Tooth decay is one of the most common dental problems in the world, but it's also one of the most preventable. Whether you're dealing with an early cavity or trying to stop decay from getting worse, there are clear steps you can take to protect your teeth and keep your smile healthy.
In this article, we'll walk you through what causes tooth decay, how it's treated at different stages, and what you can do at home to reduce your risk.
On this page
What Causes Tooth Decay?
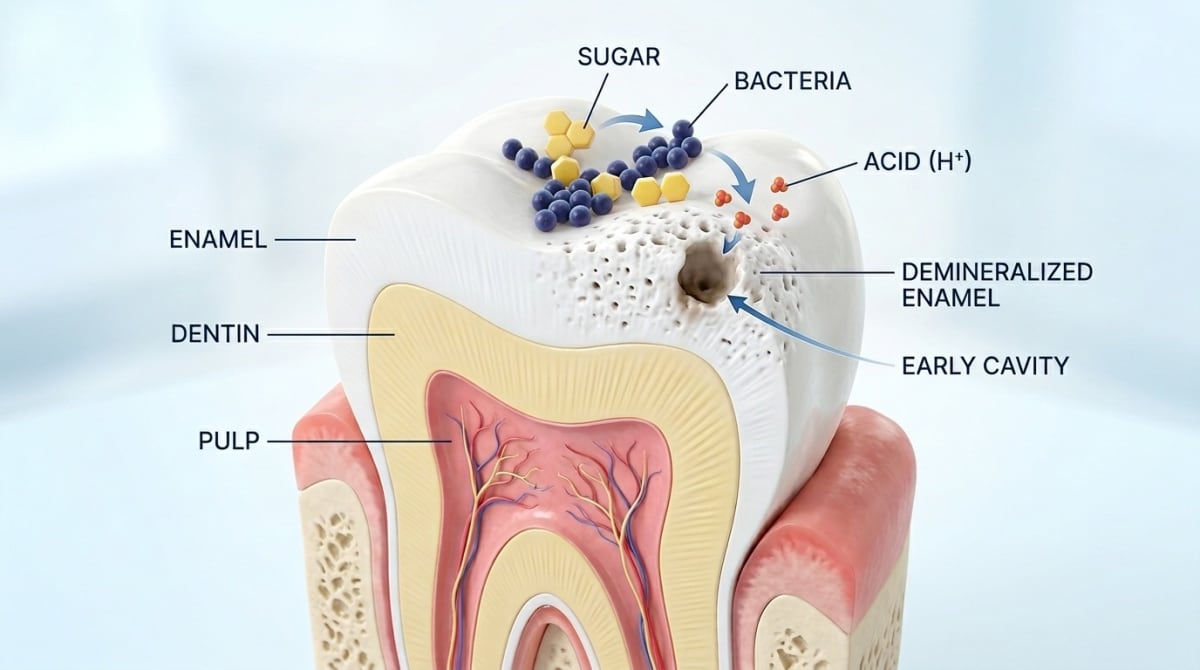
Tooth decay (also called dental caries) happens when bacteria in your mouth feed on sugars from food and drink, producing acids that gradually dissolve the hard outer layer of your teeth (enamel). Over time, this creates a cavity, a small hole in the tooth that can grow deeper if left untreated.
A foundational study by Selwitz et al. (2007) published in The Lancet confirmed that dental caries is a diet-dependent disease driven by the interaction between oral bacteria, fermentable carbohydrates, and time. The good news is that because the process is well understood, it can be interrupted at every stage.
How to Prevent Tooth Decay
Watch your sugar intake
Sugar is the main fuel for decay-causing bacteria. This doesn't mean you can never have a treat, but being aware of how often you consume sugary foods and drinks throughout the day makes a real difference. It's the frequency of sugar exposure, not just the amount, that matters most.
Try keeping a food diary for a few days and sharing it with your dentist. You might be surprised by hidden sugars in things like juice, flavoured yoghurt, or cereal.
Brush twice a day with fluoride toothpaste
Fluoride strengthens enamel and helps reverse the very earliest stages of decay. For most adults, a regular fluoride toothpaste (1,000 ppm) is sufficient. If your dentist identifies you as high risk for cavities, they may recommend a prescription-strength fluoride toothpaste (5,000 ppm) for a period of time.
