Most women know that menopause brings hot flushes, mood changes, and disrupted sleep. But very few realise that their mouth is one of the first places where hormonal changes show up. Bleeding gums, a persistent dry feeling, a strange burning sensation on your tongue, or teeth that suddenly feel more sensitive can all be connected to the hormonal shifts happening in your body.
If you have been noticing changes in your mouth and wondering what is going on, you are not alone. Research shows that the majority of women going through menopause experience at least one oral health change, yet most are never told to expect it. According to a 2025 integrative review published in the Journal of Midwifery & Women's Health, there is a significant gap in awareness among both women and healthcare providers about the connection between menopause and oral health.
This guide covers everything you need to know about how perimenopause, menopause, and postmenopause affect your teeth, gums, and overall oral health. We will walk through what happens at each stage, what the science says, and what you can do to protect your smile.
Table of Contents
How Hormones Affect Your Mouth
Your mouth is far more sensitive to hormonal changes than most people realise. Oestrogen, progesterone, and testosterone all play important roles in keeping your oral tissues healthy, from the gums and bones that support your teeth to the salivary glands that keep your mouth moist and protected.
A landmark study by Leimola-Virtanen et al. (2000) confirmed that oral mucosa contains oestrogen receptors. This means that when oestrogen levels decline during menopause, the tissues lining your mouth are directly affected. The gums become thinner, less resilient, and more prone to inflammation. Salivary glands produce less saliva. And the jawbone that holds your teeth in place can begin to lose density.
Emerging research published in Scientific Reports (Tramice et al., 2022) has also revealed that hormonal changes during menopause alter the composition of your oral microbiome. The balance of bacteria in your mouth shifts, which may increase your susceptibility to infections, gum disease, and cavities.
Perimenopause: The Early Warning Signs
Perimenopause typically begins in your early to mid 40s, though it can start earlier for some women. During this transitional phase, oestrogen and progesterone levels begin to fluctuate unpredictably. You might still have regular periods, but behind the scenes, your body is already changing.
Many women notice the first oral health changes during perimenopause without connecting them to their hormones. Common early signs include:
Gums that bleed more easily when brushing or flossing, even if your oral hygiene routine has not changed
Increased sensitivity to hot, cold, or sweet foods and drinks
A dry or sticky feeling in the mouth, especially at night or first thing in the morning
Subtle taste changes, where familiar foods may taste slightly metallic or different
More frequent mouth ulcers or tender spots on the gums
Increased teeth grinding or jaw clenching, often linked to disrupted sleep during this stage
If you are in your 40s and have noticed any of these changes, it is worth mentioning them at your next dental visit. Early awareness allows your dentist to adjust your preventive care and monitor for any progression.
Menopause and Your Oral Health: The Key Challenges
Once oestrogen levels drop significantly and periods stop (menopause is confirmed after 12 consecutive months without a period), the oral health effects tend to become more pronounced. A comprehensive 2024 review by Shrivastava identified several key oral manifestations that affect women during and after menopause.
Dry Mouth (Xerostomia)
Dry mouth is one of the most common oral complaints during menopause. Studies suggest that up to 50% of menopausal women experience dry mouth to some degree. Saliva is essential for neutralising acids, washing away food particles, and fighting bacteria. When production drops, your risk of cavities, gum disease, and oral infections increases significantly.
Dry mouth during menopause is caused by the decline in oestrogen, which affects salivary gland function. It can also be made worse by medications commonly prescribed during this life stage, including antidepressants, blood pressure medications, and antihistamines.
What you might notice: A sticky or dry feeling in the mouth, difficulty swallowing dry foods, cracked lips, bad breath, or a sore throat. Many women find that symptoms are worse at night.
