Summary:
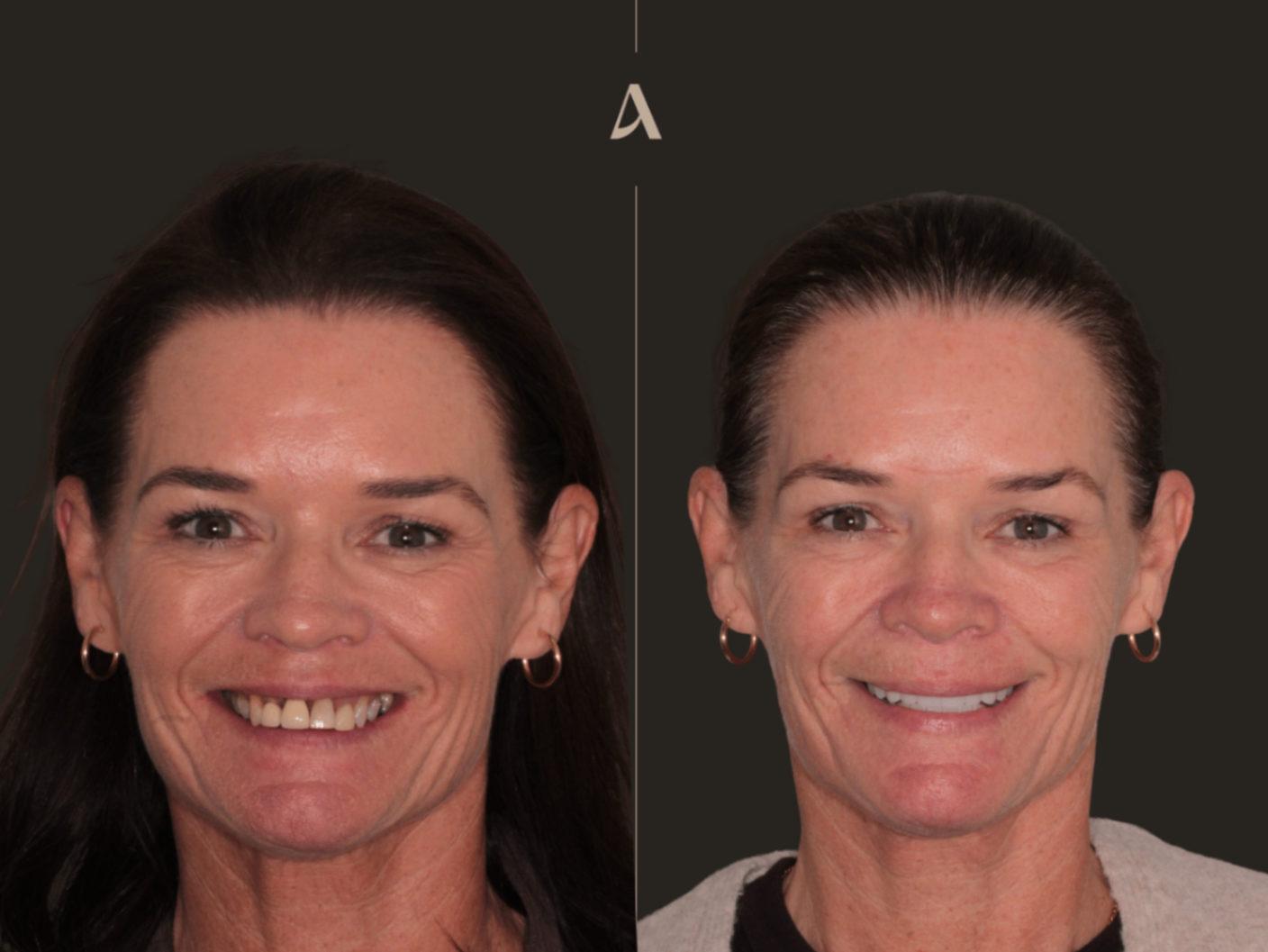
This is a real 5 year full mouth rehab case study from our practice. The patient came in with failed composite veneers in upper and lower arches, that kept chipping and debonding. We replaced them with porcelain (e.max) veneers and crowns, and we raised the height of the bite by about 3mm. The case was delivered between June and August 2021, photographed again at the 3-year review, and reviewed once more this April 2026. The restorations are still intact. The honest finding at 5 years is minor gum recession on the two upper front teeth, which we believe is from brushing pressure.
