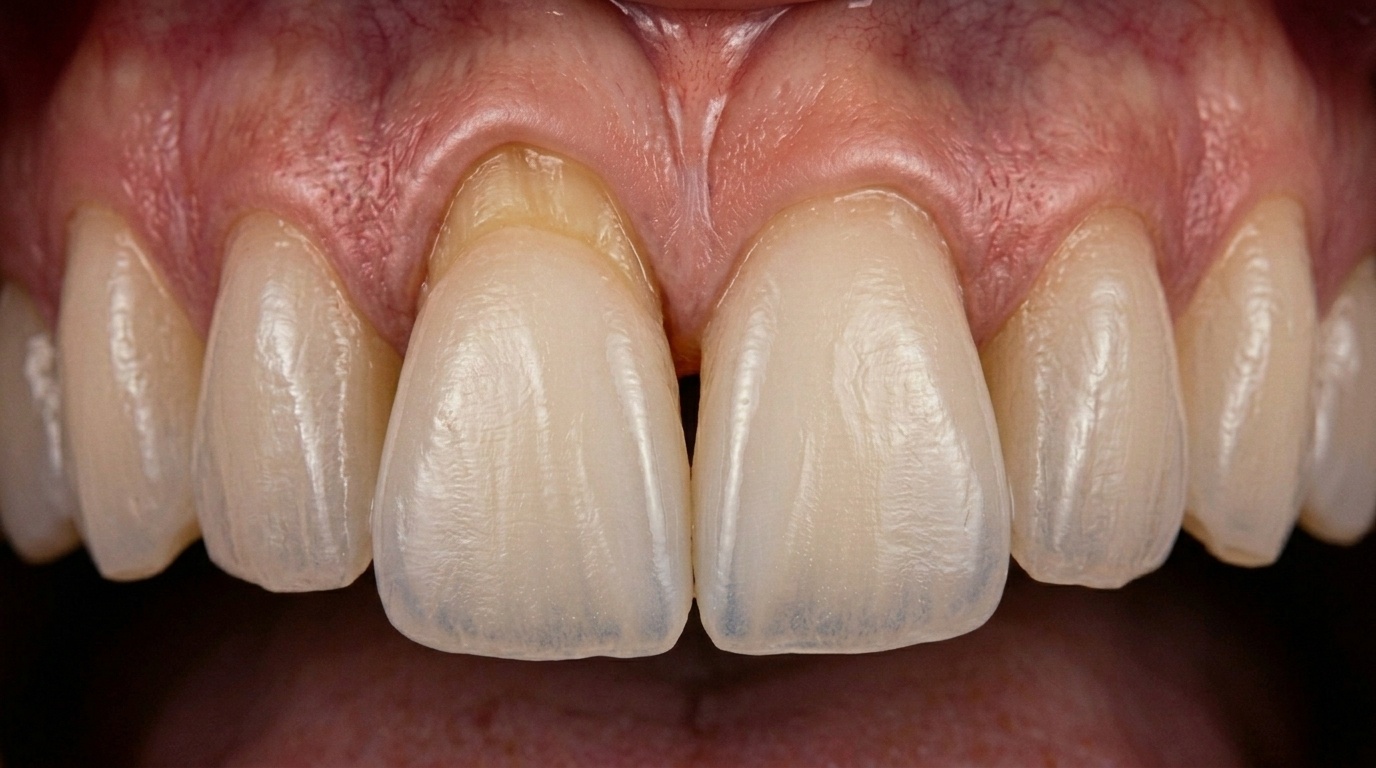
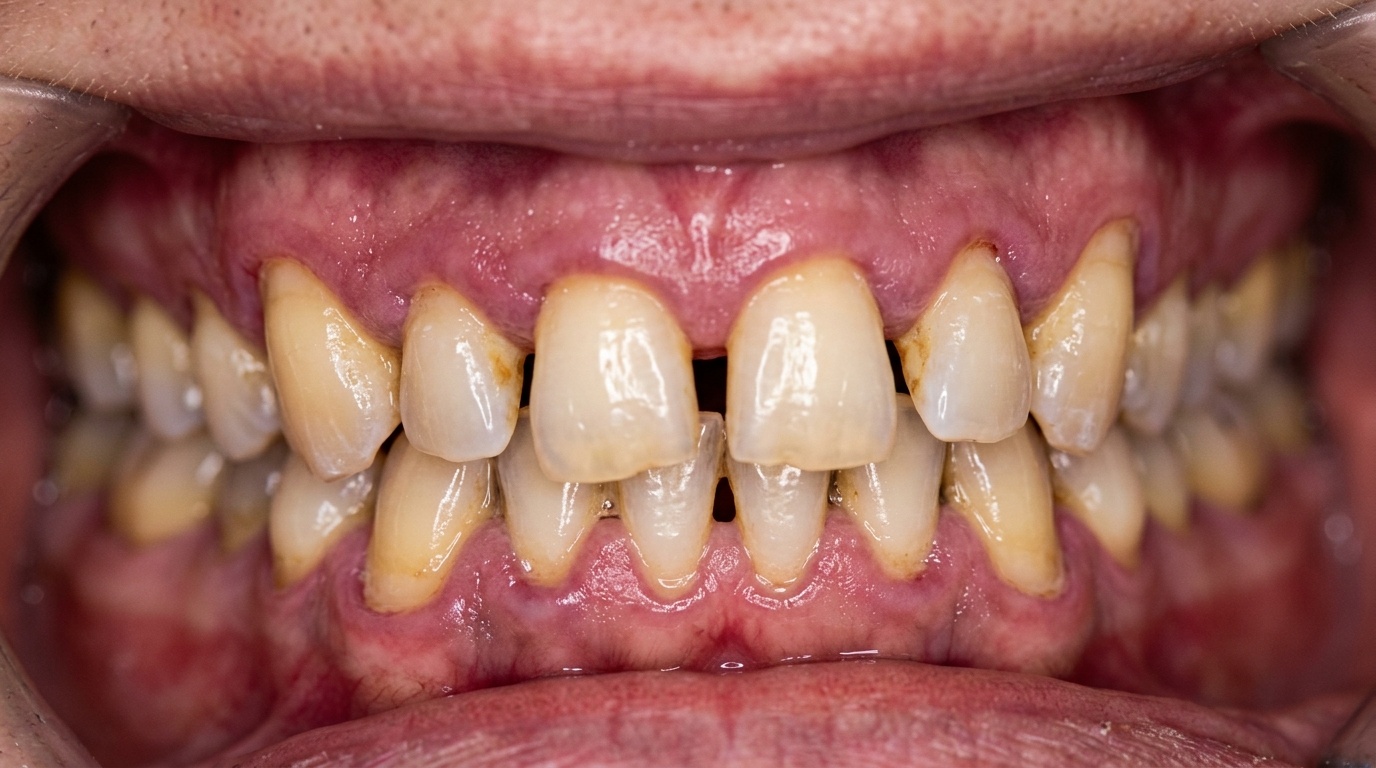
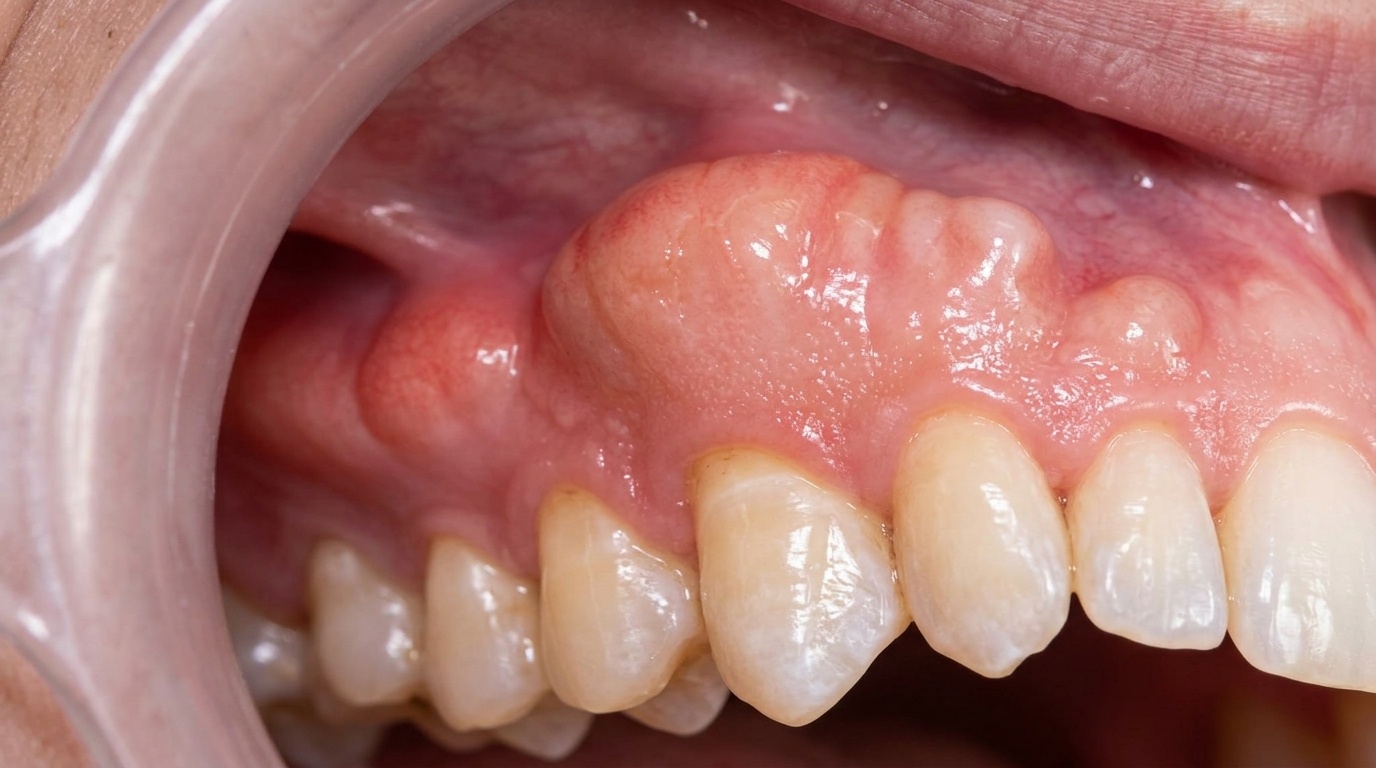
Gum recession happens when the gumline gradually pulls back, exposing the root surface of the tooth. Many patients first notice it when their teeth start looking longer than usual or when cold foods cause sudden, sharp sensitivity.
While it might seem like a cosmetic issue, recession usually points to something deeper — and the earlier it is assessed, the easier it is to stop progression and protect the tooth. As Kassab and Cohen (2003) noted, gingival recession is one of the most common conditions seen in clinical practice and affects a wide range of age groups.
What Gum Recession Really Is
Healthy gums sit snugly around each tooth, forming a protective seal over the roots and underlying bone. When recession occurs, that seal breaks down:
The gumline pulls back from its normal position
The root surface becomes exposed
Sensitivity increases, especially to cold and touch
The area becomes more prone to decay and wear
Because tooth roots are softer than enamel and lack the same protective layer, recession is a structural concern — not just an aesthetic one. Tugnait and Clerehugh (2001) highlighted that exposed roots are more susceptible to caries, abrasion, and sensitivity, making early management important.
