Occasional bad breath is normal — morning breath and food-related odour happen to everyone. But when bad breath keeps coming back despite brushing, flossing, and mouthwash, it usually points to something deeper going on inside the mouth.
Persistent bad breath, clinically known as halitosis, affects roughly 25–30% of the global population according to a review by Scully and Greenman (2012). It is rarely just a hygiene problem. In most cases, it is linked to bacterial build-up below the gumline, gum disease, untreated decay, dry mouth, or failing dental restorations.
Because many of these problems develop without pain, bad breath is often the first noticeable sign that something needs attention.
Where Does Chronic Bad Breath Come From?
Most chronic bad breath originates inside the mouth, not the stomach — despite what many people assume. Research by Yaegaki and Coil (2000) established that approximately 85–90% of halitosis cases have an oral source.
The primary culprits are anaerobic bacteria that break down proteins and release volatile sulphur compounds (VSCs). These gases — mainly hydrogen sulphide and methyl mercaptan — are responsible for the unpleasant smell.
These bacteria tend to accumulate in areas that are difficult to clean:
Deep gum pockets around the teeth
The back of the tongue
Between tightly spaced teeth
Around old fillings, crowns, or bridges
Inside deep cavities
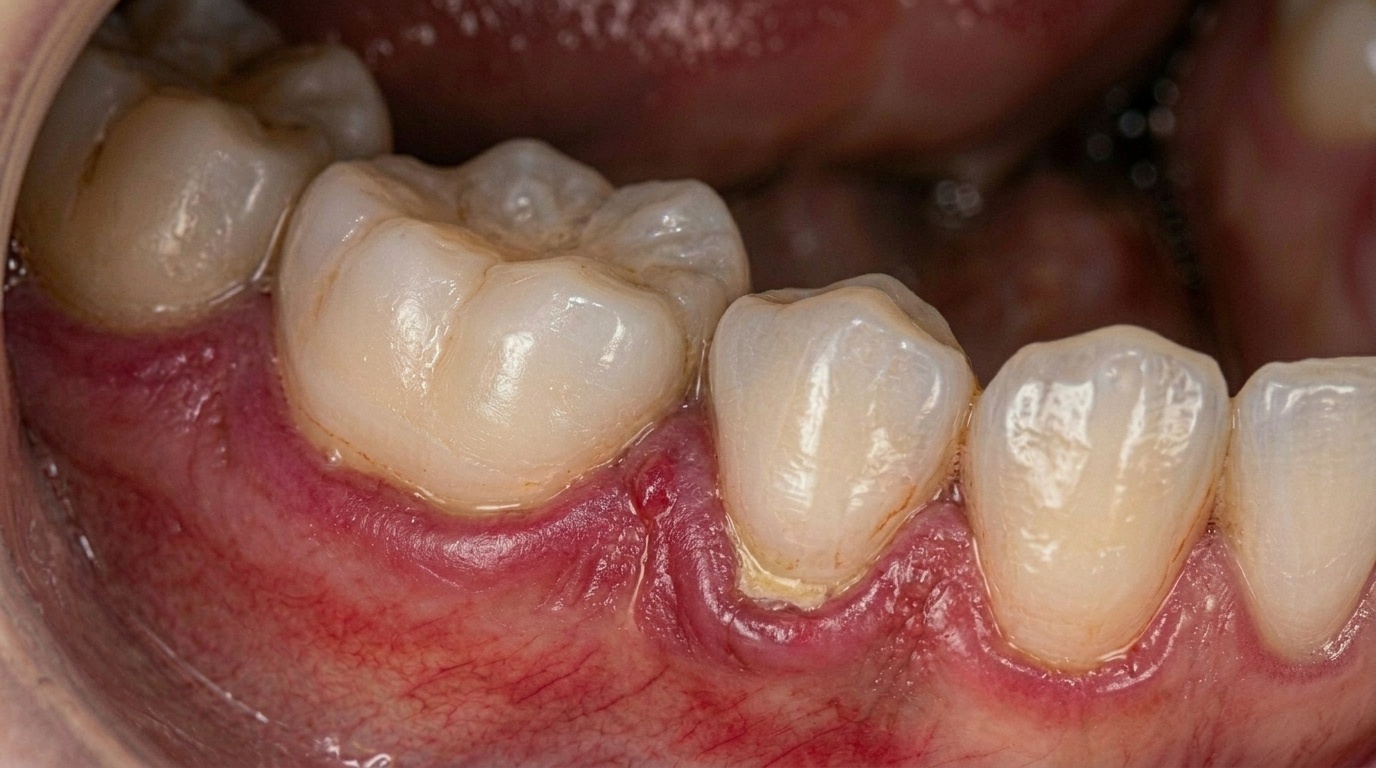
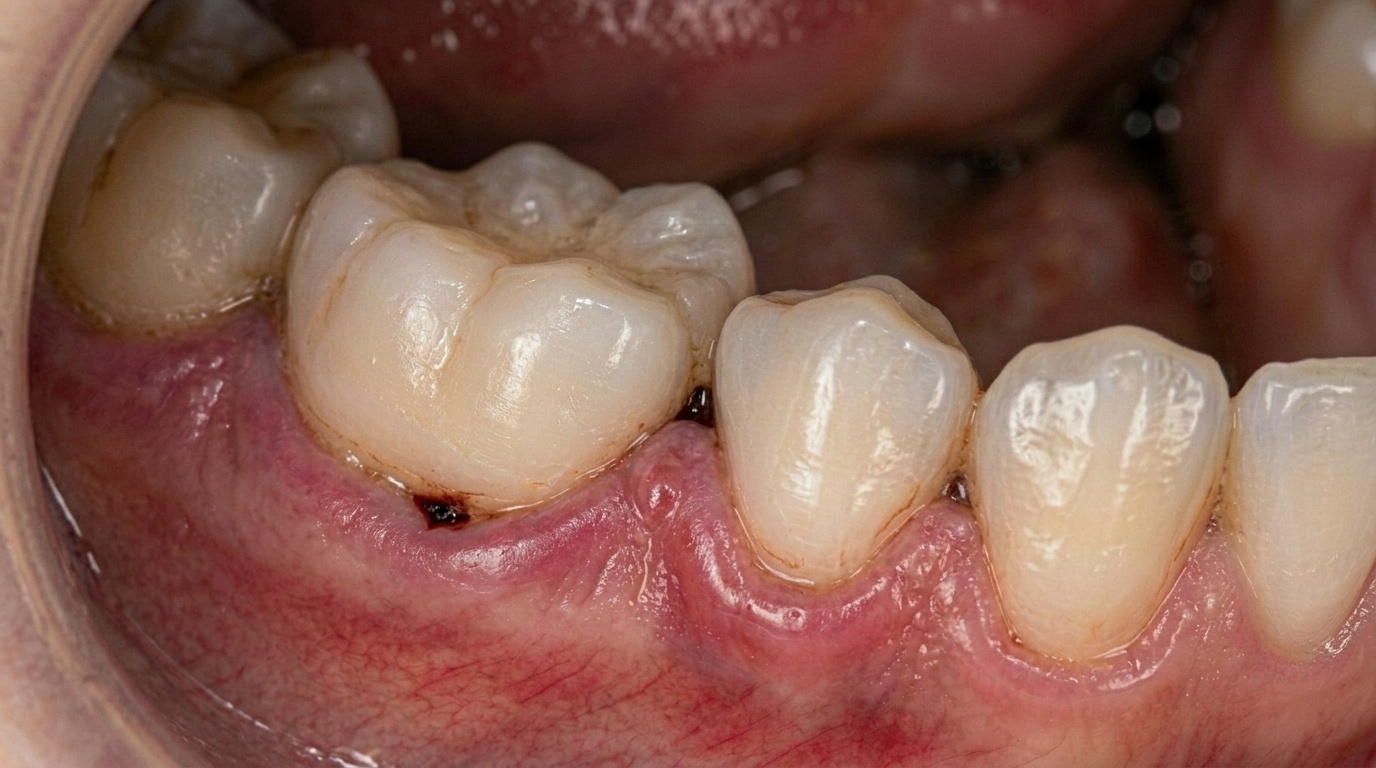
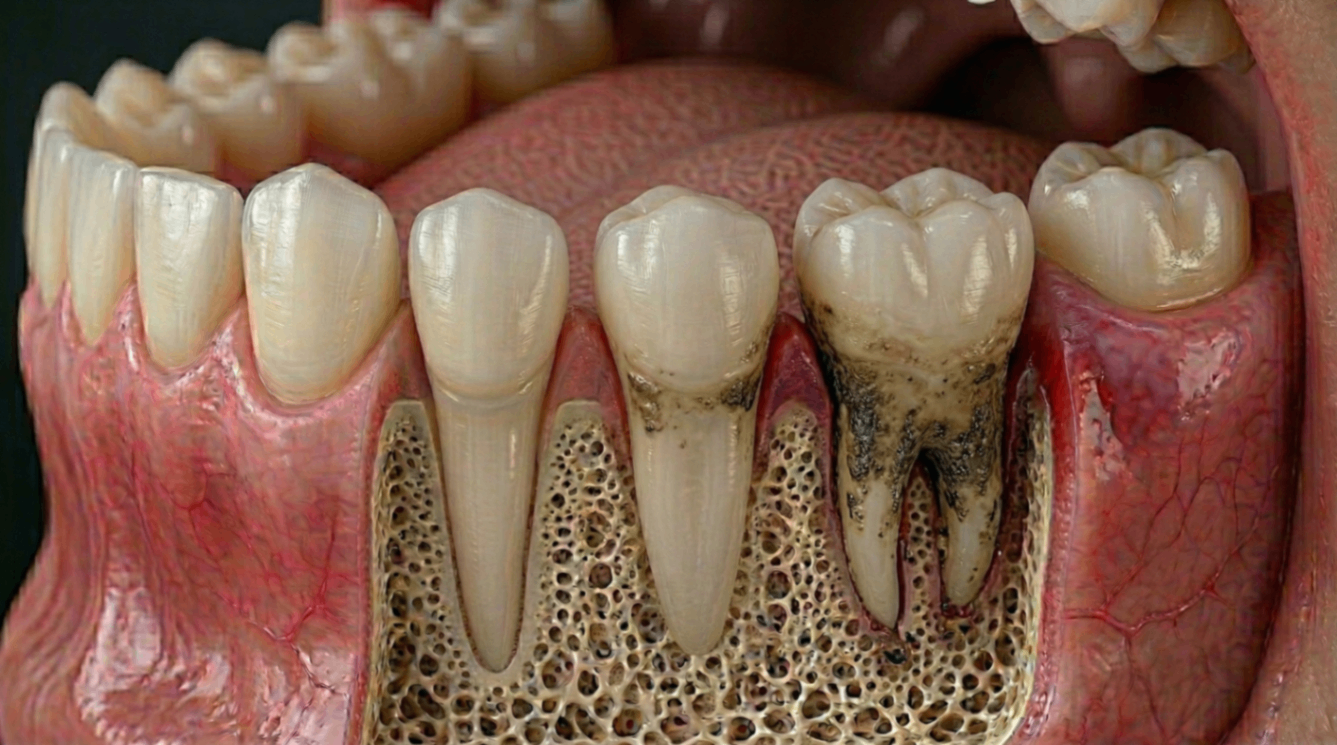
Gum Disease: The Most Common Cause
Gum disease is one of the leading causes of chronic bad breath. A systematic review by De Geest et al. (2016) confirmed a strong association between periodontal disease and halitosis, with bacteria living deep under the gumline thriving in low-oxygen environments and producing high concentrations of VSCs.
Common signs that gum disease may be driving your bad breath include:
Breath that smells unpleasant soon after brushing
A persistent bad or metallic taste
Bleeding gums when brushing or flossing
Food getting trapped between teeth more easily than before
Receding gums or teeth that appear longer
Gum disease often progresses without pain. For many patients, bad breath is the earliest warning sign that bacterial infection is present below the gumline.