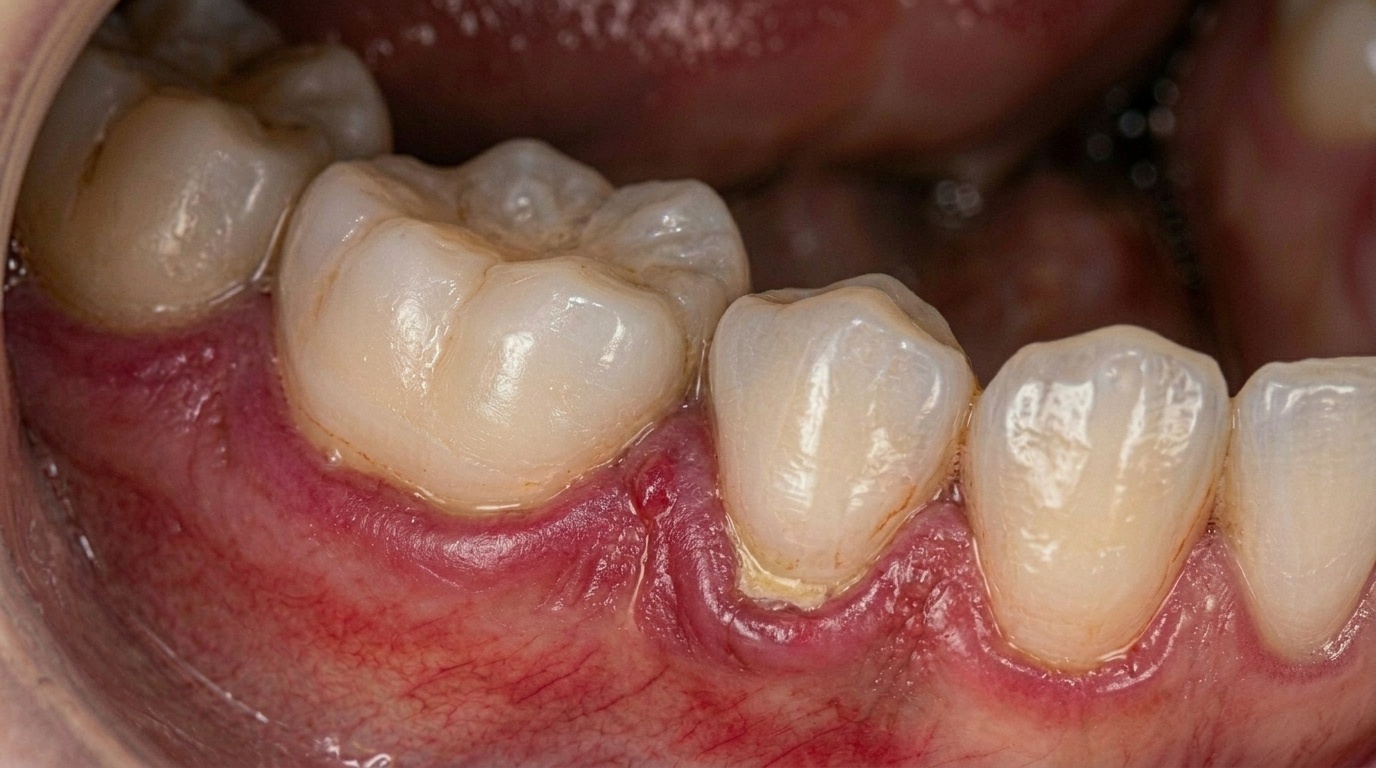
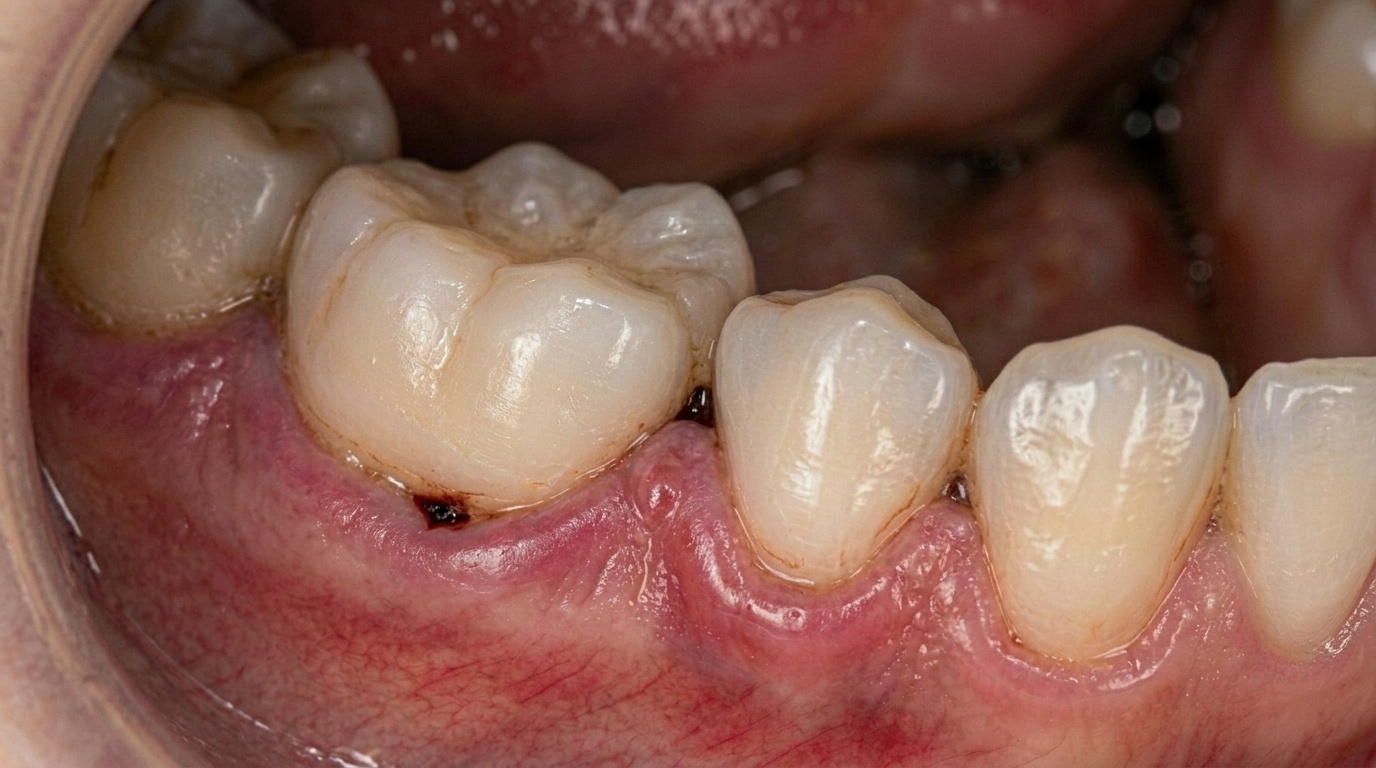
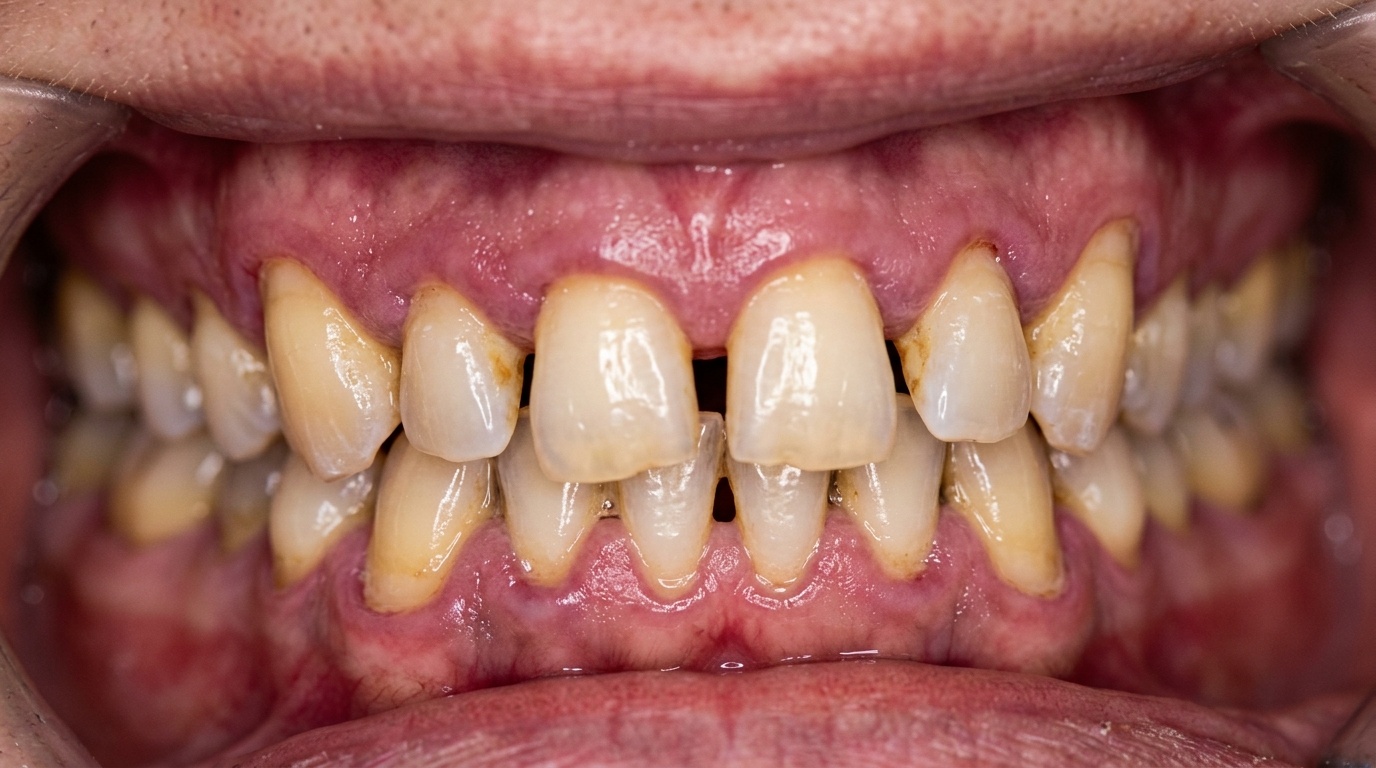
Gum Disease and Periodontitis
The relationship between menopause and gum disease is well established in the scientific literature. Declining oestrogen triggers an increase in inflammatory markers in the body, and the gums are particularly vulnerable.
According to Dutt et al. (2013), periodontal health is the most severely affected area, with up to 60% of menopausal women experiencing some degree of gum disease. The gums may appear red, swollen, or receded. You might notice that they bleed when you brush, or that your teeth seem slightly longer than before due to gum recession.
Research by Haas et al. (2009) found that postmenopausal women who were not using hormone replacement therapy had 2.1 times the risk of periodontitis compared to premenopausal women. This highlights how significant the hormonal factor really is.
Burning Mouth Syndrome
Burning mouth syndrome (BMS) is a condition that causes a persistent burning or tingling sensation in the mouth, most commonly on the tongue, palate, or lips. It is particularly prevalent during menopause, with studies reporting rates of 10% to 40% in menopausal women (Dahiya et al., 2013).
The exact mechanism is still being studied, but research by Ślebioda et al. (2014) suggests it involves changes to the small sensory nerve fibres in the mouth, triggered by declining oestrogen levels. Many women describe it as a scalded feeling, similar to burning your tongue on hot coffee, but without any visible cause.
If you are experiencing this, know that you are not imagining it. BMS is a recognised medical condition, and there are management strategies your dentist and doctor can recommend.