Brush for at least two minutes, focusing on all surfaces of your teeth, especially along the gum line where plaque tends to build up. After brushing, spit out the excess toothpaste but don't rinse with water, because you want the fluoride to stay on your teeth and keep working.
Floss every night
Cavities frequently develop between teeth where your toothbrush can't reach. Daily flossing removes the plaque and food debris from these areas before bacteria have a chance to cause damage. Another good alternative for interdental cleaning is a waterflosser. Between-meal sugar-free gum with xylitol can also help neutralise acid and boost saliva flow, which is your body's own anti-cavity system.
Visit your dentist regularly
How often you need to visit depends on your risk level:
Low risk: Once a year may be enough
Moderate risk: Every 6 months is recommended
High risk: Every 3 to 4 months for closer monitoring
Your dentist can assess your personal risk based on your history, diet, saliva quality, and existing dental work. If you're on medication that causes a dry mouth, mention it at your next appointment, because reduced saliva can sharply increase your cavity risk.
Can You Treat Tooth Decay at Home?
We get asked this most weeks, usually by people who already suspect something is wrong but aren't quite ready to pick up the phone. It's worth being honest about what home care can and can't do, so you can make a sensible call about what to do next.
Good home care is powerful for preventing decay and for stopping the earliest stage in its tracks. It is not powerful enough to fix a cavity once one has formed. Knowing which side of that line you're on is what matters.
What home care can't do
Once the enamel has broken and a cavity has formed, no amount of home care will rebuild the missing tooth. Enamel is the hardest tissue in your body, but it doesn't regrow. You can't scrub a cavity out, you can't dissolve it, and you can't fill it with anything you'd find in a pharmacy or supermarket. Untreated cavities won't fix themselves, and the longer you wait, the more tooth you tend to lose.
Home remedies that don't work for established cavities
A quick word on the remedies that pop up in online searches:
Oil pulling doesn't fill cavities. It may have mild effects on plaque but doesn't treat decay.
Charcoal toothpaste is abrasive. It can scratch enamel and make things worse over time.
Baking soda alone has no fluoride, so you lose the main benefit of modern toothpaste.
Cloves or clove oil can temporarily numb a painful tooth but don't treat the cavity underneath.
Crushed garlic, turmeric pastes, and bentonite clay "tooth powders" have no credible evidence for reversing cavities.
None of these are a substitute for treatment, and some actively damage enamel.
Is there a medicine for tooth decay?
There isn't a tablet you can take that reverses decay. What does exist are two in-chair options your dentist can apply directly to the tooth: silver diamine fluoride (SDF), a liquid that can arrest early decay in some situations (it stains the decayed area black, so it's used most often on baby teeth or back teeth), and high-concentration fluoride varnish, painted on to help remineralise very early decay. The evidence base for SDF in arresting caries is reasonably strong (Seifo et al. 2019 umbrella review). For high-risk adults, your dentist may also prescribe a high-concentration fluoride toothpaste (typically around 5,000 ppm), a step that's backed by a Cochrane review on fluoride toothpaste concentrations. Both SDF and fluoride varnish are applied in the dental chair, not at home.
Can You Fix Tooth Decay? Fix vs Reverse vs Treat
People use "fix", "reverse", and "treat" as if they mean the same thing, but they don't, and the difference matters when you're deciding what to do about a tooth.
Reverse applies only to the very earliest stage, before a cavity has formed. With fluoride, saliva, and dietary changes, your tooth can remineralise and early decay can disappear. This window closes the moment the enamel breaks.
Treat is broader. You can treat tooth decay at any stage, meaning stopping it from progressing, protecting the rest of your mouth, and relieving any pain.
Fix means restoring the damaged tooth itself. Once a cavity has formed, the missing structure has to be rebuilt with a composite filling, an onlay, or a crown. If decay has reached the nerve, fixing the tooth means root canal treatment followed by a crown. A cavity can't un-cavity itself.
The Stages of Tooth Decay and How Each Is Treated
Tooth decay doesn't happen all at once. It moves through stages, and knowing where yours is on that path tells you what treatment is most likely.
