Compiled from clinical pathology references. Medically reviewed by Dr Cristian Dunker , Principal Dentist, ArtSmiles Cosmetic Dentistry.
Quick summary
Also called | EM, redness (erythema) multiforme minor, erythema multiforme major (when more severe) |
How urgent? | 🔴 See a dentist or doctor promptly, the sudden onset, painful mouth ulcers, and crusted lips need assessment, especially if eyes or skin are also involved |
Common or rare? | Uncommon, but well recognised |
Who it affects | Most often young adults in their 20s and 30s, with a slight male predominance |
Who treats it | General dentist working alongside a GP or dermatologist; severe cases may need hospital care |
Based on | Regezi, Neville, Cawson, Laskaris |
What is it?
Erythema multiforme is a sudden, short-lived reaction of the skin and the lining of the mouth. It typically shows up as widespread mouth ulcers, badly cracked and crusted lips, and a distinctive ring-shaped rash on the hands and arms. Despite how dramatic it can look, the condition is usually self-limiting and tends to settle within two to six weeks.
Who tends to get it?
Erythema multiforme most commonly affects young adults in their 20s and 30s, although it can occur at any age. Men are affected slightly more often than women. Many people who develop it are otherwise healthy, and episodes often appear in spring or autumn. Around 25% of people who experience it will have it return at some point, sometimes more than once over a year or two.
When the mouth is involved, anywhere from a quarter to two-thirds of patients with the skin form will also develop oral lesions. In some patients, the mouth is the only site affected, which is why a dentist is often the first clinician to recognise it.
What causes it?
Erythema multiforme is a hypersensitivity reaction, the body's immune system overreacts to a trigger and attacks its own skin and mouth lining (mucosa) in the process. A trigger can be identified in roughly half of cases, and the most common ones are:
Herpes simplex virus (HSV) infection, the single most frequent trigger, particularly for recurrent episodes. The cold sore comes first, and the erythema multiforme follows a few days later. Sophisticated DNA testing has confirmed herpes virus material in the lesions of patients with recurrent disease.
Mycoplasma pneumoniae infection, a particular type of chest infection (sometimes called 'walking pneumonia') that can trigger an episode, especially in younger patients.
Medications, sulphonamide antibiotics, anticonvulsants such as carbamazepine and phenytoin, barbiturates, and certain pain relievers (including some NSAIDs and aspirin) are recognised triggers.
Less common triggers, other infections such as tuberculosis or histoplasmosis (a fungal lung infection), vaccinations, autoimmune disease, malignancy, and radiotherapy have all been reported.
In many cases, however, no trigger is ever identified. This does not mean the condition is imagined, it simply means the immune trigger remains unknown.
How does it develop?
Think of erythema multiforme as a case of mistaken identity inside the immune system. A virus, a medication, or another trigger leaves behind protein fragments that look, to the immune system, a little too similar to proteins on the lining of the skin and mouth. The immune system targets those proteins, and the small blood vessels and surface cells underneath get caught in the crossfire.
The surface cells start to die off in patches. Tiny blisters form just beneath the skin or mouth lining, then break open to leave the shallow ulcers and crusted lips that give the condition its appearance. The reaction is intense but limited, once the trigger has passed and the immune system calms down, the tissue heals.
What might you notice?
