Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker , Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | Cracked tooth, incomplete tooth fracture, cuspal fracture |
How urgent? | 🟡 Worth checking soon, the crack tends to extend over time and may eventually reach the nerve, infect or split the tooth |
Common or rare? | Common in adults, particularly in heavily restored back teeth |
Who it affects | Adults, especially those with large fillings, those who grind or clench their teeth, and those with a history of biting on hard objects |
Who treats it | General dentist, treatment ranges from a protective onlay (a tooth-shaped cap that covers part of the chewing surface) or crown to root canal treatment or extraction depending on the depth of the crack |
Based on | Cawson, with cross-references in Neville |
What is it?
Cracked tooth syndrome is the cluster of symptoms caused by a fine, often invisible, crack running through a tooth. Most commonly the crack runs from the chewing surface of a back tooth down toward the root, dividing one cusp (the pointed part of the chewing surface) from the rest of the tooth. The crack may not yet have separated the tooth into two pieces, but each time the patient bites, the two halves move slightly against each other and irritate the dentine (the hard layer under the enamel) and pulp (the soft nerve and blood vessel core of the tooth). The result is a typically sharp, brief pain that puzzles patients because nothing looks broken in the mirror.
Who tends to get it?
The textbooks describe cracked tooth most often in adults, particularly:
People with heavily restored teeth, Cawson specifically notes that restored premolars (the two teeth between the canines and molars) are particularly prone to splitting under chewing forces. Large fillings weaken the surrounding tooth structure.
People who grind or clench their teeth (bruxism), repeated heavy loading of cusps creates fatigue cracks.
People who bite on hard or unexpected objects, popcorn kernels, ice, olive pits, bones, or hard nuts can be the trigger event.
Older teeth, like other materials, enamel and dentine become slightly more brittle with age.
Posterior teeth, particularly lower molars and upper premolars (the back teeth in each jaw), the way these teeth are loaded during chewing concentrates stress on individual cusps.
There is no strong sex predilection in the textbooks. The condition is uncommon in children whose teeth are largely intact.
What causes it?
A crack appears when forces on a tooth exceed its capacity to withstand them. The textbooks list these contributing factors:
Masticatory stress, repeated heavy chewing, especially on a tooth weakened by a filling or a deep groove.
Sudden hard biting, a single bite on something unexpectedly hard can split a cusp.
Existing fillings, particularly large, wedge-shaped restorations that act like a splitting force on the surrounding tooth.
Bruxism (clenching and grinding), generates very high cyclic loads on cusps and is a recognised driver of crack formation.
Steep cusps and unfavourable bite contacts, focus the load on a small area.
Pre-existing weakness, for example, a previously root-filled tooth that has not been protected with a crown or onlay.
How does it develop?
A microscopic crack starts at a point of stress concentration on the tooth, often a deep groove or the edge of a filling. With each bite, the crack extends a little further, sometimes only by a fraction of a millimetre. As the crack reaches the dentine, it begins to flex when the tooth is loaded, allowing fluid and bacteria to move within the dentinal tubules, the tiny channels that connect the tooth surface with the pulp. The pulp interprets this as a stimulus and produces the characteristic sharp pain on biting. Cawson notes that "minute cracks are often invisible, but allow bacteria into the pulp chamber", meaning that, over time, an undetected crack can lead to inflammation of the pulp (pulpitis) and eventually death of the nerve, even if the tooth still looks intact from the outside.
What might you notice?
