You want whiter teeth, and you'd rather sort it at home if you can. Fair enough. The question is: what actually works, and what's marketing?
This guide answers that honestly. Every claim here is sourced to peer-reviewed research, the Australian Dental Association, the Cochrane Library, or the Therapeutic Goods Administration. We'll cover strips, kits, custom trays, the "natural" methods trending on TikTok, and when in-chair whitening is actually the better call.
We are not going to tell you that everything works. Some popular methods do nothing. One or two cause permanent damage. And one very common kit feature, the LED light, has been studied repeatedly and found to add no whitening benefit at all.
At ArtSmiles, we'd rather you spend your money on something evidence-backed than on a gadget that doesn't do what the box promises. No upselling, no scare tactics. Just what the research says about how to whiten teeth at home safely.
In this article
First, Why Are Your Teeth Yellow in the First Place?
Not all stains are the same, and that matters because it changes which method will work for you.
Extrinsic stains are the surface ones. Coffee, tea, red wine, curry, smoking, and vaping all deposit chromogens (coloured molecules) onto the outside of the enamel. These respond well to mechanical stain removal, whitening toothpastes, and surface-level peroxide bleaching.
Intrinsic stains sit inside the tooth. They come from age-related dentine yellowing, tetracycline antibiotic exposure in childhood, fluorosis (from too much fluoride during tooth development), or old trauma that darkened a tooth. These only respond to peroxide that diffuses through the enamel into the dentine underneath, and some types, like severe tetracycline staining, respond poorly even then (Watts & Addy, 2001).
If your yellowing is intrinsic and severe, home methods will underperform. The causes of tooth discolouration page walks through the treatment options for stained teeth in more detail.
Things Peroxide Will NOT Whiten
Crowns, porcelain veneers, and composite (tooth-coloured) fillings keep their original shade forever. Peroxide does nothing to them. If you have any of these on your visible front teeth and you whiten the natural teeth around them, you'll end up with a colour mismatch. Plan the order of treatment with your dentist.
The Only Active Ingredient That Whitens Teeth
There is one. It's hydrogen peroxide (H₂O₂). Everything else in a whitening product is either a delivery system, a surface stain-remover, or marketing.
You'll also see carbamide peroxide on labels. That's the same active in a slow-release form. Carbamide peroxide breaks down on contact with saliva into hydrogen peroxide plus urea, at roughly a 1:3 ratio. So a 10% carbamide peroxide gel delivers about 3.5% hydrogen peroxide (Carey, 2014).
Everything else you see advertised, enzymes, activated charcoal, coconut oil, baking soda, blue LED light, is not the bleaching agent. If peroxide isn't in the product, it isn't a whitener in the bleaching sense. It might remove surface stains. It will not lighten the colour of your teeth.
The Australian Legal Ceiling You Need to Know About
The TGA Poisons Standard caps over-the-counter whitening products at 6% hydrogen peroxide or 18% carbamide peroxide (TGA Poisons Standard). Anything stronger can only be supplied to you by a registered dental practitioner, and that supply has to follow the Australian Dental Association's guidance (ADA Australia Policy 2.2.8).
The ACCC has taken enforcement action against importers selling kits above the legal limit (ACCC media release). Practical takeaway: if a kit on Amazon, eBay, or a salon shelf is shouting "35% peroxide!" or "44% peroxide!", it's either illegal to sell to you in Australia, mislabelled, or both. Don't use it.
Whitening Strips, the Most-Studied At-Home Option
Whitening strips have more published clinical data behind them than any other at-home option.
The 2018 Cochrane systematic review pooled 71 randomised trials and 3,780 adults, and found that hydrogen peroxide strips do produce a measurable shade change compared to placebo (Eachempati et al., 2018). The Cochrane team rated the certainty of evidence as low to very low, which means the effect is real, but the size varies from person to person.
In the published trials, most participants saw around 2 to 4 shade groups of lightening over 2 to 4 weeks of daily use, with some change typically visible from about week one. Individual results vary. Crest-style strips with 6 to 14% hydrogen peroxide have the most RCT data behind them (Gerlach, 2004).