What it looks like
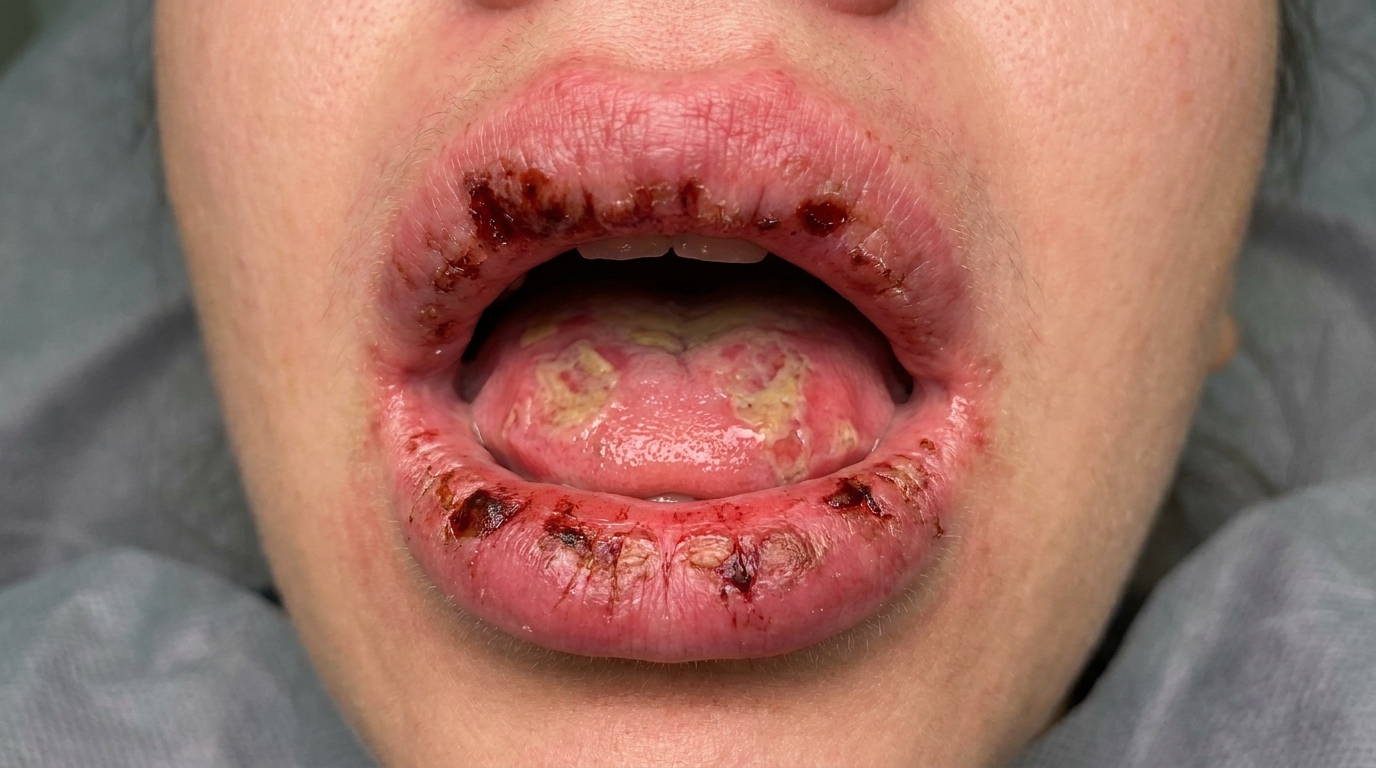
The most recognisable sign is the lips. They often become swollen, split, and covered in a thick blood-stained crust that bleeds when disturbed. Inside the mouth, you may see widespread shallow ulcers with irregular, ragged edges, most often on the lips, inside the cheeks, the tongue, and the soft palate. The gums and the hard palate are usually spared, which helps distinguish it from other conditions.
On the skin, the classic clue is the target lesion, a round red patch a centimetre or more across, with concentric rings that look like a bullseye or an archery target. These typically appear on the hands, forearms, palms, and feet in a symmetrical pattern. In milder cases there may be only patchy redness; in more severe cases, blisters can form in the centre of the targets.
What it feels like
The oral lesions are genuinely painful. Eating, drinking, and even talking can be uncomfortable, and some patients become dehydrated simply because swallowing hurts too much. Many people also feel generally unwell in the days leading up to the rash, with fever, headache, sore throat, cough, and muscle aches, a flu-like prodrome (early warning symptoms) that arrives roughly a week before the lesions appear.
What an X-ray might show
X-rays are not used to diagnose erythema multiforme, because the condition affects only the soft tissues. The diagnosis is made from the clinical picture.
What happens at the dentist?