Key takeaways
Glass ceramic (porcelain) has a flexural strength roughly 3 to 4 times higher than composite resin.
Lithium disilicate veneers show around 98% survival at the 5-year mark in published studies.
Raising the bite height by 2 to 4mm is described in the literature as a predictable approach when full-coverage porcelain is used and the case is planned carefully.
Sensitivity after a bite-height change is common, and in most cases settles over the following months. Timing varies between patients.
The long-term result depends on two things working together: the material we choose and the way you look after it at home.
In this article
Why this patient came to us in 2021
The patient had been living with composite veneers for two years before walking into ArtSmiles. He was tired. The composite kept chipping at the edges, two of the veneers had debonded, and one had a vertical fracture down the front. Every few months, something needed a repair.
He wanted three things from us. Better tooth shape that suited his face. A material that would not keep breaking. And honest information about what the result would actually look like five and ten years down the track.
Two clinical points helped us plan the case. First, there were no signs of teeth grinding (bruxism). The wear patterns were normal for someone in their mid fifties, and the jaw muscles were not enlarged. Second, the patient had realistic expectations. He was not chasing a Hollywood Smile. He wanted teeth that looked natural and held up to everyday life.
That kind of clarity at the start of a case matters. It shaped every decision we made about a full mouth rehabilitation.

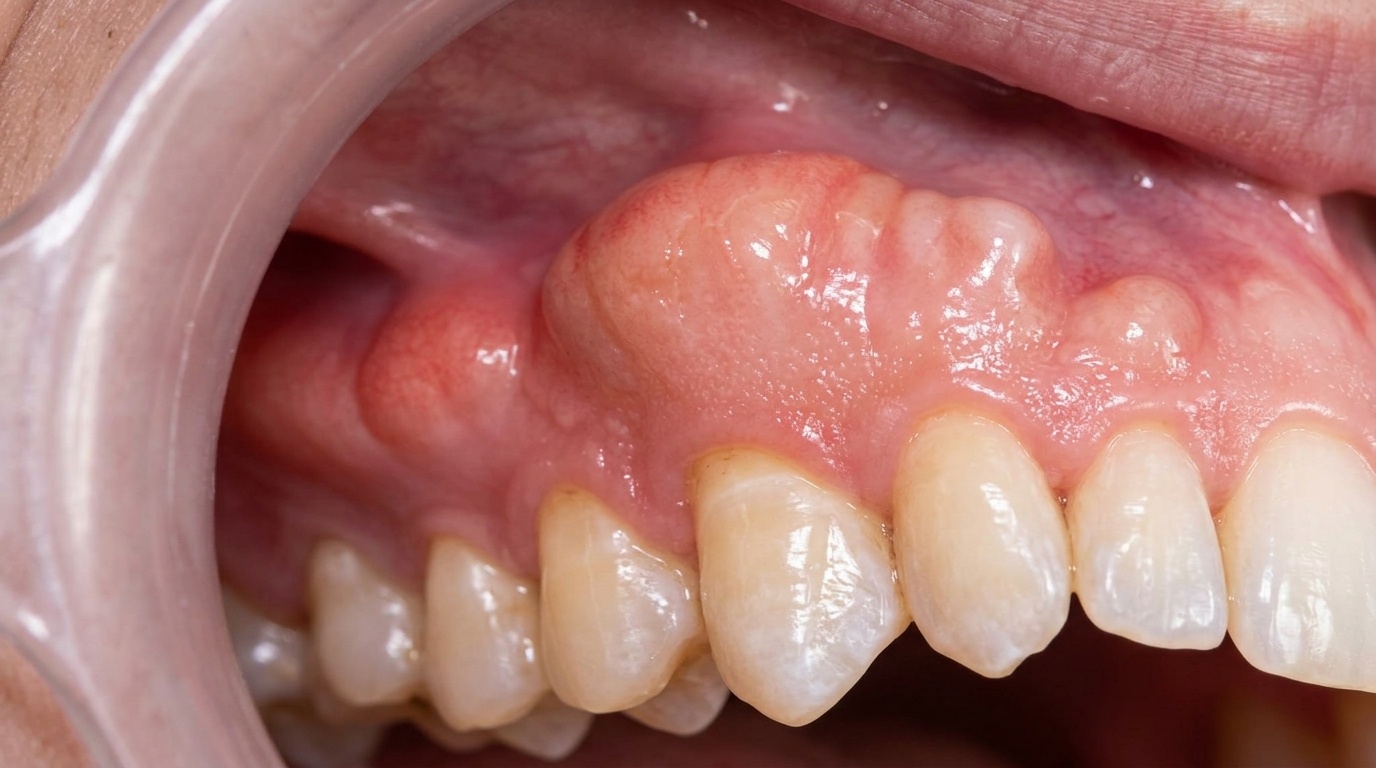
Aspect of the bite showing initial bite and upper arch highlighting veneers with shape deficiency.
Why we chose porcelain instead of more composite
The single biggest reason this case has held so well at 5 years is the material selection. Porcelain is a different category of strength compared to composite.
Here is the plain-language version. Flexural strength is how much bending pressure a material can handle before it cracks. The higher the number, the tougher the material. Composite-based materials sit at around 127 to 140 MPa. Lithium disilicate (the e.max porcelain we used) sits between 360 and 500 MPa, depending on the form and processing. That is roughly 3 to 4 times the strength of composite, as confirmed in Awad and colleagues' comparative flexural strength study.
