Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker , Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | Vegetating pemphigus, pemphigus vegetans (Neumann type and Hallopeau type are the two recognised forms) |
How urgent? | 🔴 See a dentist or dermatologist promptly, it's a variant of a serious autoimmune blistering disease that needs systemic treatment |
Common or rare? | Very rare, it is the least common subset of pemphigus vulgaris |
Who it affects | Adults, most often in the fourth to fifth decades, with a slight predilection for people of Mediterranean, Jewish or South Asian heritage |
Who treats it | Specialist team, a dermatologist or oral medicine specialist usually leads care, with your general dentist supporting oral health |
Based on | Regezi, Neville, Cawson, Laskaris |
What is it?
Pemphigus vegetans is a rare form of pemphigus vulgaris, an autoimmune blistering disease of the skin and mucous membranes. Instead of leaving flat raw ulcers like classic pemphigus vulgaris, the healing skin and mouth lining (mucosa) here pile up into thickened, warty, vegetating plaques. These tend to favour body folds such as the groin and armpits, and around the mouth they often appear at the corners of the lips and on the gums.
Who tends to get it?
Pemphigus itself is uncommon, with around one to five new cases per million people each year (very rare, fewer than the chance of being struck by lightning in a year for many populations), and pemphigus vegetans makes up only a small fraction of those. Most people are diagnosed in their forties or fifties, although it can appear in any adult age group. Some reports suggest a slight female predilection, and there's a recognised increase in pemphigus among people of Mediterranean, Jewish, South Asian and Middle Eastern background. Childhood cases exist but are unusual.
Two patterns are described in the literature, named after the doctors who first described them. The Neumann type begins much like classic pemphigus vulgaris, with flaccid blisters that rupture and then heal with vegetating, warty plaques, it tends to be the more severe form. The Hallopeau type is milder, often starting with grouped pustules rather than blisters, and frequently shows a better long-term course.
What causes it?
Pemphigus vegetans shares the same underlying cause as pemphigus vulgaris. It is an autoimmune disease, which means the body's immune system mistakenly produces antibodies (called IgG autoantibodies) that target its own tissue. In this case, the target is desmoglein 3, a protein that acts like a tiny rivet holding skin and mucosal cells together.
The trigger that sets this autoimmune reaction off is usually unknown. Genetic and ethnic factors clearly play a role, with certain tissue-typing markers (HLA types — genetic markers used to match tissue compatibility) more common in affected people. Some medications can occasionally bring on a pemphigus-like eruption, including penicillamine, captopril and other ACE inhibitors, penicillins, cephalosporins, rifampin and non-steroidal anti-inflammatory drugs. Pemphigus is also more often seen alongside other autoimmune conditions such as myasthenia gravis, lupus, rheumatoid arthritis, Hashimoto's thyroiditis and Sjögren's syndrome.
How does it develop?
Think of skin and mucosa as a wall built from cells stacked together with tiny rivets called desmosomes. In pemphigus, the immune system attacks one of the proteins that makes up those rivets (desmoglein 3). Once the rivets fail, the cells in the deep layers of the surface lining (epithelium) drift apart, a process called acantholysis (the surface skin cells lose their connections to one another), and a fragile blister forms just above the basal layer (the bottom row of the surface lining).
In classic pemphigus vulgaris that's where the story tends to stop: the blister bursts and leaves a painful raw ulcer. In pemphigus vegetans the body's healing response goes a step further. After the initial blister or pustule ruptures, the surface epithelium piles up rather than re-flattening, producing a thickened, cauliflower-like growth. Under the microscope these vegetating plaques contain little pockets of inflammatory cells called eosinophilic abscesses (small pockets of immune cells called eosinophils), which are characteristic of this variant.
What might you notice?
