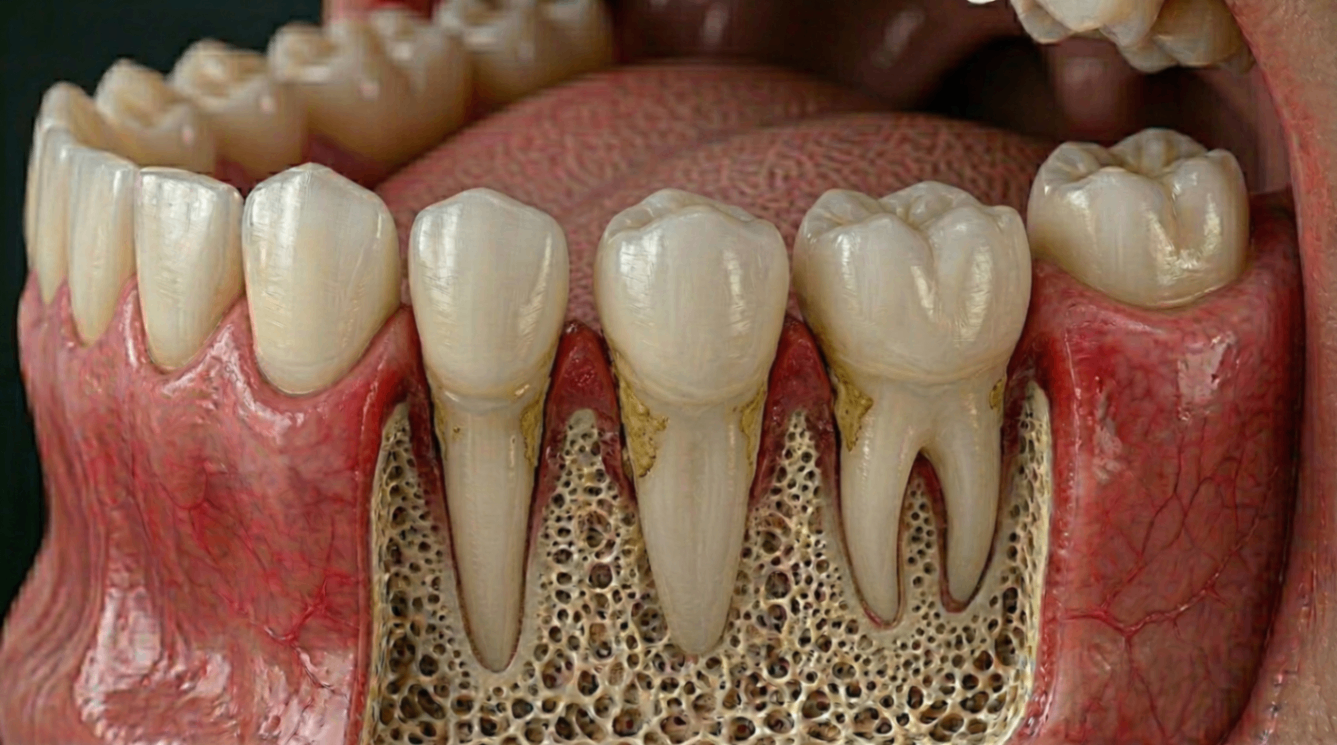
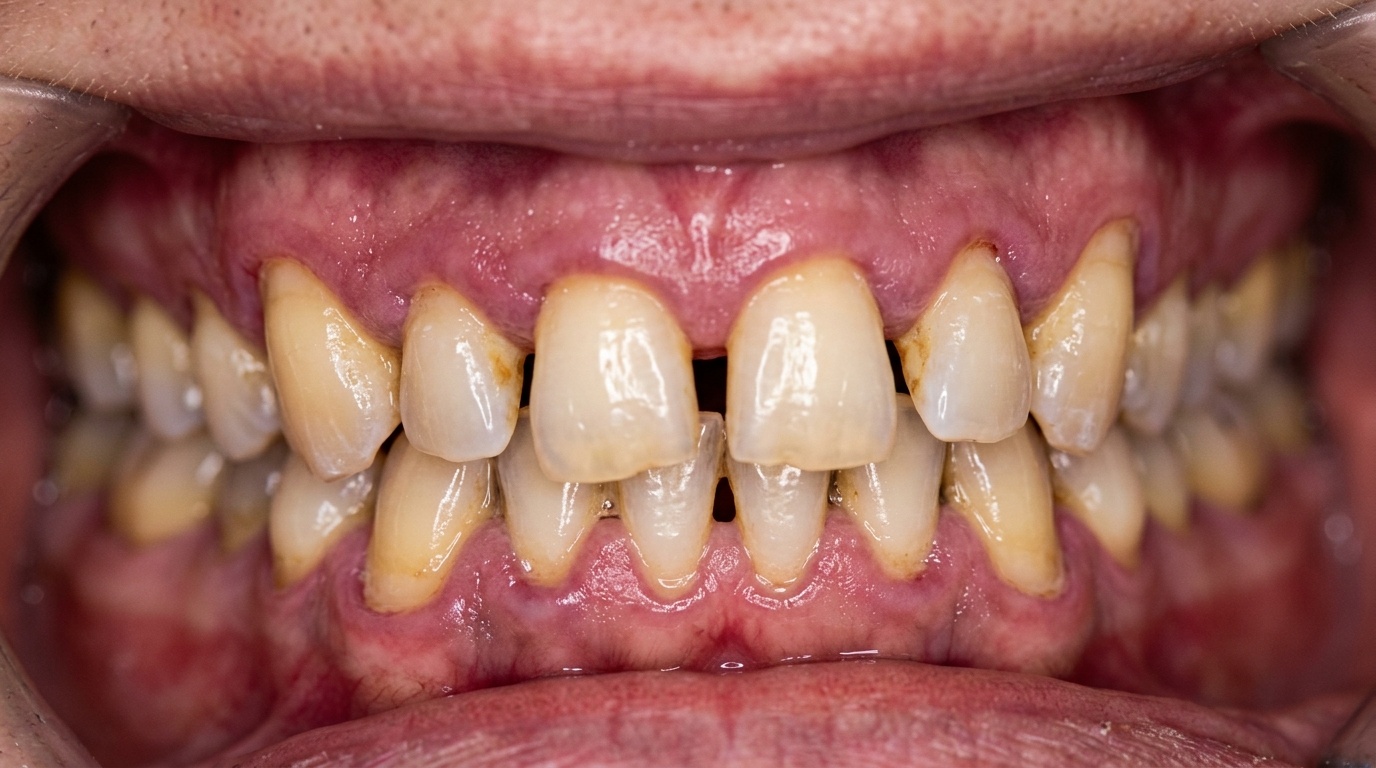
Ignoring gum disease means leaving bacterial inflammation of the gums untreated. It progresses silently from gingivitis (reversible) to periodontitis (permanent bone loss) over months to years, and raises the risk of tooth loss, heart disease, diabetes, and dementia.
Gum disease is one of the most common chronic conditions in the world, yet most people who have it don't know it. That's because the early stages rarely cause pain and the visible signs are easy to dismiss. A little blood when brushing. Slightly red gums. Nothing that feels urgent.
But gum disease does not stay mild. Without treatment, it moves through a series of predictable stages, each one harder to reverse. By the time symptoms become obvious, permanent damage has often already occurred.
This guide explains what happens at each stage of gum disease, what the clinical evidence tells us, and why early action consistently leads to better outcomes.
Key facts
Gum disease affects roughly half of adults over 30 (CDC and Australian population estimates).
Gingivitis is the only stage that fully reverses. Once it becomes periodontitis, bone loss is permanent.
Untreated gingivitis typically progresses to early periodontitis within 2 to 6 months.
Research links periodontitis to a 20% higher risk of cardiovascular disease, bidirectional risk with type 2 diabetes (approximately 25% each way), higher rates of preterm birth, and, in 2019 research, to brain inflammation seen in Alzheimer's.
An ArtSmiles periodontal assessment at Southport takes about 30 minutes and identifies which stage you are at.
If you ignore gum disease, it moves through four stages, from months to years. Stage one (gingivitis) reverses. Cross into periodontitis and the bone loss stays, permanently. Early treatment halts damage at any stage, but what's already gone is gone.
7 Signs of Gum Disease We See Patients Miss
Most of these get dismissed as normal. They aren't. If you notice two or more in the same month, book an assessment.
Bleeding when brushing or flossing
Puffy or bright red gums at the margin
Receding gum line (teeth look longer)
Persistent bad breath despite brushing
New spaces between teeth
Food packing more than usual
Tooth mobility or shifting
Stage One: Gingivitis (first weeks to first month untreated)
Gum disease begins with bacterial plaque building up along the gum line. When plaque is not removed thoroughly through brushing and flossing, the body responds with inflammation. This is gingivitis.
