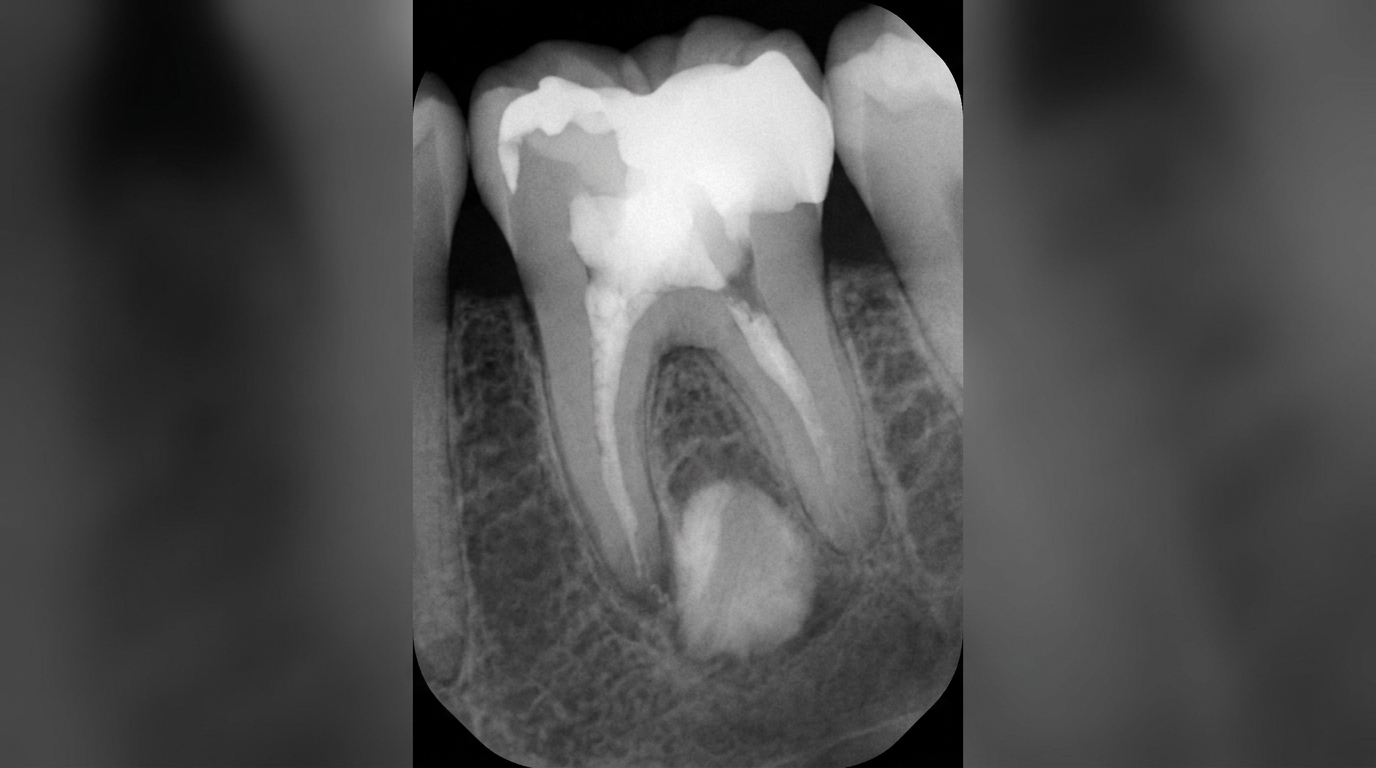
This is usually how the condition is found. On a dental radiograph, your dentist may see:
A small, round dark area at the very tip of the root
Loss of the thin white line (the lamina dura) that normally outlines the root
A lesion ranging from barely visible to over 2 cm across
Sometimes mild shortening of the root tip from gentle resorption (gradual dissolving of a tooth root or surrounding bone)
Importantly, on an X-ray a periapical granuloma cannot be reliably distinguished from a periapical (radicular) cyst. Even with newer imaging like cone-beam CT (a 3D dental X-ray), the two often look identical, and a definitive answer only comes if the tissue is sent for examination after surgery.