What it looks like
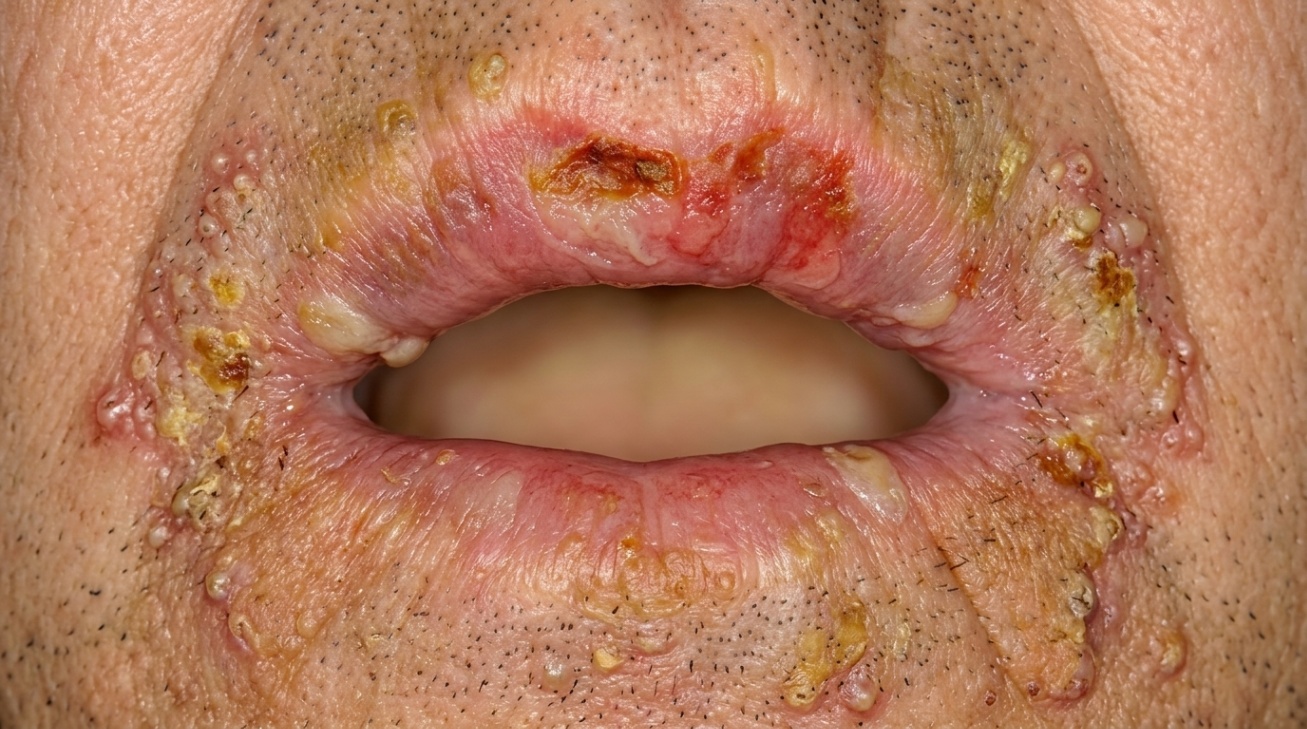
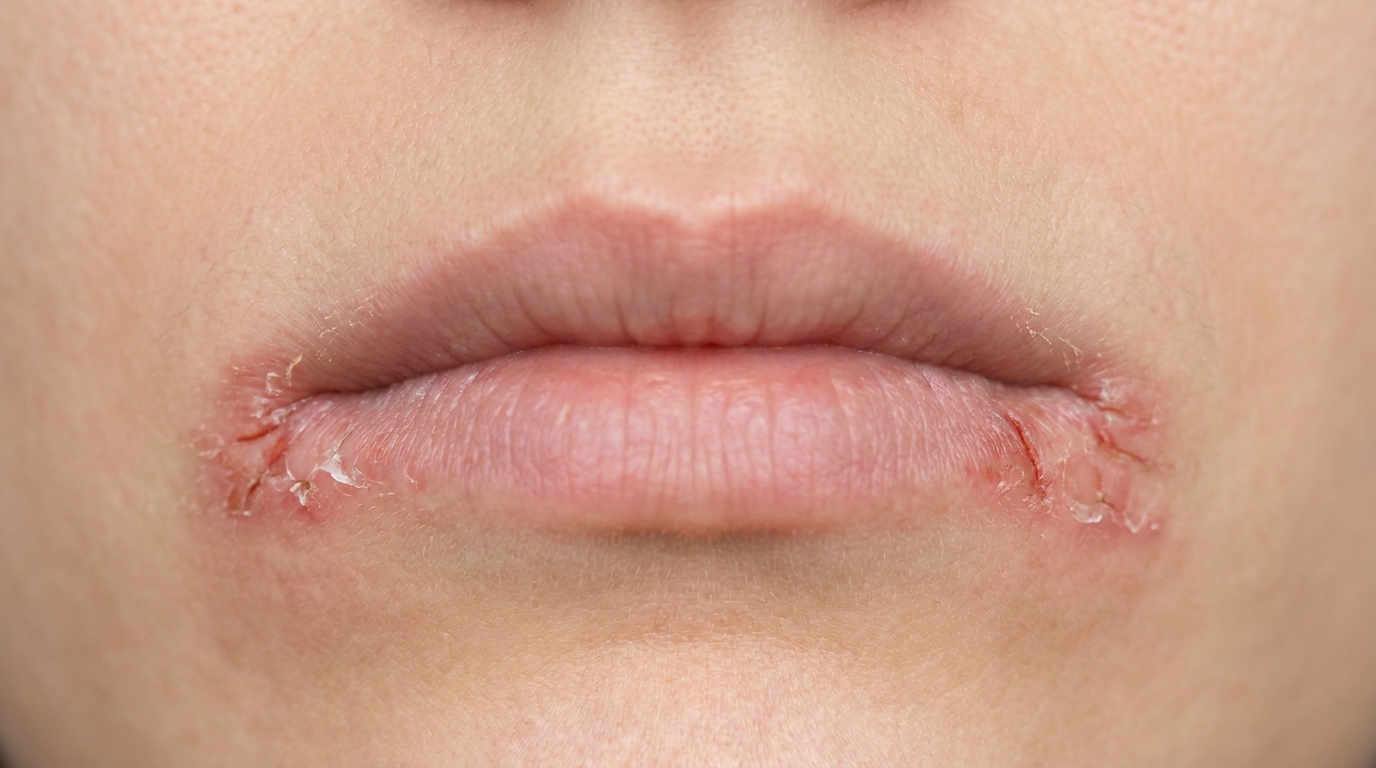
The earliest changes can look like ordinary pemphigus, soft, easily-popped blisters or, in the Hallopeau form, grouped pustules. Where it differs is what happens next. The raw areas don't heal smoothly. Instead they thicken into pink or skin-coloured warty plaques, sometimes with a moist or