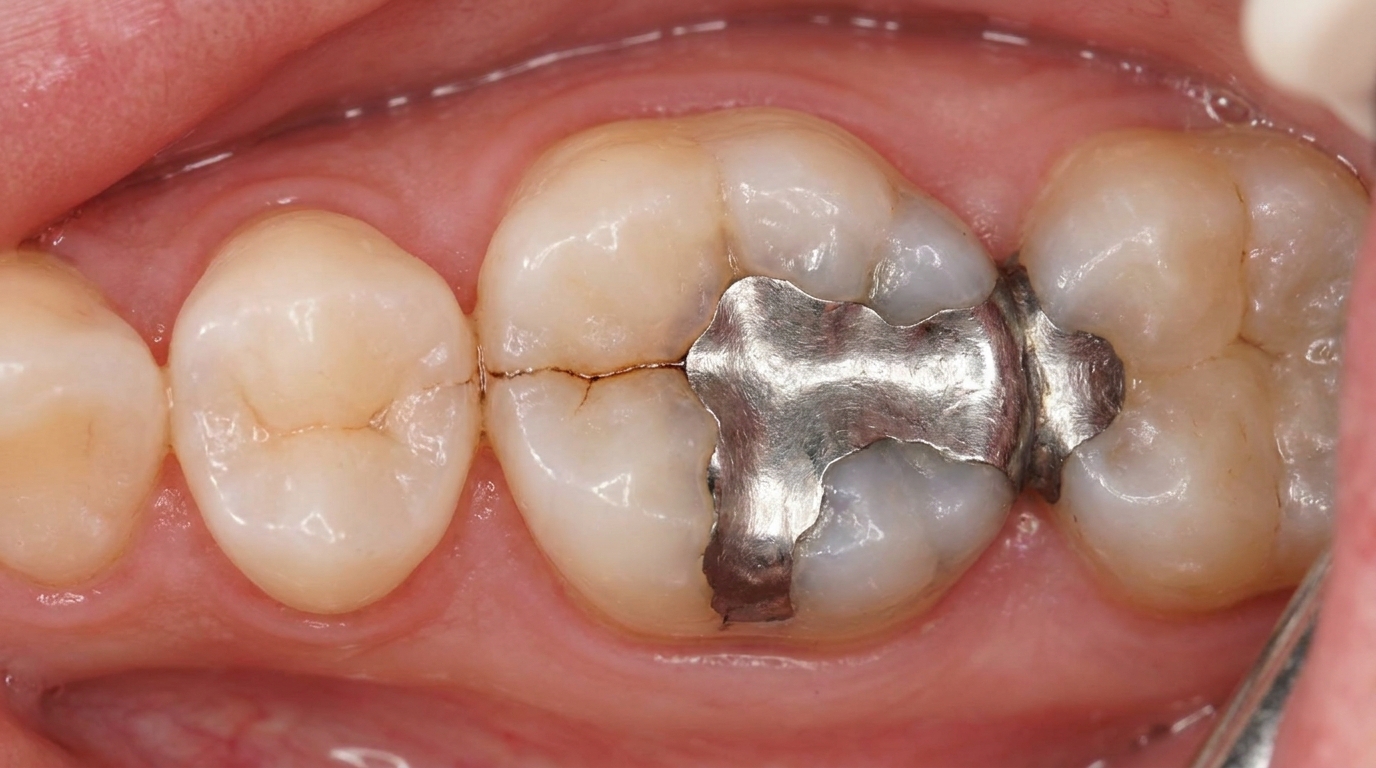
What it looks like
Often, nothing obvious. The tooth may look completely normal in the mirror. Sometimes a fine line is visible across a cusp or along a groove, particularly when light is angled across the surface. There may also be a large filling or an old restoration nearby.
What it feels like
The classic pattern of cracked tooth symptoms is fairly distinctive:
Sharp pain on biting, especially on certain foods (typically firm, fibrous, or grainy textures), or on biting in a particular direction. The pain often happens as you release the bite, when the two halves of the cracked cusp spring back into place.
Brief sensitivity to cold, a stab of pain that disappears within seconds. (Persistent throbbing pain that lingers suggests the pulp is now irreversibly inflamed.)
Difficulty pinpointing which tooth is causing the pain. Pulpal pain is poorly localised, and patients often struggle to identify the offending tooth, sometimes pointing to the wrong jaw.
Pain that comes and goes, sometimes for months, before becoming more constant.
What an X-ray might show
X-rays are often unhelpful for cracked tooth syndrome. Hairline cracks usually run through the tooth in a direction the X-ray beam cannot capture, so the radiograph looks normal even when a significant crack is present. X-rays are mainly useful for ruling out other causes of toothache (caries, abscess) and for checking the bone around the root.
What happens at the dentist?
Diagnosing a cracked tooth is one of the more detective-style examinations in dentistry. A dentist at ArtSmiles will typically:
Take a careful history of when the pain started, what triggers it, and which side of the mouth it affects.
Examine the suspected teeth for visible cracks, large fillings, worn cusps, or signs of bruxism.
Apply pressure to individual cusps with a small tool such as a Tooth Slooth or a ball-ended burnisher, asking the patient to bite and release. Pain on release of the bite is a classic indicator. Cawson specifically describes this technique.
Use oblique transillumination (shining a bright light through the tooth so a crack appears as a dark line), shining a bright fibre-optic light across the tooth so that any crack appears as a dark interruption in the light. Cawson notes this can also be done with the help of a fluorescein dye (a special dye that glows under ultraviolet light) and ultraviolet light.
Test the pulp with cold or electric pulp testing to gauge how inflamed the nerve is.
Take a bite-wing radiograph to rule out caries and check the bone.
Check for grinding or clenching patterns and discuss any associated jaw discomfort.