Cavities and Failing Restorations
Deep cavities trap food particles and bacteria, even when there is no pain. Old or leaking fillings can also create microscopic gaps where bacteria collect underneath the restoration.
As Porter and Scully (2006) noted, decaying teeth and defective restorations are recognised contributors to oral malodour because they create sheltered environments for odour-producing bacteria.
Watch for these signs:
Dark areas or discolouration on teeth
Sensitivity to sweet, hot, or cold foods
Rough or chipped edges on existing fillings
Food consistently getting stuck in the same spot
Left untreated, decay can progress deeper into the tooth and eventually reach the nerve, potentially requiring root canal treatment.
The Tongue: An Often Overlooked Source
Even with clean teeth and healthy gums, bacteria can form a thick coating on the back of the tongue. Research by Van Tornout et al. (2013) found that tongue coating is a significant independent contributor to bad breath, harbouring large numbers of anaerobic bacteria that produce VSCs.
Signs that tongue bacteria may be contributing to your bad breath:
White or yellow coating on the tongue surface
Particularly strong morning breath
Persistent dry mouth
Changes in taste
Tongue cleaning can help reduce surface bacteria, but a persistent coating often points to a deeper bacterial imbalance or underlying gum disease that needs professional assessment.
Dry Mouth Makes Everything Worse
Saliva plays a critical role in controlling oral bacteria and washing away food debris. When saliva production drops, odour-producing bacteria multiply faster and the mouth loses its natural self-cleaning ability.
Common causes of dry mouth include:
Certain medications (antidepressants, antihistamines, blood pressure drugs)
Habitual mouth breathing
Dehydration
Chronic stress
Sleep apnoea
Age-related changes in saliva production
If dryness is constant, it is worth discussing with your dentist, as it affects not only breath but also your risk of decay and gum problems.
How ArtSmiles Treats Persistent Bad Breath
At ArtSmiles, we focus on treating the cause rather than masking the smell. Our approach may include:
A thorough oral assessment to identify the source
Deep cleaning if gum disease is present
Repair or replacement of decayed teeth or leaking fillings
Tongue cleaning guidance and tailored home-care advice
Dry mouth management and protective treatments
Addressing the underlying source is what delivers lasting results — not mouthwash, mints, or breath sprays.
When to Book a Check-Up
Consider seeing your dentist if:
Bad breath persists despite regular brushing and flossing
Someone close to you has mentioned it
Your gums bleed when you brush
You frequently experience dry mouth
Food gets trapped in the same areas regularly
You notice a coating on your tongue
You have not had a dental check-up in the past year
Chronic bad breath is not something you have to live with, and it is almost always treatable once the cause is identified.
Take the Next Step
Bad breath that does not go away is more than a social concern. It is often a sign that harmful bacteria are active below the gums, inside cavities, or on the tongue. Identifying the cause early protects both your breath and your long-term oral health.
If persistent bad breath has been a concern for you, the team at ArtSmiles Gold Coast can help find the source and put you on the right path. Book an appointment online or get in touch to take the first step.
References
Yaegaki K, Coil JM. Examination, classification, and treatment of halitosis; clinical perspectives. J Can Dent Assoc. 2000;66(5):257-261. PubMed
Porter SR, Scully C. Oral malodour (halitosis). BMJ. 2006;333(7569):632-635. PubMed
Scully C, Greenman J. Halitology (breath odour: aetiopathogenesis and management). Oral Dis. 2012;18(4):333-345. PubMed
De Geest S, Laleman I, Teughels W, Dekeyser C, Soviet M, The R, The M. Periodontal diseases as a source of halitosis: a review of the evidence and treatment approaches for dentists and dental hygienists. Periodontol 2000. 2016;71(1):213-227. PubMed
Van Tornout M, Dadamio J, Declerck D, De Lenteer M, Quirynen M. Tongue coating: related factors. J Oral Pathol Med. 2013;42(1):9-14. PubMed