pus-filled surface. These vegetating lesions favour skin folds where moisture and friction are highest: the groin, the armpits, under the breasts, and around the eyes and nose.
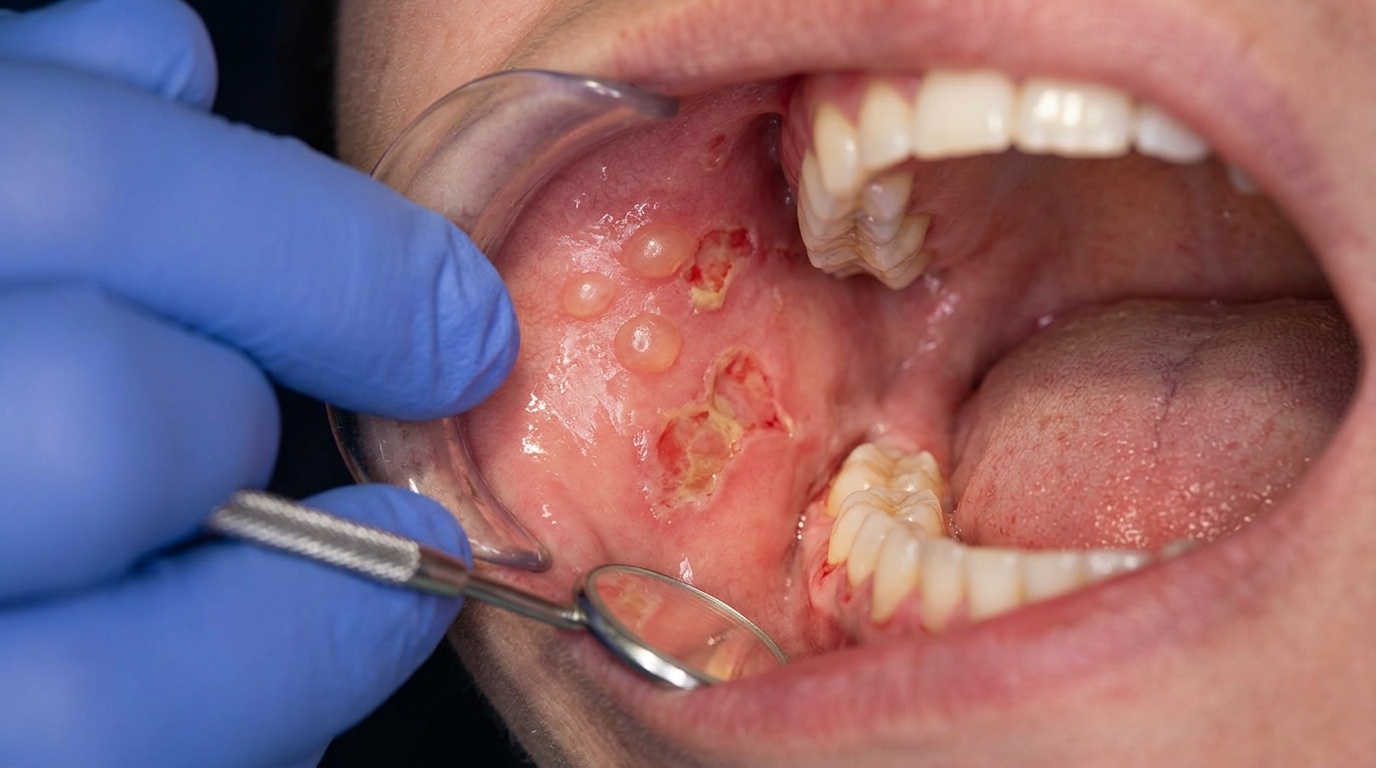
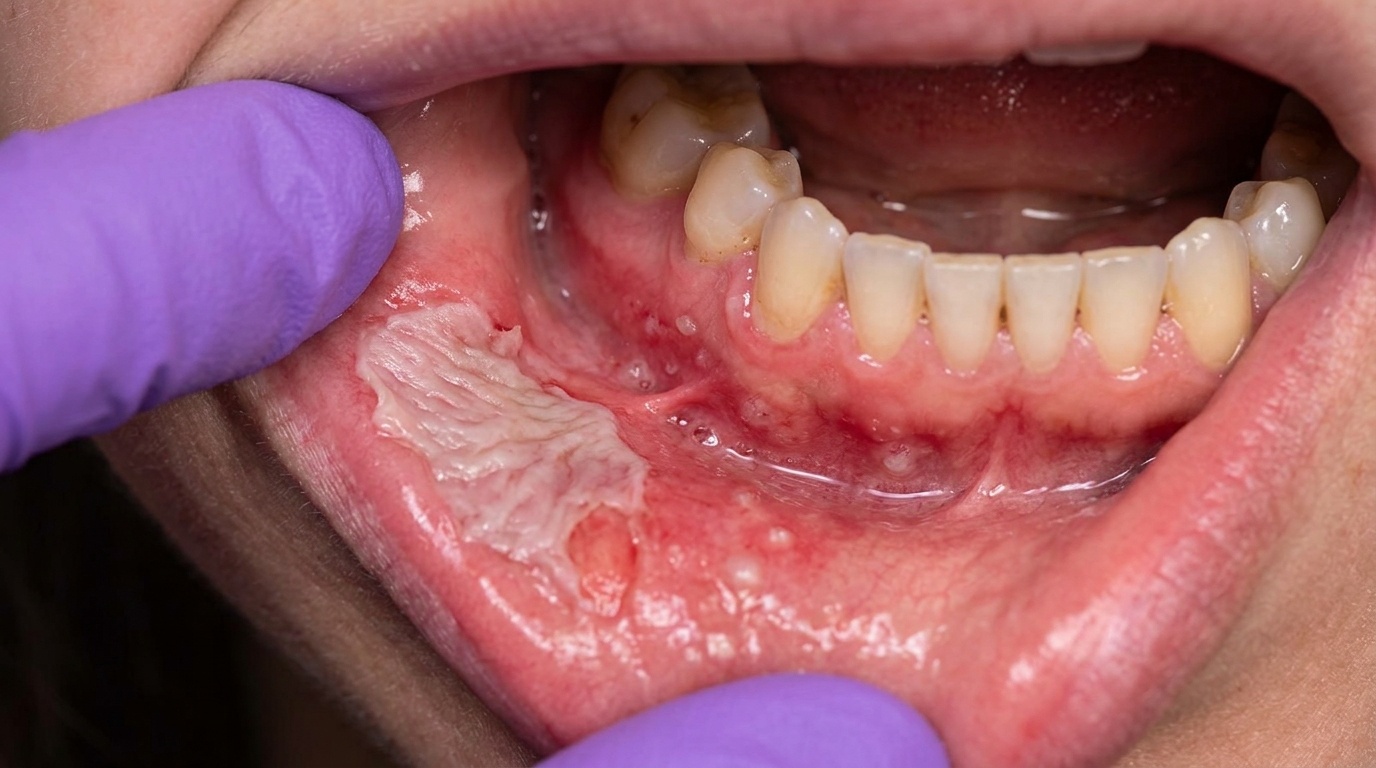
In the mouth, the lesions tend to appear at the angles (corners) of the lips and along the vermilion border (the lip's red edge), and may also affect the gums, buccal mucosa (cheek-side lining) and palate. Rather than the flat, ragged erosions of classic pemphigus vulgaris, oral pemphigus vegetans can produce raised, granular or papillomatous (warty) plaques. Gentle stroking of the surrounding mucosa may dislodge the upper layer of epithelium, a finding called a positive Nikolsky sign (the surface lining slides off when gently rubbed).
