Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker , Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | External root resorption (the gradual dissolving of a tooth root or surrounding bone), external cervical resorption, idiopathic external resorption |
How urgent? | 🟡 Worth checking, often painless but progressive; early identification can sometimes save the tooth |
Common or rare? | Very common in mild form; one large radiographic review found some degree of root resorption in 86% of teeth, although severe resorption affects only about 10% of patients |
Who it affects | Adults of any age; risk rises after orthodontic treatment, dental trauma, replanted/transplanted teeth, or with adjacent impacted teeth, cysts or tumours |
Who treats it | General dentist, often in coordination with an endodontist (a dentist who specialises in root canal treatment) or oral surgeon depending on the pattern and depth of resorption |
Based on | Cawson, Neville, Regezi |
What is it?
External tooth resorption is the loss of tooth structure from the outside of the root. Specialised cells called osteoclasts (the cells that break down bone and tooth tissue, the same cells that also shape bone) attach themselves to the cementum (the thin tissue layer that covers the root surface) and dentine (the softer layer under the enamel) of the root and gradually dissolve it. Because the surface of the root is normally protected by the periodontal ligament (the thin layer of fibres that holds a tooth into its socket), a thin cushion of fibres that suspend each tooth in its socket, resorption only takes hold when this protective layer is damaged or pressed on by something nearby. The result, on an X-ray, is an irregular notch or saucer in the root surface that was not there before. Mild resorption is extremely common and rarely causes any problem. Severe forms can eat into the pulp and lead to loss of the tooth.
Who tends to get it?
The textbooks describe external resorption as something that "the potential for is inherent within the periodontal tissue of each patient". In other words, anyone can develop it, but some situations dramatically increase the risk:
People who have had orthodontic treatment, particularly with heavy or prolonged forces. Most of these resorptions are minor, but a small percentage of patients lose a noticeable amount of root length. Genetics modifies the risk: people who carry certain variants of the interleukin-1B (IL-1B) gene have been reported to have up to a 5.6-fold higher risk during orthodontics.
People with a history of dental trauma, including a knocked-out (avulsed) and replanted tooth, a luxated (dislocated) tooth, or a heavily traumatised tooth from a sporting injury or fall.
People with reimplanted or transplanted teeth, these teeth almost always undergo gradual resorption as the body replaces them with bone.
People with adjacent impacted teeth, particularly an unerupted canine pressing against a neighbouring root.
People with periapical or periodontal infection, chronic inflammation around a non-vital (with a dead nerve) tooth or in a deep gum pocket can drive surface resorption.
People with cysts or tumours of the jaw, the pressure of an expanding lesion can resorb the roots of adjacent teeth.
People with Paget disease of bone, a generalised bone-remodelling disease.
Idiopathic cases, sometimes resorption appears without any identifiable cause, occasionally affecting more than one tooth, and occasionally clustering within families.
There is no strong age or sex predilection. Molars are the least likely tooth to develop the idiopathic pattern.
What causes it?
External resorption is the end result of an osteoclast (or "dentinoclast") becoming activated on the outside of the root. The textbooks group the triggers into a familiar list:
Periapical periodontitis, inflammation around the root tip of a non-vital tooth. The most common cause overall, though usually mild.
Periodontitis, chronic gum inflammation extending down the side of the root.
Orthodontic forces, particularly heavy or prolonged.
Dental trauma, luxation (a tooth that has been pushed loose in its socket without coming out), avulsion (a tooth that has been knocked completely out of its socket), intrusion, or repeated micro-trauma from grinding.
Reimplantation or transplantation of a tooth, because the periodontal ligament is no longer alive, the body remodels the tooth into bone.
Pressure from an impacted tooth, for example, an unerupted canine pressing on the root of a lateral incisor.
Pressure from a cyst or tumour, chemical mediators and physical pressure both contribute.
Paget disease of bone.
Systemic factors, including occasional reports linked to medications and to particular genetic profiles.
Idiopathic, no identifiable trigger.
How does it develop?