What happens at the dentist?
If your dentist at ArtSmiles spots a small radiolucency (a dark area on an X-ray, suggesting bone loss or a cavity) at a root tip, the next steps are usually straightforward:
Vitality testing, gentle hot, cold or electric pulp tests on the suspect tooth and its neighbours to confirm the nerve is dead. A non-vital tooth in the right place strongly supports the diagnosis.
Percussion and palpation, tapping the tooth and pressing the gum over the root to check for tenderness.
Periodontal probing, to rule out gum disease as the source of the dark spot.
Targeted radiographs or, in selected cases, a small-volume cone-beam CT scan to map the lesion in three dimensions.
Biopsy, usually only needed if the lesion is unusually large, has unclear borders, fails to heal after good root canal treatment, or sits beside a vital tooth (which would point to a different diagnosis).
Specialist referral, your dentist may suggest seeing an endodontist for complex root canal anatomy, or an oral surgeon if minor surgery is required.
Because around one in three to one in two periapical lesions turn out to be cysts rather than granulomas under the microscope, all surgically removed periapical tissue should be sent for histopathology (microscope examination of the removed tissue) to confirm the diagnosis.
Is this serious?
🟡 Worth treating, but rarely an emergency.
Left alone, a periapical granuloma will not heal on its own because the bacterial source inside the tooth keeps it active. It can:
Slowly enlarge and resorb more bone
Transform into a periapical cyst, which tends to grow larger over time
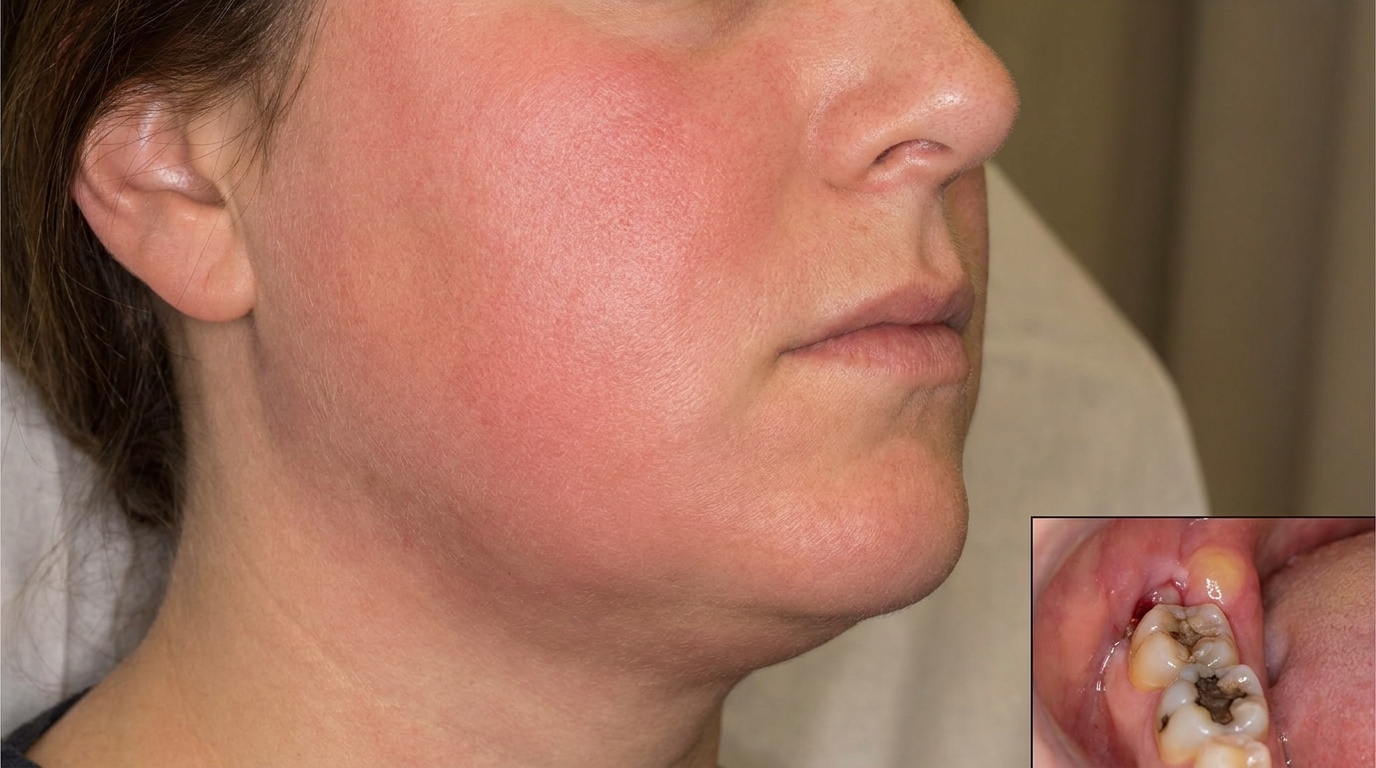
Flare up acutely into a periapical abscess, with pain, swelling and sometimes facial cellulitis
Very rarely, in untreated severe flare-ups, contribute to spreading infections such as Ludwig's angina or cavernous sinus thrombosis, these are the dangerous exceptions, not the rule
With timely treatment, the outlook is excellent. The lesion is essentially curable in the vast majority of cases.
If you've noticed any of these signs for more than two weeks, it's worth booking an assessment.
Could it be something else?
On an X-ray, a small dark circle at a root tip can have several explanations. Your dentist will work through these possibilities carefully, because treatment depends on getting the right answer.
Periapical (radicular) cyst, the next stage along from a granuloma; looks identical on a radiograph and is associated with the same non-vital tooth. Only microscopic examination of removed tissue can tell them apart with certainty.