Survival data lines up with what we see in the chair. A retrospective case series of pressable glass-ceramic (porcelain) veneers showed survival of around 98% at 5 years and 95% at 10 years (Layton and Walton 2019). A 2025 meta-analysis by Klein and colleagues in the Journal of Esthetic and Restorative Dentistry reached similar conclusions across a much larger pooled sample.
Composite, by contrast, is a softer, more forgiving material. It is excellent for small repairs and single-tooth fixes. But across a full mouth, on someone whose previous composite veneers had already failed, it was not the right choice. You can read more in our guide to the materials used for dental veneers and our porcelain veneers service page.
Why we increased the vertical dimension by 3mm
The clinical term is "increasing vertical dimension of occlusion". In plain English, we made the bite taller.
The patient's enamel had worn down over years of normal use. As the biting surfaces got shorter, the lower jaw rotated up slightly, the face shortened, and the front teeth lost their natural proportions. By the time we saw the patient, the bite looked deep and required intervention.
Raising the bite by 2 to 4mm with full-coverage porcelain is described as predictable in the PMC review on increasing vertical dimension of occlusion, provided the case is planned carefully. We chose roughly 3mm based on a digital mock-up and a wax-up that the patient could see and approve before any teeth were prepared.
The result was natural-looking proportions. The centrals matched the laterals again, the canines had room to function, and the molars carried the bite the way they were designed to.
How we delivered the case in 4 stages
We split the treatment across four clear stages between 30 June and 6 August 2021. Our lab partner was Cosmetic Dental Design, and the agreed shade was 1M1.
Stage 1: Digital planning. We started with a digital smile design. The patient saw a photo-realistic preview of the proposed shape and shade, then a physical mock-up was placed in the mouth so they could test-drive the look before we touched any tooth structure.