The Most Common Causes of Gum Recession
Gum disease
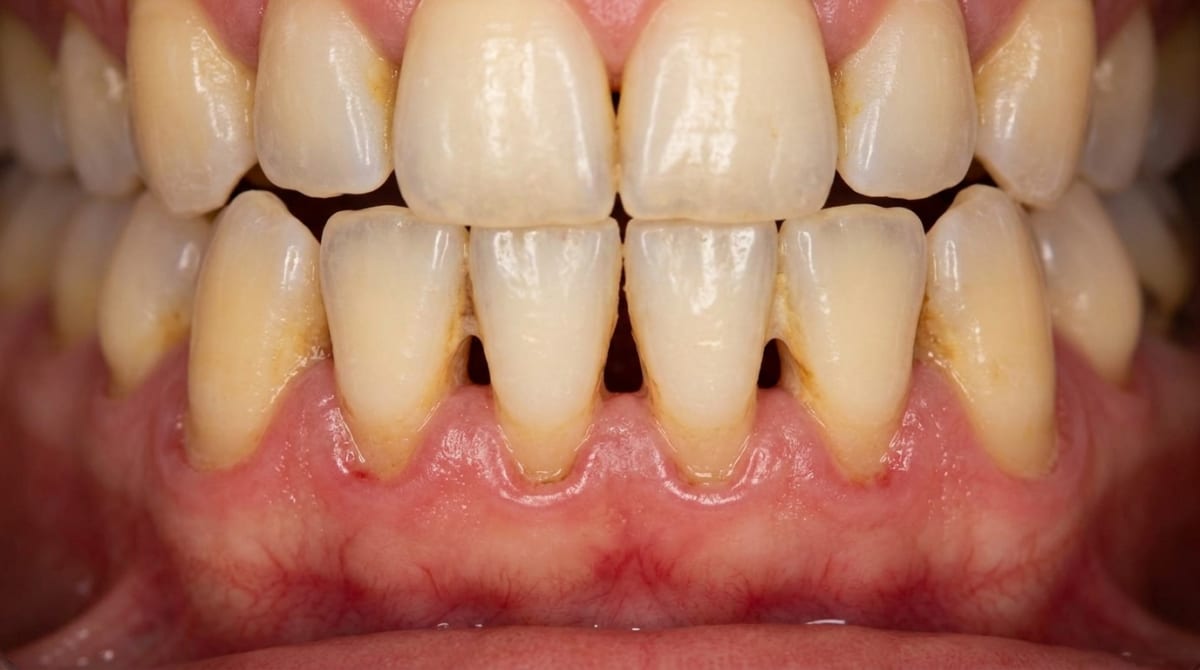
This is the leading cause of recession in adults. Chronic inflammation caused by bacterial plaque damages the bone and supporting tissues over time. As bone is lost, the gums recede along with it. Common signs include bleeding gums, persistent bad breath, tooth movement, and deepening pockets around the teeth. Cortellini and Bissada (2018) classified recession as a key mucogingival condition often linked to periodontal disease. If you are experiencing any of these signs, learn more about gum disease and how it is treated.
Overbrushing or hard toothbrushes
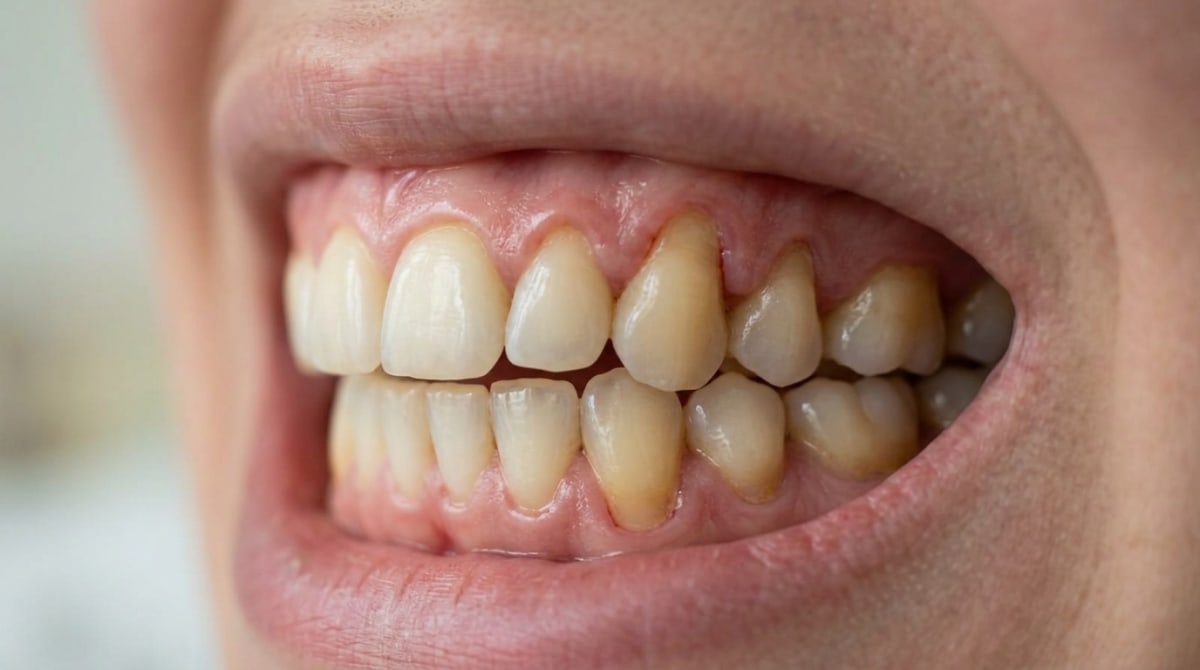
Aggressive brushing can physically wear away the gum margin, even in people who otherwise have good oral hygiene. Using a hard-bristled brush or scrubbing side to side with too much pressure gradually strips the tissue away from the tooth.
