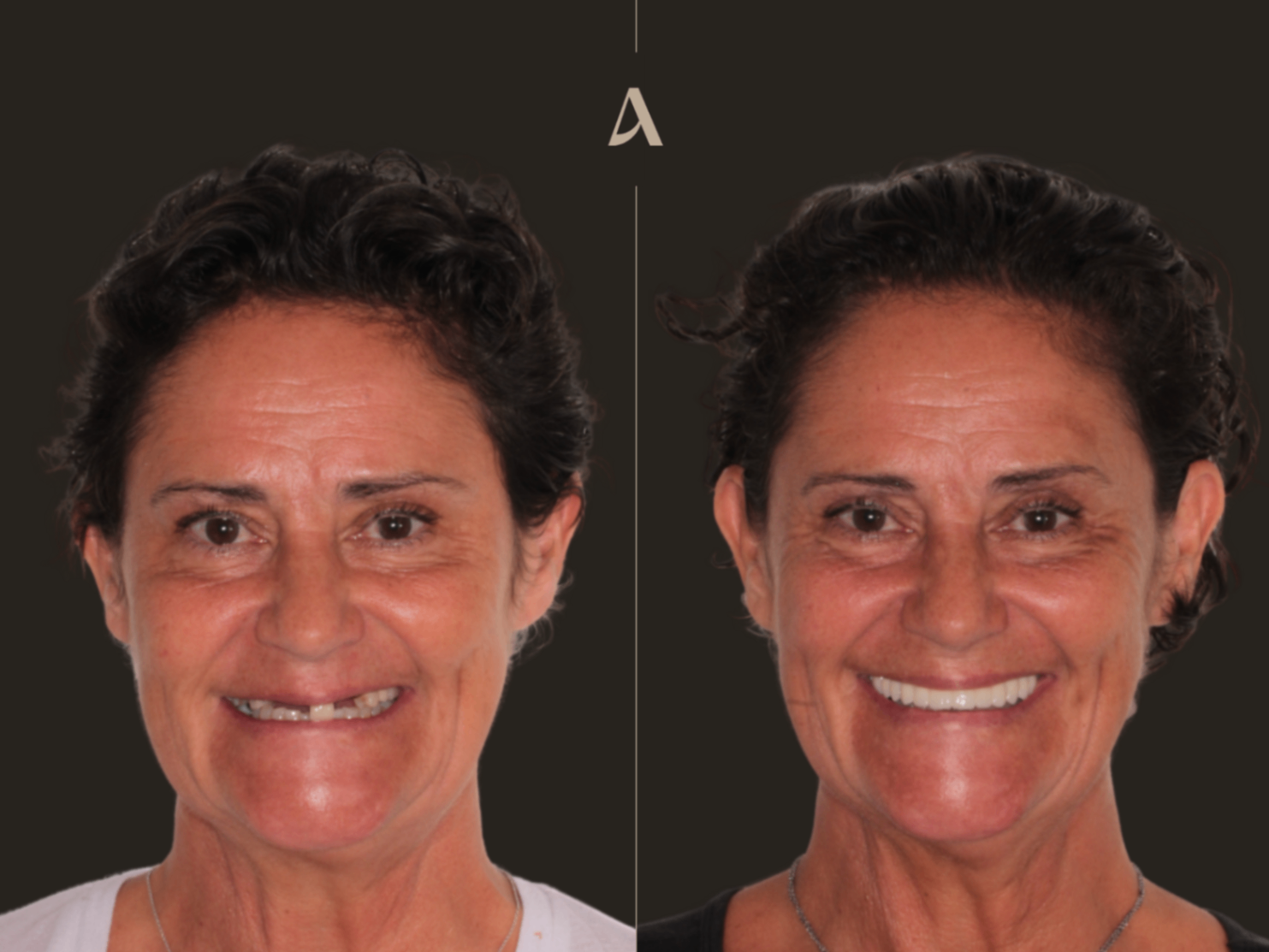
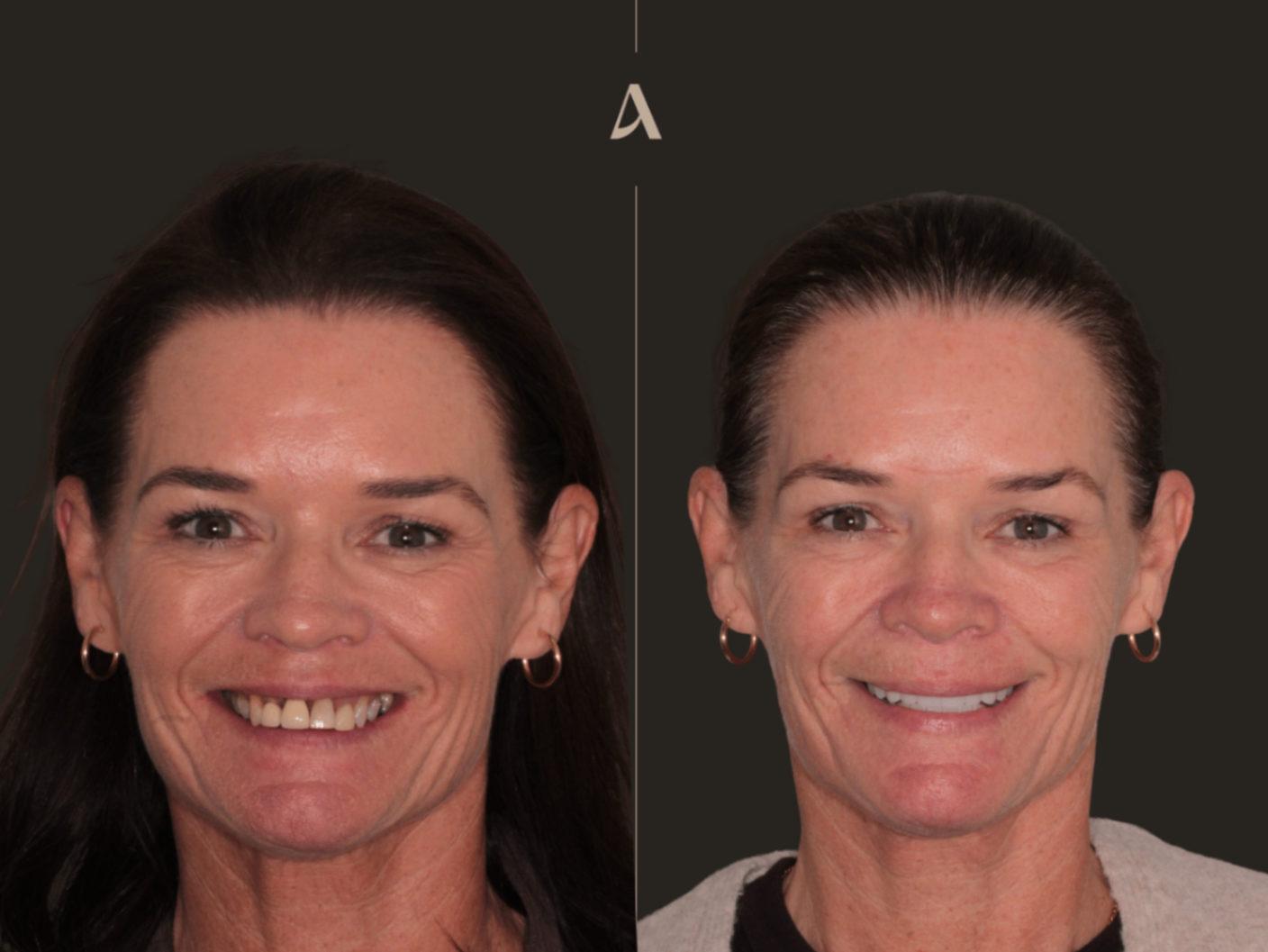
Some cases stay with you. This is one of those cases. When this patient first walked into our clinic, she was in constant pain, dealing with swelling, and avoiding social situations because of her missing front teeth. She told me she had stopped smiling in photos and felt embarrassed in conversations. That is the kind of thing that goes far beyond dentistry. It affects every part of someone's life.
Research confirms just how deeply anterior tooth loss impacts a person. A systematic review by Gerritsen et al. (2010) found that tooth loss is consistently associated with poor oral health related quality of life, with anterior tooth loss having a significantly greater psychological and social impact than posterior tooth loss. A qualitative study by Johannsen et al. (2012) described how patients facing the loss of their front teeth often experience periods of fear, shame, and social withdrawal.
I knew from the first consultation that we could change this patient's life. But it would take careful planning, patience, and a staged approach to get there safely.
