Gum disease does not always get louder as it gets worse. In many cases, it becomes quieter. That is what makes it dangerous.
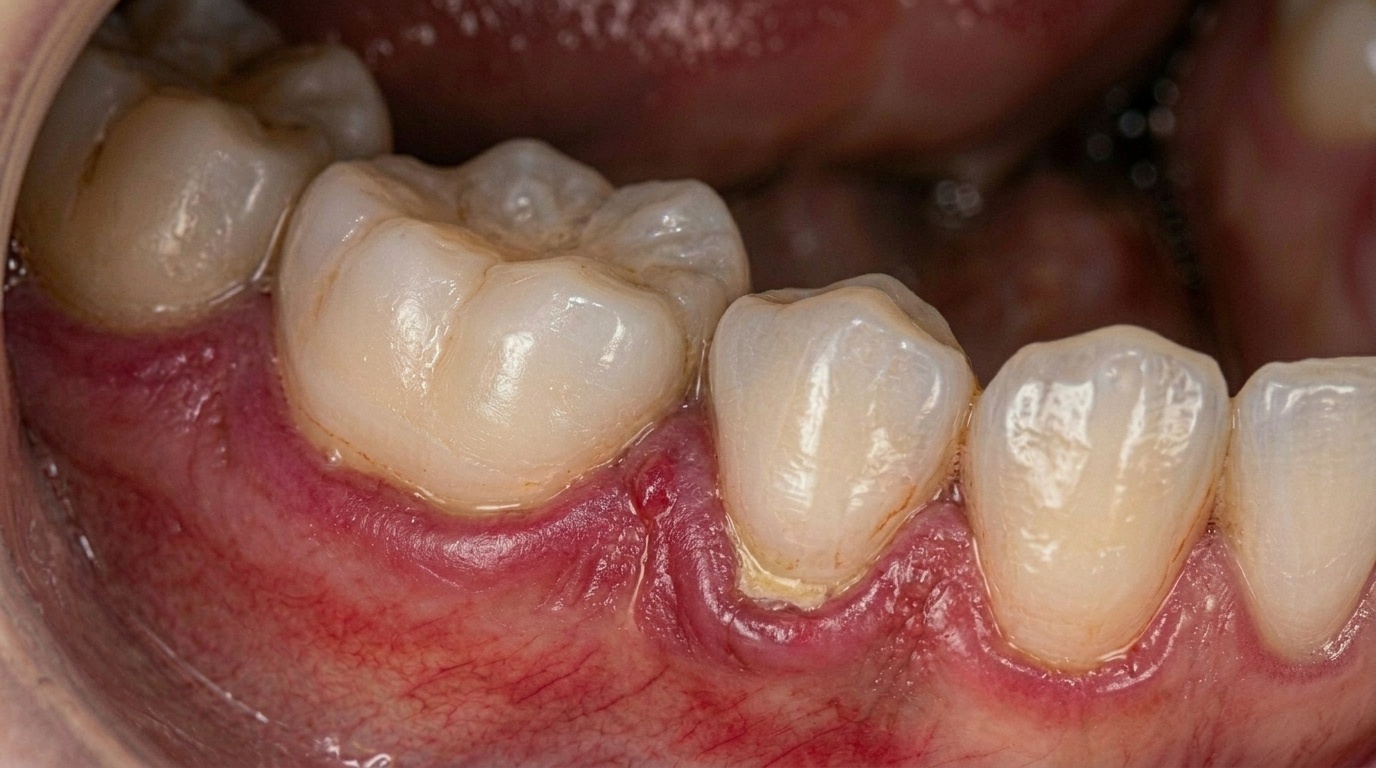
In the early stages, gum disease sends clear signals. Gums bleed when you brush. They feel sore or swollen. Sometimes they look red or irritated. These signs are uncomfortable, but they are also helpful. They are your body's way of asking for attention.
As the condition progresses, those warning signs can fade. Bleeding may stop. Tenderness may disappear. Everything can feel calm on the surface, while the structures that support your teeth continue to break down underneath.
By the time teeth begin to feel loose or bad breath becomes persistent, the damage is often already advanced.
