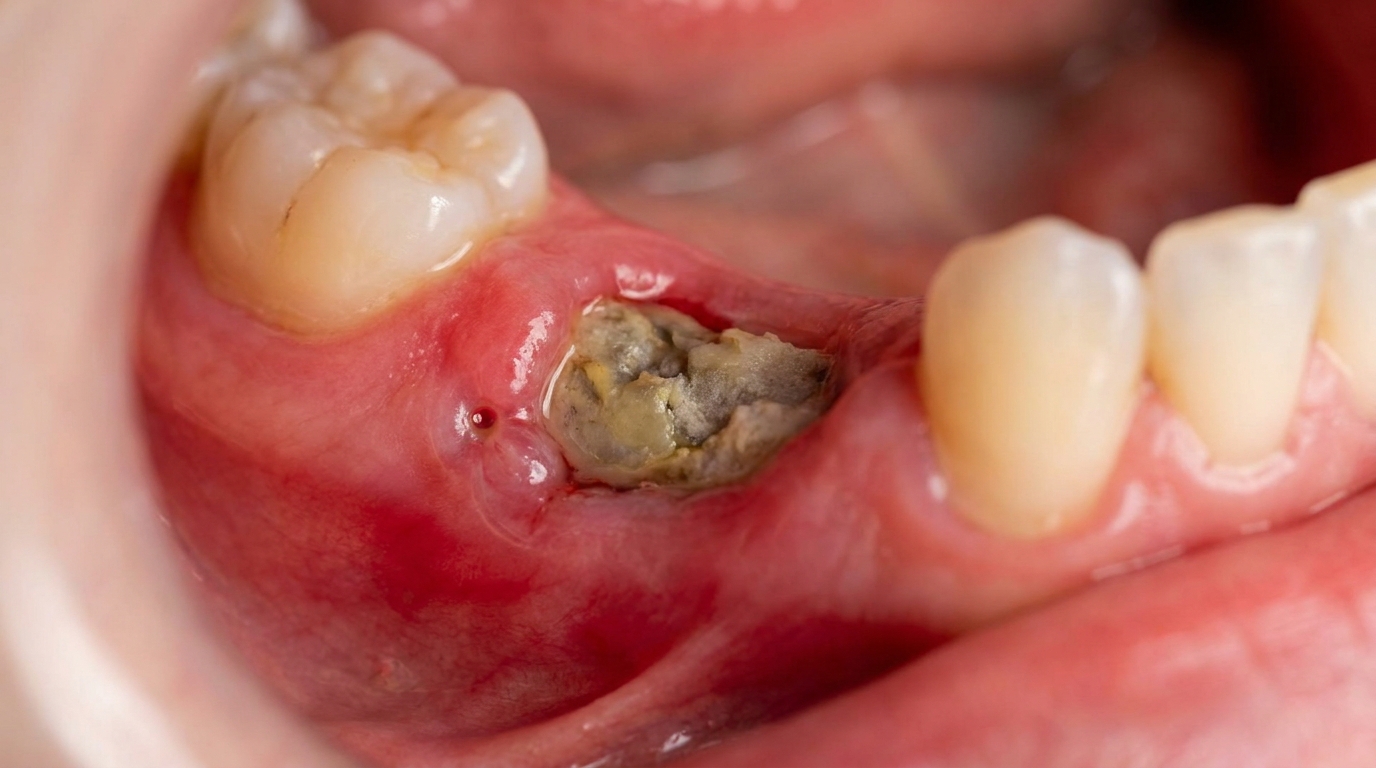
Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker , Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | Spreading dental infection, odontogenic cellulitis (a spreading bacterial infection through the soft tissues), fascial space infection, cervicofacial cellulitis; severe forms include Ludwig's angina (a fast-spreading infection in the floor of the mouth) and cavernous sinus thrombosis |
How urgent? | 🔴 See a dentist promptly, and head to a hospital emergency department straight away if you have facial swelling with fever, difficulty swallowing, drooling, trouble breathing or eye changes |
Common or rare? | Localised dental abscess (a collection of pus walled off from surrounding tissue) is common; severe spreading cellulitis is uncommon in Australia; Ludwig's angina and cavernous sinus thrombosis are rare but life-threatening |
Who it affects | Adults and children of any age; risk is higher with diabetes, immunosuppression, poorly controlled medical conditions, IV drug use or delayed dental care |
Who treats it | General dentist for early stages; hospital and oral and maxillofacial surgical team for spreading or severe infections |
Based on | Regezi, Neville, Cawson and Laskaris |
What is it?