In this article
What I Found During the Examination
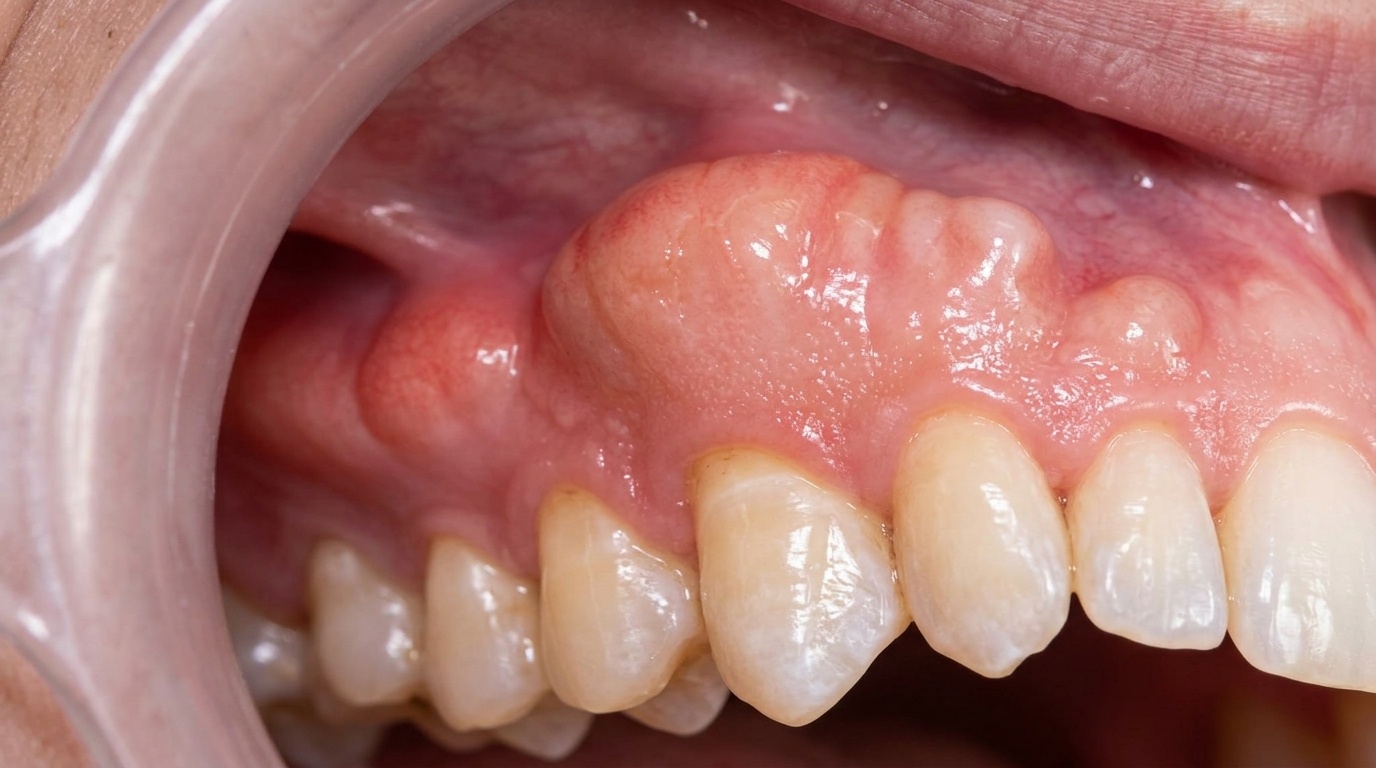
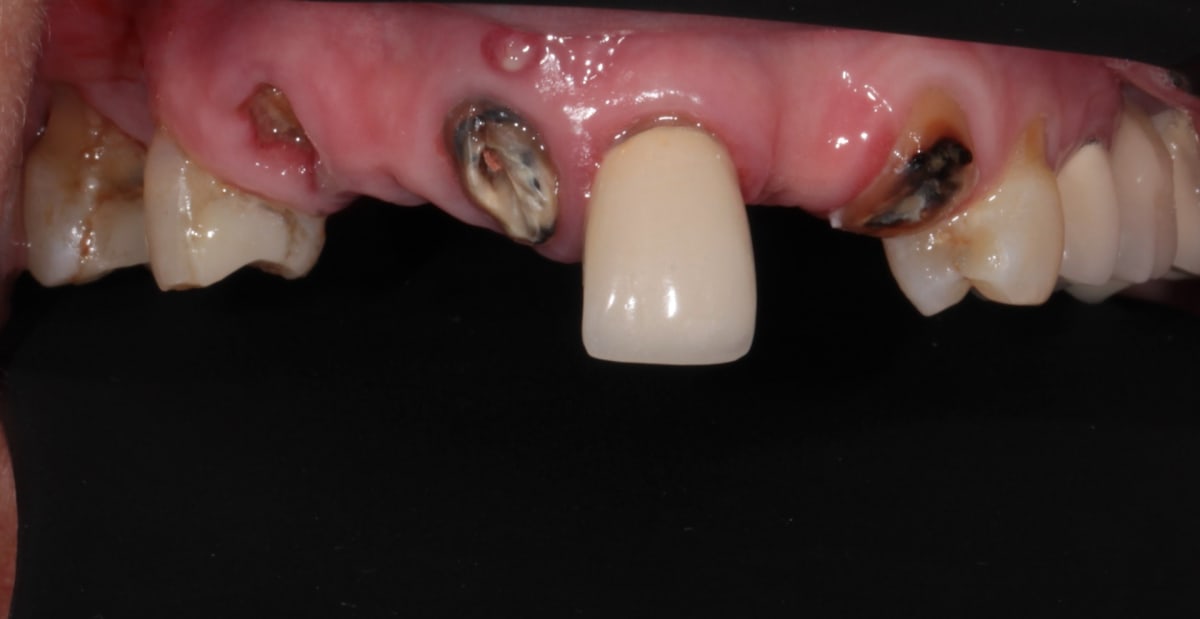
The oral examination revealed a complex situation in the upper arch. There was active gum disease (periodontitis) that needed to be addressed before anything else. Several anterior teeth were unrestorable due to infection and significant bone loss. However, the posterior teeth in the upper arch still had a good prognosis and could be saved with crowns and bridges.
The lower arch was in reasonable condition and did not require treatment at this stage. My focus was entirely on rehabilitating the upper arch.
The Treatment Plan
I designed a staged treatment plan that would address each issue in the right order:
Deep cleaning to bring the gum disease under control
Extraction of the infected anterior teeth that could not be saved
Bone grafting in the extraction sites to rebuild the foundation for future implants
A temporary denture so the patient would have teeth while healing
Crowns and bridges on the restorable posterior teeth to complete the back of the upper arch
Placement of three implants in the anterior region once the bone graft had matured
A fixed implant supported bridge to replace the temporary denture with a permanent solution
Treating the gum disease first was non negotiable. As Sousa et al. (2016) demonstrated in their systematic review, patients with a history of periodontitis face higher rates of biological complications around implants. Stabilising the periodontal condition before placing implants is one of the most important steps in ensuring long term success.
Stage 1: Treating the Gum Disease and Restoring the Posterior Teeth
We started with a thorough deep clean to manage the active periodontal infection. Once the gums had responded well to treatment and the inflammation was under control, I extracted the infected anterior teeth and placed bone graft material in the extraction sites.
At the same time, I fitted the patient with a temporary denture. While a removable denture is never ideal, it gave her teeth immediately so she could eat and speak while we waited for the bone to heal. It also gave her something she hadn't had in a long time: the confidence to smile.