If you have noticed changes in your gums, or if it has been a while since your last dental check-up, this article will help you understand what may be happening and when to act.
Table of Contents
Why Gum Disease Can Feel Better as It Gets Worse
In its earliest stage, known as gingivitis, gum disease is very reactive. The gums respond strongly to plaque build-up. They swell, bleed easily, and feel sensitive. Because this stage affects only the surface tissues, the symptoms tend to be noticeable. Research by Löe et al. (1965) first demonstrated how quickly gingivitis develops once plaque is left undisturbed.
If plaque and hardened calculus remain in place, inflammation gradually moves deeper. This is when gingivitis progresses into periodontitis.
Here is the part most people do not expect: periodontitis is usually painless.
Bone has no pain receptors. As the infection shifts from the gums to the bone that supports the teeth, the body no longer sends the same warning signals. Bleeding and tenderness may reduce, even though damage continues. This is why periodontal disease is often described as a silent condition in dental research (Page & Schroeder, 1976). The absence of pain does not mean the absence of disease.
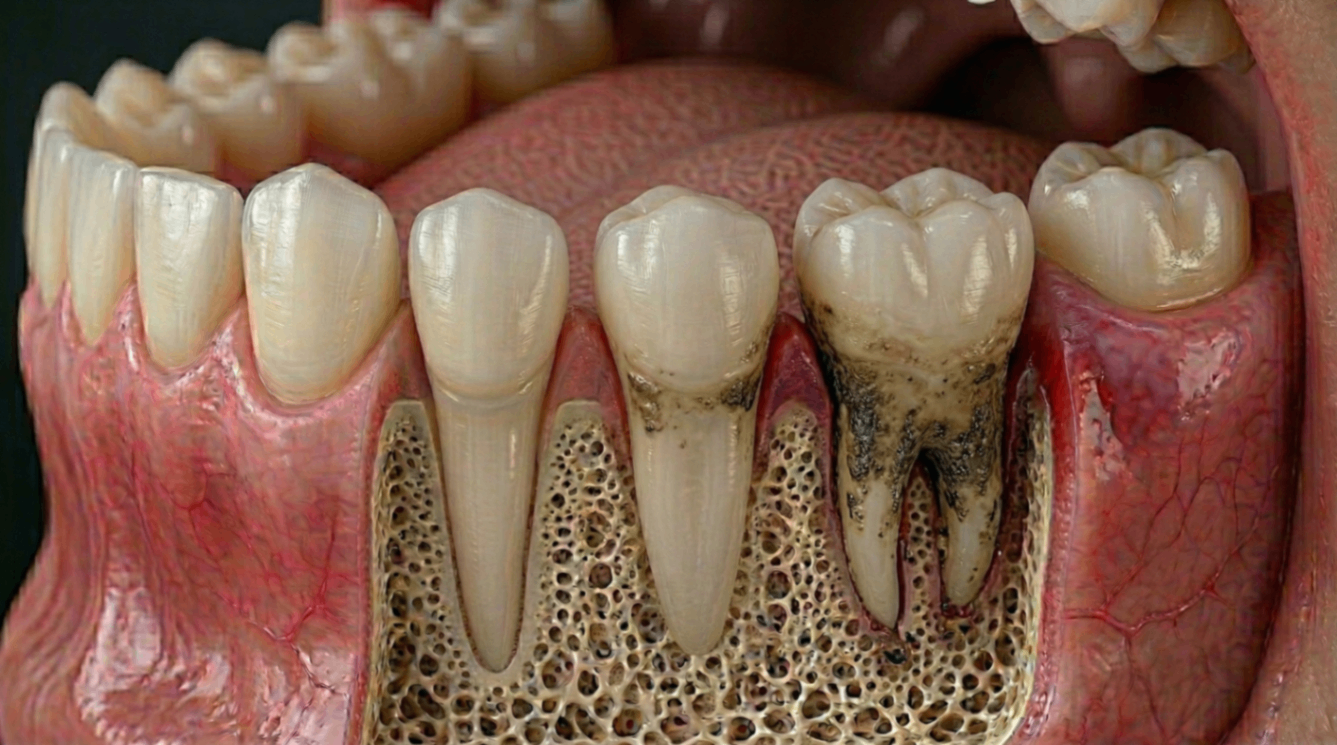
What Is Really Happening Beneath the Gumline
Once bacteria move below the gumline, they settle into an environment that is difficult to clean and easy for harmful bacteria to thrive. Over time, several things happen at once (Socransky & Haffajee, 2005):
Bacteria form a sticky biofilm under the gums
Calculus hardens onto the tooth roots
The immune system stays permanently activated
Chronic inflammation causes the surrounding bone to slowly dissolve
Gum pockets deepen and become harder to reach with daily brushing
Teeth gradually lose their support
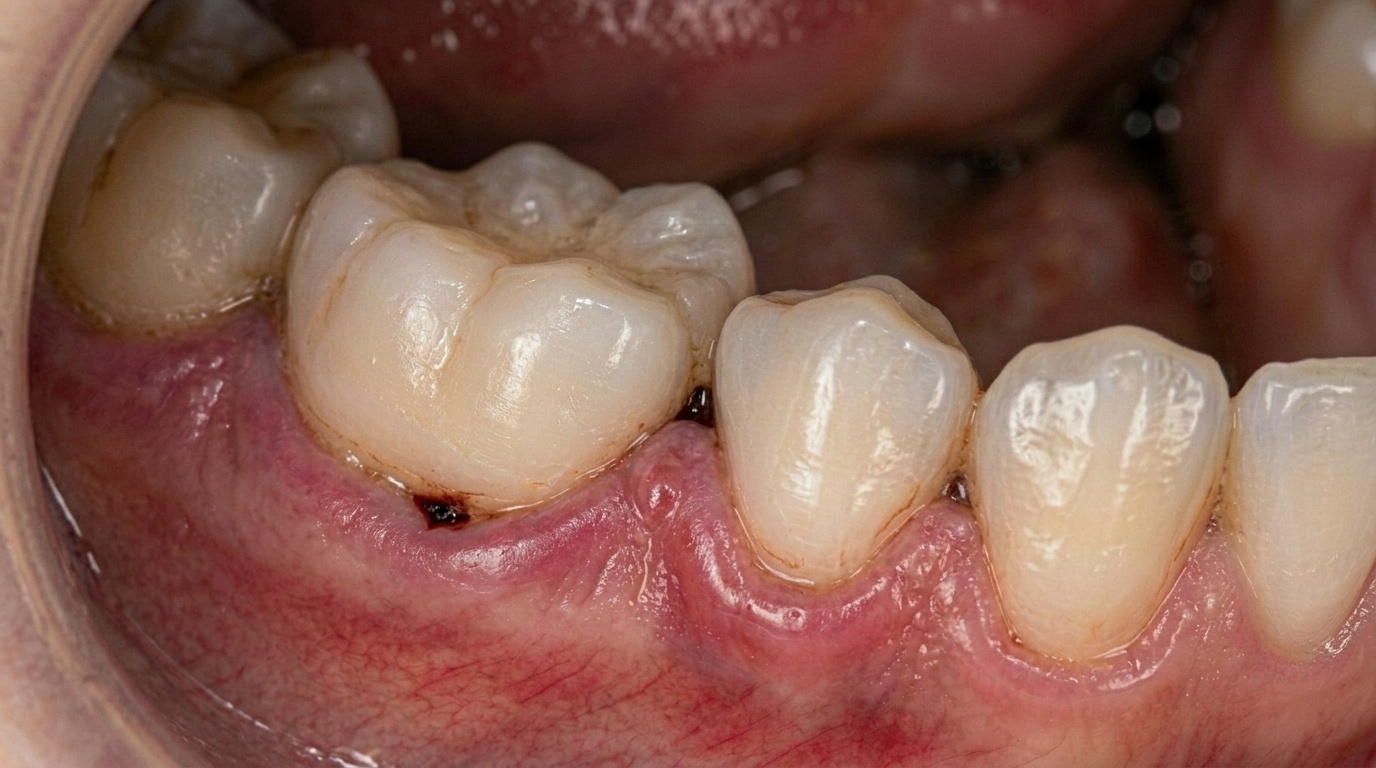
Most patients do not feel this process unfolding. Instead, they may notice subtle changes such as food getting trapped more easily, small gaps appearing, or gums slowly receding.