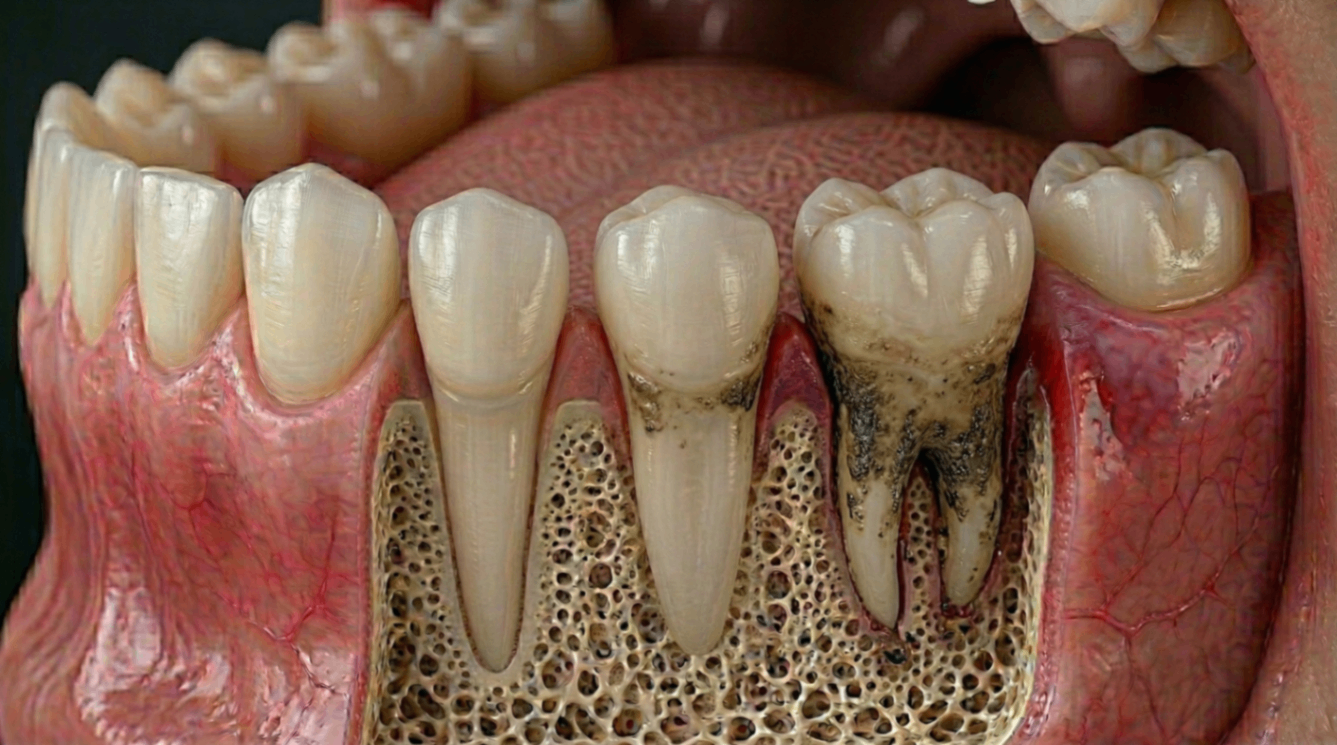
Bone Loss and Tooth Stability
Oestrogen plays a critical role in maintaining bone density throughout the body, including the jawbone. When oestrogen levels drop during menopause, bone resorption (the process of bone breaking down) can accelerate. For the jaw, this can mean less support for the teeth, increasing the risk of loosening or tooth loss over time.
A study by Munakata et al. (2011) found that menopause significantly affects both the quality and quantity of jawbone. Women who are also diagnosed with osteoporosis face a compounded risk. This is one reason why maintaining strong bone health through nutrition and exercise is especially important during this stage of life.
Some women also notice that their teeth seem to shift slightly or that their bite feels different. This is often related to changes in the supporting bone and gum tissue.
Reduced saliva flow and slower remineralisation through menopause can also leave enamel more vulnerable, making teeth more prone to chipping or fracture, particularly along the biting edges and around older fillings.
Taste Changes and Tooth Sensitivity
Many women report altered taste perception during menopause. Foods may taste more bitter, metallic, or simply "off." This condition, known as dysgeusia, is thought to be related to changes in the taste buds and the reduction in saliva that normally helps transport flavour molecules.
Tooth sensitivity also becomes more common as gums recede and expose more of the tooth root. The root surface does not have the same protective enamel layer as the crown, making it more reactive to temperature and certain foods.