While the bone graft was maturing, I restored the posterior upper teeth with crowns and bridges. This meant that by the time we placed the implants, the back of the arch was already solid and functional.
Stage 2: Implant Placement
After six months of healing, the bone graft had integrated well and there was sufficient bone volume to support implants. I placed three implants in the anterior upper arch in the positions that would give the best structural and aesthetic result.
A systematic review by Aghaloo et al. (2016) confirmed that bone augmentation techniques in the edentulous maxilla, including guided bone regeneration, can successfully restore ridge dimensions for implant placement with high survival rates. Research by Hof et al. (2015) comparing different timing protocols for implant placement in the anterior maxilla found that delayed placement after grafting achieves comparable long term results, with mean peri-implant bone loss of just 1.6 mm across all protocols evaluated.
After placing the implants, we waited another three months for osseointegration, the process where the implants fuse with the bone and become a permanent part of the jaw.
Stage 3: The Final Bridge
Once the implants were fully integrated, I designed and fabricated the final implant supported bridge for the anterior region. This fixed bridge replaced the temporary denture permanently, giving the patient teeth that look, feel, and function like natural ones.
A 2020 systematic review by Ramani et al. (2020) found that implant supported fixed restorations in the aesthetic zone have an overall positive impact on oral health related quality of life, with patients reporting high satisfaction with aesthetics, phonetics, and function.
The Moment That Made It All Worth It
When I handed the patient the mirror after installing the final bridge, she cried. Not from pain or discomfort, but from happiness. She told me it had transformed her life. After months of treatment, patience, and trust in the process, she finally had the smile she deserved.