The diagnosis of erythema multiforme is largely a clinical one, meaning your dentist or doctor recognises it from the pattern of signs and symptoms rather than from a single laboratory test.
At an appointment with ArtSmiles, your dentist may:
Take a careful history, asking about recent cold sores, chest infections, new medications, and previous similar episodes.
Examine the mouth and lips closely, looking for the characteristic crusted lips, ragged ulcers, and the typical sparing of the gums and hard palate.
Inspect the skin, particularly the hands and forearms, for target lesions.
Check the eyes and other mucosal sites, or refer to a GP or specialist if eye, genital, or airway involvement is suspected.
Consider a biopsy (a small tissue sample sent to the lab for testing) in less typical cases. The microscopic appearance is suggestive, although it cannot confirm the diagnosis on its own. A biopsy is more often used to rule out other blistering diseases such as pemphigus or pemphigoid.
If the presentation is severe, or if more than one mucosal site is involved, prompt referral to a dermatologist or hospital is appropriate. Severe forms can affect the eyes and lead to long-term scarring if not managed early.
Is this serious?
🔴 See a dentist or doctor promptly. The mild form of erythema multiforme, sometimes called erythema multiforme minor, is uncomfortable but not dangerous, and usually settles in 2,6 weeks. It is not contagious, even when herpes is the underlying trigger.
The more severe form, erythema multiforme major, involves widespread skin lesions plus two or more mucosal sites (mouth, eyes, genitals). When the eyes are involved, scarring of the conjunctiva (the clear membrane covering the white of the eye) can affect vision if it is not managed early. Patients who cannot eat or drink because of mouth pain may need fluids through a drip.
A closely related but distinct group of conditions, Stevens-Johnson syndrome and toxic epidermal necrolysis, sit at the most serious end of this spectrum. They are almost always triggered by medications, cause large areas of skin to slough off, and require hospital care, often in a burns unit. Modern pathology textbooks now consider these to be a separate disease process from erythema multiforme, even though they were once grouped together.
If you've noticed sudden mouth ulcers, crusted lips, or a target-shaped rash on your hands, it's worth booking an assessment promptly, particularly if your eyes are red or sore, or if you've recently started a new medication.
Could it be something else?
Several conditions can resemble erythema multiforme in the mouth, and your dentist will work through these as part of the diagnosis.
Primary herpes simplex (herpetic gingivostomatitis), also causes painful mouth ulcers and lip crusting. It tends to affect children rather than young adults, the ulcers are smaller and clustered, and the gums are typically inflamed (which is unusual in erythema multiforme). Target skin lesions are absent.
Aphthous ulcers (canker sores), can be widespread but are usually round, well-defined, and limited to non-keratinised mucosa. They lack the lip crusting and skin rash.
Pemphigus vulgaris, also causes oral blisters and erosions, but tends to affect older adults, develops more slowly, and is confirmed by characteristic immunofluorescence (a special lab stain that highlights immune-system markers in tissue) on biopsy.
Mucous membrane pemphigoid, typically affects the gums (desquamative gingivitis, where the gum surface peels and reddens, looking sore and raw) and progresses gradually rather than appearing suddenly.
Paraneoplastic pemphigus, a rare blistering disease linked to underlying cancer; biopsy and antibody tests distinguish it.
Erosive lichen planus, usually has lacy white striae (fine lace-like white lines) alongside the red, raw areas, and runs a chronic rather than acute course.
Stevens-Johnson syndrome and toxic epidermal necrolysis, sit at the severe end of the spectrum, are almost always drug-induced, and involve much larger areas of skin sloughing.
Stomatitis medicamentosa (drug reaction in the mouth), a generic drug reaction can mimic erythema multiforme; a careful medication history and timeline help separate them.
Kawasaki disease, in young children, fever with cracked lips and a rash can superficially resemble erythema multiforme but has its own characteristic features and needs urgent paediatric review.
Reiter's disease (reactive arthritis), can produce oral lesions but is accompanied by joint and urinary symptoms.