What it feels like
Oral lesions are usually painful and tender. Eating, brushing and speaking can all aggravate the soreness, and severe involvement may make swallowing difficult. Skin lesions in body folds may be itchy, sticky or malodorous because moisture and bacteria collect in the crevices. Some people develop a low-grade fever or feel generally unwell during flare-ups.
What an X-ray might show
X-rays don't help diagnose pemphigus vegetans, it is a soft-tissue condition and dental imaging looks normal. Diagnosis depends on clinical examination and tissue biopsy (a small tissue sample sent to the lab for testing) rather than imaging.
What happens at the dentist?
If your dentist at ArtSmiles sees suspicious lesions inside the mouth or at the corners of the lips, they will usually arrange a referral to an oral medicine specialist or dermatologist. The diagnosis is confirmed by combining clinical examination with a biopsy.
Because pemphigus is a body-wide disease (systemic disease), your dentist works alongside the medical team. Their role includes managing oral hygiene during flare-ups, checking for thrush (a common side effect of corticosteroid therapy), and making sure dental procedures don't trigger fresh lesions through trauma.
Is this serious?
🔴 Yes, pemphigus and its vegetans variant should always be taken seriously. Untreated pemphigus historically carried a mortality rate of 60,90%, mostly from infection, dehydration and electrolyte loss through widespread skin breakdown. With modern treatment that figure has fallen to roughly 5,10%, and most of the remaining risk relates to side effects of long-term immunosuppressive medication rather than the disease itself.
Pemphigus vegetans tends to behave like pemphigus vulgaris overall, but with two notable differences. The Hallopeau subtype generally runs a milder course, and spontaneous remission with complete recovery has been reported, something that's distinctly unusual in classic pemphigus vulgaris. The Neumann subtype is more severe and behaves much like ordinary pemphigus vulgaris.
If you've noticed any of these signs for more than two weeks, it's worth booking an assessment.
Could it be something else?
Several other oral and skin conditions can produce blisters, ulcers or warty plaques that overlap with pemphigus vegetans. The textbooks list the following differentials:
Pemphigus vulgaris, the parent disease, with the same blistering and Nikolsky sign. A dentist or pathologist tells them apart by the warty, vegetating quality of the healing lesions and the eosinophilic abscesses seen on biopsy in vegetans.
Paraneoplastic pemphigus, also produces severe oral ulceration and skin lesions, but is associated with an underlying lymphoma or other malignancy, and immunofluorescence shows antibody deposits both between cells and along the basement membrane (the thin layer that anchors the surface skin to the connective tissue beneath).
Mucous membrane pemphigoid (cicatricial pemphigoid), also causes blisters and desquamative gingivitis, but the split is below the epithelium rather than within it, and the autoantibody targets the basement membrane zone.
Bullous pemphigoid, predominantly a skin disease in the elderly, with subepithelial blisters; oral involvement is rare.
Erosive lichen planus, can cause persistent oral erosions and desquamative gingivitis, but typically shows white striae and a band of lymphocytes on biopsy rather than acantholysis.
Erythema multiforme, produces crusted, bleeding lips and irregular oral erosions, but is acute, often triggered by herpes or drugs, and shows target lesions on the skin rather than vegetating plaques.
Recurrent herpes simplex infection, can give crusted lip lesions but heals within a couple of weeks and shows a different pattern on viral testing.
