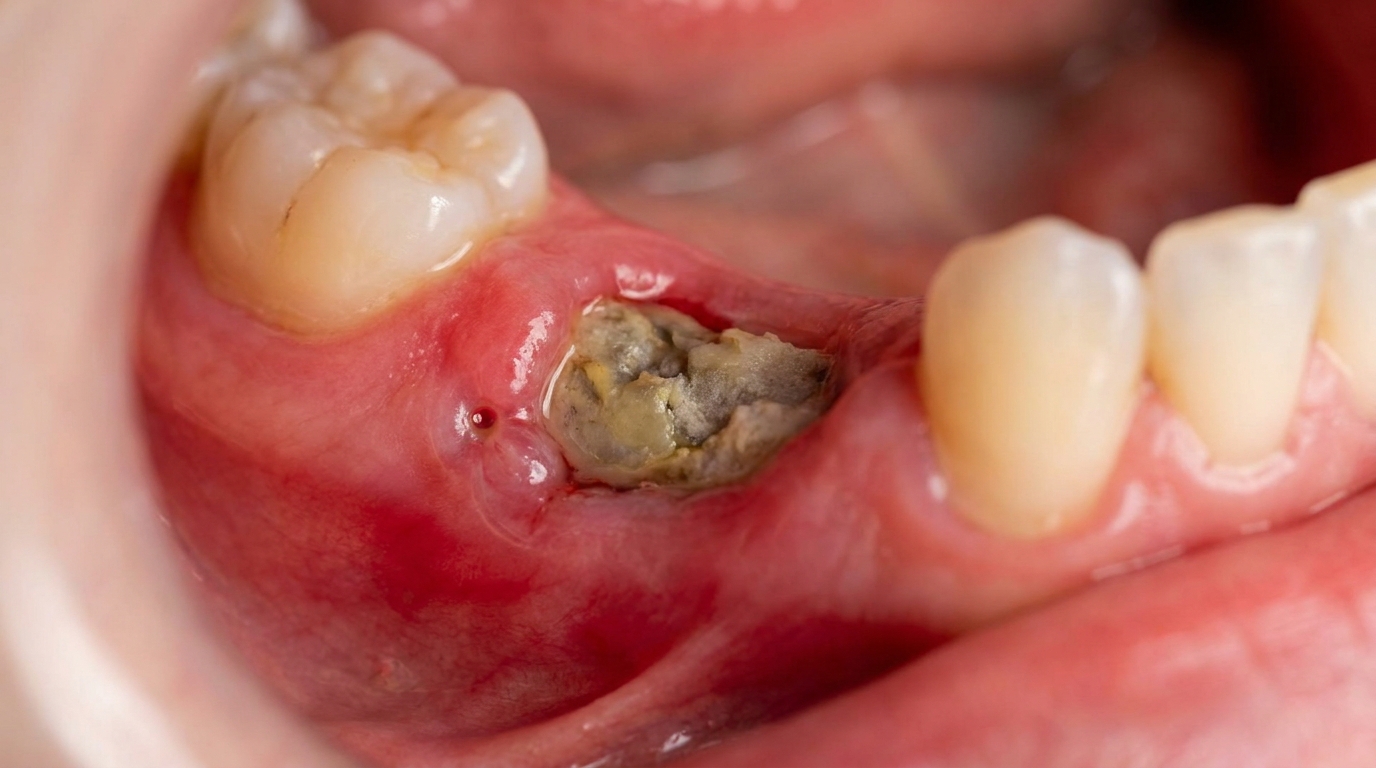
Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker , Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | Tooth decay, cavities, dental cavities, caries |
How urgent? | 🟡 Worth checking, early lesions can be reversed; once a cavity has formed, treatment is needed before it reaches the nerve |
Common or rare? | One of the most common diseases in humans worldwide and a major cause of tooth loss |
Who it affects | Children and adults; rises with frequent sugar intake, plaque (the soft, sticky film of bacteria on tooth surfaces) retention, dry mouth, and gum recession in older adults |
Who treats it | General dentist, through prevention, fillings and, in deeper cases, root canal treatment |
Based on | Cawson, with cross-references in Neville and Regezi |
What is it?