Stage 1: Enamel demineralisation (white-spot lesion)
Acid from plaque has started to draw minerals out of the enamel, leaving a chalky white or dull patch. There's no pain, and the surface is still intact. This is the one stage where decay can be reversed with fluoride, dietary changes, and careful cleaning. In-chair fluoride varnish is often used to speed remineralisation. Average cost: a check-up ($80 to $140) plus a varnish application.
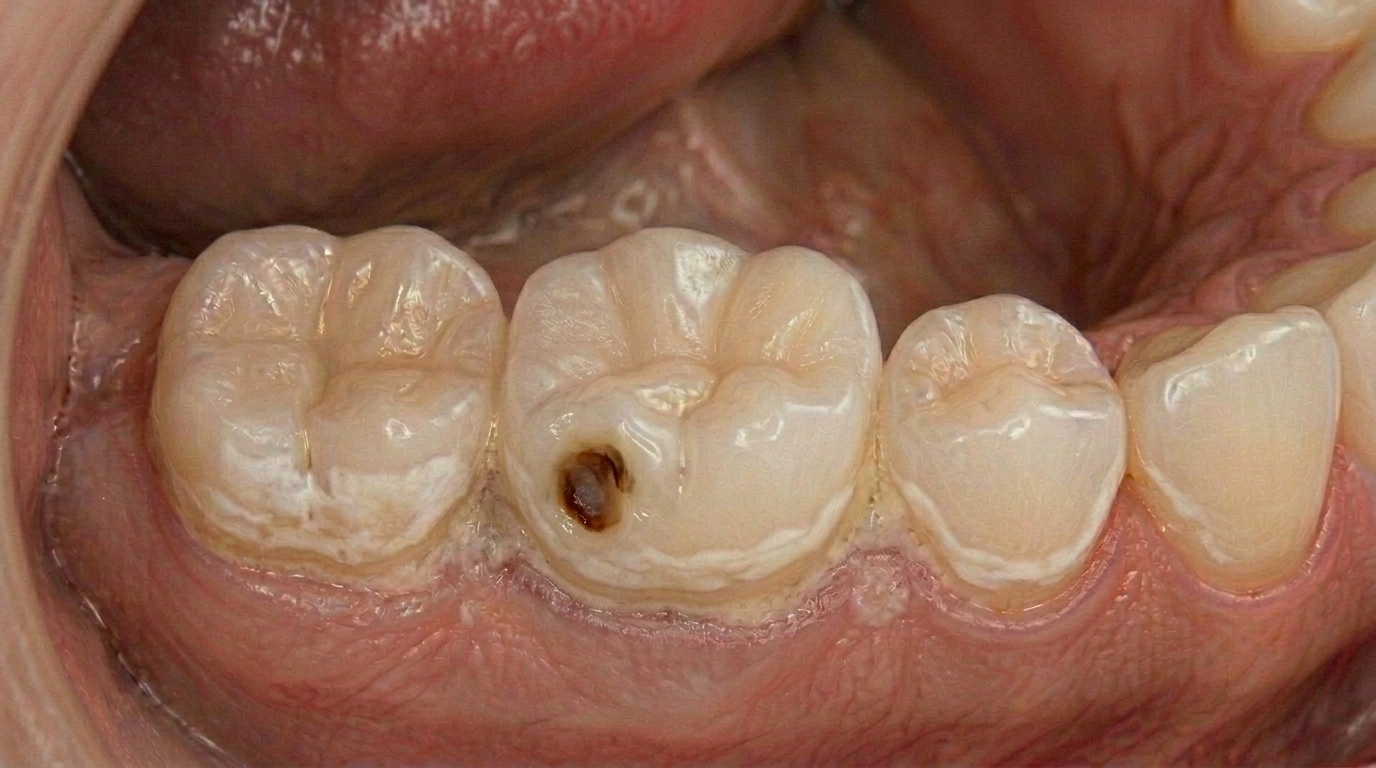
Stage 2: Enamel decay (small cavity forms)
The enamel has broken and a small pit or rough edge has appeared. You might feel it with your tongue or notice food catching. There's rarely pain yet, which is why cavities at this stage are picked up at a check-up rather than because you noticed them. A straightforward composite filling is the standard treatment. Cost: $180 to $320 per tooth.