The four patterns of external resorption described in the textbooks help explain how the process develops differently depending on the cause:
External inflammatory resorption. Triggered by infection or inflammation either at the root tip (from a dead pulp) or along the side of the root (from periodontal disease). Granulation tissue replaces normal periodontal ligament, osteoclasts arrive, and the root surface is gradually eaten away.
External surface resorption. Mild, often microscopic, lesions caused by a transient stimulus, such as orthodontic movement or a minor knock. Many lesions of this type repair themselves over a few weeks once the stimulus is removed.
External replacement resorption (ankylosis, when a tooth fuses to the surrounding bone, losing its normal hinge). Most often seen in reimplanted, transplanted or severely traumatised teeth where the periodontal ligament has died. The body slowly replaces the root with bone, and the tooth becomes "ankylosed", fused to the surrounding jaw. Over years, the entire root is replaced and the crown eventually breaks off at the gum line.
External cervical resorption. A particular pattern that begins at the neck of the tooth, just below the gum line at the cementoenamel junction (where the enamel meets the root). It can be triggered by trauma, orthodontics, internal whitening of a discoloured root-canal-treated tooth, or for no apparent reason. Cervical resorption can spread within the dentine while leaving a thin shell of enamel above and the pulp itself untouched until late, which makes it particularly difficult to detect in its early stages.
What might you notice?
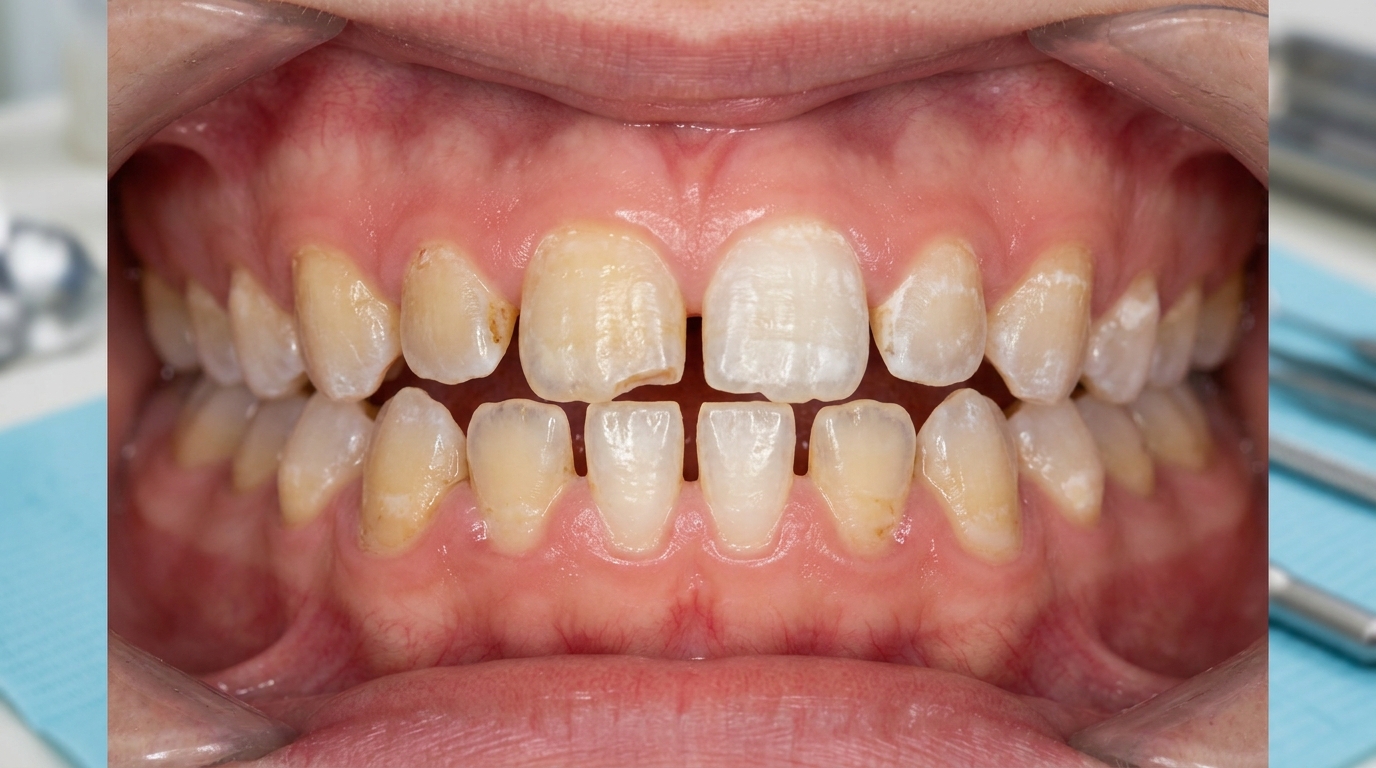
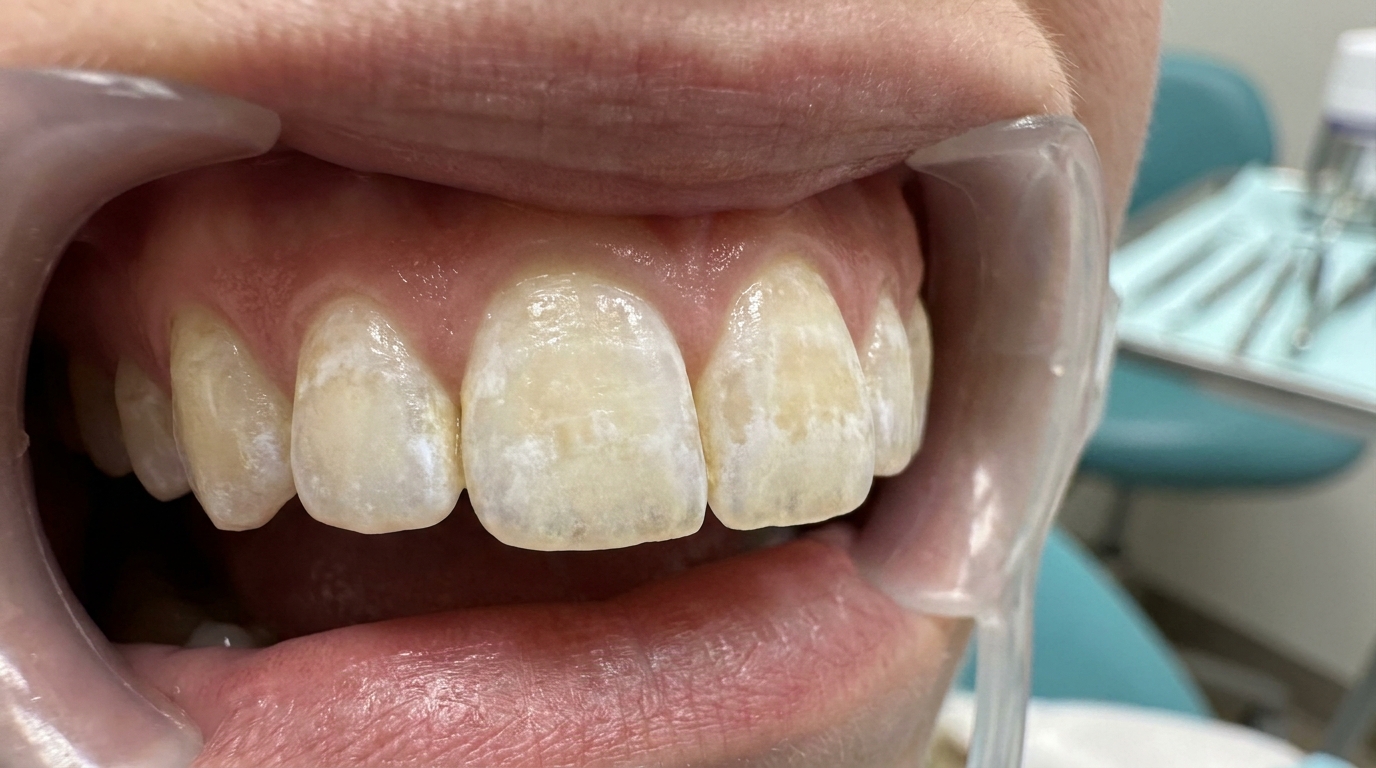
What it looks like
External resorption is usually invisible to the patient. When it does become visible, it can look like:
A dark or pink shadow showing through the enamel, particularly on a front tooth (if cervical resorption has progressed enough to thin the enamel).