Stage 2: Crown and veneer preparation. We prepared the upper and lower teeth conservatively. Where we needed strength against biting forces (back teeth and a couple of structurally compromised front teeth), we prepared full crowns and onlays. Where we wanted to preserve as much enamel as possible, we prepared veneers.
Stage 3: Cementation of porcelain restorations. The lab returned the e.max restorations within the planned window. We tried each restoration in and got patient’s approval, then bonded them with a resin cement protocol.
Stage 4: Adjustments and protective night splint. After cementation, we fine-tuned the bite contacts at follow-up visits. We also made a custom night splint to protect the new restorations from any future clenching, even though the patient was not a known grinder. A splint is cheap insurance on a case this size.

Managing post-treatment sensitivity
Any time you change the height of the bite, you change how forces load through each tooth. Sensitivity is a known and well-documented side-effect, with both pulpal and dentinal contributions described in the PMC dentin hypersensitivity etiology review.
Our patient noticed cold sensitivity in the upper and lower premolars during the first three months. It was uncomfortable but not severe. We did three things to manage it.
First, we adjusted the night splint and re-checked the bite at multiple reviews among 6 months. Tiny adjustments can make a big difference. Second, we used infrared low-level laser therapy (LLLT) at three sessions. The evidence for laser therapy in tooth sensitivity is strong. A 2021 review in Clinical Oral Investigations pooled 20 randomised trials and found that patients who received real laser treatment had noticeably less sensitivity than patients who received a placebo, with the gap actually widening over the months that followed. In plain terms: the laser keeps working long after the session ends.
The sensitivity began to ease at the 3-month mark and was gone by 8 to 10 months. That timeline is normal, and we set the expectation up front so the patient was not surprised.
3-year follow-up (April 2024)
At the 3-year review, the photos told a calm story. No chips on any of the porcelain. No debonded units. No fractures. The gums looked pink and healthy around every margin.
Plaque scores were excellent. The patient had stayed on top of cleaning, attended every 6-month review, and was wearing the night splint regularly. The bite was stable and the restorations were behaving the way the published 3-year data would predict.

5-year follow-up (April 2026)
This month we saw the patient again for the 5-year review. The good news first. All restorations are intact. No fractures, no debonds, no porcelain chips, and no evidence of marginal breakdown on radiographs. That is consistent with the 95 to 98% survival rates reported in the lithium disilicate literature.
Now the honest finding. We documented minor gum recession on teeth 11 and 12, the two upper incisors on the left side of the photo. The recession is small, around 0.5 to 1mm, but it is new since the 3-year review. The veneers margins are appearant now, due to the recession.
When we worked through the likely causes, the most plausible explanation was brushing technique. The patient had been brushing harder, particularly on the upper front teeth. Toothbrushing force above 3N combined with medium or hard bristles is associated with cervical abrasion and gingival recession, as discussed in this 2025 narrative review on toothbrushing and recession.
Three things changed at the visit. We coached technique with a pressure-sensing brush. We swapped the patient back to a soft-bristle brush. And we applied a fluoride desensitiser at the cervical margins of 11 and 12 to support those exposed root surfaces.
We will photograph and re-measure at the 6-12 month review to make sure the recession has stabilised.

What this 5-year case tells us about long-term cosmetic dentistry
Looking back at the case file, four things are worth pulling out.
Material choice does more than change how the teeth look. The same shape and shade can be carved in composite or pressed in lithium disilicate, but the 5-year story those two materials tell is very different. For full-mouth work, porcelain earns its place.
Vertical dimension can be opened predictably, but only when the planning and the material choice line up, with a night splint to protect the work. A 3mm increase is not a casual decision. It is a planned one, with a digital mock-up the patient signs off on before any tooth is touched.
Home care is part of the result. The reason this case still looks good at 5 years is partly the material and partly what the patient does at the bathroom sink twice a day. When that home care drifted, even slightly, we saw it in the gum tissue.