Dental caries is a bacterial disease in which acid produced by certain mouth bacteria slowly dissolves the mineral structure of the tooth. The early phase happens beneath an apparently intact surface, the tooth becomes weaker before any visible hole appears. Eventually the surface breaks down, forming the cavity most people recognise as "tooth decay". If the process continues, bacteria reach the soft inner tissue of the tooth (the pulp), the soft nerve and blood vessel core of the tooth, causing pain, infection and, in severe cases, tooth loss. Caries is one of the most common diseases in humans and remains a major reason teeth are lost.
Who tends to get it?
Caries can affect anyone with teeth, but some groups are more at risk:
Children, especially those given sweetened drinks, sweets between meals, or whose teeth are not well brushed. Decay in baby teeth often progresses faster because their enamel (the hard outer layer of the tooth) is thinner and the pulp sits closer to the surface.
Older adults with gum recession that exposes the softer root surface to plaque.
People with reduced saliva flow (dry mouth, or xerostomia), dry mouth from medications, salivary gland disease, or radiotherapy to the head and neck. Saliva is one of the body's most important defences against caries, and rampant decay is well-recognised when it is reduced.
People with frequent sugar intake, particularly between meals or in sticky form.
People with crowded teeth, deep grooves, or fixed appliances (such as orthodontic brackets) that trap plaque.
People with high-carbohydrate, high-snacking diets during stress, illness or shift work.
Caries is not strongly inherited. Some old beliefs about "soft teeth" or vitamin deficiency causing decay have been disproven, well-nourished populations have historically had the highest decay rates, while populations on poor diets have had the lowest.
What causes it?
The textbooks describe four key ingredients that all need to be present for caries to develop. If any one of them is missing, decay does not occur:
cariogenic (decay-causing) bacteria, particularly Streptococcus mutans (a common cavity-causing bacterium), supported later by lactobacilli (acid-producing bacteria often found in deeper cavities). These bacteria are very good at producing acid and at sticking to tooth surfaces.
Dental plaque, a sticky biofilm (a thin sticky bacterial layer) of bacteria and food residue that holds the acid in close contact with the tooth and shields it from saliva.
A fermentable substrate, most commonly sucrose (table sugar). The bacteria convert sucrose into lactic acid and into a sticky, glue-like polysaccharide (glucan) that helps plaque grip the tooth.
A susceptible tooth surface and time, places where plaque can sit undisturbed (deep grooves, between teeth, around the gum line) and enough time for repeated acid attacks to outpace the tooth's natural repair.
A few important nuances from the textbooks:
Sucrose is the most cariogenic sugar because it both feeds acid production and helps build sticky plaque.
Other sugars (glucose, fructose, lactose) are less cariogenic.
Sugar substitutes such as xylitol, sorbitol, mannitol and the artificial sweeteners (saccharin, aspartame, acesulfame K) are non-cariogenic and can be used as safer alternatives.
Frequency matters more than amount. The classic Vipeholm study showed that sticky sweets eaten between meals caused far more decay than the same amount of sugar eaten only at mealtimes.
Saliva and fluoride are the two strongest natural and added defences.
How does it develop?
Caries develops in stages, each of which is described clearly in the textbooks.
1. The early (white spot) lesion. Acid from plaque diffuses just below the enamel surface and dissolves a tiny amount of mineral. The surface still looks intact and feels smooth, but a chalky-white area appears beside contact points or in grooves. Critically, this stage is reversible. Saliva, fluoride and reduced acid attacks can rebuild the lost mineral.
2. Cavitation. If demineralisation (the loss of minerals from the tooth surface) continues to outpace repair, the surface eventually breaks down and a cavity forms. Once cavitation has occurred, the lesion is no longer reversible and a filling will be needed to restore the tooth.
3. Dentine caries. Bacteria pass through the broken enamel and spread along the junction between enamel and dentine (the softer layer under the enamel). Dentine is softer than enamel and decay spreads more easily. The lesion is shaped like a cone with the point heading toward the pulp.
4. Pulpitis (inflamed nerve). Acids and bacteria reach the dentine close to the pulp. The pulp tries to defend itself by laying down extra (reactionary) dentine, but if decay is fast or deep, inflammation sets in. This is when toothache typically begins.