A dental abscess is a pocket of pus that builds up around the root of a tooth when bacteria from a deeply decayed, cracked or non-vital (with a dead nerve) tooth invade the surrounding tissue. If that infection breaks out of the bone and spreads diffusely through the soft tissues of the face and neck instead of staying contained, it becomes cellulitis, a rapidly spreading inflammation that follows the natural tissue planes between muscles. In its most severe forms, this spreading infection can threaten the airway and even become life-threatening, so an urgent dental assessment is critical.
Who tends to get it?
Dental abscesses can occur at any age, in anyone with an untreated dead tooth, a deep cavity, a failed root canal, a fractured tooth or advanced gum disease. The spread into cellulitis is more likely when treatment is delayed or when the body's defences are weakened.
According to the source textbooks, people at higher risk of severe spreading infection include those with:
Diabetes mellitus, particularly when poorly controlled
Long-term corticosteroid or chemotherapy use
Cancer or blood disorders such as neutropenia or aplastic anaemia
HIV/AIDS or other immune suppression
Heavy tobacco or alcohol use, or intravenous drug use
Limited access to regular dental care
Ludwig's angina, the most feared form, most often develops in adults and follows infection of a lower second or third molar in around 90 percent of cases. Most deaths occur in patients over 40 with other medical conditions.
What causes it?
A dental abscess almost always starts inside a tooth. Common triggers include:
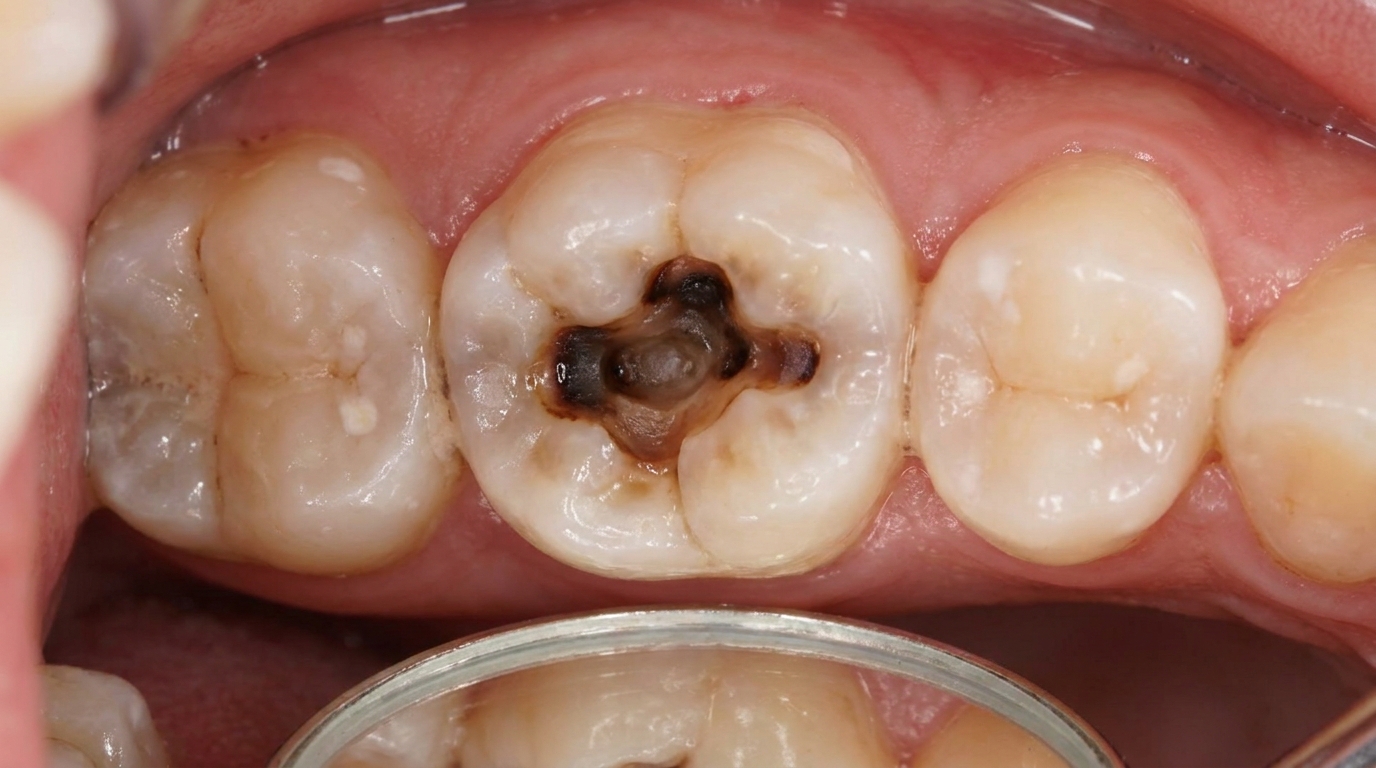
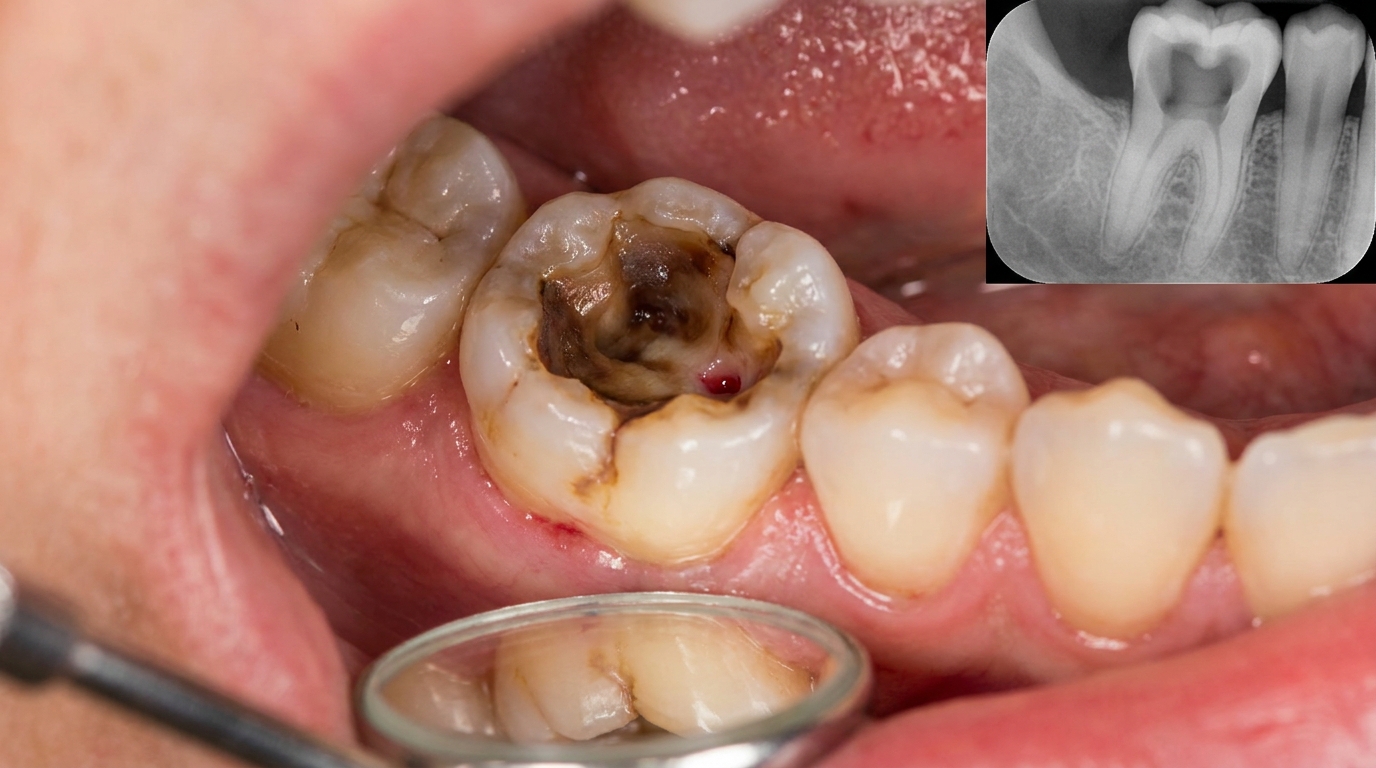
A deep cavity that reaches the nerve
A cracked or fractured tooth
Trauma that has killed the pulp (the soft nerve and blood vessel core of the tooth), sometimes years earlier
A failed or incomplete root canal treatment
Advanced gum disease producing a periodontal abscess
Pericoronitis around a partly erupted wisdom tooth
The bacteria responsible are not a single organism but a mixed community drawn from the mouth's normal flora. Anaerobic bacteria (those that thrive without oxygen) play a leading role, alongside streptococci and other facultative species. Modern molecular studies show even greater microbial diversity than older culture methods suggested.
