
Dental
Caries
Stop cavities before they start.
Tooth decay isn’t just about getting a filling. It’s a disease process that keeps going unless you address the root cause. At ArtSmiles, we don’t just fix the damage, we help you understand why it happened so you can prevent it from coming back. That’s what makes the real difference between dental work that lasts years and dental work that lasts decades.
What Are
Dental Caries?
- Plaque build-up — bacteria on tooth surfaces that produce acid
- Sugars and starches — food and drink that feed those bacteria
- Repeated acid attacks — weakening the tooth's minerals over time
- Not enough protection — low saliva flow, not enough fluoride, or inconsistent brushing and flossing
Research shows that past decay experience is the single strongest predictor of future cavities across all age groups (Mejàre et al., 2014). Dental caries is now classified as a chronic, sugar-driven disease — not an isolated event (Pitts et al., 2017).
Signs of Active Decay
- Visible white spot or chalky area near gumline
- Sensitivity to cold, sweets, or biting
- Food trapping between teeth
- Visible discolouration or darkening
- Persistent toothache or dull ache
- Fillings that feel rough or have broken edges

These teeth have no visible cavity, but the chalky white areas along the gumline are white spot lesions — early signs of mineral loss caused by dental caries. Most patients would not notice this without a clinical examination. At this stage, decay can still be reversed without drilling.
Decay and
Systemic Health
- Diabetes, reduces saliva flow, increases glucose concentration in saliva, and elevates susceptibility to oral infection
- Dry mouth (xerostomia), saliva buffers acids, delivers minerals, and provides antimicrobial defence; hyposalivation significantly elevates caries risk
- Acid reflux (GERD), repeated acid exposure from gastric content weakens enamel and increases susceptibility to decay
Why Decay
Keeps Returning
Why Patients Keep Getting Cavities
- Frequent snacking or sugary beverages
- Acidic drinks (including "healthy" juices)
- Dry mouth (medications, mouth breathing, medical conditions)
- Poor plaque control at the gumline
- Orthodontic appliances or retainers
- History of high decay activity
How to Stop Tooth Decay
- Reducing the frequency of sugar exposure, timing matters more than total quantity
- Optimising fluoride exposure based on individual risk level
- Improving plaque control with personalised technique instruction
- Supporting saliva function where hyposalivation is identified
- Monitoring high-risk areas at regular, structured intervals
Dental Caries and Your Health
Tooth decay is one of the most studied diseases in medicine. The table below summarises the strongest available evidence — all from peer-reviewed systematic reviews and clinical studies published in leading dental journals.
Book Your Tooth Decay Assessment
Share your details and our team will be in touch within 1 business day to confirm your appointment.
Prefer to call? Reach us on (07) 5588 3677
How We Treat
Tooth Decay
Every patient receives a structured risk assessment before treatment is planned. We treat biology, not just holes.
Caries Risk Assessment
Every patient receives a structured risk assessment aligned with CAMBRA and CariesCare frameworks. Treatment is planned around biology, not assumptions.
- —Disease indicators: new cavities, white spot lesions, radiographic findings
- —Risk factors: sugar frequency, dry mouth, acid reflux, medical history
- —Protective factors: fluoride exposure, saliva flow, oral hygiene effectiveness
- —Recall interval and prevention intensity determined by risk level
 Step 01 · ArtSmiles
Step 01 · ArtSmilesReady to take the next step?
Book a consultation to discuss your personalised plan.
Risk-Based
Assessment Model
Based on CAMBRA (Caries Management by Risk Assessment). Featherstone et al., 2021 — Evidence-Based Caries Management
Stages of
Dental Caries
 Reversible
ReversibleWhite Spot Lesion
Enamel begins losing minerals. A chalky white area may appear. The surface can still be intact. Often reversible with fluoride and risk control, no drilling required.

Enamel Breakdown
Enamel weakens and begins to collapse. Food trapping and plaque retention increase. Conservative restoration required to prevent progression.