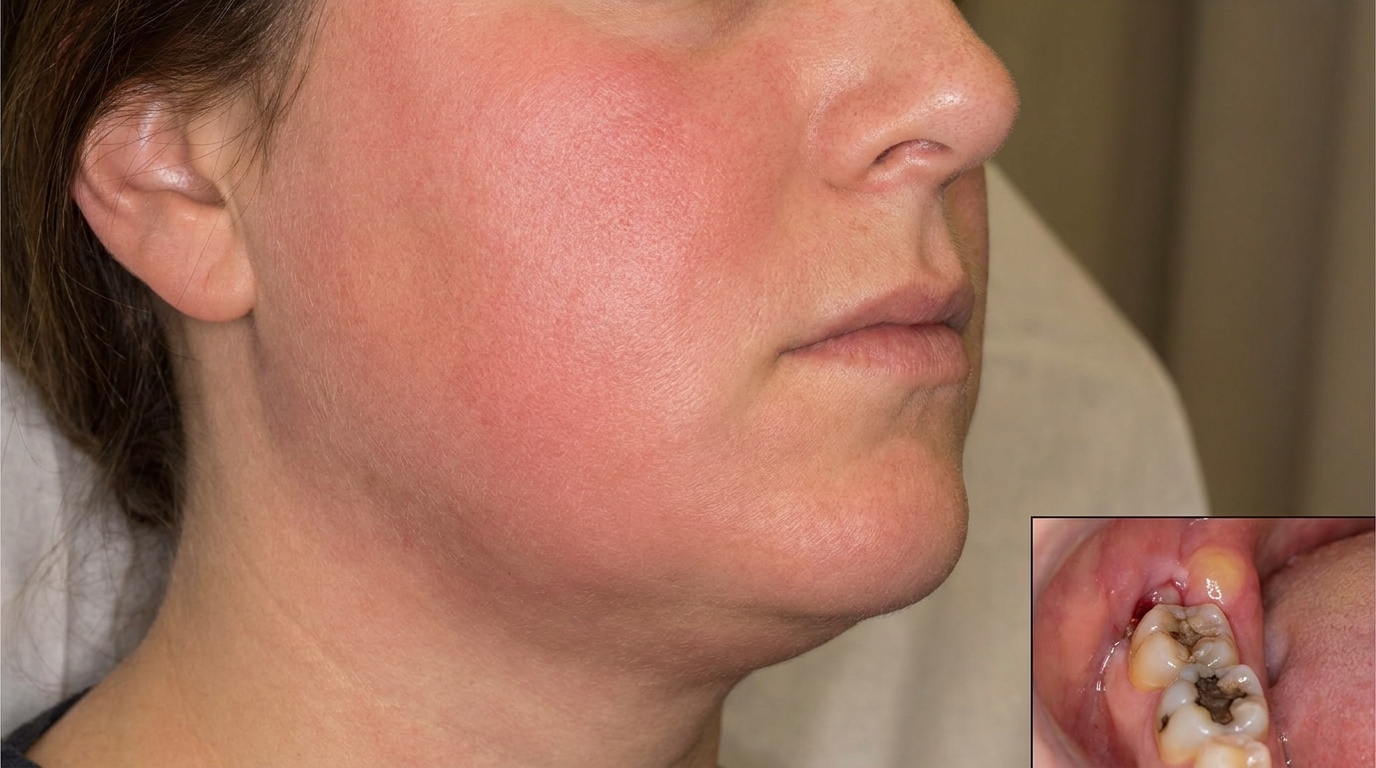
5. Apical periodontitis and abscess. If pulpitis is left untreated, the pulp can die and bacteria spread out the tip of the root, causing inflammation and infection of the bone around the root tip. This may form an abscess and, in rare cases, infection can spread further into the jaw.
Two natural protections slow this process. Saliva washes food and acid away and contains bicarbonate that buffers acid. Fluoride, from drinking water, toothpaste and professional gels, both makes enamel less soluble in acid and helps damaged enamel rebuild itself. Cawson notes that "fluoride is the only nutrient that has been proven to have this protective action" and that the introduction of fluoridated water and toothpaste has had a major impact on caries rates worldwide.