Common side effects are mild and temporary: some gum irritation where the strip touches the gumline, and some tooth sensitivity during and just after treatment. Both settle when you finish the course.
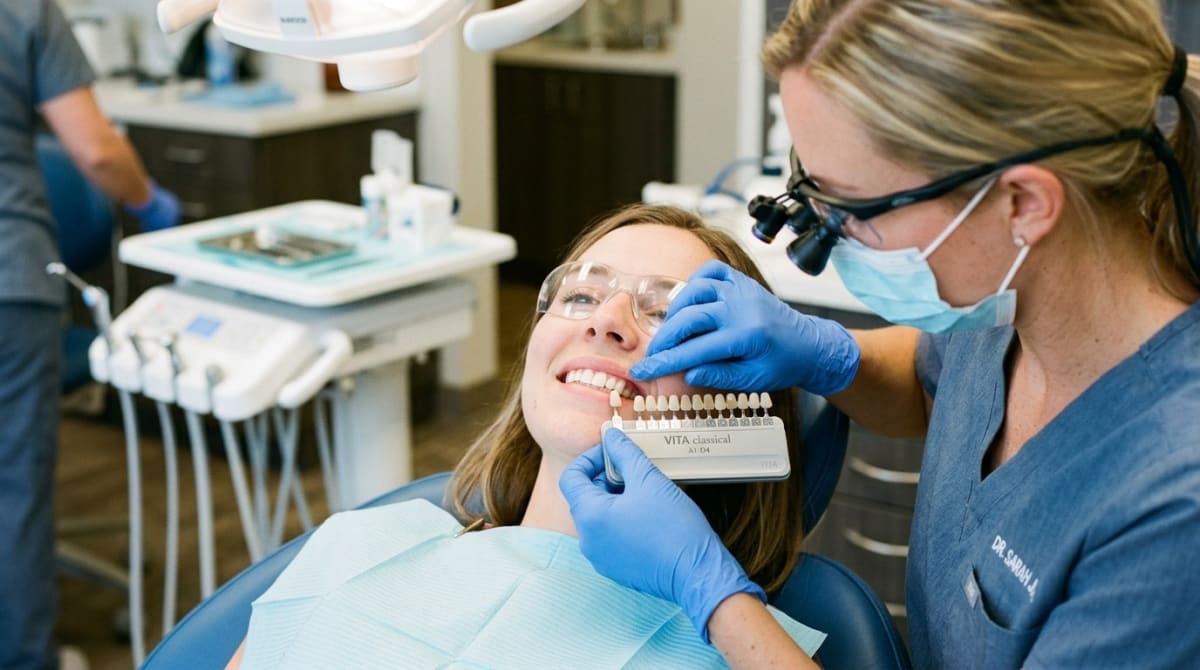
This is the shade guide dentists use to measure how white are your teeth.
What to Look For When Buying Strips in Australia
Hydrogen peroxide as the active ingredient (carbamide peroxide is also fine, but less common in strip form)
Concentration listed on the label. Anything claimed above 6% H₂O₂ should make you pause. Check the Australian legal ceiling section above.
A real ingredient list and an Australian importer or contact. If the pack has none of that, don't put it in your mouth.
At-Home Whitening Kits, What's in the Box and What Earns the Evidence
"Whitening kit" covers a wide range. Some are genuinely evidence-based. Some are a gel plus a theatre prop.
Custom-Fit Tray Kits (the Dentist-Prescribed Kind)
This is the most-evidenced take-home approach in the Cochrane review. Your dentist takes an impression of your teeth, makes a tray that fits precisely over them, and prescribes a carbamide peroxide gel (typically 10 to 16%). You wear it nightly, or for a set contact time, over 2 to 4 weeks.
Why the custom tray matters: the gel sits evenly across every tooth surface, there's less overflow onto the gums, and your dentist can adjust the concentration if you're getting sensitivity. It's the most-studied at-home method in the published literature, and it's what the long-term studies are actually measuring when they report two-year colour stability.