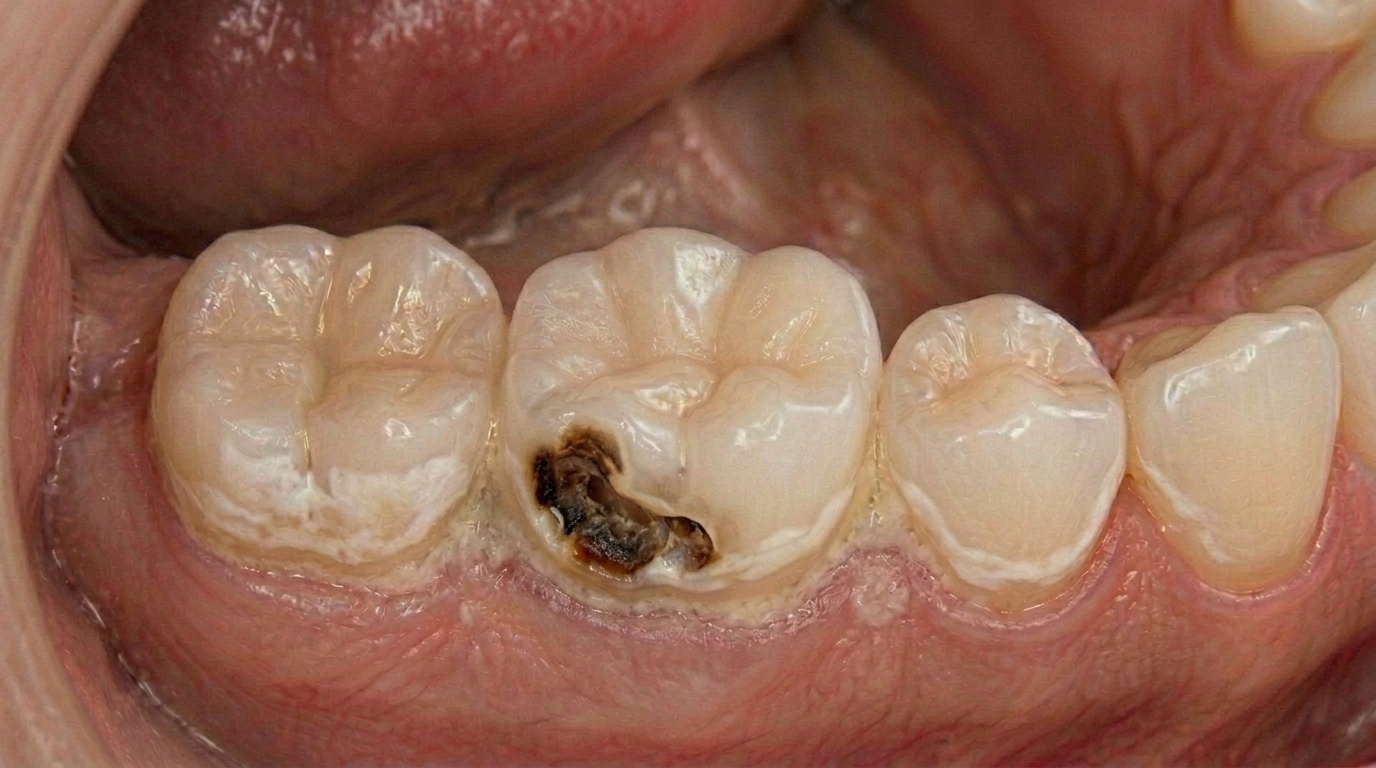
Stage 3: Dentine decay
Once decay passes through the enamel into the softer dentine underneath, it spreads more quickly and you start to notice sensitivity to sweet, cold, or hot foods. A larger filling or an onlay is usually needed. Cost: $250 to $600.
Stage 4: Pulpal involvement
If decay keeps going, it eventually reaches the pulp, which is the soft tissue containing the nerve and blood vessels. Pain tends to become more serious at this point, with a throbbing ache or sensitivity that lingers long after the trigger is gone. A filling is no longer enough. Root canal treatment followed by a crown is the way to save the tooth. Cost: $1,800 to $4,000.