Aphthous ulcers, recurrent painful round ulcers, but they lack vesicles, lack a positive Nikolsky sign and resolve within one to three weeks.
Dermatitis herpetiformis, itchy blistering skin disease, distinguished by IgA deposits at the dermal papillae (small bumps in the upper layer of skin) and association with coeliac disease.
Linear IgA disease, subepithelial (under the surface lining) blistering with linear IgA along the basement membrane on immunofluorescence.
IgA pemphigus, rare; produces skin pustules with IgA rather than IgG autoantibodies.
Pemphigus foliaceus and pemphigus erythematosus, superficial pemphigus variants that target desmoglein 1 and rarely involve the mouth.
Hailey,Hailey disease (chronic benign familial pemphigus), a genetic condition that causes erosive lesions in skin folds; oral involvement is uncommon, and there are no circulating autoantibodies.
Condyloma acuminatum and verruca vulgaris, warty skin and mucosal lesions caused by HPV (human papillomavirus) that may resemble vegetating plaques but are viral and don't produce blisters or acantholysis.
Focal epithelial hyperplasia (Heck disease), multiple soft, papillomatous oral plaques caused by HPV, distinguished on biopsy.
Amyloidosis, can rarely cause oral blisters and erosions, distinguished by Congo-red staining (a special stain used to identify amyloid) of the tissue.
How is it treated?
Pemphigus vegetans is a systemic disease, so treatment must be systemic too. Topical measures alone are not enough. Care is usually shared between a dermatologist or oral medicine specialist and your general dentist.
First-line treatment has traditionally been a systemic corticosteroid such as prednisone or prednisolone. Typical regimens use an intermediate to high dose to bring the disease under control, followed by a slow taper to the lowest effective maintenance dose. Because long-term steroid use can cause weight gain, raised blood sugar, osteoporosis, mood changes, peptic ulcers and increased infection risk, a steroid-sparing immunosuppressant (drug that dampens down the immune system) is usually added in. Options listed in the textbooks include:
Azathioprine
Mycophenolate mofetil
Cyclophosphamide
Cyclosporine
Dapsone
More recent regimens often start with rituximab, a monoclonal antibody that targets the B-cells responsible for producing the autoantibodies. Rituximab combined with a lower dose of corticosteroid is now widely used and produces faster, more durable remissions. For severe or unresponsive disease, options include intravenous immunoglobulin (IVIg, antibody preparation given through a drip), plasmapheresis (a procedure that filters harmful antibodies from the blood) and immunoadsorption (a procedure that removes specific antibodies from the blood).
Alongside systemic therapy, dental care focuses on:
Gentle oral hygiene to keep gums healthy without traumatising fragile mucosa
Soft-bristled toothbrushes and bland toothpastes
Antifungal therapy if oral thrush develops as a side effect of steroid use
Avoiding hard, sharp or spicy foods during flare-ups
Treating dental infections promptly and gently, to avoid triggering new lesions
Ideally, treatment is monitored by a clinician experienced in immunosuppressive therapy, with periodic blood tests to track autoantibody levels and watch for medication side effects.
What's the long-term outlook?
With modern treatment, the outlook for pemphigus vegetans has improved dramatically. The Hallopeau subtype has the more favourable course, with spontaneous remission and complete recovery reported in some cases, a feature that distinguishes it from classic pemphigus vulgaris. The Neumann subtype tends to behave like pemphigus vulgaris itself: a chronic disease with periods of remission and relapse that usually requires lifelong, low-dose maintenance therapy.
One large series found that up to three-quarters of pemphigus vulgaris patients achieved disease resolution after 10 years of treatment, although most centres have historically reported sustained remission rates of around 30 per cent. Mortality, once 60,90 per cent, is now around 5,10 per cent, and that figure is expected to fall further as B-cell-targeted therapies become more widely used.