TMJ Disorders and Teeth Grinding
This is one of the lesser known connections, but research suggests that postmenopausal women experience temporomandibular joint (TMJ) symptoms at a significantly higher rate. Jaw pain, clicking, difficulty opening the mouth fully, headaches, and teeth grinding (bruxism) can all become more frequent during menopause.
The relationship appears to involve both the direct effects of oestrogen loss on joint tissues and the indirect effects of increased stress, disrupted sleep, and changes in pain perception that accompany menopause. If you have been clenching your jaw or grinding your teeth at night, a custom protective splint from your dentist can help prevent damage to your teeth and relieve jaw tension.
Oral Infections: Thrush and Lichen Planus
The thinning and drying of oral tissues during menopause creates an environment where infections can take hold more easily. Two conditions that become more common during this time are oral thrush (candidiasis) and oral lichen planus.
According to Ciesielska et al. (2021), the incidence of oral lichen planus in perimenopausal women is approximately 10.9%, compared to just 0.5% to 2% in premenopausal women. Oral thrush, a fungal infection that causes white patches or redness in the mouth, is also more prevalent due to changes in saliva composition and reduced immune function in the oral cavity.
Both conditions are treatable, but they require proper diagnosis. If you notice unusual white patches, persistent redness, or sore areas in your mouth that do not heal within two weeks, see your dentist promptly.
Postmenopause: Long Term Oral Care
After menopause, oestrogen levels remain permanently low. The oral health challenges that began during perimenopause and menopause continue, and ongoing care becomes essential.
Dental Implant Considerations
Many women consider dental implants to replace missing teeth during or after menopause. The good news is that dental implants can be highly successful in postmenopausal women. However, bone quality and density need to be carefully evaluated, as these may be compromised.
Research by Munakata et al. (2011) emphasises the importance of thorough assessment, including 3D imaging, to evaluate jawbone health before implant placement. If bone density is a concern, procedures like bone grafting may be recommended to create a solid foundation for the implant.
Women taking bisphosphonate medications for osteoporosis should always inform their dentist, as these medications can affect healing after dental procedures.
Ongoing Monitoring
Postmenopausal women benefit from more frequent dental check ups, ideally every six months. Regular professional cleaning helps manage gum disease risk, while periodic X rays can monitor bone density around the teeth. Your dentist can also screen for oral conditions like lichen planus or thrush that may develop over time.
Nutrition for Oral Health During Menopause
What you eat plays a significant role in how well your mouth copes with hormonal changes. Here are the key nutrients to focus on:
Nutrient | Why It Matters | Good Sources |
|---|---|---|
Calcium (1,000 to 1,300mg daily) | Supports jawbone density and tooth structure | Dairy, sardines, almonds, leafy greens, fortified plant milks |
Vitamin D (600 to 800 IU daily) | Helps the body absorb calcium; supports immune function in the mouth | Sunlight, fatty fish, eggs, fortified foods |
Omega 3 fatty acids | Reduce inflammation, supporting gum health | Salmon, mackerel, walnuts, flaxseeds, chia seeds |
Vitamin C | Essential for collagen production and gum tissue repair | Citrus fruits, capsicum, strawberries, broccoli |
Water (at least 2 litres daily) | Combats dry mouth and supports saliva production | Plain water, herbal teas, water rich fruits |
Try to limit sugary and acidic foods, as dry mouth already reduces your mouth's natural ability to neutralise acids. Sugar free chewing gum can help stimulate saliva production between meals. This is not medical advice. Please consult your doctor for instructions how to manage menopause.