Progression speed varies with risk factors. Smoking, diabetes, and genetics accelerate the timeline.
At this stage, you might notice:
Gums that bleed when brushing or flossing
Slight redness or puffiness along the gum margin
Occasional tenderness
The critical point about gingivitis is that it is fully reversible. No permanent tissue destruction has occurred. A professional clean and consistent daily care can resolve it completely.
Unfortunately, many patients dismiss bleeding gums as normal. A study by Heitz-Mayfield (2005) found that patients often underestimate the significance of gingival bleeding, allowing the condition to progress unchecked (PubMed).
Stage Two: Early Periodontitis (2 to 6 months untreated)
When gingivitis is left untreated, the inflammation moves deeper. The gums begin to detach from the teeth, forming periodontal pockets where bacteria thrive. The bone that supports the teeth starts to resorb.
This stage is significant because bone loss is permanent. Unlike soft tissue, alveolar bone does not regenerate naturally once it is lost.
Clinical signs at this stage include:
Pockets measuring 4 to 5 millimetres
Minimal or no pain
Increased plaque and calculus below the gum line
Early gum recession in some areas
As of 2025, the staging system developed by Tonetti et al. (2018) remains the accepted framework. It classifies this as Stage I or II periodontitis, where treatment through non-surgical deep cleaning can still halt the disease effectively (PubMed).
Stage Three: Moderate Periodontitis (6 months to 2 years untreated)
As bone loss continues, the teeth begin to lose structural support. The damage is no longer limited to one or two areas. Multiple teeth may be affected.
Patients at this stage often notice:
Teeth that look longer due to receding gums
Spaces opening between teeth that were not there before
Food packing between teeth more frequently
Persistent bad breath despite good brushing
A slight change in how the bite feels
At this point, non-surgical deep cleaning remains a cornerstone of treatment, but more frequent maintenance visits become essential to prevent further progression. Some patients may need localised surgical treatment to access and clean deep pockets.
Stage Four: Advanced Periodontitis (2 years and beyond)
Advanced periodontitis involves significant bone loss, tooth mobility, and, in many cases, tooth loss. This is the stage where the consequences become most visible and most difficult to manage.
Symptoms include:
Noticeable tooth mobility or shifting
Teeth drifting apart
Pain when chewing
Recurring abscesses
Difficulty eating comfortably
Treatment at this stage may involve periodontal surgery, extraction of teeth that cannot be saved, and replacement with dental implants or bridges. Full mouth rehabilitation becomes necessary in severe cases.
Gum Disease and Your General Health
The consequences of untreated gum disease extend beyond the mouth. A growing body of research links periodontitis to several systemic conditions.
Cardiovascular disease
A 2021 meta-analysis by Larvin et al. found a 20% increased relative risk of cardiovascular disease in patients with periodontal disease (PubMed). Chronic oral inflammation is thought to contribute to atherosclerosis by seeding inflammatory markers into the bloodstream.
Type 2 diabetes
Research by Stöhr et al. (2021) demonstrated a bidirectional relationship between periodontitis and type 2 diabetes, with each condition increasing the risk of the other by approximately 25% (PubMed). Active gum disease worsens glycaemic control, which in turn accelerates periodontal breakdown.
Pregnancy complications
Corbella et al. (2012) found that periodontitis is associated with higher rates of preterm birth and low birth weight (PubMed). The mechanism is thought to involve inflammatory mediators crossing the placental barrier.
Alzheimer's disease and cognitive decline
A 2019 study led by Dominy et al. detected Porphyromonas gingivalis, a key gum disease bacterium, in post-mortem brain tissue of Alzheimer's patients at rates well above healthy controls (PubMed). The finding supports an inflammation-linked hypothesis that chronic oral infection may contribute to cognitive decline over time.
Why this matters
These findings reinforce why treating gum disease early matters for more than just your teeth.
Why Gum Disease Is Easy to Ignore
The main reason gum disease reaches advanced stages is that it does not follow the pattern most people expect. There is rarely a moment of sharp pain that forces action. The process is slow, painless, and cumulative.
Many patients are surprised to learn they have significant bone loss because they assumed their teeth were healthy. The absence of pain is not the same as the absence of disease.
When to Book an Assessment
Book now if you have tooth mobility, pain, recurring abscesses, or it's been three or more years since your last dentist visit.