What might you notice?
What it looks like
Decay can look very different depending on the stage and location:
Chalky white spot on a smooth surface, often near the gum line or just beside where two teeth touch, the earliest visible sign.
Brown spot lesion, the same sub-surface lesion after years of slow remineralisation (the re-strengthening of the tooth surface with minerals from saliva and fluoride), when the porous enamel has picked up dietary pigments. These can be stable and inactive.
Dark line in a groove on a chewing surface, sometimes with chalky enamel around it (an occlusal (chewing) surface lesion).
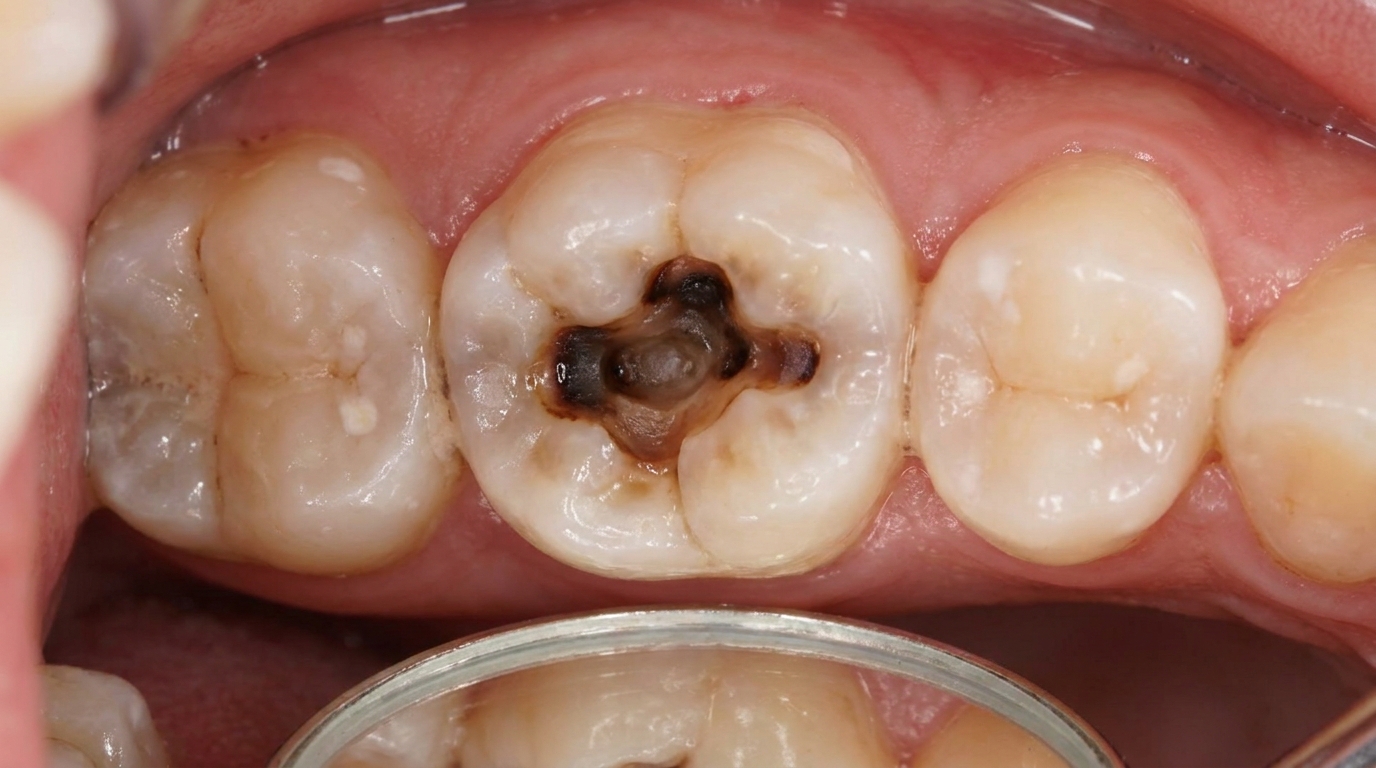
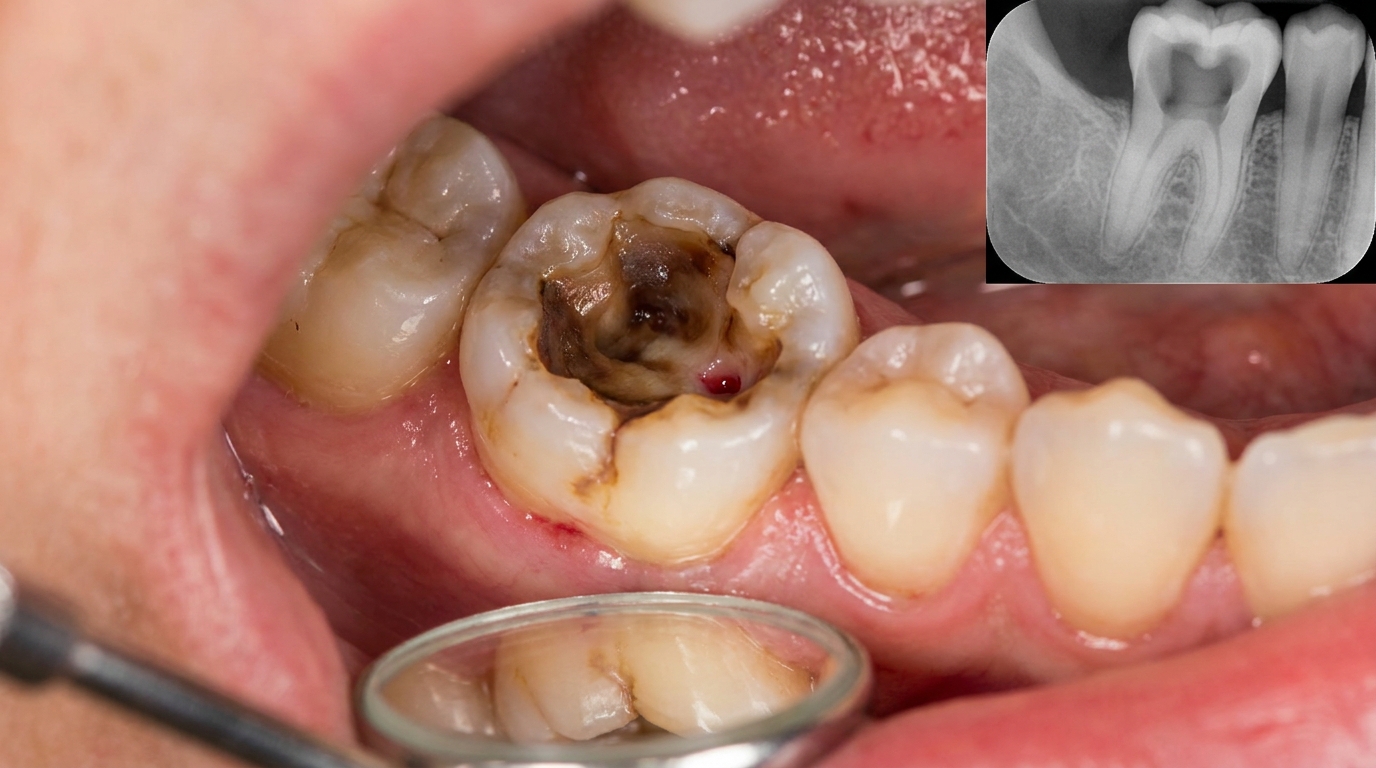
Visible hole or cavity, with brown or black soft tissue inside.
Grey shadow under an apparently intact enamel surface, often the first clue on a back molar that decay has spread within the dentine.
Soft, leathery root surface at the gum line in older adults (root caries).
What it feels like
Early caries does not hurt at all. Symptoms generally appear only once the decay reaches the dentine or pulp:
Sensitivity to cold drinks or sweet foods, which fades quickly when the trigger is removed.
A sharp pain when biting on the tooth, especially with sticky foods (this can also signal a cracked tooth).
Persistent toothache, including pain that wakes you at night, suggests the pulp is significantly inflamed.
A bad taste or visible food packing in a tooth that did not previously trap food.