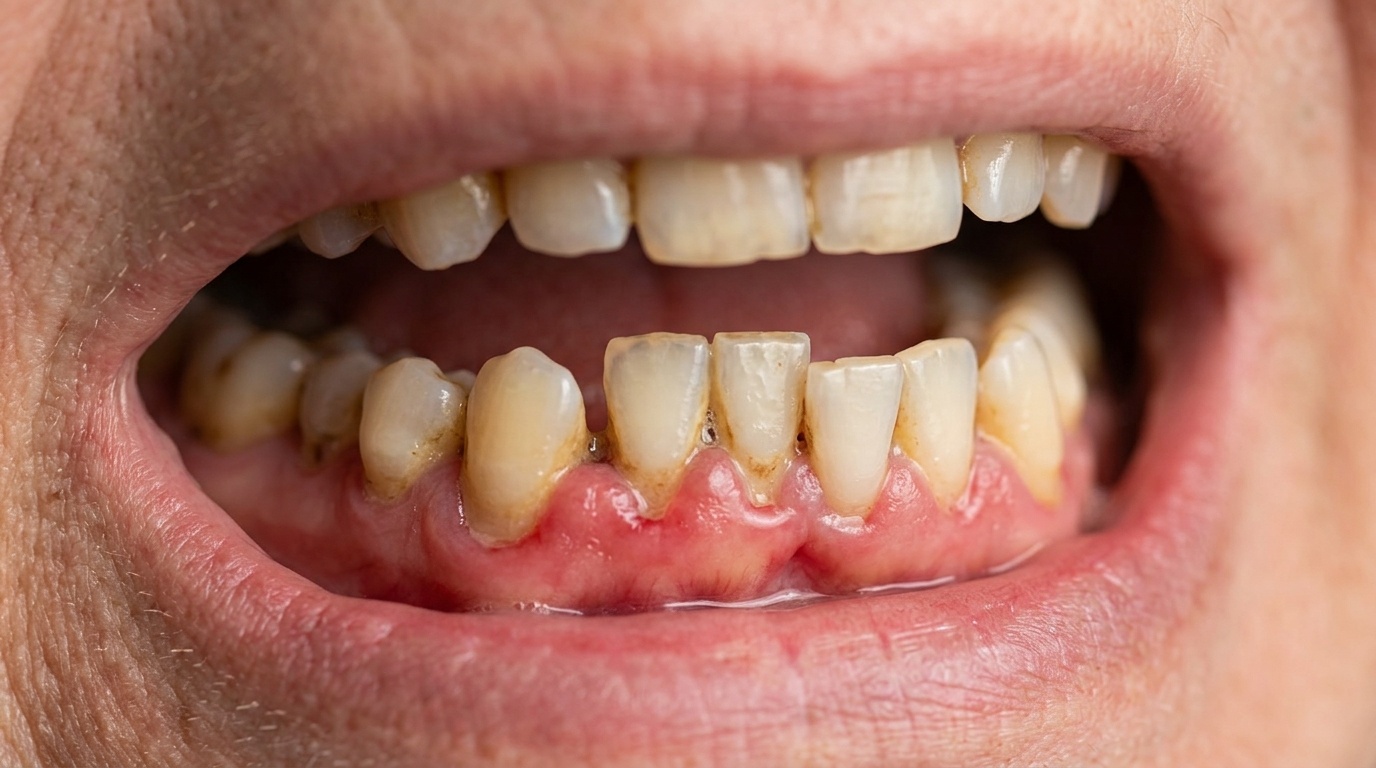
Stage 5: Abscess formation
When infection pushes out through the root into the surrounding bone, you have a dental abscess. Signs include facial swelling, a bad taste or pus, fever, or pain that radiates to your jaw, ear, or neck. This is a dental emergency and needs same-day care from an emergency dentist. At this late stage, an untreated cavity can progress into a cracked tooth or an extraction that might otherwise have been avoided. Cost: $2,000 to $4,500, depending on whether the tooth can be saved.