When Bleeding Stops but the Disease Has Not
One of the most common misconceptions is believing that gums are healthier because they no longer bleed.
Bleeding can stop even while periodontitis continues to progress. This can happen for several reasons:
You may unconsciously avoid brushing sensitive areas
The infection may have moved deeper where bleeding is not visible
The gum tissue can become less reactive over time
Smoking can reduce blood flow to the gums
The immune response can become blunted after years of inflammation
If bleeding has stopped but you notice gum recession, persistent bad breath, or changes in how your teeth feel, it is worth having your gums assessed. Clinical measurement of pocket depth remains one of the most reliable ways to detect ongoing disease (Listgarten, 1980).
Subtle Signs That Gum Disease Has Progressed
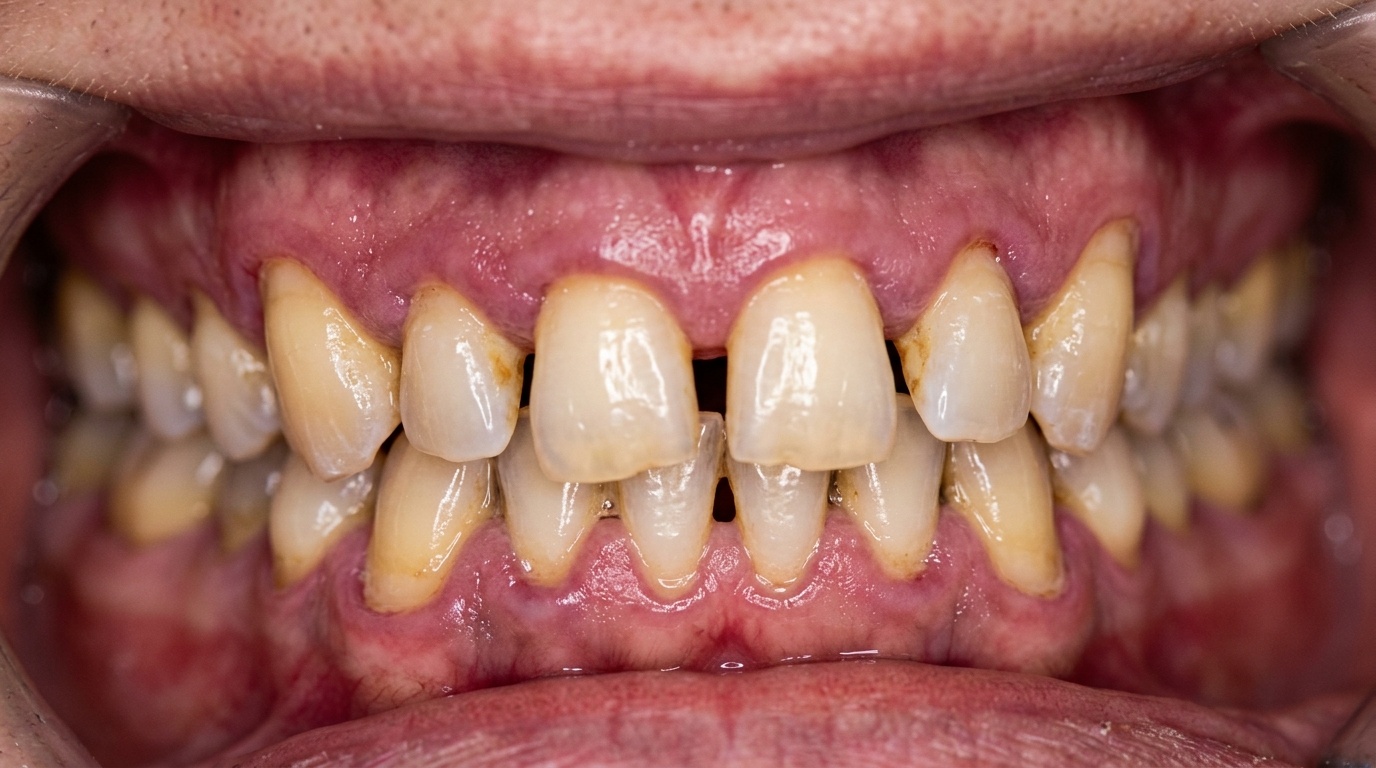
Advanced gum disease rarely announces itself with pain. Instead, it shows up in quieter ways:
Teeth may start to feel slightly loose
New spaces can appear between teeth
Bad breath may persist even with good hygiene (Quirynen et al., 2009)
Gums may recede, making teeth look longer
Food may lodge more often between teeth
Sensitivity can develop near the gumline
Your bite may feel different when you close your teeth together
These signs do not mean tooth loss is inevitable. When addressed early, further damage can often be slowed or stabilised. Modern classification systems now use staging and grading to assess how far the disease has progressed and how quickly it is likely to worsen (Tonetti et al., 2018).