That reaction is why I do what I do. Research by Chen et al. (2012) showed that implant restoration of missing anterior teeth significantly improves dental self confidence and reduces the negative psychosocial impact of poor dental aesthetics. But no study can capture the feeling of watching someone see their new smile for the first time.

Key Takeaways from This Case
Gum disease must be treated first. Placing implants in an unhealthy mouth puts the entire treatment at risk
Bone grafting creates the foundation. When teeth are lost to infection, the bone often needs to be rebuilt before implants can be placed
A staged approach is worth the wait. Taking the time to heal properly at each stage leads to better, longer lasting results
Temporary teeth matter. A provisional denture gives the patient function and dignity during the healing process
Restoring the whole arch matters. By combining implants anteriorly with crowns and bridges posteriorly, we achieved a complete, functional upper arch
The emotional impact is real. For patients who have lived with pain and embarrassment, a new smile can genuinely change their life
If you are living with missing front teeth, gum disease, or a denture that no longer works for you, I would love to help. Book a consultation at ArtSmiles and let's talk about what is possible for your smile.
Disclaimer
This article documents one patient's treatment at ArtSmiles. It is shared for educational purposes with the patient's written consent. Individual results vary and depend on factors including oral health, bone and gum condition, general medical history, and how well the restoration is maintained after treatment. Nothing in this article is a guarantee of outcome, a substitute for a clinical examination, or advice specific to your case. Any treatment carries risks and potential complications, which will be explained to you at consultation.
Case executed by Dr Cristian Dunker
General Dentist
AHPRA DEN0002257085
ArtSmiles, Southport, Gold Coast
Frequently Asked Questions
Can you get dental implants if you have gum disease?
Not immediately. Active gum disease has to be brought under control before any implant surgery. In this case we treated the periodontitis with a deep clean first, waited for the gums to respond, then planned the implants. Research by Sousa et al. (2016) confirms that implants placed in patients with a history of periodontitis are at higher risk of biological complications, which is why stabilising the gums first is non-negotiable.
How long does this kind of smile restoration take?
Around 9 to 12 months for a staged case like this one. The bone graft needs 3 to 6 months to mature before implants are placed. The implants then need roughly 3 more months to fuse with the bone (osseointegration) before the final bridge goes on. The timeline is driven by biology, not by the clinic.
Do you have to lose all your upper teeth for this kind of treatment?
No. This patient only lost the front teeth that were unrestorable. The back teeth still had enough bone and structure to be saved with crowns and bridges, so we rebuilt the arch in two halves: implants at the front and crowns and bridges at the back. Saving teeth is always the first choice when the long-term prognosis is good.
Is a temporary denture needed while the implants heal?
Almost always, for an anterior case. A temporary denture gives the patient teeth during the 6 to 9 month healing window so they can eat, speak, and smile. It's not the final result, it's a bridge to the final bridge.
What is the alternative to an implant bridge for missing front teeth?
A conventional bridge supported by the neighbouring natural teeth, or a removable partial denture. Both are viable for some patients. Implants are usually preferred when we want to avoid grinding down healthy adjacent teeth and when long-term bone preservation matters. A consultation and 3D scan will show which option suits your mouth.
Written by Dr Cristian Dunker, BDSc, MBA.
Medically reviewed on 23 April 2026 by Dr Cristian Dunker.
References
Gerritsen et al. (2010). Tooth loss and oral health-related quality of life: a systematic review and meta-analysis. Health Qual Life Outcomes. PubMed
Johannsen et al. (2012). Dental implants from the patients' perspective: transition from tooth loss, through amputation to implants. J Clin Periodontol. PubMed
Sousa et al. (2016). A systematic review of implant outcomes in treated periodontitis patients. Clin Oral Implants Res. PubMed
Aghaloo et al. (2016). Bone augmentation of the edentulous maxilla for implant placement: a systematic review. Int J Oral Maxillofac Implants. PubMed
Hof et al. (2015). Does timing of implant placement affect implant therapy outcome in the aesthetic zone? Clin Implant Dent Relat Res. PubMed
Ramani et al. (2020). Patient satisfaction with esthetics, phonetics, and function following implant-supported fixed restorative treatment in the esthetic zone. J Esthet Restor Dent. PubMed
Chen et al. (2012). The psychosocial impacts of implantation on the dental aesthetics of missing anterior teeth patients. Br Dent J. PubMed