A chip in the enamel at the gum line that doesn't match a typical filling or worn area.
A mobile tooth in late stages, particularly when much of the root has been resorbed.
A shortened crown in cases of long-standing replacement resorption, where the tooth has gradually been ground down by the opposing teeth while the root has fused to the bone.
What it feels like
Most people feel nothing at all. The textbooks all stress that external resorption is usually asymptomatic until very late. Symptoms, when they appear, may include:
A mild discomfort or aching if the pulp is irritated.
Sensitivity to cold or sweet foods if the resorption has reached the dentine close to the pulp.
Looseness of the tooth in the late stages.
Pain on biting if the lesion has perforated into the periodontal ligament.
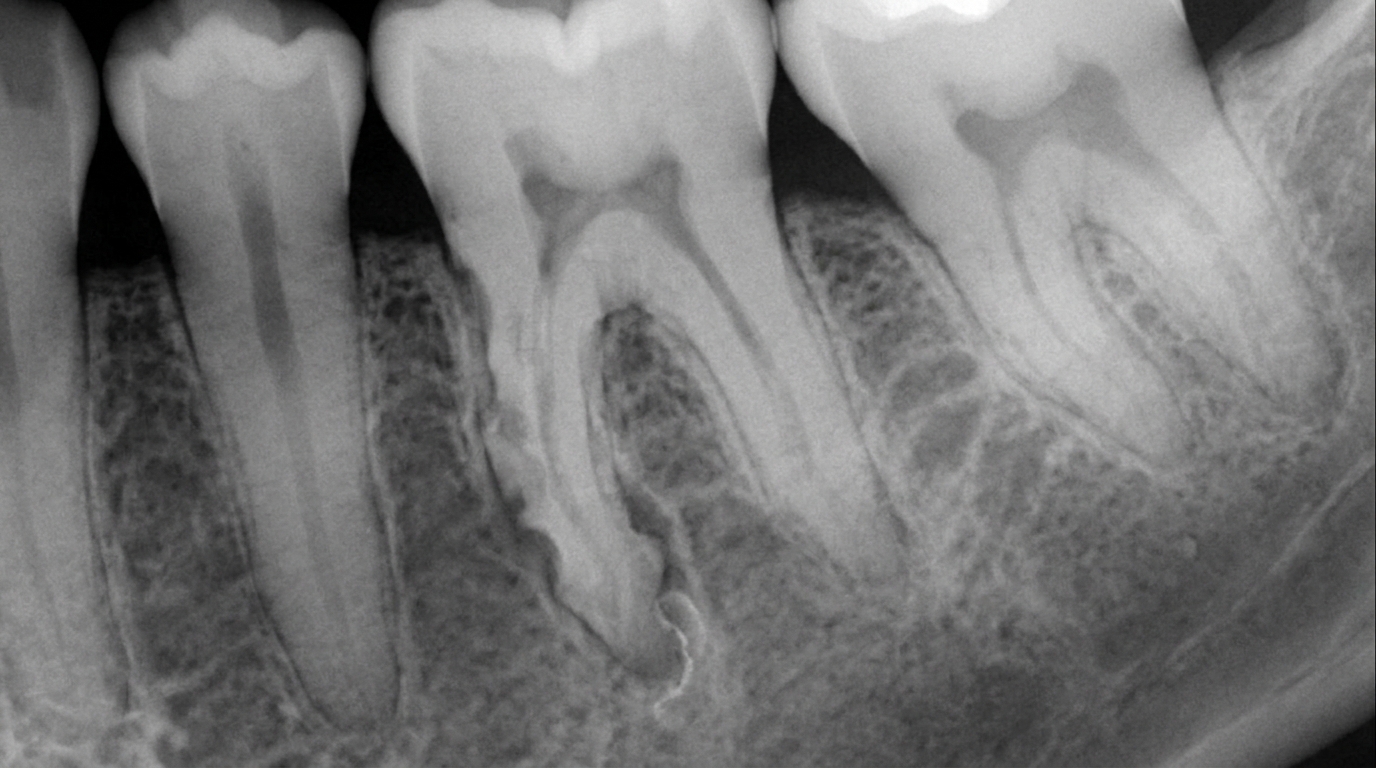
What an X-ray might show
X-rays, particularly bite-wing, periapical and small-field cone-beam CT or CBCT (a 3D dental X-ray) imaging, are the standard way external resorption is found. Typical findings:
An irregular, ragged, saucer-shaped defect on the side of the root.