Whether a localised abscess stays contained or breaks loose into cellulitis depends on the virulence of the bacteria, how quickly drainage is achieved and how strong the patient's immune defences are.
How does it develop?
Think of the inside of a tooth as a sealed room with one tiny door at the root tip. When bacteria gain access through a cavity or crack, they kill the nerve and multiply in this protected space. Pressure builds until the infection is forced out through that tiny door at the apex of the root, into the bone of the jaw.
From there, pus follows the path of least resistance. Often it perforates the thin outer layer of bone (usually on the cheek side, where the bone is thinnest) and forms a swelling under the gum or skin. If it can drain, through a small opening in the gum called a parulis or "gum boil", or through the tooth itself, symptoms ease and the infection becomes chronic.
If drainage is blocked, the pus has to go somewhere. It can:
Spread through the medullary spaces of the jawbone, causing osteomyelitis
Burst out into the soft tissues of the face, cheek or neck as cellulitis
Travel along the natural slip-planes between muscle layers (the fascial spaces, the connective-tissue planes between muscles where infection can spread) which connect the floor of the mouth, neck and even the chest
Unlike a localised abscess, cellulitis is not walled off. The inflammatory fluid actively opens up the fascial spaces and carries bacteria with it, so the infection moves quickly.
What might you notice?
What it looks like
In the early stages, you may see a small pimple-like spot on the gum next to a sore tooth, sometimes with a yellow-white head where pus is draining. The gum and cheek over the tooth may look red and puffy.
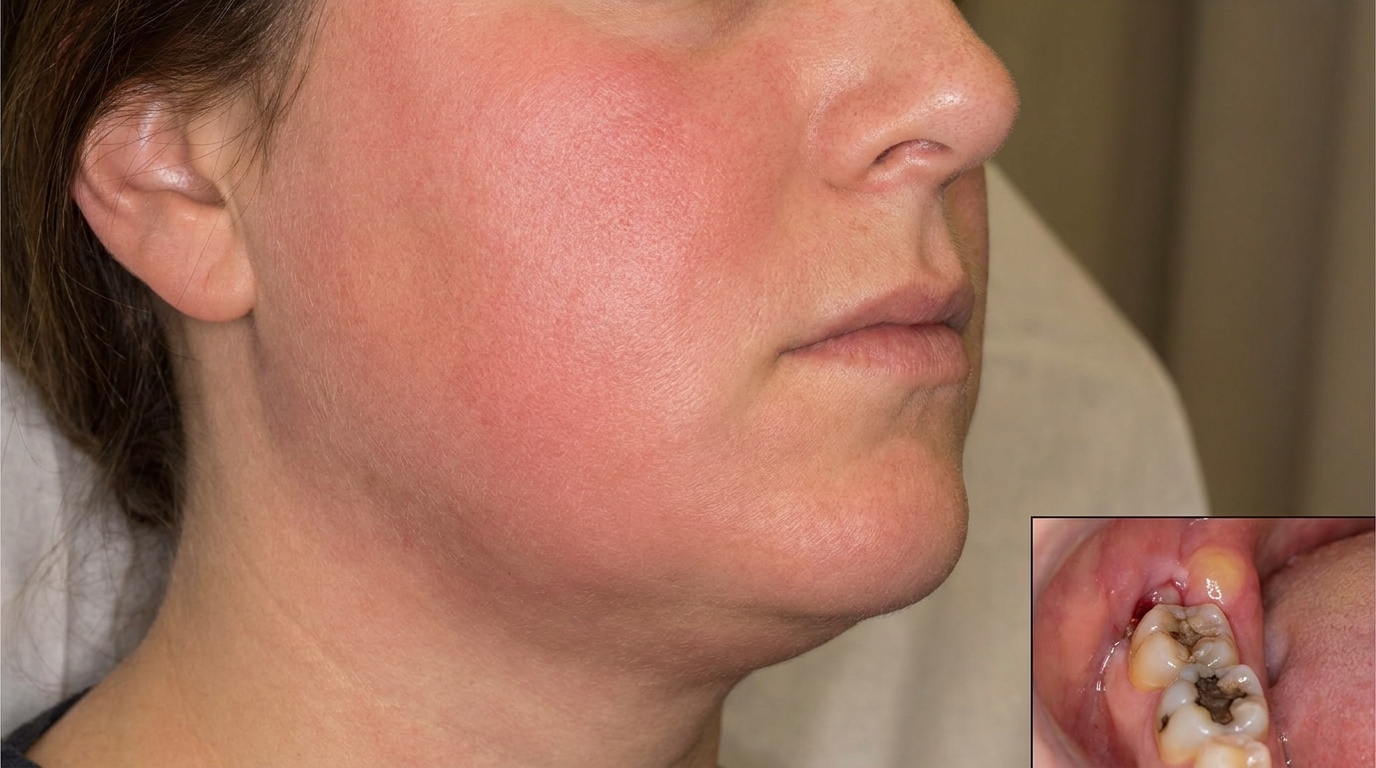
As the infection spreads, the swelling enlarges and changes character. The face becomes visibly distorted, sometimes the swelling closes the eye on the affected side, particularly with infections of the upper canine, or pushes out from under the jawline. The skin overlying a true cellulitis is taut, shiny and dusky red, and the swelling feels firm or even "woody" rather than soft. Both sides of the neck may swell in Ludwig's angina, with the floor of the mouth raised and the tongue pushed up against the palate.
