Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker, Principal Dentist, ArtSmiles Cosmetic Dentistry.
Some toothache wakes you at three in the morning. The tooth throbs, hot drinks make it worse, cold sometimes brings short relief, and lying down seems to amplify the pain. This pattern of severe, lingering, sometimes spontaneous tooth pain is the hallmark of irreversible pulpitis, inflammation of the tooth nerve that has gone past the point of recovery.
Quick summary
Also called | Acute pulpitis, pulpal nerve inflammation past the point of recovery |
How urgent? | 🔴 Urgent, severe lingering pain almost always needs same-day or next-day dental care, and the condition can progress to a dental abscess |
Common or rare? | Common, one of the most frequent reasons people present to a dentist with severe toothache |
Who it affects | Adults with deep cavities, large or repeated fillings, cracked teeth, dental trauma, or untreated reversible pulpitis |
Who treats it | General dentist, definitive treatment is either root canal therapy to keep the tooth or extraction with later replacement |
Based on | Neville, Cawson and Regezi |
What is it?
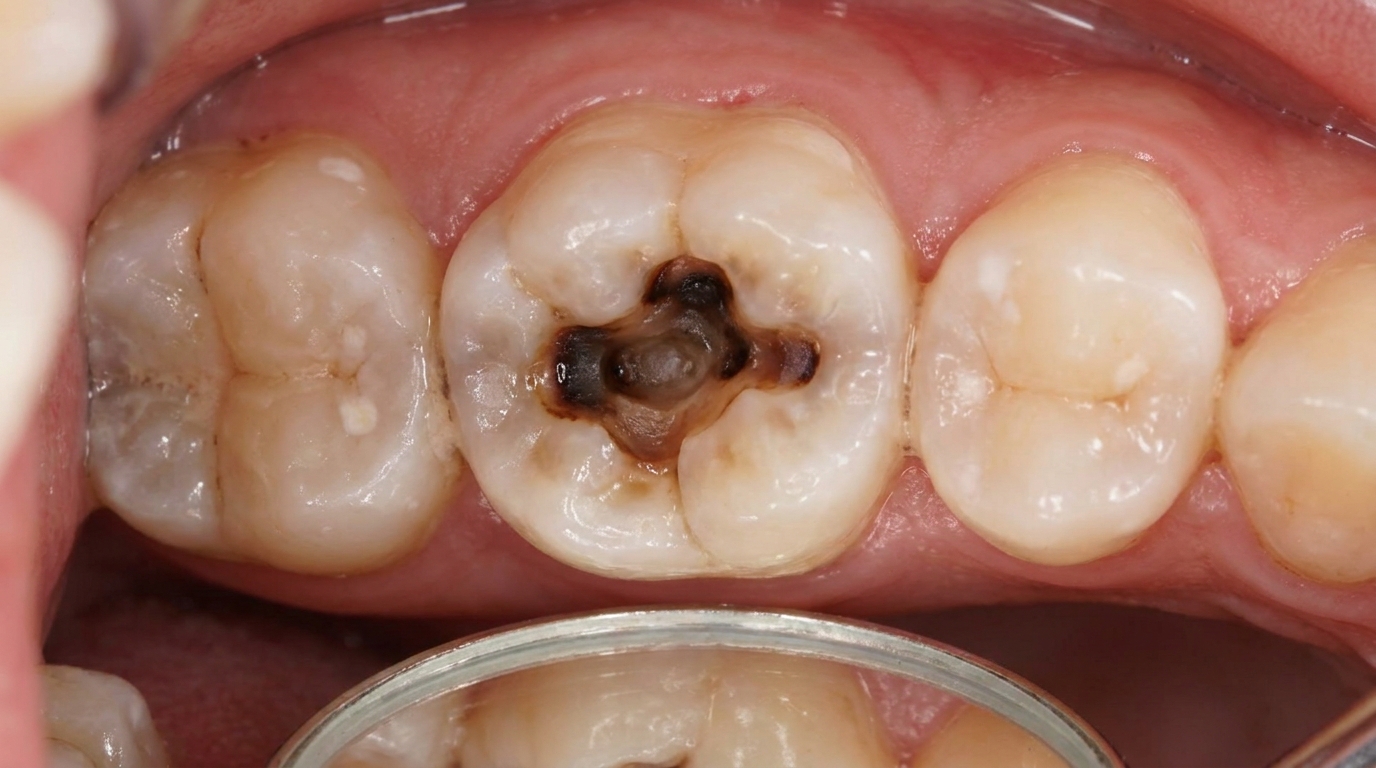
The pulp is the soft tissue at the centre of a tooth, nerve, blood vessels and connective tissue. Irreversible pulpitis means inflammation of the pulp that is too severe for the nerve to recover, even if the cause is removed. The tooth has effectively reached a point of no return for keeping the nerve alive.