Boil-and-Bite and Prefabricated Tray Kits
The published evidence shows prefabricated and boil-and-bite trays underperform custom trays at the same peroxide concentration. The gel pools unevenly. Some teeth get too much contact, some too little, and the gum often gets more than it should.
They're cheaper, and you can start them immediately. Reasonable for mild surface staining if that's all you want. Not ideal if you're chasing an even, front-tooth result.
LED Whitening Kits, a Hard Truth
The light in a blue-LED whitening kit is, by the published evidence, doing nothing to whiten your teeth.
Two major meta-analyses have looked at this. He et al. (2012) pooled the clinical evidence and found LED or light activation does not improve shade outcomes at the hydrogen peroxide concentrations used in over-the-counter kits. What the light does only increases the risk of tooth sensitivity, with an odds ratio of 3.53. More sensitivity, no more whitening.
Maran et al. (2018) reached the same conclusion across a broader range of concentrations. The Carey (2014) review of the clinical evidence on whitening puts it plainly: light activation offers no benefit for the amount of whitening, the persistence of the result, or sensitivity.
So what is the gel doing in your LED kit? Working. Same as it would without the light. If you've already bought a light-up kit, don't throw the whole thing out. Use the gel as directed, and skip the light step. Your money is better spent on a second course of gel than on another light.
Paint-On Gels and Pens
Shorter contact time, lower concentration, lower outcome. These are fine for a small touch-up or a pre-event surface refresh, particularly if you've already whitened and want to brighten a single area. They're not a substitute for a proper tray or strip course.
At-Home "Natural" Whitening Methods, Honest Assessments
This is where most clinic articles get coy. We won't.
Activated Charcoal Toothpaste
The Journal of the American Dental Association published a literature review of 118 charcoal dentifrices in 2017 and concluded there is insufficient clinical and laboratory evidence to back the safety or efficacy claims manufacturers make (Brooks, Bashirelahi & Reynolds, 2017). Several products in the review were measured to be abrasive enough to damage enamel over time.
Verdict: skip it. You're paying for a black paste that doesn't whiten and might wear your enamel.
Oil Pulling
Swishing coconut oil around your mouth has become a whitening trend on social media. The American Dental Association states there are no reliable scientific studies showing oil pulling whitens teeth (ADA MouthHealthy: Oil Pulling). There is some low-quality evidence it may reduce plaque and gum inflammation, but none for bleaching.
Verdict: harmless, not a whitening method.
Baking Soda
Baking soda on its own is a mild abrasive that removes some surface stains. It is not a bleach, and it does not change the intrinsic colour of your teeth. A toothpaste that combines baking soda with hydrogen peroxide does have modest published evidence for shade change over 4 to 6 weeks of use (Ghassemi et al., 2012), but the active part of that formula is still the peroxide.
Verdict: a commercial baking-soda-plus-peroxide toothpaste is a fine surface-stain helper. Mixing baking soda with water at home is not necessary or particularly useful.
Lemon Juice (and Other Acidic Folk Remedies)
Lemon juice does change the colour of your teeth. The mechanism is not bleaching. It's acid erosion of the enamel (Abidia et al., 2023). You're removing the outer layer of your tooth, which temporarily exposes a different optical surface. The enamel doesn't grow back. Ever.
Verdict: do not do this. You're trading permanent enamel loss for a brief, illusory brightness.
Banana Peels, Strawberries, Apple Cider Vinegar
No peer-reviewed RCT evidence supports banana peels whitening teeth. Strawberries contain malic acid, which has the same erosion problem as lemon. Apple cider vinegar is just dilute acetic acid, and brings the same enamel damage.
Verdict: skip all three.
How At-Home Stacks Up Against In-Chair Whitening
The honest comparison surprises people.
The 2024 Heliyon umbrella review pooled 28 systematic reviews and 416 randomised trials comparing in-office and at-home peroxide whitening. The finding: no significant difference in final shade between in-office and at-home techniques over equivalent total contact time (Aidos et al., 2024).
In-chair is faster, not necessarily whiter. You can walk out with a visible change after 1 to 3 appointments, versus 2 to 4 weeks of nightly tray wear at home. For durability, the most reliable long-term result in the literature is the combined approach: an in-chair start, followed by short monthly take-home top-ups.