A chronic abscess that has been quietly draining for some time can produce a small lump on the chin or jaw skin (a cutaneous sinus), sometimes mistaken for a skin condition for months or years before someone looks at the teeth.
What it feels like
A developing abscess hurts. The classic features include:
Severe, throbbing toothache that worsens when you bite down
A feeling that the tooth is "high" or has been pushed slightly out of its socket
Sharp pain on tapping the tooth
Tenderness when chewing or putting pressure on the area
Swelling that may temporarily ease as pus finds a way to drain
With spreading cellulitis, the local pain is joined by general signs of being unwell, fever, chills, malaise, fatigue and swollen tender lymph nodes in the neck. As swelling involves the floor of the mouth and the muscles of swallowing and chewing, you may notice difficulty opening the mouth (trismus, difficulty opening the mouth), trouble swallowing, drooling, a muffled voice or sore throat.
Red flag warning signs that need emergency care, not a routine appointment:
Difficulty breathing, noisy breathing or stridor
Trouble swallowing your own saliva or drooling
Inability to open the mouth more than a finger's width
Tongue pushed up so the floor of the mouth feels hard and raised
Fever above 39°C with rapidly growing facial or neck swelling
Eye involvement, swelling of the eyelid, bulging of the eye, double vision or loss of vision
Confusion, stiff neck or severe headache
Rapidly spreading dusky or purplish skin discolouration
What an X-ray might show
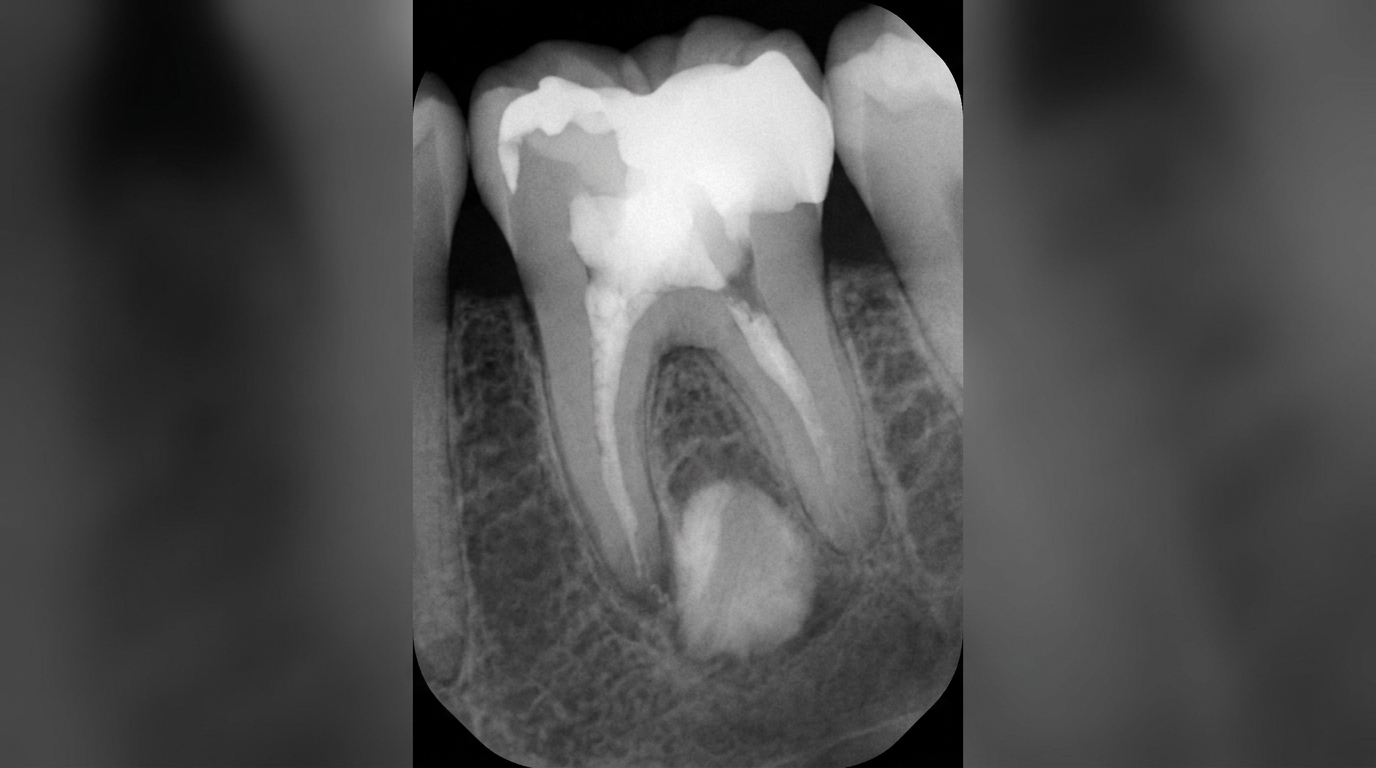
In the very early stages of an acute abscess, an X-ray may look almost normal because there has not been enough time for bone changes. As the infection persists, a dental film often shows a widened periodontal ligament space at the tip of the root, or an ill-defined dark area (radiolucency) in the bone around the apex.