Honestly, the gum recession was a useful reminder of why we keep these reviews going. The restorations themselves were doing their job. The small adjustment we needed to make was on the home-care side. That is the real value of long-term reviews: pretending nothing changes between year 0 and year 5 would be misleading, and small findings get caught earlier when you keep looking. You can see other long-term cases in our clinical case gallery, our full mouth rehabilitation case for a patient with bruxism, and our full mouth restoration case for grinding damage.
Disclaimer
This article documents one patient's treatment at ArtSmiles. It is shared for educational purposes with the patient's written consent. Individual results vary and depend on factors including oral health, bone and gum condition, general medical history, and how well the restoration is maintained after treatment. Nothing in this article is a guarantee of outcome, a substitute for a clinical examination, or advice specific to your case. Any treatment carries risks and potential complications, which will be explained to you at consultation.
Before starting any dental treatment, book a consultation so we can assess your teeth, gums, and bone in person, take the imaging we need, and discuss the options, timelines, and costs that apply to your situation.
Case executed by Dr Cristian Dunker
General Dentist
AHPRA DEN0002257085
ArtSmiles, Southport, Gold Coast
Frequently asked questions
How long do porcelain veneers last compared to composite?
Porcelain (lithium disilicate) veneers typically last around 10 years, with published survival rates near 98% at 5 years and 95% at 10 years for pressable porcelain. Composite veneers tend to last 4 to 7 years before needing a meaningful repair, polish, or replacement. The difference comes down to material strength. Porcelain handles roughly 3 to 4 times the bending pressure of composite before cracking. That said, composite is still a great choice for small touch-ups, single-tooth work, or patients who want a low-cost starting point.
Is it safe to raise the bite with veneers and crowns?
Yes, when it is planned carefully and the right material is used. Raising the bite by 2 to 4mm with full-coverage lithium disilicate is described as predictable in the published literature. The keys are a digital mock-up so the patient can preview the result, full-coverage restorations on the back teeth to handle the new loading, and a protective night splint after delivery. Some short-term sensitivity is common in the first few months and usually settles over the following months.
Why do some patients get sensitivity after a full mouth rehab?
When the height of your bite changes, the forces running through each tooth change too. The nerves inside the teeth respond to that new loading pattern, and you can feel it as cold sensitivity, pressure sensitivity, or a low-grade ache. It is not a sign that anything is wrong. In most cases it eases at the 3-month mark and resolves within several months. We help it along with bite adjustments, a night splint, low-level laser therapy, and a fluoride desensitiser at home if needed.
What does maintenance look like after a full mouth rehab?
Three things matter most. Brush twice a day with a soft-bristle brush and gentle pressure, no scrubbing. Floss or use interdental brushes daily so the gum margins around the restorations stay clean. Wear the protective night splint we make for you, every night, even if you do not think you grind. On top of that, attend a 6-monthly review so we can take photos, check the bite, polish the porcelain, and pick up small changes early. Maintenance is the reason these cases hold up.
Can my gums recede after getting veneers?
Yes, gums can recede after veneers, but it is rarely caused by the veneers themselves. The most common cause is brushing too hard or using a brush with stiff bristles. Toothbrushing force above 3N combined with medium or hard bristles is linked to gum recession in the literature. Other causes include grinding, gum disease, and natural ageing. If you do notice recession, it can be managed by correcting brushing technique, swapping to a soft-bristle brush, and applying a fluoride desensitiser at the exposed margin.
If you are thinking about replacing failing veneers, or you want to understand what a full mouth case might look like for you, we offer a complimentary cosmetic consultation where we can talk through options, materials, and realistic timelines. There is no obligation to proceed.
Written by Dr Cristian Dunker, principal dentist at ArtSmiles Cosmetic Dentistry, Southport.
Medically reviewed by Dr Cristian Dunker.