Why Home Care Is Not Enough Once Disease Is Deep
Brushing and flossing are essential, but they cannot clean deep periodontal pockets.
Once calculus forms beneath the gums, professional treatment is required to remove it safely and thoroughly. Evidence confirms that scaling and root planing remains one of the most effective non-surgical treatments for periodontitis (Cobb, 2002).
At ArtSmiles, periodontal care usually includes:
A detailed gum assessment
Deep cleaning to remove bacterial build-up from below the gumline
Personalised home care guidance
Regular maintenance visits for patients with a history of gum disease
Deep cleaning allows the gums to heal, reduces inflammation, and helps prevent further bone loss.
What to Do If You Suspect Gum Disease Is Progressing
You do not need to wait for pain before taking action. Gum disease is far easier to manage when it is identified early (Armitage, 2004).
If you are concerned about your gums, the most important steps are straightforward:
Have a deep clean if pockets are detected
Use interdental brushes if recommended
Replace your toothbrush regularly
Maintain consistent professional reviews if you have had gum disease before
When bone loss is detected early, many teeth can be preserved for years with the right care.
Frequently Asked Questions About Gum Disease
Can gum disease be completely painless?
Yes. Periodontitis, the advanced form of gum disease, is often entirely painless. As the infection moves from the gums to the underlying bone, the body stops producing the same warning signals. Bone tissue has no pain receptors, which means significant damage can occur without causing any discomfort. This is why regular periodontal check-ups are so important, even when your gums feel fine.
Why did my gums stop bleeding?
Bleeding can stop for several reasons that are not necessarily signs of improvement. You may be avoiding brushing in tender areas, the disease may have moved deeper where it is no longer visible, the gum tissue may have become less reactive over time, or smoking may be reducing blood flow. Stopping bleeding does not mean gum disease has resolved. If you have noticed other changes such as recession or bad breath, a professional assessment is worthwhile.
What are the signs that gum disease is getting worse?
Gum disease that is progressing tends to show up through subtle changes rather than pain. These include teeth feeling slightly loose, new gaps appearing between teeth, persistent bad breath, gums pulling away from the teeth, food getting trapped more often, and your bite feeling different. If any of these sound familiar, early treatment can help slow further damage.
How often should I have gum checks if I have had gum disease before?
Most people who have had periodontitis benefit from maintenance visits every three to six months, rather than the standard annual or biannual check. This is because the bacteria that cause gum disease can recolonise within weeks. More frequent professional cleaning helps keep levels under control and gives your dentist the chance to detect any early signs of recurrence.
Can gum disease affect my general health?
Research has found links between periodontitis and a number of systemic conditions including cardiovascular disease, diabetes, and adverse pregnancy outcomes. The exact mechanisms are still being studied, but chronic inflammation from gum disease is thought to play a role. Managing your periodontal health is not just about protecting your teeth. It may also contribute to your overall wellbeing.
Understanding Your Next Steps
Gum disease does not behave the way most people expect. As it progresses, it often becomes quieter, not louder. The absence of pain is not reassurance — it is often a signal to look closer.
If you have noticed subtle changes in your gums, or if you simply want clarity about your oral health, a periodontal check can protect your smile before irreversible damage occurs.
To learn more or to book an appointment, visit ArtSmiles Gold Coast.
Written by Dr. Cristian Dunker, BDSc, MBA.
Medically reviewed by Dr. Cristian Dunker.