Common features include:
Severe pain that lasts minutes to hours.
Spontaneous pain without any trigger.
Pain that lingers long after a cold or hot stimulus.
Pain in bed or when lying down.
Throbbing pulse-like pain in many cases.
Hot foods and drinks making it worse.
Cold sometimes giving brief relief in late stages (a worrying sign).
Pain that disturbs sleep and concentration.
Who tends to get it?
Irreversible pulpitis can affect anyone with:
A long-standing deep cavity.
A large filling or crown that has been disturbed by decay or fracture.
A cracked tooth with the crack reaching the pulp.
Repeated dental treatment on the same tooth.
Trauma to the tooth.
Untreated reversible pulpitis that has progressed.
It is one of the most common reasons people visit a dentist urgently.
What causes it?
The cause is deep inflammation of the pulp, usually from:
Bacterial invasion through a deep cavity.
Microleakage (tiny gaps that let bacteria seep in around a filling) around an old filling.
A crack allowing bacteria to reach the nerve.
Direct trauma that has fractured the tooth.
Repeated insults, multiple fillings on the same tooth.
Severe orthodontic forces in rare cases.
Iatrogenic (caused by dental treatment itself) exposure of the pulp during deep filling work.
Once the pulp's blood supply cannot keep up with the inflammation, the tissue starts to die and the inflammation becomes irreversible.
How does it develop?
The course is progressive:
The pulp becomes mildly inflamed (reversible pulpitis).
Without treatment, the inflammation worsens.
Pressure builds up inside the rigid pulp chamber, compressing blood vessels.
Pulp tissue begins to die.
Pain becomes severe, lingering and sometimes spontaneous.
As the pulp dies completely (called necrosis, the death of pulp tissue), pain may temporarily reduce.
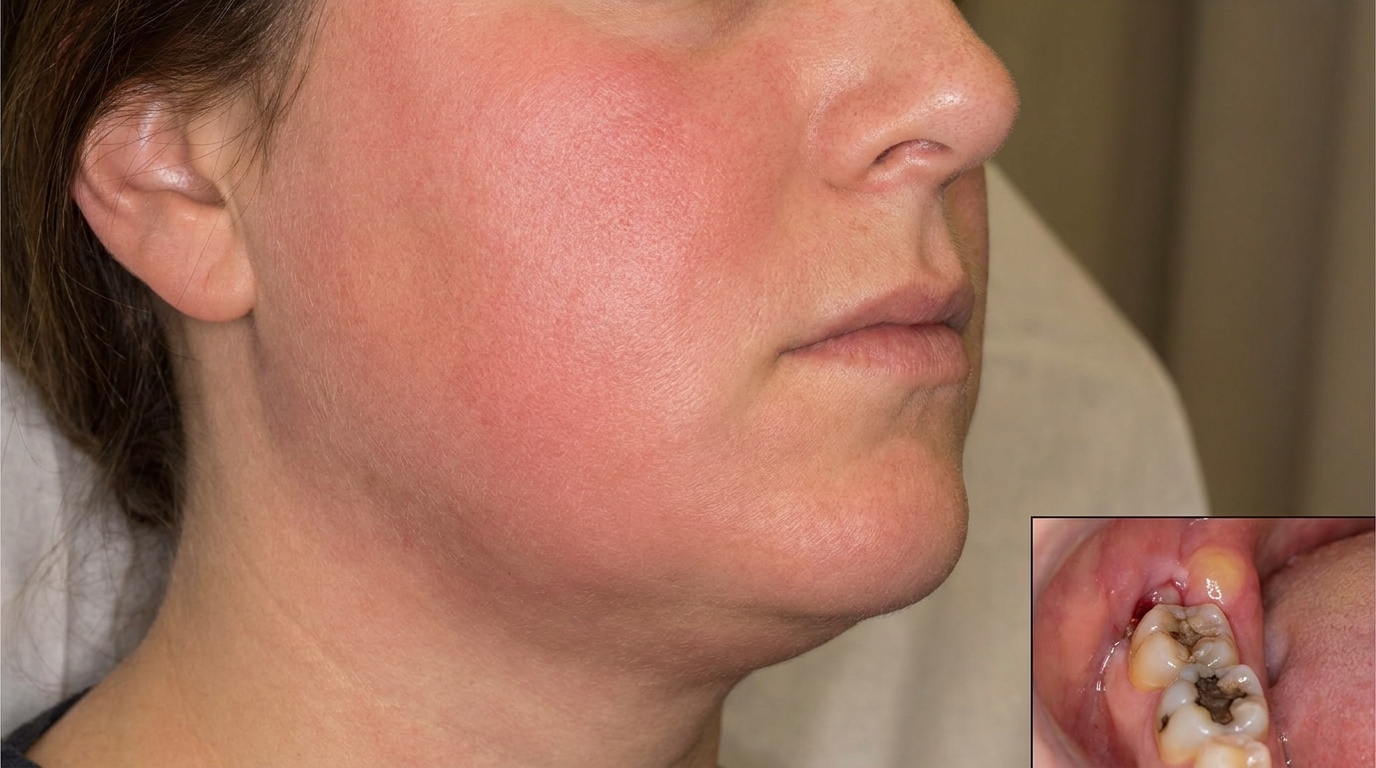
Bacteria spread beyond the root tip, producing periapical (around the root tip of the tooth) inflammation, abscess and possible facial swelling.