Grinding and clenching
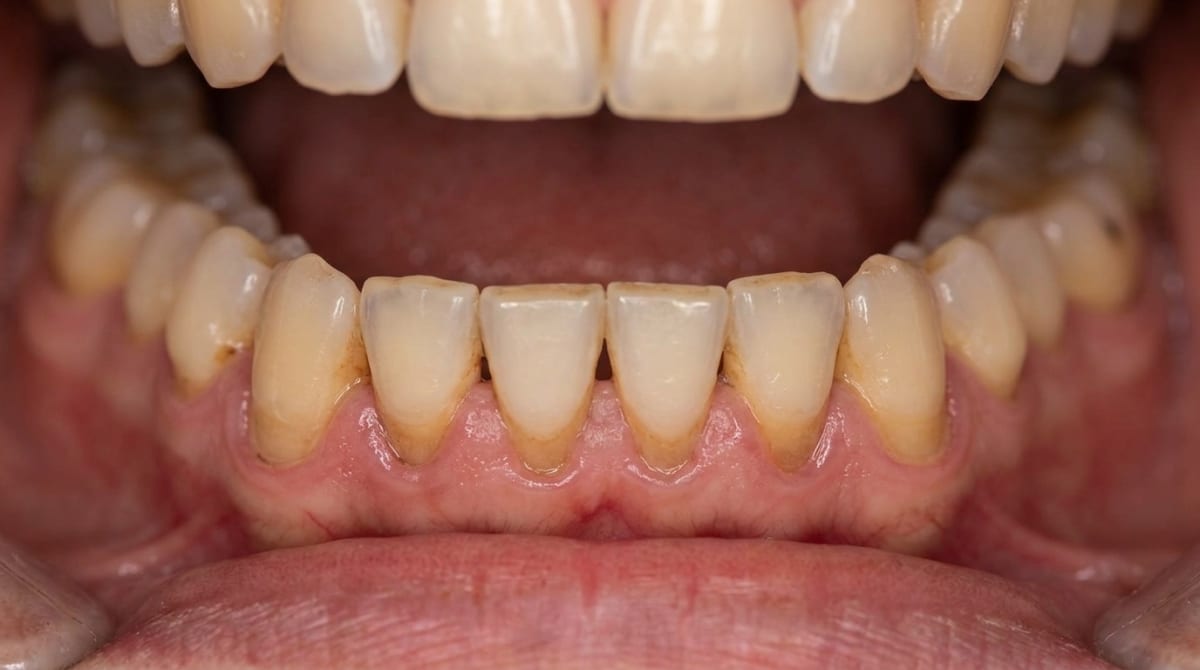
Excessive bite forces overload the teeth and supporting tissues, contributing to recession in areas under the most stress. If you clench or grind your teeth — especially at night — this may be a contributing factor. Read more about bruxism and how it affects your teeth and gums.
Thin gum tissue
Some people naturally have thinner gums, sometimes called a thin biotype. This tissue is more vulnerable to irritation from brushing, orthodontic movement, or bite pressure, and may recede more easily than thicker tissue.