Sometimes no symptoms at all, important caries is often picked up only on routine examination or X-ray.
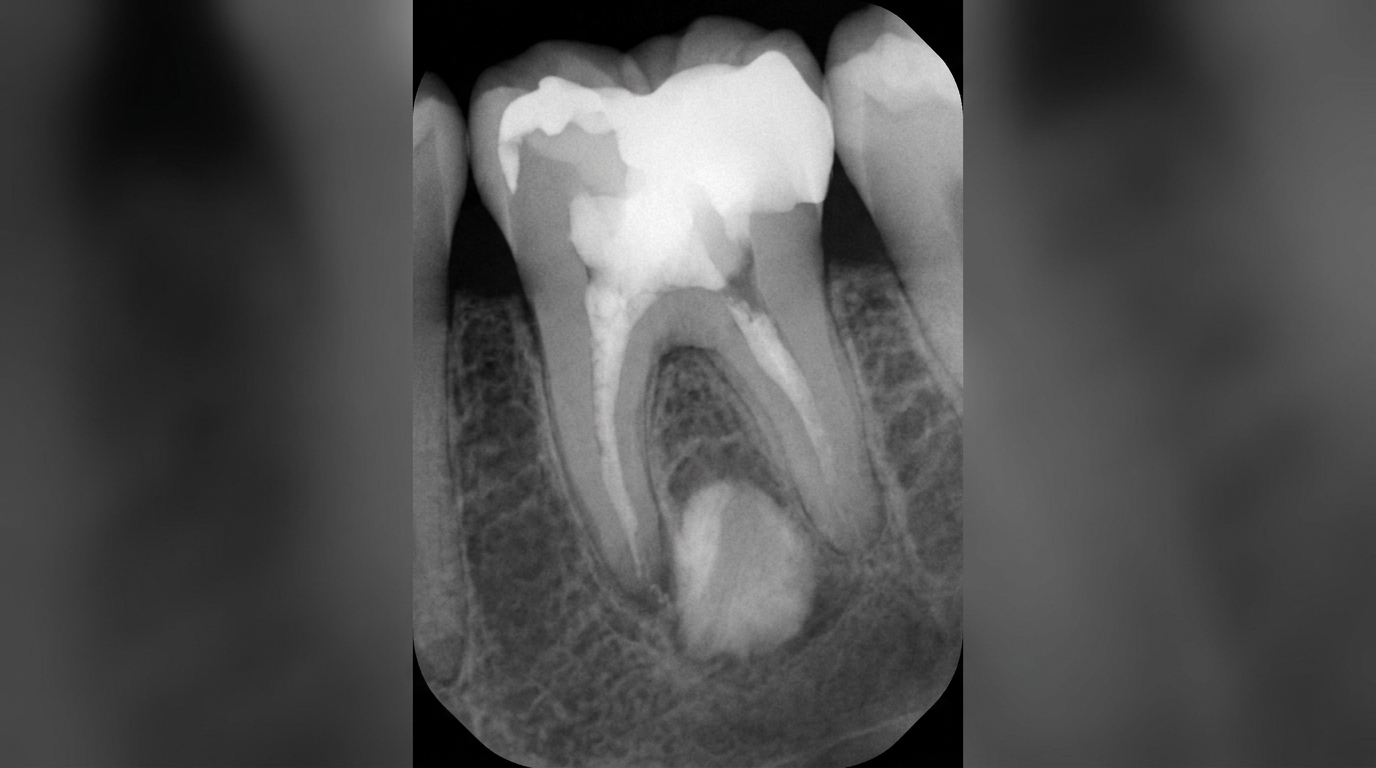
What an X-ray might show
Bite-wing X-rays are the standard tool for finding caries between the teeth, where it cannot be seen on the surface. On these images, a carious lesion shows up as a dark notch or wedge eating into the enamel and, later, the dentine. Bite-wings can also reveal "occult" caries, decay hidden beneath an intact occlusal surface where the underlying lesion is much larger than the surface suggests.
What happens at the dentist?
Caries is most often picked up at a routine dental check-up and clean at ArtSmiles. The dentist will typically:
Examine each tooth visually under good light, looking for white spots, brown spots, dark grooves, broken enamel and soft surfaces.