Treatment and Management
The good news is that most oral health changes associated with menopause are manageable with the right approach. Here is what you can do:
At Home
Use a soft bristled toothbrush and fluoride toothpaste to protect sensitive teeth and gums
Consider a toothpaste designed for dry mouth or sensitivity
Stay hydrated throughout the day, sipping water regularly
Use an alcohol free mouthwash to avoid further drying out the mouth
Chew sugar free gum containing xylitol to stimulate saliva production
If you grind your teeth at night, ask your dentist about a custom night guard
Professional Care
Schedule dental check ups every six months (or more frequently if recommended)
Ask about fluoride treatments or remineralising products to strengthen enamel
Discuss gum disease treatment options if you are noticing gum changes
Request a thorough screening for oral conditions like lichen planus or candidiasis
Talk to your dentist about how your current medications might be affecting your mouth
Hormone Replacement Therapy and Oral Health
There is growing evidence that hormone replacement therapy (HRT) can have a positive effect on oral health. A 2021 study by Wang et al. found that HRT significantly increased salivary oestradiol levels and reduced dry mouth symptoms. Research by Ageel et al. (2025) also showed that HRT was associated with a lower prevalence of periodontitis in postmenopausal women.
If you are considering HRT, it is worth discussing the potential oral health benefits with both your GP and your dentist. Every woman's situation is different, and the decision should be made as part of your overall health plan.
Some women on HRT notice changes in oral comfort during the first few months of treatment, including increased sensitivity, occasional mouth ulcers, or recurrent oral thrush. These tend to settle as the body adjusts. If symptoms persist or interfere with eating, mention them to your GP and dentist so dosage or topical care can be reviewed.
When to See Your Dentist
While many menopausal oral changes are gradual, some signs should prompt a visit sooner rather than later:
Persistent bleeding gums that do not improve with better brushing and flossing
A burning or tingling sensation in the mouth that lasts more than a few days
White patches, persistent redness, or sores that do not heal within two weeks
Loose teeth or a noticeable change in your bite
Severe dry mouth that affects your ability to eat, speak, or sleep comfortably
Jaw pain, clicking, or difficulty opening your mouth
Tell your dentist about your menopausal status and any medications you are taking. This information helps them tailor your care and catch potential issues early.
Frequently Asked Questions
Can menopause cause gum disease?
Yes. Declining oestrogen levels increase inflammation in the body and reduce the resilience of gum tissue. Research shows that up to 60% of menopausal women experience some degree of gum disease. Regular dental visits and good oral hygiene can help manage this risk.
Why is my mouth so dry during menopause?
Oestrogen plays a role in salivary gland function. As levels drop, saliva production can decrease. Certain medications commonly used during menopause (like antidepressants and blood pressure medications) can compound the problem. Staying hydrated and using saliva stimulating products can help.
Is burning mouth syndrome related to menopause?
Yes. Burning mouth syndrome is significantly more common in menopausal women, with studies reporting prevalence rates of 10% to 40%. It is thought to be related to changes in the small sensory nerve fibres in the mouth caused by oestrogen decline.
Can I get dental implants after menopause?
Absolutely. Dental implants can be very successful in postmenopausal women. Your dentist will evaluate your jawbone density and overall health to determine the best approach. If bone loss is a concern, bone grafting procedures may be recommended before implant placement.
Does HRT help with dental problems during menopause?
Research suggests that HRT can have oral health benefits, including reduced dry mouth and lower rates of periodontitis. However, HRT is a personal medical decision that should be discussed with your healthcare team based on your individual circumstances.
How often should I see the dentist during menopause?
Most dental professionals recommend check ups every six months during menopause. If you are experiencing active gum disease, dry mouth, or other oral health concerns, your dentist may suggest more frequent visits.
Your Smile Through Every Stage
Menopause is a natural transition, and understanding how it affects your oral health puts you in a much stronger position to take care of your smile. The changes are real and backed by science, but they are also manageable with the right support and preventive care.
At ArtSmiles, we understand the unique oral health needs of women going through perimenopause, menopause, and beyond. Our team takes the time to listen, assess your individual situation, and create a care plan that works for you. Whether you are concerned about gum health, considering dental implants, or simply want a thorough check up, we are here to help.
Book an appointment at our Southport clinic or call us on (07) 5588 3677 to start the conversation about your oral health.
Written by Dr. Cristian Dunker, BDSc, MBA. Medically reviewed by Dr. Cristian Dunker.