For severe cellulitis, plain X-rays are not enough. A contrast-enhanced CT scan is generally the best way to map the spread of infection through fascial spaces and identify any pockets of pus that need draining. High-resolution ultrasound and MRI are used in some situations.
What happens at the dentist?
At ArtSmiles, a dentist will start by asking about your symptoms and medical history, then examine the area. They will typically:
Look for a deeply decayed, cracked, heavily restored or discoloured tooth
Tap on suspect teeth, a sharp response usually means an inflamed periapical (at the tip of a tooth root) area
Test the tooth's response to cold or, sometimes, an electric pulp tester (a non-vital tooth gives no response)
Feel the gum and face for swelling, tenderness, fluctuance (a soft spot suggesting pus) or firm board-like infiltration
Take dental X-rays to look for periapical changes
Check your temperature and assess how unwell you appear overall
For a small, well-localised abscess in an otherwise healthy patient, this is usually enough to plan treatment in the chair. Antibiotics alone are not recommended in this situation because they have minimal benefit and don't address the source.
When the dentist sees signs of spreading infection, significant facial swelling, fever, lymph node enlargement, trismus, floor-of-mouth elevation or a medically vulnerable patient, the situation is treated as more urgent. A sample for culture and sensitivity may be taken before antibiotics are started, imaging (often CT) may be requested, and hospital admission under an oral and maxillofacial surgery team is usually arranged for severe or life-threatening cases. Cavernous sinus thrombosis and Ludwig's angina are medical emergencies that require immediate hospital management, often in an intensive care setting, with airway protection as the top priority.
Is this serious?
🔴 A spreading dental infection is a serious problem that should not be put off.