Probe gently along surfaces and grooves, without pressing hard into apparently intact spots, since pressure can convert a remineralising lesion into an active cavity.
Take bite-wing X-rays at intervals appropriate to risk, looking for early lesions between the teeth.
Use transillumination (shining a bright light through the tooth) to detect cracks and small lesions on front teeth.
Assess overall caries risk, diet, fluoride exposure, saliva flow, oral hygiene, medical conditions, to decide whether the right next step is observation and prevention, or restoration.
Discuss findings honestly, including whether an early lesion can be remineralised rather than restored, and what would change that decision later.
This last point matters. The textbooks emphasise that not every lesion needs a filling. Small, slow-moving enamel lesions in a low-risk patient may be observed and remineralised. Lesions in a high-risk patient cavitate earlier and are restored sooner.
Is this serious?
🟡 Caries itself is not life-threatening, but it is one of the most important reasons teeth are lost over a lifetime. Untreated decay almost always progresses, eventually leading to severe toothache, infection of the bone around the root, abscess formation, tooth loss, and, in rare cases, spread of infection into the jaw and beyond. Children with deep decay can lose baby teeth before they would naturally fall out, which can affect how the adult teeth come through. Catching caries at the white-spot stage almost always avoids drilling, and catching it as a small cavity almost always avoids root canal treatment.
If you've noticed a hole on a tooth, sensitivity to sweet or cold, or pain when biting that has lasted more than a couple of days, it's worth booking an assessment so the cause can be identified and the right next step recommended.
Could it be something else?
Several conditions can mimic caries or cause similar symptoms. The textbooks list these as the main differentials:
Dental erosion, loss of tooth surface from non-bacterial acid (acid reflux, fizzy drinks, frequent vomiting). Erosion produces shallow, smooth, polished hollows on cusp tips and the tongue side of upper front teeth, rather than dark cavities at contact points.
Tooth wear from attrition, flat, polished facets on biting surfaces from grinding or clenching.
Tooth wear from abrasion, V-shaped notches at the gum line from over-vigorous toothbrushing, often with hard bristles.
Abfraction, small notches at the necks of teeth thought to relate to bending stresses; can look similar to early root caries but is not bacterial.
Dental fluorosis, chalky white or mottled brown patches on enamel formed during tooth development from excessive fluoride exposure. Fluorosis affects symmetrical teeth in patterns rather than localised contact-point lesions.
Enamel hypoplasia, areas of thin or pitted enamel from disturbances during tooth formation (illness, trauma to a baby tooth, certain medications). The defect is present from the moment the tooth erupts, not progressive.
Internal resorption, the tooth dissolves from the inside, sometimes producing a pinkish patch on a front tooth (the "pink tooth of Mummery"). This is uncommon and usually identified on X-ray.
Cracked tooth syndrome, pain on biting from a fine crack rather than a cavity, often without any visible decay. Distinguished by special tests such as biting on a wedge or transillumination.
How is it treated?
Treatment depends on how far the decay has progressed and on the patient's overall caries risk. The textbooks lay out a clear hierarchy: prevent first, remineralise where possible, restore conservatively where necessary, save the pulp where you can.
At-home measures that may help:
Brush with fluoride toothpaste twice a day, last thing at night and at one other time. Don't rinse vigorously after brushing; allowing a thin film of fluoride to remain on the teeth helps remineralisation.
Floss or use interdental brushes daily to break up plaque between teeth, where most adult decay starts.
Reduce frequency of sugar intake. The Vipeholm finding still stands, sticky sweets between meals are far more damaging than the same amount of sugar eaten with a meal.
Choose sugar substitutes (xylitol, sorbitol, aspartame) where possible, especially in chewing gum, since chewing sugar-free gum after meals also stimulates protective saliva flow.
Drink fluoridated tap water where available, Australian water is fluoridated in most metropolitan areas, including the Gold Coast.
Address dry mouth if you have it, sip water often, use saliva substitutes, and review medications with your GP. Dry mouth dramatically accelerates decay, including in people who otherwise had healthy teeth. (See the related article on xerostomia.)