When In-Chair Whitening Is Genuinely the Better Call
There are situations where home methods underperform and you're better off in a dental chair:
Your staining is intrinsic and severe (tetracycline-grade, heavy fluorosis, or significant age-related dentine yellowing)
You have a real deadline, like a wedding or graduation, and need a result in days, not weeks
You've tried strips or kits and the result was uneven or disappointing
You've had sensitivity trouble at home and want supervised treatment with a desensitiser
You have multiple front-tooth crowns, veneers, or composite fillings and need a planned approach so the colours match afterwards
If any of these describe you, it's worth talking to a dentist about in-chair whitening at our practice instead of buying another kit that won't fix the underlying issue.
What About Sensitivity?
Tooth sensitivity is the most common side effect of any peroxide whitening, at home or in-chair. Across the studies, it's mild and transient for most people, and it resolves within a few days of stopping or reducing treatment (Cochrane Review, 2018).
Higher peroxide concentrations increase sensitivity risk. LED lights increase it too, without adding whitening benefit (He et al., 2012). So if you're sensitive, dropping the concentration and ditching the light are both sensible moves.
A potassium-nitrate desensitising toothpaste, used for 1 to 2 weeks before and during whitening, has been shown to reduce post-bleach sensitivity in a dedicated systematic review and meta-analysis (Martini et al., 2021). If pain becomes sharp, lasts longer than a few days, or wakes you up at night, stop and see your dentist.
Who Should Not Whiten Their Teeth at Home
Whitening is not for everyone, and a few situations are clear contraindications (reasons not to do this):
Pregnant or breastfeeding. There's no peroxide safety data in pregnancy, so it's a precautionary no.
Children and teenagers. The Australian Dental Association limits supply, and full-arch cosmetic bleaching is not recommended in mixed dentition (when baby and adult teeth are both present).
Untreated decay, exposed dentine, active gum disease, or recent oral surgery. Fix the underlying problem first. Peroxide on damaged tissue hurts.
Crowns, veneers, or visible composite fillings on front teeth. Peroxide doesn't change their colour. Whitening the natural teeth around them creates a mismatch. Plan the sequence with your dentist.
Tetracycline staining. Vital bleaching usually doesn't reach the dentine deeply enough. Veneers or crowns are the recognised treatment for this kind of discolouration.
Known allergy to peroxides.
How Long Will Whitening Actually Last?
Roughly 6 to 12 months for most people, and longer if you avoid heavy chromogens.
The longest-running follow-up data comes from Meireles et al. (2010), which tracked patients for two years after a course of 10% and 16% carbamide peroxide home whitening. At the 24-month mark, shade was still lighter than baseline for both concentrations, though some regression had occurred.
What speeds up the regression: coffee, tea, red wine, dark berries, curry, soy sauce, smoking, and vaping. Rinsing with water after a coffee helps. Using a straw for iced coffee helps a bit too.
For maintenance, a short top-up course every 6 to 12 months helps hold the shade for most people. That might be a 3 to 5 day strip refresher, or one to two nights in a custom tray. It's cheaper and less effort than starting from scratch each year.
Our Honest Take, A Sensible 4-Week At-Home Plan
This is where most clinic articles get vague. Here's the actual plan, based on the evidence we've cited above.
Week minus 1. If you're due a check-up, book one. Confirm you have no untreated decay, no exposed root surfaces, no leaky fillings. Ask your dentist to confirm there are no crowns, veneers, or visible composite fillings on the teeth you want to whiten. This five-minute conversation saves you from whitening around a front crown and ending up with an obvious colour mismatch.
Week 0. Switch to a potassium-nitrate sensitivity toothpaste. Use it twice a day for the whole week before you start. Don't brush immediately after acidic food or drink, since enamel is softer in that window.
Weeks 1 to 4. Pick ONE proven method and stick with it:
The easiest start: hydrogen peroxide whitening strips, used as directed on the box, usually over 14 days.
