What Really Happens When a Cavity Is Left Untreated
Most cavities start so small that you would never know they were there. No pain. No visible hole. No change in how the tooth looks or feels. And because nothing hurts, it is easy to assume nothing needs to be done.
But tooth decay does not pause. It does not stay the same size. Once it starts, it follows a predictable path from the outer enamel through to the inner nerve, becoming more serious and more costly to treat at every stage.
This article explains exactly what happens inside a tooth as decay progresses, what treatment looks like at each point, and why a small filling today can prevent a much bigger problem tomorrow.
How Decay Begins: Demineralisation
Before a cavity even forms, the process starts with demineralisation. Bacteria in the mouth feed on sugars and starches from food and produce acid as a byproduct. This acid dissolves minerals from the enamel surface in a process that happens every time you eat or drink.
Saliva naturally helps to remineralise enamel between meals, but when acid exposure is frequent or prolonged, the balance tips in favour of mineral loss. Over time, the enamel weakens in localised spots.
At this stage, the damage may still be reversible. Fluoride application, improved oral hygiene, and dietary changes can help the enamel repair itself. No drilling is needed. No filling is required.
This is also the stage that is easiest to miss, which is why regular dental examinations are so valuable. A clinician can identify early demineralisation and intervene before it becomes a cavity.
Stage One: Enamel Cavity
Once mineral loss progresses beyond what the body can repair, a physical break in the enamel occurs. This is a cavity in its earliest form.
Enamel has no nerve supply, so there is no pain. The cavity may not even be visible to the naked eye. It is typically detected through dental X-rays or careful clinical examination.
A comprehensive review by Hummel et al. (2019) found that enamel cavities can take several years to reach the next layer of the tooth (PubMed). This is a significant window of opportunity for treatment with a small, conservative filling.
Treatment at this stage is straightforward. A small composite (tooth coloured) filling restores the tooth with minimal removal of natural structure. The appointment is typically quick and comfortable.
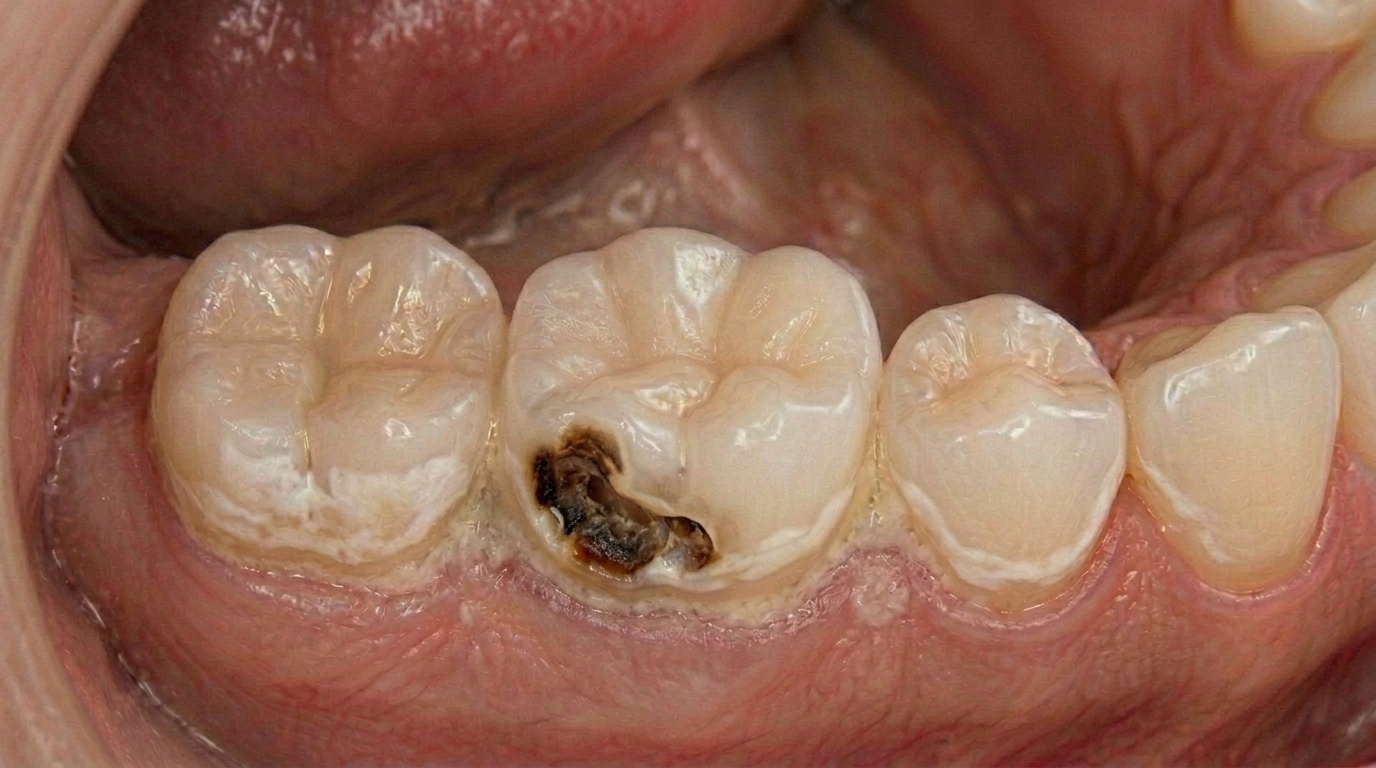
Stage Two: Dentine Involvement