A shortening or "blunting" of the root tip (apex), often after orthodontic treatment.
A moth-eaten radiolucent area at the cervical region, with the pulp canal still visible through the lesion (this distinguishes it from internal resorption, where the canal itself is enlarged).
Replacement resorption showing the root gradually being replaced by bone, with the periodontal ligament space narrowing or disappearing.
The textbooks emphasise that on a 2D radiograph, external and internal resorption can sometimes be hard to distinguish. A CBCT scan is often the most useful next step.
What happens at the dentist?
External resorption is most often picked up incidentally at a routine dental check-up and clean at ArtSmiles, often on routine X-rays. The dentist will typically:
Examine the suspected tooth for any visible defect, pink discoloration or unusual mobility.
Take periapical X-rays from different angles to clarify the location of the lesion. Where 2D imaging is inconclusive, a small-volume CBCT scan provides a 3D view that makes the diagnosis much clearer.
Test the pulp with cold and electric pulp testing to see whether the nerve is still alive.
Check the periodontal ligament space and lamina dura (the thin layer of bone lining the socket) on the X-ray for changes that suggest ankylosis or inflammation.
Take a careful history of any past trauma, orthodontic treatment, replanted teeth, internal bleaching, or recent illnesses.
Identify any local cause such as an impacted canine, a periapical lesion, or a cyst that could be driving the resorption.
Refer to an endodontist or oral surgeon when the lesion is complex, internal cervical resorption in particular can require specialist endodontic management or surgical exposure.
Is this serious?
🟡 Most external resorption is mild and clinically insignificant. The ones the textbooks describe as truly serious are those that progress quickly, perforate into the pulp, or compromise enough of the root that the tooth becomes mobile or unrestorable. Catching resorption early gives the best chance of preserving the tooth, particularly for cervical resorption, where a small defect can sometimes be cleaned and restored before it reaches the pulp.
If you have been told a tooth has root resorption, whether from orthodontics, trauma, an impacted tooth, or no obvious cause, it's worth booking an assessment so the pattern can be properly mapped and a tailored plan put in place.
Could it be something else?
Several conditions can mimic external resorption on an X-ray. The textbooks list these as the main differentials:
Internal tooth resorption (pink tooth of Mummery), looks similar at first glance, but the resorption is happening inside the tooth, with a balloon-like enlargement of the pulp canal. In external resorption, the canal itself remains its normal size and the radiolucency is superimposed on it.
Dental caries, can produce a dark area on an X-ray, but caries usually starts at the chewing surface or contact point, not on the root surface, and the tooth is often visibly broken down.
Periapical (apical) inflammatory disease, produces a radiolucency at the root tip, but the tooth has typically died and the lesion is centred on the apex rather than along the side of the root.
Ankylosis without obvious resorption, a tooth fused to the bone without much visible loss of root structure. Diagnosed by absence of normal periodontal ligament space and a characteristic high-pitched sound on percussion.
Periodontal pocket lesion, gum disease can produce a radiolucent defect on the side of the root, but periodontal probing identifies the deep pocket and inflammation.
Idiopathic dentine sclerosis or other developmental defects, rarely confused, but should be considered when the appearance is atypical.
How is it treated?
Treatment is much harder than for caries because the attacking cells are part of the body itself. The textbooks all stress that there is no medication that reliably stops the process, and that early identification of an underlying cause is the most important step. Specific options depend on the pattern:
At-home measures and habits that may help:
Maintain excellent oral hygiene to control any inflammatory contribution from periodontal disease.
Manage clenching or grinding habits with a custom night splint where indicated, since heavy occlusal loads can aggravate resorption.
Attend regular check-ups so any change can be tracked over time.