What might you notice?
Common features include:
Severe toothache, often the worst pain of the patient's life.
Difficulty identifying which tooth is affected, particularly with upper teeth.
Pain that lasts hours, not seconds.
Pain on lying down or bending over.
Spontaneous pain, without any trigger.
Disturbed sleep.
Pain often radiating to the ear, jaw or temple.
Hot food worsening the pain dramatically.
Cold giving brief relief in late-stage cases.
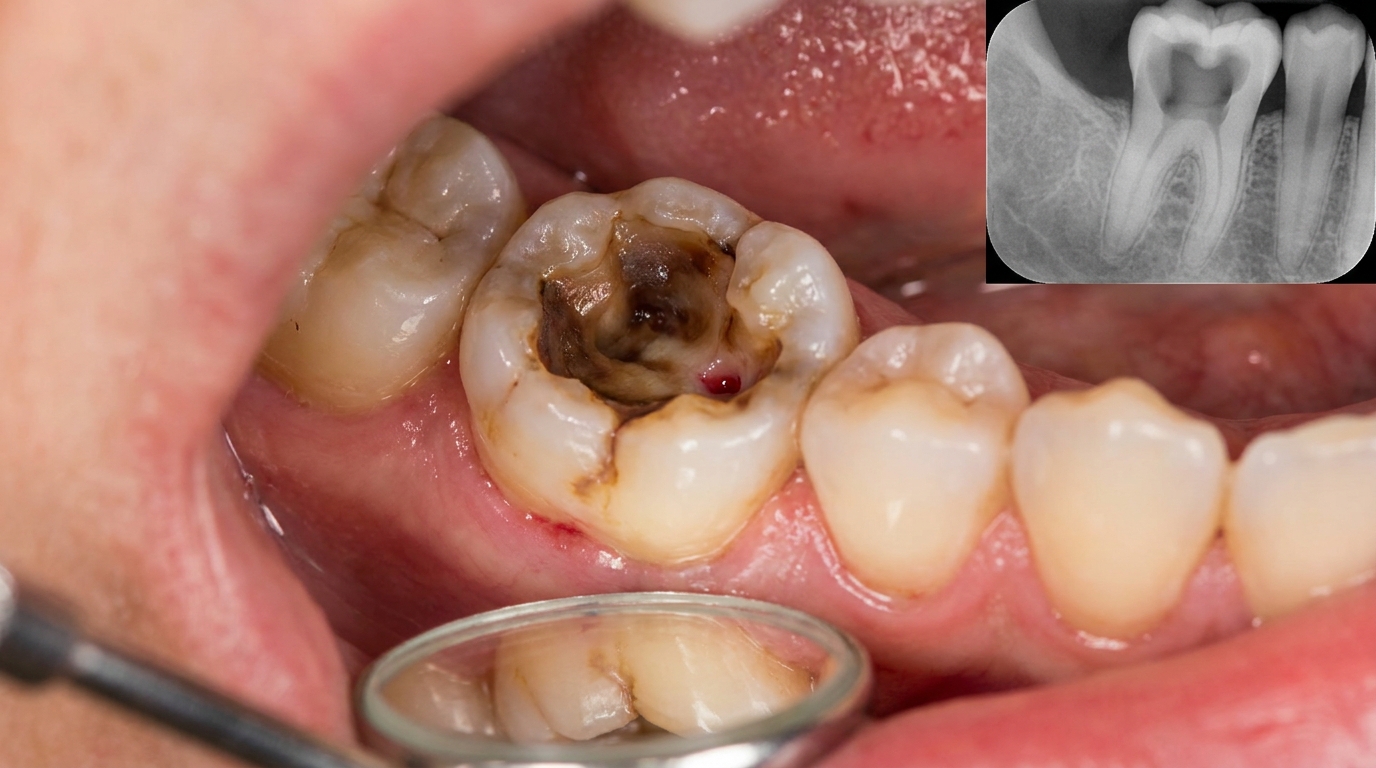
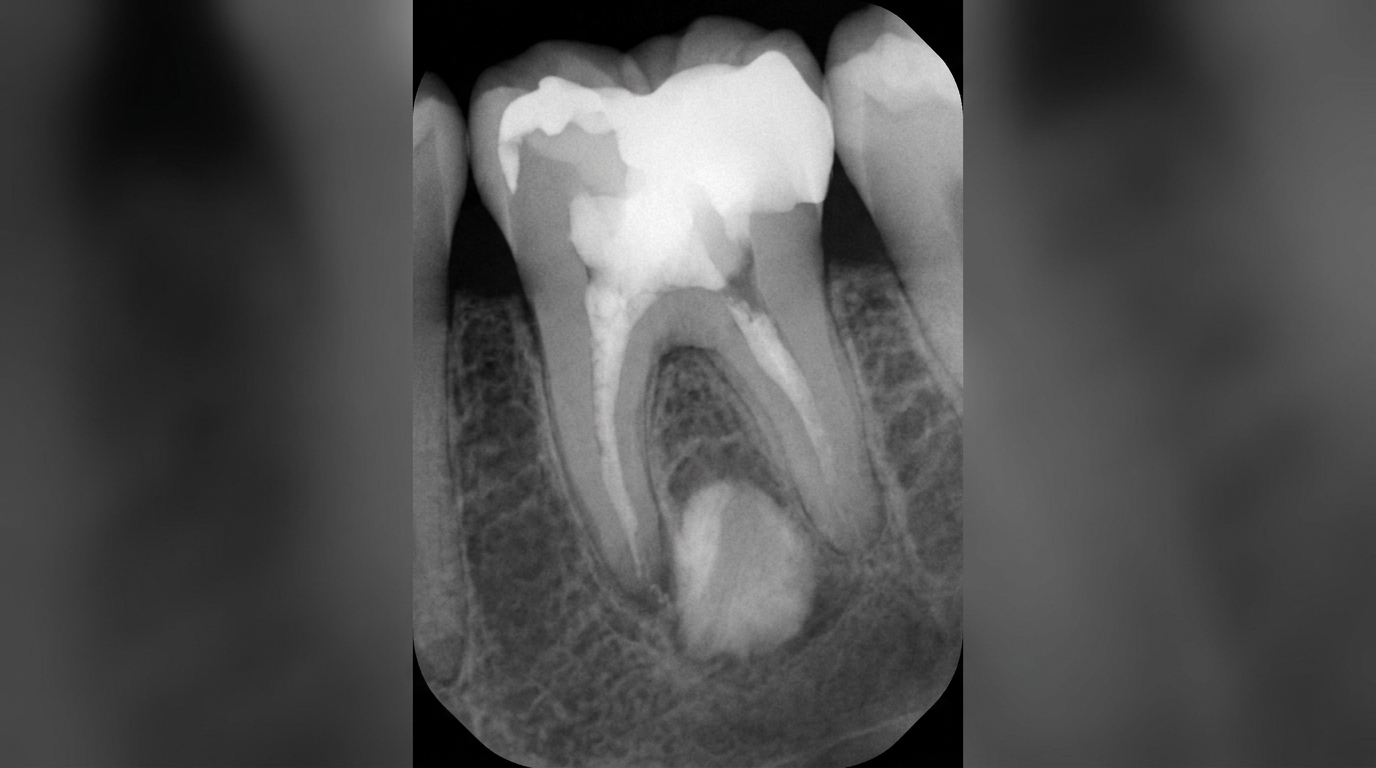
What an X-ray might show
X-rays cannot show inflammation of the pulp directly, but they are essential for understanding the tooth and surrounding bone. A periapical radiograph (close-up X-ray of one or two teeth) may show a deep cavity reaching the pulp chamber, an old filling close to the nerve, a fractured restoration or root, or early changes around the root tip that suggest the infection has started to spread beyond the pulp. Findings on the X-ray help decide whether root canal therapy or extraction is the better option.