Dentine Involvement
Decay reaches dentine. Progression accelerates significantly. Sensitivity to cold or sweets is common. Prompt restoration is essential to protect the nerve.
 Urgent
UrgentPulp Involvement
Decay reaches the nerve. Persistent pain, infection, and swelling may occur. Root canal treatment or extraction may be required.
The earlier decay is found, the simpler and less invasive the treatment. Once it reaches the nerve, options become limited and more complex.
Concerned About Cavities?
A thorough clinical assessment is the first step. Our Southport dentist welcomes patients from across the Gold Coast, including Bundall, Labrador, Main Beach, Surfers Paradise and Parkwood. Share your details and our team will be in touch within 1 business day.
Ready to get started?
Prefer to call? (07) 5588 3677
Understand Your
Oral Health Risk
Our risk assessment takes less than two minutes and helps us identify potential vulnerabilities before they compromise your treatment. The results allow our team to build a personalised prevention plan alongside your care.
- —Decay risk, dietary habits, saliva quality, and bacterial balance
- —Gum disease risk, inflammation patterns, bone support, and hygiene effectiveness
- —Grinding & clenching risk, bite forces, wear signs, and jaw tension
Start Your Assessment
Takes less than 2 minutes. No obligation.
Why Early Tooth Decay
Treatment Matters
Consequences of Delayed Treatment
Progressive Tooth Destruction
Cavities enlarge with each acid cycle. What begins as a minor lesion steadily undermines sound tooth structure, making conservative restoration increasingly difficult.
Cracked Teeth
Weakened tooth structure is more susceptible to fracture under normal bite forces. Cracks can extend below the gum line, sometimes making the tooth non-restorable.
Nerve Infection
Untreated decay reaching the pulp causes irreversible inflammation and abscess formation. Pain, swelling, and systemic infection risk increase significantly at this stage.
Root Canal Treatment
Once infection reaches the pulp, root canal treatment is required to save the tooth. This is avoidable with early intervention at the enamel or dentine stage.
Tooth Loss
Severely decayed teeth may require extraction, creating the need for complex restorative rehabilitation including implants, bridges, or dentures to restore function.
Restoration Failure
Restorations placed in a high-risk oral environment have a shortened lifespan. Bacteria at margins, recurrent decay, and acid exposure cause even quality ceramic work to fail prematurely.
Related Articles

Is Oil Pulling Good for Oral Health?
Updated 25 April 2026

"It Doesn't Hurt"… and That's Why Dental Problems Are Often Missed
Updated 25 April 2026