Periapical abscess, a collection of pus rather than chronic inflammation; typically painful, with the tooth tender to touch and sometimes swelling of the gum or face. Borders on the X-ray tend to be hazy rather than crisp.
Periapical (fibrous) scar, a healed area filled with collagen instead of bone, usually after previous apical surgery; the tooth has often been root-treated and is symptom-free.
Periapical cemento-osseous dysplasia, typically seen at the apex of vital lower front teeth in middle-aged women; the tooth tests vital, which is the key clue.
Traumatic (simple) bone cyst, an empty cavity in the jaw, more common in younger patients and in the lower jaw; the adjacent tooth is vital.
Odontogenic keratocyst, a developmental cyst that can occasionally appear in a periapical position; teeth involved are usually vital, and the lesion may be larger or less rounded than expected.
Dentigerous cyst, forms around the crown of an unerupted tooth, so it is centred on the crown rather than the root tip.
Lateral periodontal cyst, sits along the side of a vital tooth root rather than at the apex, most often between the lower canine and premolar.
Nasopalatine duct (incisive canal) cyst, found between the roots of the upper central incisors; the teeth are vital and the cyst arises from non-tooth tissues in the midline.
Central giant cell granuloma, ameloblastoma or other odontogenic tumours, rare possibilities, usually larger and with features that look "off" for a simple granuloma; teeth are often vital.
Metastatic disease, lymphoma or myeloma, uncommon, but worth ruling out when a periapical lesion is associated with vital teeth, has ill-defined edges, or causes numbness of the lip.
How is it treated?
The goal of treatment is simple: remove the source of bacteria from the root canal so the body can mop up the inflammation and rebuild bone.
At home, you can help by:
Keeping up gentle, thorough brushing and flossing around the area
Avoiding chewing hard foods on a sensitive or recently treated tooth
Not delaying treatment for known deep decay or cracked teeth
Returning for recommended check-ups after any tooth trauma, even if the tooth still looks fine
At the dentist, treatment may include:
Root canal treatment (endodontic therapy), the most common option. The dentist or endodontist cleans, shapes, disinfects and seals the inside of the tooth. Most small periapical granulomas resolve quietly over the following months once the bacterial source is removed.