What happens at the dentist?
When irreversible pulpitis is suspected at ArtSmiles, the visit usually involves:
A history conversation about the pattern of pain.
A clinical examination to identify the affected tooth.
Pulp testing, cold test, electric pulp test, to characterise the response.
Bite testing and percussion to assess any periapical involvement.
An X-ray to see decay, fillings, cracks and the periapical area.
A discussion of treatment options, root canal therapy vs extraction.
Immediate pain relief, local anaesthetic and starting treatment that day where possible.
Is this serious?
Irreversible pulpitis is dental-urgent. Reasons it deserves prompt care:
Severe pain affects sleep, eating, work and quality of life.
Untreated pulpitis progresses to abscess.
Abscess can produce facial swelling and, rarely, spread to deep neck spaces.
Earlier treatment is easier and more comfortable.
Could it be something else?
Conditions that can produce similar pain include:
Cracked tooth syndrome, sharp pain on bite-and-release rather than constant ache.
Reversible pulpitis, short-lived pain only with stimuli.
Sinus pain, pressure pain in upper back teeth, worse on bending.
Trigeminal neuralgia, sharp lightning pain rather than a throbbing ache.
Atypical odontalgia, chronic pain without clear dental cause.
Maxillary sinusitis, multiple upper teeth tender, with sinus symptoms.
TMJ disorder, muscle and joint pain rather than tooth pain.
A combination of clinical examination, pulp testing and X-rays sorts these out.
How is it treated?
Two definitive options:
Root canal therapy, removing the inflamed pulp, cleaning and shaping the root canals, and filling them. The tooth is then restored, often with a crown to protect it long-term. The tooth survives but is no longer alive.
Extraction, when the tooth cannot be saved, is heavily damaged, or the patient does not want root canal therapy. Replacement options include implant, bridge or denture.
In the short term:
Local anaesthetic for immediate pain relief.
Pulpotomy (removing the top portion of the inflamed pulp as a holding step) as a temporary measure if full root canal therapy cannot be done at the first visit.
Pain relief with paracetamol and ibuprofen.
Antibiotics are not routinely indicated, most cases respond to drainage and treatment.
Avoiding hot foods and drinks until treatment.
What's the long-term outlook?
The outlook depends on the option chosen:
Root canal therapy has high success rates (around 85 to 95% over many years), particularly when followed by a well-fitted crown.
Extraction removes the problem at the cost of the tooth; replacement options give back chewing function and appearance.
Untreated, pain eventually settles when the nerve dies fully, but a chronic infection often follows, with future flare-ups.
If you have severe lingering tooth pain, please book the next available appointment. We can usually offer immediate relief and a clear plan for definitive treatment.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
The cover image above is an AI-generated illustration based on the most common visible features of this condition described in clinical pathology references. It is not a photograph of a real case and should not be used to diagnose or rule out the condition in your own situation. If you are concerned about something you have noticed, please book an assessment with a registered dental practitioner.
References
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2016). Oral and maxillofacial pathology (4th ed., Ch. 3: Pulpal and Periapical Disease, Irreversible Pulpitis). Elsevier.
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed., Ch. 4: Pulpal Disease). Elsevier.
Regezi, J. A., Sciubba, J. J., & Jordan, R. C. K. (2017). Oral pathology: clinical pathologic correlations (7th ed., Ch. 3: Pulpal and Periapical Disease). Elsevier.
Frequently asked questions
What does irreversible pulpitis feel like?
Typical features are spontaneous, lingering, often throbbing tooth pain that gets worse when lying down. Hot drinks and food often trigger or intensify the pain, sometimes for many seconds or minutes after the stimulus is removed. The pain can be difficult to localise to a single tooth and may keep you awake at night.
Can irreversible pulpitis heal on its own?
No. Once the pulp inflammation has reached the irreversible stage, the inner nerve and blood supply cannot recover, even if the symptoms briefly ease. Definitive treatment is either root canal treatment, which removes the inflamed pulp and saves the tooth, or extraction.
Is irreversible pulpitis an emergency?
It is an urgent dental problem rather than a life-threatening emergency. Pain is often severe and disruptive, and the affected tooth tends to progress to a more serious infection (such as an apical abscess) if left untreated. Same-day or next-day dental care to start treatment is the usual recommendation.
Is root canal treatment painful?
Modern root canal treatment is typically done under local anaesthetic and most patients describe it as similar in comfort to a routine filling. Some tenderness over the next day or two is normal. The procedure relieves the original pulp pain that prompted treatment.