The oral lesions of pemphigus are sometimes described as "the first to show, and the last to go", they often appear before the skin disease and may persist after the skin has cleared. That makes ongoing dental review an important part of long-term care, both for monitoring the disease and for protecting your overall oral health while on immunosuppressive treatment.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
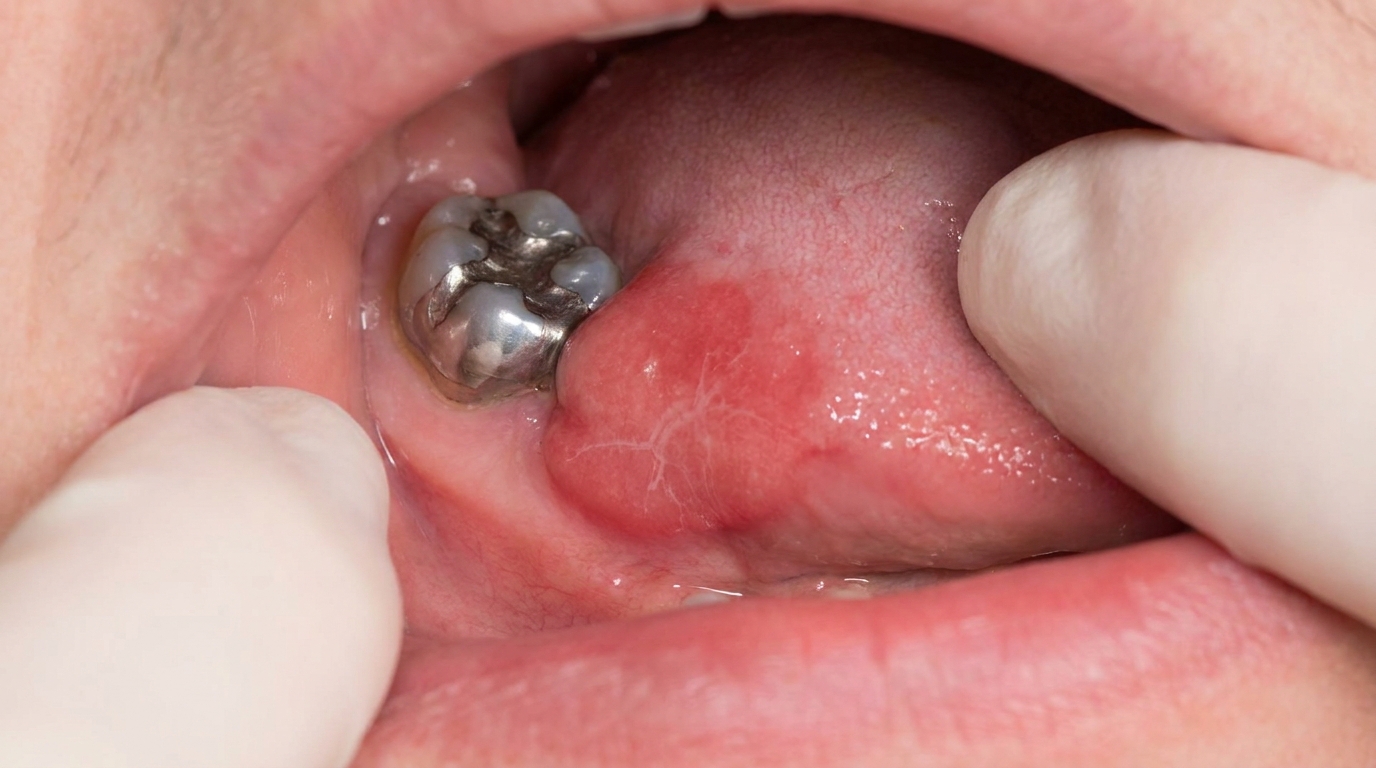
The cover image above is an AI-generated illustration based on the most common visible features of this condition described in clinical pathology references. It is not a photograph of a real case and should not be used to diagnose or rule out the condition in your own situation. If you are concerned about something you have noticed, please book an assessment with a registered dental practitioner.
References
Regezi, J. A., Sciubba, J. J., & Jordan, R. C. K. (2017). Oral pathology: Clinical pathologic correlations (7th ed.). Elsevier. Chapter 1, Vesiculobullous Diseases (Pemphigus Vulgaris and Pemphigus Vegetans), pp. 11,16.
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2023). Oral and maxillofacial pathology (5th ed.). Elsevier. Chapter 16, Dermatologic Diseases (Pemphigus), pp. 768,774.
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 13, Diseases of the Oral Mucosa: Non-infective Stomatitis (Pemphigus Vulgaris and Pemphigus Variants), pp. 232,243.
Laskaris, G. (2003). Color atlas of oral diseases (3rd ed.). Thieme. Chapter 22, Skin Diseases (Pemphigus Vegetans), pp. 202,204.