Some people delay dental care because nothing hurts. Others because life gets busy, finances are tight, or priorities shift.
What many don't realise is that untreated dental disease doesn't stay confined to the mouth. Chronic oral inflammation can influence the entire body — often without obvious warning signs.
This article explains that connection, grounded in current clinical research.
Your Mouth Is Connected to the Rest of Your Body
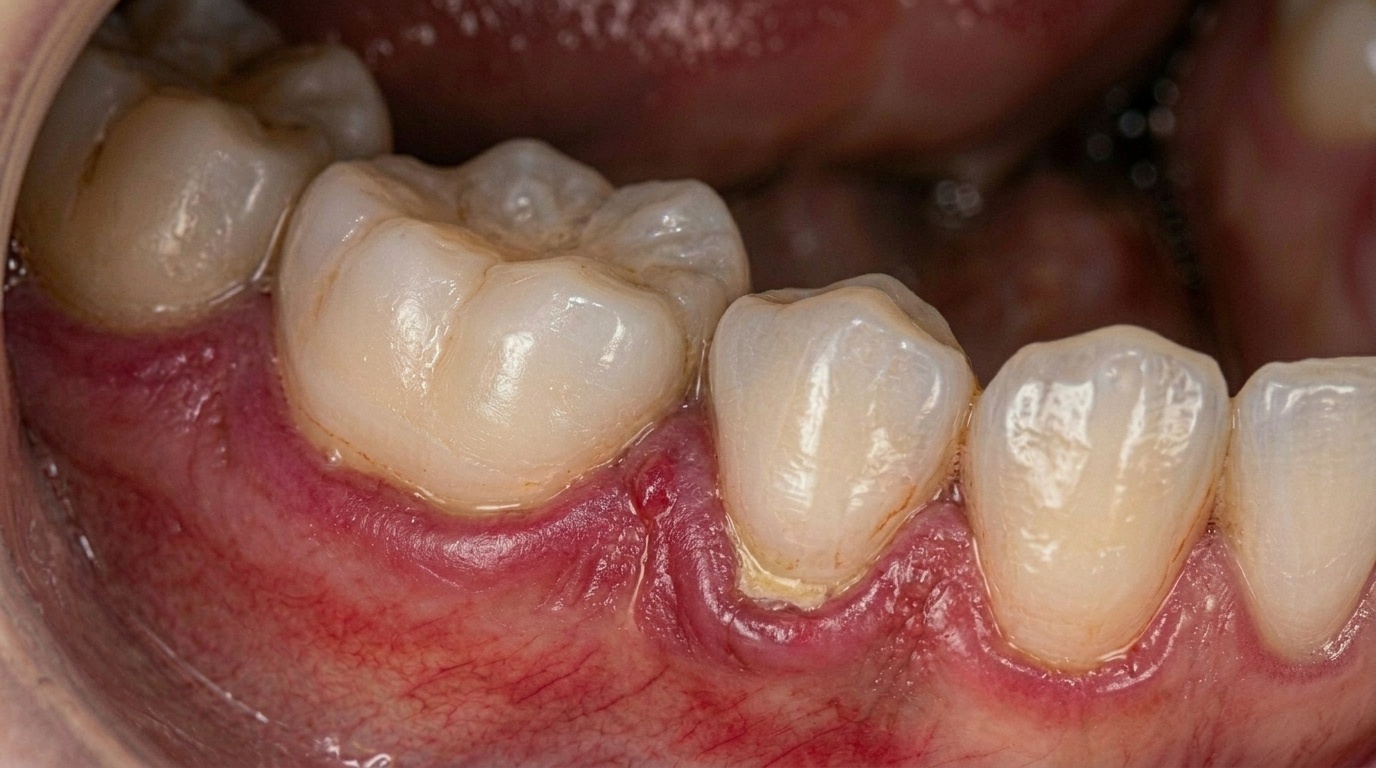
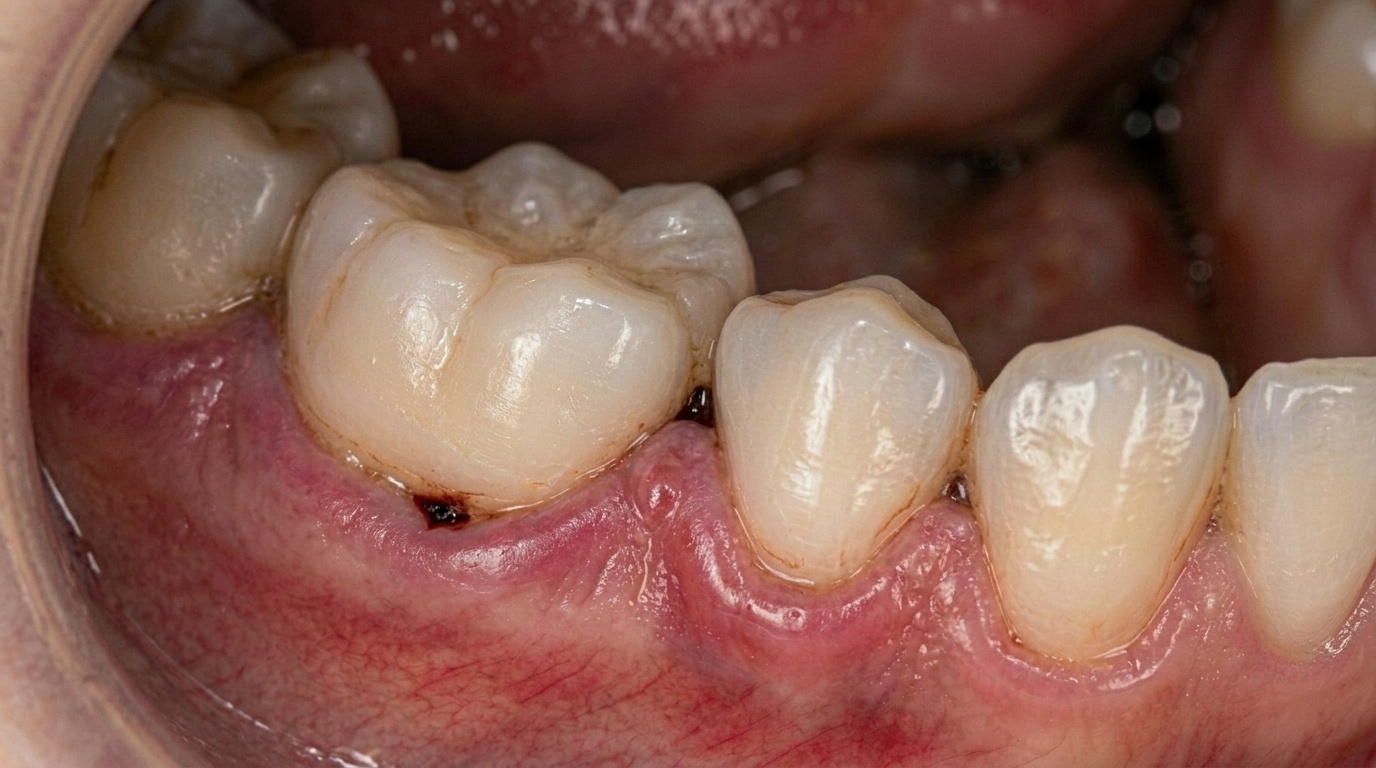