Best at-home result, if you're willing to invest: a custom-fit tray from your dentist, with prescribed carbamide peroxide gel, worn nightly for 2 to 3 weeks.
During treatment. If sensitivity flares up, take a 1 to 2 day break, then resume at a shorter contact time. Cut back on coffee, tea, and red wine if you can. If you can't, rinse with water afterwards.
After treatment. One short top-up every 6 to 12 months keeps the result stable. And skip the LED gimmick. Your money's better spent on a second course of gel than on a light that doesn't do anything.
Frequently Asked Questions
Does baking soda whiten teeth?
Baking soda on its own is a mild abrasive that removes surface stains, not a true bleach. It doesn't change the intrinsic colour of your teeth. A commercial toothpaste that combines baking soda with hydrogen peroxide does have modest published evidence for shade change over 4 to 6 weeks, but the active bleaching agent in that formula is the peroxide, not the baking soda. Home-made baking soda paste isn't necessary and isn't particularly helpful.
Are at-home teeth whitening kits actually safe?
Kits that stay within the Australian legal limit (6% hydrogen peroxide or 18% carbamide peroxide) have a good safety record in the published trials. The most common side effects are mild, temporary gum irritation and tooth sensitivity, both of which resolve after you finish the course. Kits sold above that limit are not legal for retail sale in Australia and should be avoided. If you have decay, gum disease, or front-tooth restorations, see a dentist first.
What's the difference between hydrogen peroxide and carbamide peroxide?
They're the same active ingredient in different forms. Carbamide peroxide breaks down on contact with saliva into hydrogen peroxide plus urea, in roughly a 1:3 ratio. So a 10% carbamide peroxide gel delivers about 3.5% hydrogen peroxide. Carbamide peroxide releases more slowly, which is why it's typical in overnight tray systems. Hydrogen peroxide acts faster and is more common in strips and in-chair treatments. Both whiten teeth through the same chemistry.
Do LED teeth whitening kits really work?
The gel works. The light doesn't. Two major meta-analyses (He 2012, Maran 2018) found that LED or blue-light activation does not improve shade outcomes at the hydrogen peroxide concentrations used in over-the-counter kits. The He 2012 study actually found the light increases the risk of sensitivity. If you've bought an LED kit, use the gel as directed and skip the light step. You're not missing out on any whitening effect, and you may get less sensitivity without it.
How long do at-home whitening results last?
Most people hold the result for 6 to 12 months, longer if they avoid heavy chromogens like coffee, tea, red wine, and curry. Two-year follow-up data from Meireles et al. 2010 shows teeth are still lighter than baseline at 24 months for both 10% and 16% carbamide peroxide, though some regression is normal. A short top-up every 6 to 12 months keeps the shade stable and costs far less than restarting from scratch each year.
Can yellow teeth become white again?
Usually yes, but the result depends on why they're yellow. Surface (extrinsic) stains from food, drink, and smoking respond well to peroxide-based whitening at home. Age-related dentine yellowing responds, though more slowly. Severe tetracycline staining, heavy fluorosis, and darkened teeth from old trauma often need in-chair treatment, internal bleaching, or veneers to reach a satisfying shade. A dental assessment will tell you which category you're in.
Can I whiten my teeth if I have crowns or veneers?
You can whiten your natural teeth, but the peroxide will not change the colour of crowns, veneers, or composite (tooth-coloured) fillings. They keep whatever shade they were made in. If you whiten the natural teeth around them, you'll end up with a visible mismatch. Plan the order with your dentist. Usually the natural teeth are whitened first, and any replacement crowns or veneers are then matched to the new, lighter shade.
Is teeth whitening safe during pregnancy?
No human trials have assessed peroxide whitening safety in pregnancy or breastfeeding, so the precautionary recommendation is to wait. The ADA and most dental bodies advise against elective bleaching during pregnancy and lactation for that reason. If you're planning a wedding or event, either whiten before you try to conceive, or wait until after you've finished breastfeeding. Routine dental check-ups and cleans during pregnancy are fine and recommended.
Written by Dr Cristian Dunker, BDSc, MBA.
Medically reviewed by Dr Cristian Dunker.