What Happens When You Wait Too Long With a Cracked Tooth
Updated 25 April 2026
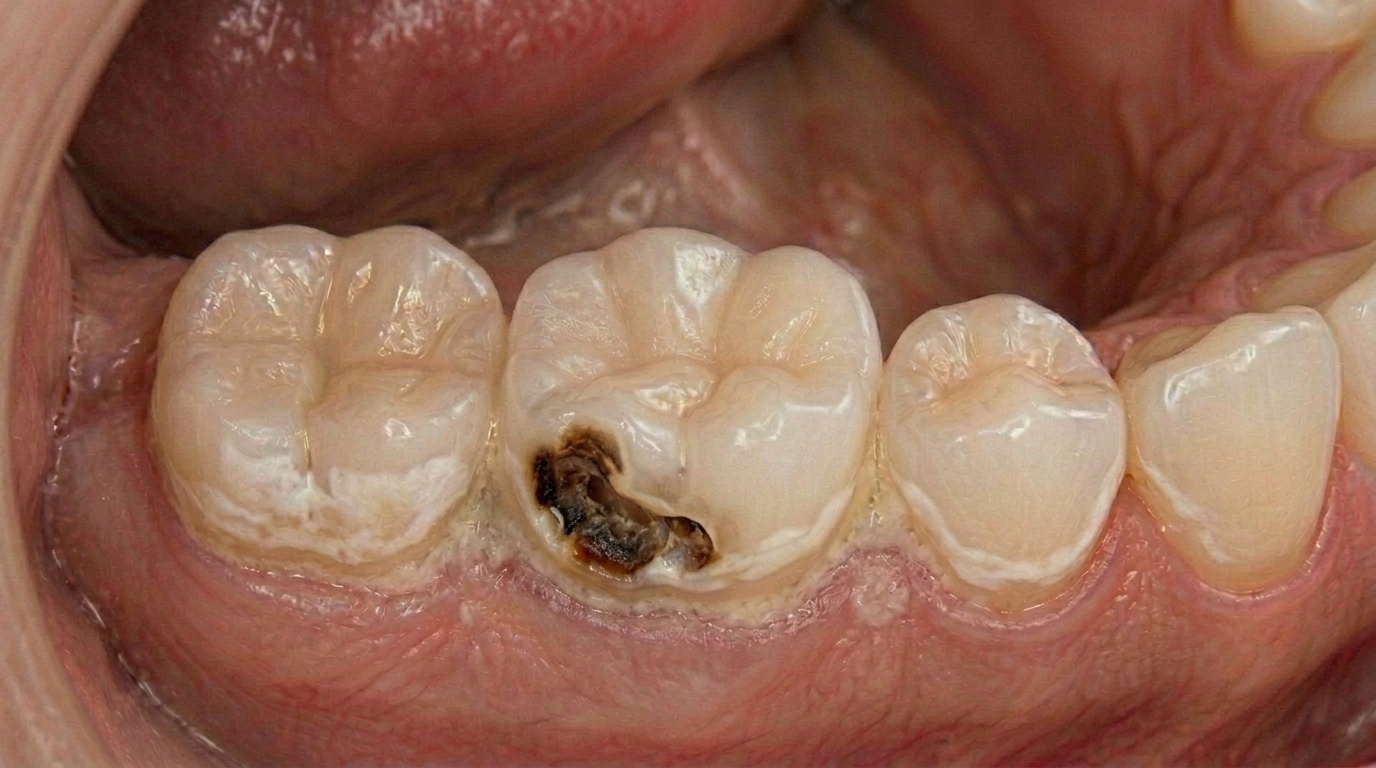
What Really Happens When You Ignore a Cavity
Updated 25 April 2026
Frequently Asked
Questions
What is a white spot lesion?
A white spot lesion is an early sign of enamel demineralisation, the first detectable stage of dental caries. It appears as a chalky-white or opaque area on the tooth surface. The enamel surface is still intact at this stage, meaning the lesion can potentially be remineralised without drilling if identified and managed promptly.
Do fillings last forever?
No. Dental restorations have a finite lifespan, and that lifespan is significantly shortened by ongoing, unmanaged caries disease. Each time a restoration fails and is replaced, it must be larger than the previous one. Managing the underlying disease process is the most effective way to extend the longevity of restorations and avoid escalating treatment complexity.
How does diabetes affect cavity risk?
Diabetes increases caries risk through several mechanisms: reduced salivary flow and altered saliva composition, higher glucose concentration in saliva (providing more substrate for acid-producing bacteria), impaired immune response, and reduced healing capacity. Patients with poorly controlled diabetes are at significantly elevated risk of rapid dental decay.
Can fissure sealants help prevent decay?
Yes. Fissure sealants are a thin protective coating applied to the grooves of back teeth, where plaque accumulates and is hardest to clean. Sealants are particularly effective for children and adolescents, but adults with deep fissures or elevated caries risk can also benefit. They are a low-cost, non-invasive preventive measure that reduces the risk of pit-and-fissure cavities significantly.
Is tooth decay treatment covered by health insurance?
Most Australian private health insurance extras policies cover a portion of preventive and restorative dental treatment, including check-ups, fluoride application, and fillings. Coverage varies by fund and level of cover. We recommend contacting your insurer or asking our team to check your eligibility before your appointment.
What is the CAMBRA model?
CAMBRA (Caries Management By Risk Assessment) is an evidence-based clinical framework for assessing and managing dental caries. It categorises patients into low, moderate, high, or extreme risk based on biological risk factors and disease indicators, and guides clinicians in tailoring prevention strategies and recall intervals accordingly. CariesCare International is a related framework with similar principles.
Can tooth decay cause tooth loss?
Yes. Advanced decay that reaches the nerve and causes pulp necrosis and periapical abscess, combined with structural breakdown, can render a tooth unrestorable. Tooth loss from caries is preventable in most cases with early detection and appropriate management.
Can acid reflux cause tooth decay?
Yes. Acid reflux (GERD) exposes teeth to gastric acid, which is highly erosive to enamel. Repeated acid exposure from reflux weakens the enamel surface, accelerates tooth wear, and significantly increases susceptibility to dental caries. Managing reflux is an important component of a complete dental prevention strategy for affected patients.
How often should I see a dentist if I have high decay risk?
High-risk patients generally benefit from a 3-monthly recall interval, more frequent than standard 6-monthly checks, to allow closer monitoring of lesion activity, early intervention if new decay appears, and regular reinforcement of prevention protocols. The appropriate interval is determined individually based on risk assessment findings and response to prevention.
Still have questions?
Our team is here to help. Book a consultation to discuss your options.
This page has been clinically reviewed by Dr. Cristian Dunker, BDSc, MBA, Principal Dentist at ArtSmiles.
Protect Your Teeth
Keeps Coming Back
A structured risk assessment identifies what is driving your decay — so we can stop it, not just patch it. Most patients see improvement within the first recall cycle.