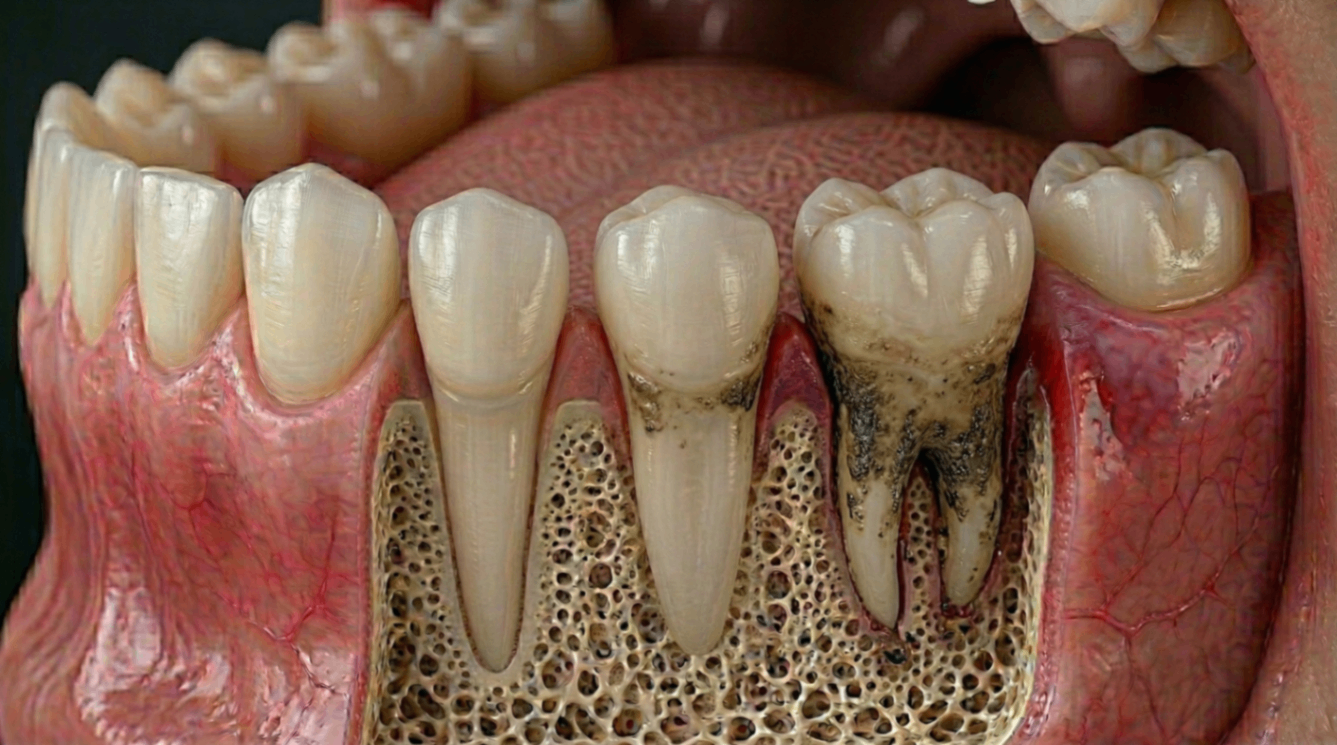
The mouth is directly linked to your immune system and bloodstream. When gum disease develops, it doesn't just affect the gums. Inflammation begins in the soft tissue, progresses into deeper structures, and eventually attacks the supporting bone.
Throughout that process, your immune system stays constantly activated. Periodontitis is now recognised not as a local dental problem, but as a chronic inflammatory disease with measurable effects on overall health.
How Oral Inflammation Moves Beyond the Mouth