A note on dental sealants
For young patients who are particularly prone to cavities (especially on their back teeth), dental sealants can be applied as a protective coating over the chewing surfaces. They're quick, painless, and can significantly reduce the risk of new cavities forming in those areas.
How Much Does Tooth Decay Treatment Cost in Australia?
Cost is one of the main reasons people put off dental treatment, and it's a fair concern to raise. The ranges below are indicative Gold Coast general dentistry fees for 2026 and should not be read as a quote. Your final fee depends on the tooth, the extent of decay, and your health fund rebate.
Stage | Typical treatment | Approximate cost (AU) |
|---|---|---|
Early / white spot | Fluoride varnish + check-up | $80 to $140 |
Enamel cavity (small) | Composite filling | $180 to $320 |
Dentine cavity (larger) | Composite filling or onlay | $250 to $600 |
Pulpal decay (nerve) | Root canal + crown | $2,000 to $5,000 |
Late stage / abscess | Root canal + crown, or extraction | $400 (extraction) to $4,500 (RCT + crown) |
Most private health extras policies cover a portion of general dentistry, with the rebate varying by fund and by how much of your annual limit you've used. At ArtSmiles, we also offer payment plans and the Blessing Program, which can help some patients spread the cost of larger treatments. Eligibility and cover vary, so ask at your appointment or see our payment options page for current terms.
For most adults, Medicare does not cover general dental treatment. Limited exceptions exist, such as the Child Dental Benefits Schedule for eligible children and some public dental services for concession-card holders.
Frequently Asked Questions
How long does it take a cavity to form?
There's no fixed timeline. Early decay can develop in a few months if your diet is high in frequent sugar and your cleaning is patchy, but it often takes a year or two for a visible cavity to form in an adult tooth. Children's teeth, with thinner enamel, can move through the stages faster.
Does tooth decay always hurt?
No, and this is one of the reasons it gets missed. Early and even moderate decay is often completely painless. Pain usually starts only when decay reaches the dentine or nerve, and by that point the cavity is already well established.
Can rotting teeth still be saved?
Often, yes, as long as there's enough healthy tooth left to work with. Even teeth that look badly decayed can sometimes be saved with root canal treatment and a crown. The only way to know for sure is an examination and an X-ray.
Is silver diamine fluoride an option for me?
Sometimes. SDF works well for arresting some early cavities, particularly on baby teeth, on back teeth that are hard to reach, or for patients who struggle with dental work. It stains the treated area black, so it isn't chosen for visible front teeth. Your dentist will let you know whether it's a sensible fit.
Is a painful cavity a dental emergency?
A cavity causing significant pain, facial swelling, fever, or keeping you awake at night should be seen the same day. Less severe discomfort, such as sensitivity to cold or sweet foods, is still worth getting looked at promptly but is generally not an after-hours emergency.
Does Medicare cover tooth decay treatment?
For most adults, no. Limited exceptions exist for eligible children under the Child Dental Benefits Schedule and for concession-card holders through some public dental services. Most adults rely on private health extras cover or pay out of pocket.
Can children get fillings?
Yes, and sometimes it's the right call even for baby teeth. Baby teeth hold space for the adult teeth coming through, and an untreated cavity in a baby tooth can cause pain, infection, and problems for the adult tooth developing underneath.
Is tooth decay contagious?
The bacteria that cause decay can be passed between people, usually from a parent or carer to a young child through shared spoons, dummies, or kisses. Catching decay as an adult from another adult isn't really how it works, but the bacterial mix in a household does tend to be shared.
Take the First Step
If it's been a while since your last dental visit, or if you've noticed any sensitivity, dark spots, or rough edges on your teeth, don't wait. The sooner we take a look, the easier it is to treat.
At our Southport practice we take a gentle, no-judgement approach to dental care. Whatever state your teeth are in, we're here to help you get back on track. Book an appointment or call (07) 5588 3677.
Written by Dr. Cristian Dunker, BDSc, MBA, general dentist and principal at ArtSmiles Cosmetic and Implant Dentistry in Southport. AHPRA registration DEN0002260623.
This article was medically reviewed by Dr Cristian Dunker in April 2026. The information here is general in nature and should not replace a personalised consultation with a qualified dentist.