Beneath the enamel lies dentine, a softer, porous layer that makes up the bulk of the tooth. Once decay breaks through the enamel and enters the dentine, the process accelerates significantly.
Dentine has a tubular structure that allows bacteria to spread more rapidly. The cavity grows in all directions, often becoming much larger beneath the surface than it appears on the outside.
Symptoms may begin to appear at this stage:
Sensitivity to sweet foods or drinks
Mild sensitivity to cold
A rough or catching sensation when running the tongue over the tooth
Visible discolouration or a small hole
A filling is still the primary treatment, but it will be larger than what would have been needed at the enamel stage. Depending on the extent of the decay, an onlay or partial crown may be recommended to provide additional structural support.
Research by Selwitz et al. (2007) in The Lancet confirmed that once enamel breakdown occurs, caries progression continues without clinical intervention (PubMed).
Stage Three: Pulp Involvement
The pulp is the living core of the tooth, containing nerves, blood vessels, and connective tissue. When decay reaches the pulp, the body mounts an inflammatory response called pulpitis.
Reversible pulpitis occurs when the inflammation is mild and the pulp can still recover if the source of irritation is removed. You might feel a brief, sharp sensitivity to cold that fades quickly.
Irreversible pulpitis occurs when the damage to the pulp is too extensive to heal. Pain becomes more intense, often throbbing, and may be triggered by heat or keep you awake at night. Abbott and Yu (2007) documented that once pulpitis becomes irreversible, conservative treatment is no longer effective (PubMed).
At this point, root canal treatment is needed to remove the infected pulp tissue, disinfect the canals, and seal the tooth. A crown is then placed to protect the remaining structure. Without treatment, the infection will spread beyond the tooth.
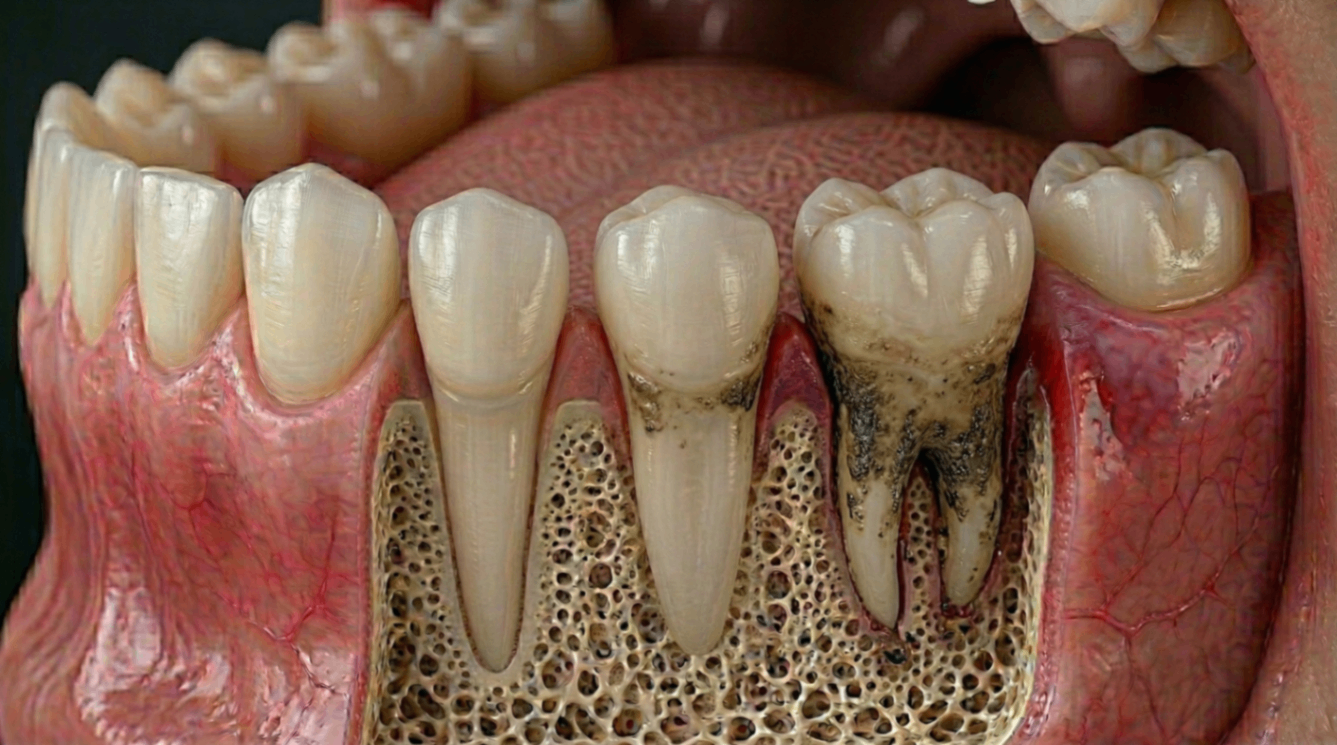
Stage Four: Abscess and Infection
When bacteria travel through the root canals and exit the tip of the root, they infect the surrounding bone and tissue. This creates a dental abscess.
An abscess can cause:
Severe, constant pain
Swelling in the face, cheek, or jaw
Fever and feeling unwell
A bad taste from draining pus
Difficulty opening the mouth or swallowing