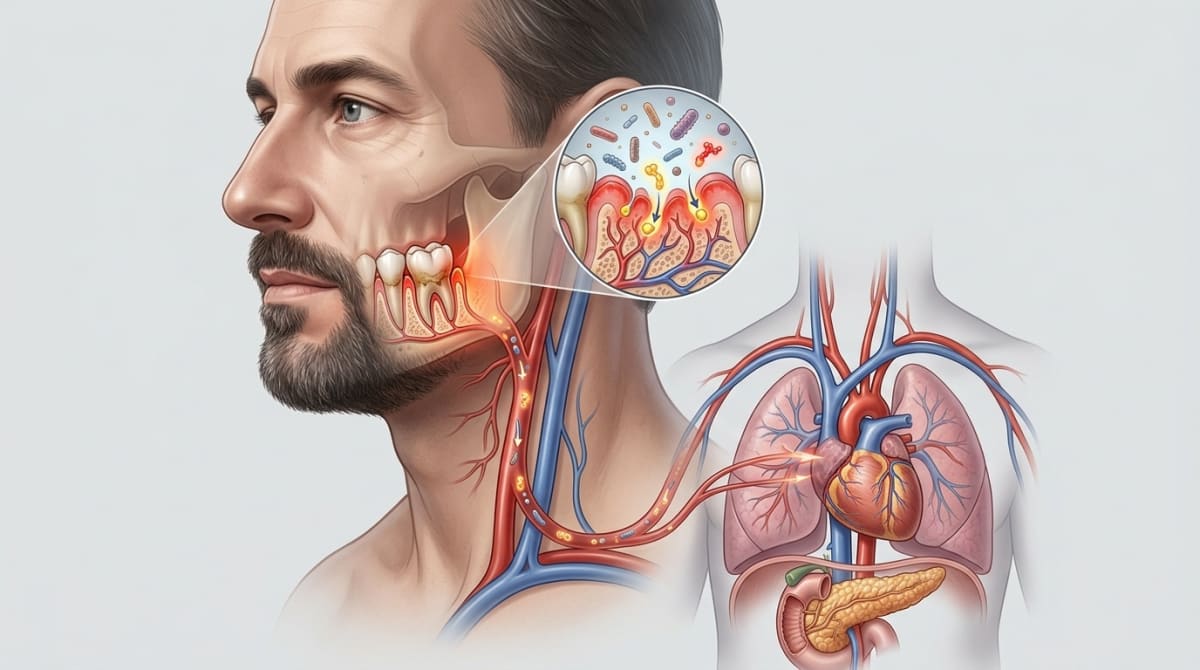
When bacteria accumulate in gum pockets, the body releases inflammatory mediators into the bloodstream — including:
Interleukin-6 (IL-6)
Tumour necrosis factor alpha (TNF-α)
C-reactive protein (CRP)
These same markers are associated with cardiovascular disease, diabetes complications, arthritis, and cognitive decline. Patients with untreated gum disease often show elevated CRP — a well-established indicator of systemic inflammatory activity and cardiovascular risk.