If a tooth has already been heavily restored, the dentist may need to remove the existing filling and look directly into the cavity, where the crack is often visible as a dark line stained with dentinal fluid.
Is this serious?
🟡 A cracked tooth is rarely dangerous in the short term, but it does tend to progress. Cracks usually do not heal, they extend a little further with each chewing cycle. If the crack reaches the pulp, root canal treatment may be needed; if it reaches below the gum line and into the root, the tooth may not be restorable. Catching the crack early is the difference between a protective onlay or crown and a more involved procedure.
If a single tooth has been giving you sharp pain on biting or cold sensitivity for more than a couple of weeks, it's worth booking an assessment so the cause can be identified before the crack extends.
Could it be something else?
Several conditions can produce similar pain patterns. The textbooks list these as the main differentials:
Dental caries (tooth decay) with reversible pulpitis, also produces sensitivity to cold and sweet foods, but a visible cavity or X-ray finding usually identifies it.
Defective restoration, an old filling with a leaky margin can mimic a crack, with similar cold sensitivity and biting pain.
Reversible pulpitis from a recently placed deep filling, typically settles within a few weeks of the procedure.
Periapical periodontitis (inflammation around the root tip from a dead pulp), produces tenderness on tapping the tooth and pain on biting, but the tooth has usually died and there are radiographic changes around the root.
Periodontal abscess, pain on biting from infection in the gum, usually with swelling and a deep gum pocket.
Dentine sensitivity from exposed root surfaces, sensitivity to cold but not sharp pain on biting, and usually affects multiple teeth at the gum line.
Sinus-related pain, upper back tooth pain from sinusitis can be confused with a cracked tooth, but usually involves multiple upper teeth and changes with head position.
How is it treated?
Treatment depends on how deep the crack is, whether the pulp is involved, and whether the tooth is restorable. Options range from conservative protection to root canal treatment or, in severe cases, extraction.
At-home measures that may help in the short term:
Avoid chewing on the affected side while you wait for an appointment.
Avoid hard or sticky foods that might extend the crack, nuts, ice, hard lollies, popcorn kernels.
Use a soft diet for a few days if the tooth is very tender.
Treat any clenching or grinding habit if you are aware of it, a custom night splint may be recommended.
Professional steps your dentist may consider:
A protective onlay or crown, when the crack is limited to enamel and superficial dentine, a well-fitting onlay or full crown that holds the cusps together is usually the most effective long-term solution.
Replacing the existing filling with a strongly bonded composite restoration that splints the cusps together, in selected cases.
Root canal treatment if the pulp has become irreversibly inflamed or has died, followed by a crown to protect the tooth.
Extraction if the crack extends below the gum line into the root, splits the tooth into two pieces, or compromises the long-term outlook beyond repair. Modern replacements such as dental implants or bridges can then restore function.
Bite adjustment to redistribute chewing forces away from the affected cusp.
Night splint for patients with bruxism, to reduce the cyclic load that drove the crack in the first place, a step that also protects neighbouring teeth.
A patient-centred approach matters. Many people with cracked tooth syndrome have spent months unsure what is causing their pain, and a careful, unhurried assessment is itself part of effective care, values that sit at the heart of our clinical philosophy.
What's the long-term outlook?
The outlook depends on how early the crack is caught. Cracks confined to the crown that are protected with an onlay or crown often have an excellent long-term prognosis. Cracks extending into the pulp can usually be saved with root canal treatment plus a crown, although the tooth is then more brittle and continues to need protection. Cracks extending into the root, or splitting the tooth completely, generally cannot be repaired and the tooth will need to be replaced. The key drivers of outcome are early detection, protection of the cusps, and addressing any underlying cause such as bruxism.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
The cover image above is an AI-generated illustration based on the most common visible features of this condition described in clinical pathology references. It is not a photograph of a real case and should not be used to diagnose or rule out the condition in your own situation. If you are concerned about something you have noticed, please book an assessment with a registered dental practitioner.
References
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 4, Pulpitis, Apical Periodontitis, Resorption and Hypercementosis: cracked tooth as a cause of pulpitis, detection by ball-ended burnisher pressure, oblique transillumination and fluorescein/UV, pp. 59 to 66.
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 4, Summary chart 4.2 Diagnosis of pulpal, periodontal and other pain in the teeth and alveolus: cracked tooth or cusp distinguished from caries, periapical periodontitis and periodontal abscess.
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2023). Oral and maxillofacial pathology (5th ed.). Elsevier. Chapter on Pulpal and Periapical Disease: cracked tooth associated with the reversible pulpitis pattern of pain, pp. 117 to 118.