Keep up regular check-ups at intervals appropriate to your risk, every 6 to 12 months is typical for low-risk adults, more often for higher-risk situations.
Professional steps your dentist may consider:
Topical fluoride applications (varnishes, gels) for higher-risk patients or where early lesions are present.
Fissure sealants, thin protective coatings placed on deep grooves of newly erupted molars to keep plaque out of stagnation areas.
Remineralisation programmes for white-spot lesions, focused fluoride, dietary advice, plaque control, and regular review rather than immediate drilling.
Dental fillings, once a cavity has formed, the decay is gently removed and the tooth is rebuilt with a tooth-coloured composite or another suitable material. The textbooks emphasise conservation: only the dentine that cannot remineralise needs to be removed under a well-sealed restoration.
Indirect restorations, inlays, onlays or crowns, for larger lesions where a filling would not be strong enough.
Root canal treatment if the pulp is irreversibly inflamed or has died, to clean and seal the canal system and save the tooth.
Extraction as a last resort if the tooth cannot be restored, followed by replacement options such as a dental implant or bridge.
A patient-centred approach matters at every step. The textbooks highlight that effective caries management is as much about understanding diet, saliva, fluoride and habits as it is about drilling and filling, values that sit at the heart of our clinical philosophy.
What's the long-term outlook?
The outlook depends heavily on what stage the decay is caught at and on long-term habits. Early enamel lesions can remineralise and never need restoration. Small cavities, restored conservatively and looked after well, can last many years. Deep lesions that have reached the pulp need root canal treatment to save the tooth, and the resulting tooth, while no longer "alive", can usually still serve for a long time. Where decay is caught late and the tooth is lost, modern replacements such as implants and bridges restore most of the function. The single most powerful predictor is whether the underlying drivers, sugar frequency, plaque control, fluoride exposure and saliva flow, are addressed. Without that, new decay tends to appear around old fillings; with it, even high-risk teeth can stabilise and last a lifetime.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
The cover image above is an AI-generated illustration based on the most common visible features of this condition described in clinical pathology references. It is not a photograph of a real case and should not be used to diagnose or rule out the condition in your own situation. If you are concerned about something you have noticed, please book an assessment with a registered dental practitioner.
References
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 3, Dental Caries: aetiology, microbiology, plaque, sucrose, fluoride, saliva, pathology of enamel and dentine caries, and clinical aspects, pp. 39 to 59.
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 4, Pulpitis, Apical Periodontitis, Resorption and Hypercementosis: caries-induced pulpitis and periapical disease, pp. 60 to 66.
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2023). Oral and maxillofacial pathology (5th ed.). Elsevier. Chapter on Pulpal and Periapical Disease: caries as the primary cause of pulpitis and apical periodontitis.
Regezi, J. A., Sciubba, J. J., & Jordan, R. C. K. (2017). Oral pathology: Clinical pathologic correlations (7th ed.). Elsevier. Chapter on Pulpal and Periapical Inflammatory Disease: caries-related pulpitis and abscess formation.
Frequently asked questions
What causes dental caries?
Dental caries (tooth decay) is caused by acids produced by plaque bacteria as they ferment sugars from food and drinks. Repeated acid attacks gradually dissolve the mineral in enamel and dentine. Risk factors include frequent sugary intake, poor brushing, low fluoride exposure, dry mouth and certain medications.
Can early dental caries be reversed?
Yes. The very earliest stage, called incipient caries or a 'white spot lesion', involves only the surface enamel and can be remineralised with fluoride toothpaste, professional fluoride applications, dietary changes and improved plaque control. Once a cavity has formed in the dentine, a filling or other restoration is needed.
Does a cavity always hurt?
No. Early and even moderate cavities are often painless. Pain typically only develops once decay reaches the inner pulp tissue, by which point treatment is more involved (often root canal). That's why routine check-ups and X-rays matter, they catch caries while it's still simple to treat.
How is dental caries prevented?
Brushing twice a day with fluoride toothpaste, daily flossing, limiting sugary snacks and drinks between meals, drinking fluoridated water, and regular dental check-ups with professional cleaning are the foundation. Sealants on the chewing surfaces of back teeth and high-fluoride products help higher-risk patients.