Within the month: gums bleeding regularly, visible recession, or bad breath that won't shift despite good brushing.
Next check-up is fine if you have no symptoms and it's been 6 to 12 months since your last clean.
What to Do if You Think You Might Have Gum Disease
If you have noticed bleeding when brushing, gum recession, or if it has been a while since your last dental visit, a thorough periodontal assessment is the most useful first step.
At ArtSmiles, we evaluate your gum health with detailed measurements, assess bone levels, and provide clear explanations of what is happening. From there, we create a treatment plan tailored to your situation, starting with the areas that need the most attention.
It is never too late to start managing gum disease. Even in advanced cases, treatment can stabilise the condition, protect remaining teeth, and restore comfort. Book an assessment to find out where you stand and what your options are.
Frequently Asked Questions
Can gum disease be reversed?
Gingivitis is fully reversible with professional cleaning and good home care. Once the disease reaches periodontitis, the damage to bone and attachment is permanent, but progression can be halted with treatment at any stage.
How long does gum disease take to progress from gingivitis to tooth loss?
It varies. Without treatment, most patients progress from gingivitis to early periodontitis within 2 to 6 months. Advanced periodontitis leading to tooth loss typically takes several years. Smokers and people with diabetes can progress faster.
Is gum disease contagious?
Gum disease itself is not contagious, but the bacteria that cause it can be transmitted through saliva, including sharing utensils or kissing. Having shared bacteria does not guarantee disease. It develops only when other risk factors are present.
What does early gum disease look like?
Gingivitis shows as gums that are slightly red, puffy, and bleed easily when brushing or flossing. You may notice a small pink tint on your toothbrush. There is typically no pain.
How much does gum disease treatment cost in Australia?
Costs vary by severity. Non-surgical deep cleaning is usually several hundred dollars per quadrant. Advanced treatment involving surgery or implants is substantially more. Your dentist should provide an itemised treatment plan and a quote in writing before proceeding.
Can you have gum disease without bleeding gums?
Yes. Smokers often have reduced gum bleeding because nicotine constricts blood vessels, masking inflammation. Smokers can progress to advanced stages without noticing classic warning signs.
Is gum disease the same as gingivitis?
No. Gingivitis is the earliest, reversible stage of gum disease. Periodontitis is the later stage where bone loss has begun. All gingivitis is gum disease, but not all gum disease is gingivitis.
What is the outcome of gum disease treatment?
Gingivitis resolves in most cases with professional cleaning. Non-surgical deep cleaning effectively halts progression for early-stage periodontitis when followed by consistent maintenance. Advanced cases are more complex and may require surgical treatment, with outcomes varying by case.
What to remember
Gum disease is painless until advanced. Absence of pain is not absence of disease.
Gingivitis reverses. Periodontitis does not.
Smokers and people with diabetes progress faster and often without bleeding as a warning sign.
Early assessment is the single highest-leverage action, at every stage.
References
Heitz-Mayfield LJA. Disease progression: identification of high-risk groups and individuals for periodontitis. J Clin Periodontol. 2005;32(Suppl 6):196-209. PubMed
Tonetti MS, Greenwell H, Kornman KS. Staging and grading of periodontitis. J Periodontol. 2018;89(Suppl 1):S159-S172. PubMed
Larvin H, Kang J, Aggarwal VR, et al. Risk of incident cardiovascular disease in people with periodontal disease. Clin Exp Dent Res. 2021;7(1):109-122. PubMed
Stohr J, Barbaresko J, Neuenschwander M, Schlesinger S. Bidirectional association between periodontal disease and diabetes mellitus. Sci Rep. 2021;11(1):13686. PubMed
Corbella S, Taschieri S, Francetti L, et al. Periodontal disease as a risk factor for adverse pregnancy outcomes. Odontology. 2012;100(2):232-240. PubMed
Dominy SS, Lynch C, Ermini F, et al. Porphyromonas gingivalis in Alzheimer's disease brains: Evidence for disease causation and treatment with small-molecule inhibitors. Sci Adv. 2019;5(1):eaau3333. PubMed
Written by Dr. Cristian Dunker, BDSc, MBA. AHPRA registration: DEN0002257085. Dr. Dunker practises general and restorative dentistry at ArtSmiles in Southport, Gold Coast.
Medically reviewed 23 April 2026. ArtSmiles reviews this article annually to ensure information reflects current clinical guidelines from the Australian Dental Association and the American Academy of Periodontology.