A dental abscess is a clinical emergency. It requires immediate treatment, which may include antibiotics, drainage, and either root canal treatment or extraction. In rare cases, the infection can spread to other areas of the head and neck, requiring hospital admission.
This is the endpoint of a process that started with a tiny, painless spot on the enamel. At every stage along the way, simpler treatment was available.
Stage Five: Tooth Loss
When a tooth has been so severely damaged by decay that it cannot be restored, extraction is the only remaining option. The tooth is removed, and the resulting gap needs to be addressed to prevent the surrounding teeth from shifting.
Replacement options include dental implants, bridges, or removable dentures. Each involves additional appointments, additional cost, and a longer overall treatment journey.
A single tooth that could have been saved with a $200 to $400 filling may ultimately require a $4,000 to $6,000 implant. The clinical outcome is also different. No replacement is quite as good as keeping your natural tooth.
Why "It Doesn't Hurt" Is Not a Reliable Guide
Pain is a late indicator of dental decay. By the time a cavity hurts, the damage has usually reached the nerve. The first three stages of decay, when treatment is simplest and most effective, are typically pain free.
This is why waiting for pain before seeking treatment means missing the best opportunities for conservative care. Regular dental check ups are designed to catch problems at the earliest possible stage, before they become complex or costly.
What to Do if You Think You Have a Cavity
If you have noticed sensitivity, a rough spot, or discolouration on a tooth, or if it has simply been a while since your last dental visit, a check up is the best next step.
At ArtSmiles, we take a thorough approach to assessing your teeth, using clinical examination and digital imaging to identify decay at the earliest stage possible. If treatment is needed, we explain your options clearly and start with the most conservative approach.
A small problem today does not have to become a big one. Book an assessment to find out where things stand.
References
Hummel R, Akveld NAE, Bruers JJM, et al. Caries Progression Rates Revisited: A Systematic Review. J Dent Res. 2019;98(7):746-754. PubMed
Selwitz RH, Ismail AI, Pitts NB. Dental caries. Lancet. 2007;369(9555):51-59. PubMed
Abbott PV, Yu C. A clinical classification of the status of the pulp and the root canal system. Aust Dent J. 2007;52(1 Suppl):S17-S31. PubMed