Endodontic retreatment, if a previously root-filled tooth still has a lesion, the existing filling may be carefully removed, the canals re-cleaned and re-sealed.
apicectomy (apical surgery, a minor procedure to trim the root tip and clear the lesion), a minor surgical procedure where the tip of the root is trimmed, the lesion curetted out and a small filling placed in the end of the canal. Often considered for larger lesions, lesions that fail to respond to retreatment, or teeth where conventional access is difficult.
Extraction with curettage (scraping the lesion out), if the tooth is not restorable, removing it together with the periapical tissue allows full healing. Any tissue removed is typically sent for laboratory examination.
Pain relief, short courses of simple anti-inflammatory medication may be recommended around treatment if needed. Antibiotics are not routinely used unless there is significant swelling, fever or spreading infection.
Follow-up X-rays at around 1 and 2 years (and sometimes earlier intervals) are important to confirm the lesion is shrinking and the bone is filling in.
What's the long-term outlook?
The outlook for a periapical granuloma is genuinely good. With well-performed root canal treatment, and a sound restoration on top of the tooth to keep bacteria out, the lesion typically shrinks gradually as new bone fills the space. Most cases resolve without any further intervention.
Failure is more often linked to gaps in treatment than to anything sinister: incomplete cleaning of complex canal anatomy, a leaky crown or filling that lets bacteria back in, or a tooth that was not really restorable to begin with. Where treatment does not work the first time, retreatment or apical surgery offers another strong chance of healing.
If the lesion has already converted to a periapical cyst, root canal treatment alone may not be enough and surgical removal is sometimes needed, but again, the prognosis remains favourable. Long-standing untreated lesions can cause more bone loss, more root resorption and a higher risk of acute flare-ups, which is the main reason your dentist will encourage you not to ignore that quiet little dark spot on the X-ray.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
The cover image above is an AI-generated illustration based on the most common visible features of this condition described in clinical pathology references. It is not a photograph of a real case and should not be used to diagnose or rule out the condition in your own situation. If you are concerned about something you have noticed, please book an assessment with a registered dental practitioner.
References
Regezi, J. A., Sciubba, J. J., & Jordan, R. C. K. (2017). Oral pathology: Clinical pathologic correlations (7th ed.). Elsevier. Chapter 10, Cysts of the Jaws and Neck (Periapical/Radicular Cyst), pp. 245 to 248; Chapter 13, Inflammatory Jaw Lesions (Pulpitis, Periapical Abscess, Periapical Granuloma), pp. 314 to 318.
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2023). Oral and maxillofacial pathology (5th ed.). Elsevier. Chapter 3, Pulpal and Periapical Disease (Periapical Granuloma / Chronic Apical Periodontitis; Periapical Cyst; Periapical Abscess), pp. 122 to 133.
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 4, Pulpitis, Apical Periodontitis, Resorption and Hypercementosis (Periapical Periodontitis; Acute and Chronic Apical Periodontitis), pp. 65 to 69.
Frequently asked questions
What is a periapical granuloma?
A periapical granuloma is a small mass of inflamed granulation tissue at the tip of a tooth root. It develops in response to a chronic, low-grade infection in the tooth's pulp tissue, usually from long-standing decay or trauma. It is benign and not cancer.
How is it different from a periapical cyst?
On X-ray they can look similar (both show a small dark area at the root tip), but microscopically a granuloma is inflamed soft tissue, while a periapical cyst has an epithelial lining and a fluid-filled cavity. A cyst tends to be larger. Definitive diagnosis is made on histopathology after removal.
Does a periapical granuloma cause pain?
Usually not. Most periapical granulomas are silent and only picked up on routine X-rays, although some give a vague ache or tenderness when biting. Pain typically develops only if the lesion becomes acutely infected and turns into an abscess.
How is it treated?
Treatment is aimed at the source tooth. Root canal treatment removes the infected pulp and allows the granuloma to heal as the body resolves the inflammation. If the tooth cannot be saved, extraction with curettage of the granulation tissue is the alternative. Healing is then confirmed on follow-up X-rays.