A simple early abscess is highly treatable and rarely dangerous when dealt with promptly. Once the infection escapes the bone, however, the picture changes quickly. The textbooks describe several recognised complications, ranging from manageable to life-threatening:
Localised cellulitis of the face, uncomfortable but usually responds well to drainage of the source and appropriate antibiotics
Osteomyelitis, infection of the jawbone itself, requiring prolonged treatment
Ludwig's angina, bilateral swelling of the floor of the mouth and upper neck, with potential airway obstruction. Even with modern treatment, mortality remains around 10 percent and most deaths involve patients over 40 with other medical conditions
Cavernous sinus thrombosis, a rare but devastating complication where infection from upper teeth tracks into the venous sinuses behind the eyes, with mortality around 20 to 30 percent and a high risk of permanent visual impairment in survivors
Necrotising fasciitis, an uncommon but rapidly destructive infection of subcutaneous tissue
Mediastinitis, sepsis (a serious whole-body reaction to infection) or pneumonia, when infection tracks down the neck into the chest
The key message: a toothache with facial swelling is never "just a toothache".
If you've noticed any of these signs for more than two weeks, or any of the red flags above for more than a few hours, it's worth booking an assessment immediately, and going to a hospital emergency department for breathing, swallowing or eye symptoms.
Could it be something else?
Several other conditions can produce facial or oral swelling and need to be told apart from a spreading dental infection. Source textbooks list the following considerations:
Periapical abscess (localised), pus contained at the root tip without significant facial spread. Looks similar in early stages, distinguished by absence of diffuse facial swelling, fever or systemic illness.
Periodontal abscess, pus arising from a deep gum pocket rather than a non-vital tooth. The tooth usually remains vital, and the swelling sits at the gumline rather than near the root tip.
Pericoronitis, inflammation around a partly erupted wisdom tooth. Pain and swelling localise to the back of the jaw with overlying gum flap, rather than originating from a clearly carious or non-vital tooth.
Acute submandibular sialadenitis, bacterial infection of the submandibular salivary gland. Painful swelling under the jaw can mimic submandibular cellulitis; distinguished by inflammation at the duct opening on the floor of the mouth and pus discharge from the duct on gland massage.
Acute suppurative parotitis, infection of the parotid gland producing swelling in front of the ear. Pus is seen draining from the parotid duct opening near the upper molars.
Erysipelas, superficial bacterial cellulitis of the skin caused by streptococcus, with a sharply demarcated raised border, unlike the diffuse spread of odontogenic cellulitis.
Buccal cellulitis of childhood (Haemophilus influenzae type B), diffuse purplish facial swelling in young children, distinguished by age, lack of dental source and characteristic skin discolouration.
Peritonsillar abscess ("quinsy"), complication of tonsillitis with swelling and redness of the tonsil. Pain is throat-centred, the tooth examination is normal, and the soft palate is pushed across the midline.
Angio-oedema, recurrent painless soft swelling of the lips, cheek or face, often allergic. No fever, no systemic illness and no dental cause; the patient is well between attacks.
Orofacial granulomatosis, Crohn's disease or sarcoidosis, recurring firm swelling of the lip or cheek with no infection. Distinguished by chronicity, lack of fever and biopsy showing non-caseating granulomas.
Insect bite, sting or trauma-related haematoma, sudden swelling with a clear history; no dental cause and no fever.
Infected jaw cyst, slow-growing swelling with X-ray evidence of a well-defined cystic lesion that has become acutely infected.
Jaw or salivary gland tumour, slowly progressive firm swelling; lack of fever, longer history and characteristic imaging help distinguish.
Actinomycosis, chronic bacterial infection that produces multiple draining sinuses with characteristic "sulphur granules". The course is far slower than acute cellulitis.
Necrotising fasciitis, distinguished from ordinary cellulitis by rapid spread of dusky-red then purplish-black skin discolouration, severe pain out of proportion to appearance and visible gas in the tissues on imaging.
A dentist will use the pattern of pain, the state of the teeth, X-ray findings, the speed of onset and overall systemic signs to work out which one is most likely.
How is it treated?
At home (early stages or while waiting for an appointment):
Take simple pain relief such as paracetamol or ibuprofen as directed by your pharmacist
Keep the area clean with gentle warm salt-water rinses
Avoid biting on the affected tooth
Stay well hydrated and rest
Do not apply heat to the outside of the face, as this can encourage spread
Do not try to lance a swelling yourself
See a dentist as soon as possible, this is not a problem that fixes itself
Professional treatment addresses two priorities: removing the source of infection and controlling its spread.