Gum Disease and Heart Health
The link between periodontal disease and heart disease is one of the most studied areas in oral-systemic medicine. A landmark clinical trial by Tonetti et al. (2007) found that treating periodontitis led to significant improvements in endothelial function — the inner lining of blood vessels — within six months.
The mechanism is thought to involve oral bacteria entering the bloodstream, chronic inflammation damaging blood vessel walls, and immune responses accelerating arterial plaque formation. A 2020 consensus report by Sanz et al., published in the Journal of Clinical Periodontology, further confirmed the association between periodontitis and cardiovascular diseases across multiple research programmes.
Diabetes and Gum Disease: A Two-Way Relationship
Diabetes increases susceptibility to gum inflammation, and gum disease makes blood sugar harder to manage. This two-way cycle is well documented in the literature.
A Cochrane systematic review by Simpson et al. (2022) found that periodontal treatment led to a clinically meaningful reduction in HbA1c levels in people with diabetes — comparable to adding a second medication. Delaying dental care may quietly undermine diabetes management without any obvious dental symptoms.
The Immune System Under Persistent Strain
When infection persists in the mouth, immune pathways stay active long term. Over time, this can contribute to:
Ongoing fatigue
Higher overall inflammatory load
Slower wound healing
Greater vulnerability to illness
For patients already managing autoimmune or inflammatory conditions, untreated gum disease adds unnecessary strain to an already busy immune system.
Symptoms You Might Not Connect to Oral Health
Many patients don't associate these experiences with their mouth, but they often are related:
Waking up tired despite adequate sleep
Dull or recurring headaches
Persistent bad breath or taste
Swollen or sensitive gums
Difficulty chewing comfortably
Low-grade facial or jaw swelling
These aren't just dental concerns — they can reflect systemic inflammatory strain that started in the mouth.
Treating Oral Inflammation Has Benefits Beyond the Mouth
The same research that established the oral-systemic link also shows that treatment works. Managing gum disease has been associated with:
Lower levels of systemic inflammatory markers
Improved blood sugar control in diabetic patients
Better endothelial (blood vessel) function
Reduced oral discomfort and bleeding
At ArtSmiles, periodontal care typically begins with a deep cleaning (scaling and root planing) to remove bacterial deposits from beneath the gum line. This is usually followed by a tailored maintenance programme to keep inflammation under control long term.
Scientific References
Tonetti MS, D'Aiuto F, Nibali L, et al. Treatment of Periodontitis and Endothelial Function. N Engl J Med. 2007;356(9):911–920.
Sanz M, Marco Del Castillo A, Jepsen S, et al. Periodontitis and cardiovascular diseases: Consensus report. J Clin Periodontol. 2020;47(3):268–288.
Simpson TC, Clarkson JE, Worthington HV, et al. Treatment of periodontitis for glycaemic control in people with diabetes mellitus. Cochrane Database Syst Rev. 2022;4:CD004714.
If dental care has been on hold, addressing oral inflammation is one of the most meaningful steps you can take for your overall health — not just your teeth. When you're ready, the team at ArtSmiles Gold Coast is here to guide you back into care, clearly and without pressure. Book online at a time that suits you.