Discoid lupus erythematosus, chronic, with characteristic skin and oral plaques rather than acute ulcer formation.
How is it treated?
Treatment depends on how severe the episode is and whether a trigger can be identified.
At home, while you are unwell:
Keep the mouth clean with bland, non-alcoholic mouth rinses such as warm salt water.
Drink plenty of fluids, even if it is only sips at a time, to avoid dehydration.
Stick to soft, cool, bland foods. Avoid acidic, spicy, salty, or crunchy foods that sting.
Use a soft-bristled toothbrush and continue gentle oral hygiene wherever possible.
Avoid kissing or sharing utensils if a cold sore was the trigger, herpes itself is contagious, even though erythema multiforme is not.
Professional treatment may include:
Identifying and removing the trigger, if a medication is suspected, your doctor may stop or switch it. If herpes simplex is the trigger, this is addressed directly.
Symptomatic care, topical anaesthetic gels or rinses to ease eating, and pain relief as advised.
Topical corticosteroids (anti-inflammatory gels or rinses applied directly to the mouth), sometimes prescribed for mouth lesions in more troublesome cases, occasionally combined with an antifungal.
Systemic corticosteroids (steroid tablets that work throughout the body), may be considered in severe cases, although the evidence is mixed and the decision is individualised.
Antiviral suppression, for patients with frequent recurrences linked to herpes simplex, a daily antiviral such as aciclovir or valaciclovir can prevent further episodes.
Hospital admission, for the severe end of the spectrum, particularly when patients are dehydrated, when the eyes are affected, or when Stevens-Johnson syndrome or toxic epidermal necrolysis is suspected. Care may include intravenous fluids, eye review by an ophthalmologist, and burns-unit-style management.
A single episode usually settles in two to six weeks. Healing of the mouth tends to follow the skin and may take a little longer.
What's the long-term outlook?
For most people, erythema multiforme is a one-off or occasional event that fully resolves and leaves no lasting damage to the skin or the lining of the mouth. It does not turn into anything more serious in its minor form.
Around 20% to 25% of patients will have recurrent episodes, often in spring or autumn. When recurrences are frequent and herpes simplex is the trigger, ongoing antiviral therapy can dramatically reduce, or even prevent, further attacks. Identifying and avoiding any drug triggers is equally important.
The outlook is more guarded for the severe end of the spectrum. Erythema multiforme major, when it involves the eyes, can occasionally cause lasting scarring of the conjunctiva and visual impairment if not treated early. Stevens-Johnson syndrome and toxic epidermal necrolysis are rare, serious conditions with significant mortality risk and require urgent hospital care, but they are now considered separate diseases rather than the worst form of erythema multiforme itself.
The key takeaway: if your lips suddenly crust and bleed, if widespread mouth ulcers appear over a few days, or if a target-shaped rash develops on your hands, see a dentist or doctor promptly. Early recognition makes a real difference to comfort and to outcome.
A note on this article
This article is for educational purposes only and does not constitute a clinical diagnosis. Please consult a registered dental practitioner for assessment and treatment advice.
References
Regezi, J. A., Sciubba, J. J., & Jordan, R. C. K. (2017). Oral pathology: Clinical pathologic correlations (7th ed.). Elsevier. Chapter 2, Ulcerative Conditions, pp. 44,47.
Neville, B. W., Damm, D. D., Allen, C. M., & Chi, A. C. (2023). Oral and maxillofacial pathology (5th ed.). Elsevier. Chapter 16, Dermatologic Diseases: Erythema Multiforme and Stevens-Johnson Syndrome / Toxic Epidermal Necrolysis, pp. 781,784.
Cawson, R. A., & Odell, E. W. (2017). Cawson's essentials of oral pathology and oral medicine (8th ed.). Elsevier. Chapter 13, Diseases of the Oral Mucosa: Non-infective Stomatitis, pp. 235,236.
Laskaris, G. Pocket atlas of oral diseases. Thieme. Chapter 22, Skin Diseases: Erythema Multiforme, pp. 198,199.