Smoking and vaping
Tobacco use reduces blood flow to the gums, impairing healing and increasing the risk of recession. Smokers are also more likely to develop gum disease, which compounds the problem.
Local trauma or habits
Lip or tongue piercings, nail-biting, or habitual pen-chewing can cause localised recession by repeatedly irritating the gum tissue in one area.
Why Gum Recession Often Has No Pain
Recession usually progresses slowly and quietly. Many patients only become aware of it when:
Teeth look noticeably longer than before
Sensitivity appears when eating or drinking cold foods
Root surfaces are visibly exposed at the gumline
A dentist identifies it during a routine examination
Because the change is gradual, it is easy to overlook until discomfort or visible changes develop.
Problems Gum Recession Can Cause
Sensitivity to cold, sweet foods, and brushing
Higher risk of root decay, since roots lack the protective enamel layer
Aesthetic concerns from an uneven or receding gumline
Further bone loss if active gum disease is present
Tooth mobility in more advanced cases
How We Identify the Cause at ArtSmiles
Effective treatment starts with understanding why recession is happening in the first place. At ArtSmiles, an assessment may include:
Periodontal charting to measure pocket depths and attachment levels
Digital X-rays to assess bone support
Evaluation of gum thickness and tissue biotype
Bite analysis to check for grinding or clenching patterns
Review of brushing habits and technique
Screening for bruxism or other contributing habits
The underlying cause determines the treatment approach. As Wennström (1996) outlined, mucogingival therapy decisions should be guided by a thorough assessment of both the defect and the patient's specific risk factors.
How Gum Recession Is Treated
Stabilising gum disease
Deep periodontal cleaning removes bacteria from below the gumline and allows the tissues to heal and stabilise. This is often the first step before any further treatment is considered.
Improving brushing technique
Switching to a soft-bristled brush, using gentle circular motions, and considering a pressure-controlled electric toothbrush can prevent further tissue loss.
Managing grinding
Custom night guards help distribute bite forces evenly and protect the teeth and gums from excessive pressure during sleep.
Reducing sensitivity
Fluoride treatments, bonding of exposed root surfaces, or specialised desensitising toothpaste can help manage discomfort while the underlying cause is addressed.
Gum grafting for advanced cases
When recession is moderate to severe, gum grafting may be recommended to rebuild and thicken the gumline. Zucchelli and Mounssif (2015) described modern periodontal plastic surgery techniques that can achieve predictable root coverage and improved tissue thickness. A Cochrane review by Chambrone et al. (2018) confirmed that several surgical approaches can effectively cover exposed roots when the right technique is matched to the right case.
When to See a Dentist About Recession
Book an assessment if you notice any of the following:
Teeth that look longer than they used to
Sensitivity near the gumline
Dark root edges becoming visible
Gums that appear thin, pulled back, or uneven
Food getting trapped in new areas
Bleeding gums or deepening pockets
Signs of grinding or clenching
Recession rarely reverses on its own. Early care makes a real difference in preserving both gum tissue and tooth structure.
Understanding Your Next Steps
Gum recession is more than a cosmetic concern. It often reflects underlying inflammation, excess force, or structural weakness in the supporting tissues. With early diagnosis and the right approach, progression can usually be stopped — and in many cases, the damage can be repaired.
If you have noticed changes in your gumline, the team at ArtSmiles Gold Coast can help identify the cause and guide you through the right treatment. Book an appointment online or get in touch to take the first step.
References
Kassab MM, Cohen RE. The etiology and prevalence of gingival recession. Journal of the American Dental Association. 2003. PubMed
Tugnait A, Clerehugh V. Gingival recession — its significance and management. Journal of Dentistry. 2001. PubMed
Cortellini P, Bissada NF. Mucogingival conditions in the natural dentition. Journal of Clinical Periodontology. 2018. PubMed
Chambrone L, et al. Root coverage procedures for recession defects. Cochrane Database of Systematic Reviews. 2018. PubMed
Zucchelli G, Mounssif I. Periodontal plastic surgery for gingival recession. Periodontology 2000. 2015. PubMed
Wennström JL. Mucogingival therapy. Annals of Periodontology. 1996. PubMed