Avoid using over-the-counter whitening products inside a previously root-canal-treated front tooth, internal bleaching with strong agents is a recognised trigger for external cervical resorption.
Professional steps your dentist may consider:
Removing the underlying trigger wherever possible, for example, removing an impacted tooth that is pressing on the root of a neighbour, or cyst enucleation.
Root canal treatment when the pulp is involved or threatened. Root canal treatment alone does not stop external resorption, but it can prevent further damage from infection.
Surgical exposure and repair of accessible cervical lesions, with removal of granulation tissue and restoration using mineral trioxide aggregate (MTA), bioceramic materials or glass ionomer cement. The textbooks note that long-term success of these repairs is "infrequent and unpredictable", but it can buy useful time.
Stopping orthodontic treatment if active resorption is identified during ortho.
Splinting and stabilisation of mobile teeth where appropriate.
Extraction and replacement when the root has been damaged beyond repair, followed by an implant, bridge or denture as appropriate.
A patient-centred approach is particularly important here. External resorption is one of the more frustrating dental conditions because there is rarely a perfect answer. Honest discussion of options, expected outcomes, and timelines is itself part of effective care, values that sit at the heart of our clinical philosophy.
What's the long-term outlook?
The outlook varies widely with the pattern and stage. Mild surface resorption following orthodontics or a minor knock often stabilises and never causes problems. Cervical resorption caught early can sometimes be repaired and the tooth retained for many years; caught late, it usually leads to extraction. Replacement resorption in reimplanted teeth is a slow, predictable loss of the tooth over years to decades, particularly important to monitor in younger patients, where the gradual ankylosis can also affect jaw growth. Inflammatory resorption from periapical disease usually halts once the underlying infection is properly treated. Across all patterns, the single most important predictor is identifying and removing the cause as early as possible.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
The cover image above is an AI-generated illustration based on the most common visible features of this condition described in clinical pathology references. It is not a photograph of a real case and should not be used to diagnose or rule out the condition in your own situation. If you are concerned about something you have noticed, please book an assessment with a registered dental practitioner.
References
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 4, Pulpitis, Apical Periodontitis, Resorption and Hypercementosis: External resorption (idiopathic, cervical, generalised), pp. 69 to 72.
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2023). Oral and maxillofacial pathology (5th ed.). Elsevier. Chapter 2, Abnormalities of Teeth: Internal and External Resorption, including patterns (inflammatory, surface, replacement, cervical) and Box 2.3 list of causes, pp. 62 to 66.
Regezi, J. A., Sciubba, J. J., & Jordan, R. C. K. (2017). Oral pathology: Clinical pathologic correlations (7th ed.). Elsevier. Chapter 16, Abnormalities of Teeth: External Resorption, including chronic inflammatory lesions, cysts, tumours, trauma, reimplantation, impaction, and idiopathic cases, pp. 386 to 388.
Frequently asked questions
What is external tooth resorption?
External tooth resorption is the loss of the outside surface of the tooth (root or crown) caused by the body's own cells (osteoclasts) breaking down the tooth structure. It can be surface, inflammatory, replacement (ankylosis), cervical (at the gumline) or pressure-related, each with different causes and prognosis.
What causes external resorption?
Common causes include dental trauma (avulsion, intrusion, severe luxation), prolonged orthodontic forces, pressure from an erupting tooth, untreated infection from a non-vital tooth, internal whitening with high-concentration hydrogen peroxide, periapical inflammation and rare systemic conditions. Some cases are idiopathic (no identifiable cause).
How is it diagnosed?
Most external resorption is diagnosed on x-ray (periapical and bitewings) or cone-beam CT, which shows the precise 3D location of the defect. Early lesions can be detected at routine check-ups before symptoms appear. Pulp testing helps determine whether the pulp is involved.
How is external tooth resorption treated?
Treatment depends on the type and stage. Surface and small inflammatory lesions are observed if mild. Cervical invasive resorption is treated by surgical exposure, removal of granulation tissue and restoration with a glass-ionomer or composite filling, sometimes combined with root canal treatment. Severe or progressive resorption may require extraction and replacement with an implant or bridge.