For a localised dental abscess, treatment may include:
Establishing drainage through the tooth (opening the pulp chamber) or through a small incision in the gum if there is a soft fluctuant swelling
Root canal treatment to clean and seal the inside of the tooth
Extraction of the tooth if it cannot be saved
A short course of antibiotics is generally only added when there are signs of spreading infection, fever, lymph node involvement or a medically vulnerable patient
For spreading cellulitis, fascial space infections and Ludwig's angina, hospital-based treatment is the standard. This typically includes:
Immediate assessment and protection of the airway (which may include intubation or, in severe cases, surgical airway access)
Intravenous antibiotic therapy, penicillin combined with metronidazole, or clindamycin where penicillin is unsuitable, with adjustments based on culture results
Surgical drainage of any collections of pus
Removal of the offending tooth
Supportive care for fever, hydration and pain
Close monitoring, often in a high-dependency or intensive care setting for severe cases
Cavernous sinus thrombosis and necrotising fasciitis require especially aggressive surgical and medical intervention by specialist teams.
What's the long-term outlook?
When a dental infection is caught early, the outlook is excellent. Drainage and definitive treatment of the source tooth usually settle symptoms within a couple of days and the bone heals over the following weeks to months. A small sinus tract on the gum or skin almost always closes on its own once the offending tooth is treated or removed.
For cellulitis that has spread but is treated promptly, most patients recover fully. The longer treatment is delayed, the more demanding the recovery, and severe complications like Ludwig's angina or cavernous sinus thrombosis carry a real risk of long-term harm or death even with modern care.
The best long-term protection comes from prevention:
Treat tooth decay early, before it reaches the nerve
Have non-vital or symptomatic teeth assessed and treated promptly
Don't ignore a discoloured front tooth, even if it doesn't hurt, pulp can die quietly after an old knock
Keep up regular dental check-ups
Manage diabetes, immune conditions and smoking, which all raise the risk of severe infection
Take any pain or swelling around a tooth seriously and seek care quickly
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
The cover image above is an AI-generated illustration based on the most common visible features of this condition described in clinical pathology references. It is not a photograph of a real case and should not be used to diagnose or rule out the condition in your own situation. If you are concerned about something you have noticed, please book an assessment with a registered dental practitioner.
References
Regezi, J. A., Sciubba, J. J., & Jordan, R. C. K. (2017). Oral pathology: Clinical pathologic correlations (7th ed.). Elsevier. Chapter 13, Inflammatory Jaw Lesions, pp. 314 to 318.
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2023). Oral and maxillofacial pathology (5th ed.). Elsevier. Chapter 3, Pulpal and Periapical Disease (Periapical Abscess and Cellulitis), pp. 129 to 134; Chapter 5, Bacterial Infections (Buccal Cellulitis and related infections).
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 4, Pulpitis, Apical Periodontitis (pp. 66 to 69); Chapter 6, Major Infections of the Mouth, Jaws and Perioral Tissues (Fascial Space Infections, Ludwig's Angina, Cavernous Sinus Thrombosis, Necrotising Fasciitis), pp. 106 to 108.
Laskaris, G. (2003). Color atlas of oral diseases (3rd ed.). Thieme. Chapter 17, Bacterial Infections (Oral Soft-Tissue Abscess, Buccal Cellulitis), pp. 146 to 149.
Frequently asked questions
Is a dental abscess an emergency?
It can be. A localised tooth abscess with mild swelling is usually treatable within 24-48 hours by a dentist. But if the swelling is spreading across the face or down the neck, if you have a fever, trouble swallowing or any change in breathing or voice, that is a medical emergency and warrants the nearest emergency department straight away.
Will antibiotics on their own fix a dental abscess?
No. Antibiotics may help control spreading infection or systemic symptoms, but they do not remove the source. A dental abscess needs the source tooth to be either drained, treated with a root canal, or extracted. Antibiotics alone often delay definitive treatment and let the infection come back.
What is the difference between an abscess and cellulitis?
An abscess is a localised pocket of pus that can usually be drained. Cellulitis (which the textbooks also describe as a phlegmon or spreading inflammation) is a more diffuse infection moving through the soft tissues, with no clear collection of pus to drain. Cellulitis tends to be more dangerous because it can spread quickly and threaten the airway.
Can a dental abscess come back after treatment?
Once the source tooth is properly treated (root canal completed or tooth extracted) and any pus has been drained, recurrence is uncommon. If symptoms return after treatment, it usually means there is a missed canal, a crack in the tooth, or persistent infection that needs further investigation.